Abstract
Objective
Sexual dysfunction and sleep problems are common in women. Nevertheless, the relationship between sleep problems and sexual dysfunction during pregnancy has yet to be fully clarified. The aim of this study was to evaluate the relationship between sleep problems and sexual dysfunction in pregnant women.
Methods
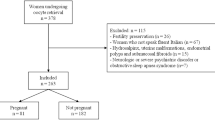
The study had a cross-sectional design and the sample was determined by employing the G*Power program on the basis of the findings of a related study. Taking the correlation value between the Female Sexual Function Index (FSFI) and the Insomnia Severity Index (ISI) into account, it was found that the minimum sample size was 219 pregnant women. Healthy pregnant women who were literate, did not have a diagnosed psychiatric disease, did not have a mental disability or communication problems, were in the gestation period, were not restricted by their doctors in terms of engaging in sexual activity, and who were willing to participate were included. The study included those pregnant women who consecutively attended the NST polyclinic in a maternity hospital in a province in the Black Sea region of Turkey between January 2022 and August 2022. The Sociodemographic Information Form, the Pittsburgh Sleep Quality Index (PSQI), the ISI, and the FSFI were used to collect data.
Results
A total of 220 pregnant women took part. The women had a mean age of 27.4 ± 6.3. Of the pregnant women, all had poor sleep quality: 61% had insomnia problems; 30% had sexual dysfunction. When the relationships between the PSQI, ISI and FSFI were examined, there was a statistically significant positive correlation between the mean PSQI and ISI scores (p = 0.000). A statistically significant negative correlation was determined between the mean ISI and FSFI scores (p = 0.044). According to the multiple regression analysis, age did not significantly predict sexual function (β = -0.112; t = -1.639; p = 0.103); insomnia severity predicted sexual function negatively (β = -0.146; t = -2.136; p = 0.034). The explained variance was 2.6%.
Conclusion
The findings suggest that sleep quality as measured by the PSQI does not correlate with female sexual dysfunction in pregnant women. However, severity of insomnia does correlate with sexual dysfunction.
Similar content being viewed by others
Data availability
The data that support the findings of this study are not openly available due to reasons of sensitivity and are available from the corresponding author upon reasonable request.
References
Çeli̇k F, Köse M (2017) Gebelikte uyku kalitesinin trimester ile ilişkisi. Kocatepe Tıp Dergisi 18:85–8
Miller EH (2004) Women and insomnia. Clin Cornerstone 6:6–18
Sharma S, Franco R (2004) Sleep and its disorders in pregnancy. Wis Med J 103:48–52
Fernández-Alonso AM, Trabalón-Pastor M, Chedraui P, Pérez-López FR (2012) Factors related to insomnia and sleepiness in the late third trimester of pregnancy. Arch Gynecol Obstet 286:55–61
Mobolaji Usman D, Peter AO, Akinyemi A, Adetunji O, Olutoyin OL (2018) Insomnia in pregnancy: Prevalence and predisposing factors in a developing country. Cent Afr J Public Health 4:65–68
Du M, Liu J, Han N, Zhao Z, Yang J, Xu X et al (2021) Maternal sleep quality during early pregnancy, risk factors and its impact on pregnancy outcomes: a prospective cohort study. Sleep Med 79:11–18
Taylor TF (2007) The origins of human sexual culture. J Psychol Hum Sex 18:69–105
Moseley A (2019) A'dan Z'ye Felsefe. Pegasus, İstanbul
Beyazıt F, Pek E, Şahin B (2018) Gebelik ve doğum sonrasında cinsel işlevlerde gözlenen değişiklikler: Önyargı mı? Yoksa Gerçek mi? Klinik Psikiyatri 21:397–406
Kennedy CM, Turcea AM, Bradley CS (2009) Prevalence of vulvar and vaginal symptoms during pregnancy and the puerperium. Int J Gynecol Obstet 105:236–239
Regan PC, Lyle JL, Otto AL, Joshi A (2003) Pregnancy and changes in female sexual desire: A review. Soc Behav Pers 31:603–611
Erol B, Sanli O, Korkmaz D, Seyhan A, Akman T, Kadioglu A (2007) A Cross-Sectional Study of Female Sexual Function and Dysfunction During Pregnancy. J Sex Med 4:1381–1387
Tosun Güleroğlu F, Gördeles BN (2014) Evaluation of sexual functions of the pregnant women. J Sex Med 11:146–153
Kling JM, Kapoor E, Mara K, Faubion SS (2021) Associations of sleep and female sexual function: good sleep quality matters. Menopause 28:619–625
Kalmbach DA, Arnedt JT, Pillai V, Ciesla JA (2015) The Impact of Sleep on Female Sexual Response and Behavior: A Pilot Study. J Sex Med 12:1221–1232
Seehuus M, Pigeon W (2018) The sleep and sex survey: Relationships between sexual function and sleep. J Psychosom Res 112:59–65
Ağargün MY, Kara H, Anlar O (1996) The validity and reliability of the Pittsburgh sleep quality index. Turk Psikiyatr Derg 7:107–115
Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research. Psychiatry Res 28:193–213
Bastien CH, Vallières A, Morin CM (2001) Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med 2:297–307
Boysan M, Gulec M, Besiroglu L, Kalafat T (2010) Psychometric properties of the insomnia severity index in Turkish sample. Anatol J Psychiatry 11:248–252
Aygin D, Eti AF (2005) Kadın Cinsel İşlev Ölçeği’nin Türkçeye Uyarlanması. Türkiye Klinikleri J Med Sci 25:393–399
Rosen R, Brown C, Heiman J, Leiblum S, Meston C, Shabsigh R et al (2000) The Female Sexual Function Index (FSFI): A Multidimensional Self-Report Instrument for the Assessment of Female Sexual Function. J Sex Marital Ther 26:191–208
Çayan S, Akbay E, Bozlu M, Canpolat B, Acar D, Ulusoy E (2004) The prevalence of female sexual dysfunction and potential risk factors that may impair sexual function in Turkish women. Urol Int 72:52–57
Sedov ID, Cameron EE, Madigan S, Tomfohr-Madsen LM (2018) Sleep quality during pregnancy: A meta-analysis. Sleep Med Rev 38:168–176
Gelaye B, Barrios YV, Zhong Q-Y, Rondon MB, Borba CPC, Sánchez SE et al (2015) Association of poor subjective sleep quality with suicidal ideation among pregnant Peruvian women. Gen Hosp Psychiatry 37:441–447
Mindell JA, Cook RA, Nikolovski J (2015) Sleep patterns and sleep disturbances across pregnancy. Sleep Med 16:483–488
Ahmed MR, Madny EH, Sayed Ahmed WA (2014) Prevalence of female sexual dysfunction during pregnancy among Egyptian women. J Obstet Gynaecol Res 40:1023–1029
Bartellas E, Crane JMG, Daley M, Bennett KA, Hutchens D (2000) Sexuality and sexual activity in pregnancy. BJOG Int J Obstet Gynaecol 107:964–8
Corbacioglu Esmer A, Akca A, Akbayir O, Goksedef BPC, Bakir VL (2013) Female sexual function and associated factors during pregnancy. J Obstet Gynaecol Res 39:1165–1172
Kerdarunsuksri A, Manusirivithaya S (2010) Attitudes and sexual function in Thai pregnant women. J Med Assoc Thai 93:265–271
Kucukdurmaz F, Efe E, Malkoc O, Kolus E, Amasyali AS, Resim S (2016) Prevalence and correlates of female sexual dysfunction among Turkish pregnant women. Turk J Urol 42:178–183
Naldoni LMV, Pazmiño MAV, Pezzan PAO, Pereira SB, Duarte G, Ferreira CHJ (2011) Evaluation of sexual function in Brazilian pregnant women. J Sex Marital Ther 37:116–129
Razali R, Balakrishnan K, Sidi H, Peter J, Razi Z (2012) Is sexual dysfunction common among pregnant Malaysian women? BJOG Int J Obstet Gynaecol 119:132
Sidi H, Puteh SEW, Abdullah N, Midin M (2007) The prevalence of sexual dysfunction and potential risk factors that may impair sexual function in Malaysian women. J Sex Med 4:311–321
Gokyildiz Surucu S, Avcibay Vurgec B, Kaya Senol D, Gozuyesil E, Bilgic D, Onat Koroglu C, Dağlar G, Avci N, Cayir G, Haliloğlu Peker B, Kizilkaya Beji N, Peker H, Yalcin O (2022) Evaluation of women’s sexual quality of life, depression, and sexual functions in the pregnancy and postpartum periods: a multi-centered study. J Obstet Gynaecol Res 48:1379–1389
Al-Badri M, Kapoor E, Faubion SS, Kling JM (2022) The Relationship Between Sleep and Sexual Function in Women. Curr Sex Health Rep 14:231–238
Ninivaggio C, Rogers RG, Leeman L, Migliaccio L, Teaf D, Qualls C (2017) Sexual function changes during pregnancy. Int Urogynecol J 28:923–929
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (name of institute/committee) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers' bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Altınayak, S.Ö., Rüzgar, Ş. & Koç, E. The relationship between sleep problems and sexual dysfunction among pregnant women in Turkey. Sleep Breath 28, 459–465 (2024). https://doi.org/10.1007/s11325-023-02896-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-023-02896-z