Abstract
Purpose
The aim of this prospective study was to investigate associations between nasal/oropharyngeal structures and a range of factors including age, gender, daytime sleepiness, and body mass index (BMI).
Methods
Patients with OSA were prospectively selected as research participants in rhinomanometric analysis as well as for otolaryngological evaluation. Participants were grouped as follows according to their apnea/hypopnea index (AHI) scores: no OSA (AHI < 5), mild OSA (5 ≤ AHI ≤ 15), moderate OSA (15 ≤ AHI < 30), and severe OSA (AHI ≥ 30). One-way analysis of variance (ANOVA), Kruskal–Wallis H, and Mann–Whitney U tests were performed to assess OSA severity in terms of the relationships between nasal resistance (NR) and anthropometric indices (body mass index (BMI), Friedman tongue position (FTP)), age, and gender.
Results
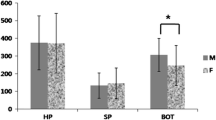
The study cohort of 177 men and 81 women ranged in age between 21 and 76 years, with BMI ranging from 23 to 45. In total, 37 patients were simple snorers (AHI < 5), and 221 patients were diagnosed with OSA. There was no significant difference among the AHI groups in terms of nasal volume (Vol05) (p = 0.952), mean flow (p = 0.778), and mean NR total (p = 0.723). A statistically significant difference was found between the AHI groups in terms of mean BMI and median FTP scores (p < 0.001).
Conclusion
This study provides evidence that that the oropharyngeal region (oropharynx, tongue, and vallecula) is a more important determinant of OSA severity than the nasal region.

Similar content being viewed by others
References
Avincsal MO, Dinc ME, Ulusoy S, Dalgic A, Ozdemir C, Develioglu ON (2017) Modified Mallampati score improves specificity of STOP-BANG Questionnaire for obstructive sleep apnea. J Craniofac Surg 28(4):904–908. https://doi.org/10.1097/SCS.0000000000003513
Nuckton TJ, Glidden DV, Browner WS, Claman DM (2006) Physical examination: Mallampati score as an independent predictor of obstructive sleep apnea. Sleep 29(7):903–908. https://doi.org/10.1093/sleep/29.7.903
Li HY, Wang PC, Hsu CY, Cheng ML, Liou CC, Chen NH (2005) Nasal resistance in patients with obstructive sleep apnea. ORL J Otorhinolaryngol Relat Spec 67(2):70–74. https://doi.org/10.1159/000084337
Miljeteig H, Hoffstein V, Cole P (1992) The effect of unilateral and bilateral nasal obstruction on snoring and sleep apnea. Laryngoscope 102:1150–1152
Schechter GL, Ware JC, Perlstrom J, McBrayer RH (1998) Nasal patency and the effectiveness of nasal continuous positive air pressure in obstructive sleep apnea. Otolaryngol Head Neck Surg 118(5):643–647. https://doi.org/10.1177/019459989811800513
Friedman M, Soans R, Gurpinar B, Lin HC, Joseph NJ (2008) Interexaminer agreement of Friedman tongue positions for staging of obstructive sleep apnea/hypopnea syndrome. Otolaryngol Head Neck Surg 139(3):372–377. https://doi.org/10.1016/j.otohns.2008.06.017
Kemppainen T, Ruoppi P, Seppä J, Sahlman J, Peltonen M, Tukiainen H, Gylling H, Vanninen E, Tuomilehto H (2008) Effect of weight reduction on rhinometric measurements in overweight patients with obstructive sleep apnea. Am J Rhinol. 22(4):410–5. https://doi.org/10.2500/ajr.2008.22.3203
Amra B, Pirpiran M, Soltaninejad F, Penzel T, Fietze I, Schoebel C (2019) The prediction of obstructive sleep apnea severity based on anthropometric and Mallampati indices. J Res Med Sci 24(24):66. https://doi.org/10.4103/jrms.JRMS_653_18
Sutherland K, Keenan BT, Bittencourt L, Chen NH, Gislason T, Leinwand S, Magalang UJ, Maislin G, Mazzotti DR, McArdle N, Mindel J, Pack AI, Penzel T, Singh B, Tufik S, Schwab RJ, Cistulli PA, SAGIC Investigators (2019) A global comparison of anatomic risk factors and their relationship to obstructive sleep apnea severity in clinical samples. J Clin Sleep Med 15(4):629–639. https://doi.org/10.5664/jcsm.7730
Rundo JV (2019) Obstructive sleep apnea basics. Cleve Clin J Med 86(9 Suppl 1):2–9. https://doi.org/10.3949/ccjm.86.s1.02
Friedman M, Maley A, Kelley K, Leesman C, Patel A, Pulver T, Joseph N, Catli T (2011) Impact of nasal obstruction on obstructive sleep apnea. Otolaryngol Head Neck Surg 144(6):1000–1004. https://doi.org/10.1177/0194599811400977
Valipour A (2014) The role of the nose in obstructive sleep apnea: a short review. Pneumologie 68(6):397–400. https://doi.org/10.1055/s-0034-1365488
Millman RP, Carlisle CC, McGarvey ST, Eveloff SE, Levinson PD (1995) Body fat distribution and sleep apnea severity in women. Chest 107(2):362–366. https://doi.org/10.1378/chest.107.2.362
Whittle AT, Marshall I, Mortimore IL, Wraith PK, Sellar RJ, Douglas NJ (1999) Neck soft tissue and fat distribution: comparison between normal men and women by magnetic resonance imaging. Thorax 54(4):323–328. https://doi.org/10.1136/thx.54.4.323.PMID:10092693;PMCID:PMC1745454
Pinto JA, Godoy LBM, Marquis VWPB, Sonego TB, Leal CFA, Ártico MS (2011) Anthropometric data as predictors of obstructive sleep apnea severity. Braz J Otorhinolaryngol 77(4):516–521. English, Portuguese. https://doi.org/10.1590/S1808-86942011000400017
Kumar HV, Schroeder JW, Gang Z, Sheldon SH (2014) Mallampati score and pediatric obstructive sleep apnea. J Clin Sleep Med 10(9):985–990. https://doi.org/10.5664/jcsm.4032
Suratt PM, Turner BL, Wilhoit SC (1986) Effect of intranasal obstruction on breathing during sleep. Chest 90(3):324–329. https://doi.org/10.1378/chest.90.3.324
Blakley BW, Mahowald MW (1987) Nasal resistance and sleep apnea. Laryngoscope 97(6):752–754. https://doi.org/10.1288/00005537-198706000-00023
Author information
Authors and Affiliations
Contributions
Concept, T.E.; design, T.E.; supervision, E.G.; materials, N.F. and T.E.; data collection and/or processing, N.F.; analysis and/or interpretation, T.E.; literature search, T.E.; writing manuscript, T.E.; critical review, N.A.
Corresponding author
Ethics declarations
Ethics approval
This study was approved as a prospective study by the Namık Kemal University Non-Interventional Clinical Research Ethics Committee with the number 2018/103/07/09. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ersözlü, T., Deniz, M., Fazlıoglu, N. et al. Understanding potential associations between anatomic and other factors in OSA severity. Sleep Breath 26, 1649–1653 (2022). https://doi.org/10.1007/s11325-021-02539-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02539-1