Abstract
Purpose
This study explored the interactive effects between polymorphonuclear neutrophils (PMNs) and vascular endothelial cells under intermittent hypoxia (IH) and investigated the mechanisms underlying these effects.
Methods
Endothelial cells were co-cultured with PMNs isolated from rats exposed to normoxia or IH. The PMN apoptotic rate was determined using flow cytometry. Expression of apoptosis-related proteins in the endothelial cells were evaluated using Western blotting, and the levels of intercellular adhesion molecules in the co-culture supernatants were measured using enzyme-linked immunosorbent assay.
Results
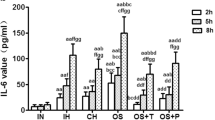
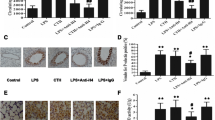
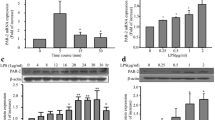
The PMN apoptotic rate in the IH-exposed rat group was significantly lower than that of the normoxia control group. There was a positive relationship between the PMN apoptotic rate and IH exposure time. In endothelial cells co-cultured with PMNs isolated from IH-exposed rats, a significant increase in the protein expression levels of Bax, Bcl-2, and caspase-3 and a significant decrease in the Bcl-2/Bax ratio were observed. Furthermore, the intercellular cell adhesion molecule-1(ICAM-1) and E-select element (E-S) levels were elevated significantly in the co-cultured supernatants of endothelial cells and PMNs from IH-exposed rats compared to that from controls. The above IH-induced alterations were partially restored by tempol pretreatment.
Conclusions
The apoptotic rate was low in PMNs from IH-exposed rats, which consequently increased the apoptotic signals in endothelial cells in vitro. This may be associated with the increased levels of intercellular adhesion molecules. Further, tempol partially attenuates the PMN-mediated pro-apoptotic effects on endothelial cells under IH.



Similar content being viewed by others
References
Benjafield AV, Ayas NT, Eastwood PR, Heinzer R, Ip MSM, Morrell MJ, Nunez CM, Patel SR, Penzel T, Pépin J-L, Peppard PE, Sinha S, Tufik S, Valentine K, Malhotra A (2019) Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Resp Med 7(8):687–698. https://doi.org/10.1016/s2213-2600(19)30198-5
Garvey JF, Taylor CT, McNicholas WT (2009) Cardiovascular disease in obstructive sleep apnoea syndrome: the role of intermittent hypoxia and inflammation. Eur Respir J 33(5):1195–1205. https://doi.org/10.1183/09031936.00111208
Arnaud C, Bochaton T, Pepin JL, Belaidi E (2020) Obstructive sleep apnoea and cardiovascular consequences: pathophysiological mechanisms. Arch Cardiovasc Dis 113(5):350–358. https://doi.org/10.1016/j.acvd.2020.01.003
Javaheri S, Barbe F, Campos-Rodriguez F, Dempsey JA, Khayat R, Javaheri S, Malhotra A, Martinez-Garcia MA, Mehra R, Pack AI, Polotsky VY, Redline S, Somers VK (2017) Sleep apnea: types, mechanisms, and clinical cardiovascular consequences. J Am Coll Cardiol 69(7):841–858. https://doi.org/10.1016/j.jacc.2016.11.069
Badran M, Golbidi S, Devlin A, Ayas N, Laher I (2014) Chronic intermittent hypoxia causes endothelial dysfunction in a mouse model of diet-induced obesity. Sleep Med 15(5):596–602. https://doi.org/10.1016/j.sleep.2014.01.013
Levy P, Kohler M, McNicholas WT, Barbe F, McEvoy RD, Somers VK, Lavie L, Pepin JL (2015) Obstructive sleep apnoea syndrome. Nat Rev Dis Primers 1:15015. https://doi.org/10.1038/nrdp.2015.15
Guo H, Cao J, Li J, Yang X, Jiang J, Feng J, Li S, Zhang J, Chen B (2015) Lymphocytes from intermittent hypoxia-exposed rats increase the apoptotic signals in endothelial cells via oxidative and inflammatory injury in vitro. Sleep Breath 19(3):969–976. https://doi.org/10.1007/s11325-015-1128-8
Williams MR, Azcutia V, Newton G, Alcaide P, Luscinskas FW (2011) Emerging mechanisms of neutrophil recruitment across endothelium. Trends Immunol 32(10):461–469. https://doi.org/10.1016/j.it.2011.06.009
Dyugovskaya L, Polyakov A, Lavie P, Lavie L (2008) Delayed neutrophil apoptosis in patients with sleep apnea. Am J Respir Crit Care Med 177(5):544–554. https://doi.org/10.1164/rccm.200705-675OC
Naruko T, Ueda M, Haze K, van der Wal AC, van der Loos CM, Itoh A, Komatsu R, Ikura Y, Ogami M, Shimada Y, Ehara S, Yoshiyama M, Takeuchi K, Yoshikawa J, Becker AE (2002) Neutrophil infiltration of culprit lesions in acute coronary syndromes. Circulation 106(23):2894–2900. https://doi.org/10.1161/01.cir.0000042674.89762.20
Zidar N, Jeruc J, Balazic J, Stajer D (2005) Neutrophils in human myocardial infarction with rupture of the free wall. Cardiovasc Pathol 14(5):247–250. https://doi.org/10.1016/j.carpath.2005.04.002
Biasucci LM, Liuzzo G, Giubilato S, Della Bona R, Leo M, Pinnelli M, Severino A, Gabriele M, Brugaletta S, Piro M, Crea F (2009) Delayed neutrophil apoptosis in patients with unstable angina: relation to C-reactive protein and recurrence of instability. Eur Heart J 30(18):2220–2225. https://doi.org/10.1093/eurheartj/ehp248
Garlichs CD, Eskafi S, Cicha I, Schmeisser A, Walzog B, Raaz D, Stumpf C, Yilmaz A, Bremer J, Ludwig J, Daniel WG (2004) Delay of neutrophil apoptosis in acute coronary syndromes. J Leukoc Biol 75(5):828–835. https://doi.org/10.1189/jlb.0703358
Haumer M, Amighi J, Exner M, Mlekusch W, Sabeti S, Schlager O, Schwarzinger I, Wagner O, Minar E, Schillinger M (2005) Association of neutrophils and future cardiovascular events in patients with peripheral artery disease. J Vasc Surg 41(4):610–617. https://doi.org/10.1016/j.jvs.2005.01.013
Vinten-Johansen J (2004) Involvement of neutrophils in the pathogenesis of lethal myocardial reperfusion injury. Cardiovasc Res 61(3):481–497. https://doi.org/10.1016/j.cardiores.2003.10.011
Jolly SR, Kane WJ, Hook BG, Abrams GD, Kunkel SL, Lucchesi BR (1986) Reduction of myocardial infarct size by neutrophil depletion: effect of duration of occlusion. Am Heart J 112(4):682–690. https://doi.org/10.1016/0002-8703(86)90461-8
Kin H, Wang NP, Halkos ME, Kerendi F, Guyton RA, Zhao ZQ (2006) Neutrophil depletion reduces myocardial apoptosis and attenuates NFkappaB activation/TNFalpha release after ischemia and reperfusion. J Surg Res 135(1):170–178. https://doi.org/10.1016/j.jss.2006.02.019
Li S, Feng J, Wei S, Qian X, Cao J, Chen B (2015) Delayed neutrophil apoptosis mediates intermittent hypoxia-induced progressive heart failure in pressure-overloaded rats. Sleep Breath 20(1):95–102. https://doi.org/10.1007/s11325-015-1190-2
Strober W (2015) Trypan Blue Exclusion Test of Cell Viability. Curr Protoc Immunol 111:A3.B.1-a3.B.3. https://doi.org/10.1002/0471142735.ima03bs111
Istvan V, Clemens H, Helga SN, R. C, (1995) A novel assay for apoptosis Flow cytometric detection of phosphatidylserine expression on early apoptotic cells using fluorescein labelled Annexin V. J Immunol Methods 184:39–51
Harbrecht BG, Billiar TR, Curran RD, Stadler J, Simmons RL (1993) Hepatocyte injury by activated neutrophils in vitro is mediated by proteases. Ann Surg 218:120–128
Dyugovskaya L, Polyakov A (2010) Neutrophil apoptosis and hypoxia. Fiziol Zh 56(5):115–124
Buckley CD, Ross EA, McGettrick HM, Osborne CE, Haworth O, Schmutz C, Stone PC, Salmon M, Matharu NM, Vohra RK, Nash GB, Rainger GE (2006) Identification of a phenotypically and functionally distinct population of long-lived neutrophils in a model of reverse endothelial migration. J Leukoc Biol 79(2):303–311. https://doi.org/10.1189/jlb.0905496
Dyugovskaya L, Polyakov A, Ginsberg D, Lavie P, Lavie L (2011) Molecular pathways of spontaneous and TNF-{alpha}-mediated neutrophil apoptosis under intermittent hypoxia. Am J Respir Cell Mol Biol 45(1):154–162. https://doi.org/10.1165/rcmb.2010-0025OC
Larissa Dyugovskaya AP, Cohen-Kaplan V, Lavie P, Lavie L (2012) Bax/Mcl-1 balance affects neutrophil survival in intermittent hypoxia and obstructive sleep apnea: effects of p38MAPK and ERK1/2 signaling. J Transl Med 10:211–224
Lavie L (2015) Oxidative stress in obstructive sleep apnea and intermittent hypoxia–revisited–the bad ugly and good: implications to the heart and brain. Sleep Med Rev 20:27–45. https://doi.org/10.1016/j.smrv.2014.07.003
Li S, Qian XH, Zhou W, Zhang Y, Feng J, Wan NS, Zhang Z, Guo R, Chen BY (2011) Time-dependent inflammatory factor production and NFkappaB activation in a rodent model of intermittent hypoxia. Swiss Med Wkly 141:w13309. https://doi.org/10.4414/smw.2011.13309
Chello M, Anselmi A, Spadaccio C, Patti G, Goffredo C, Di Sciascio G, Covino E (2007) Simvastatin increases neutrophil apoptosis and reduces inflammatory reaction after coronary surgery. Ann Thorac Surg 83(4):1374–1380. https://doi.org/10.1016/j.athoracsur.2006.10.065
Libby P (2002) Inflammation in atherosclerosis. Nature 420:868–874
Foster GE, Poulin MJ, Hanly PJ (2007) Intermittent hypoxia and vascular function: implications for obstructive sleep apnoea. Exp Physiol 92(1):51–65. https://doi.org/10.1113/expphysiol.2006.035204
Yamagata K (2020) Protective Effect of Epigallocatechin Gallate on Endothelial Disorders in Atherosclerosis. J Cardiovasc Pharmacol 75(4):292–298. https://doi.org/10.1097/FJC.0000000000000792
Perrotta I (2020) The microscopic anatomy of endothelial cells in human atherosclerosis: Focus on ER and mitochondria. J Anat 237(6):1015–1025. https://doi.org/10.1111/joa.13281
Cancel LM, Ebong EE, Mensah S, Hirschberg C, Tarbell JM (2016) Endothelial glycocalyx, apoptosis and inflammation in an atherosclerotic mouse model. Atherosclerosis 252:136–146. https://doi.org/10.1016/j.atherosclerosis.2016.07.930
Hlubocka Z, Umnerova V, Heller S, Peleska J, Jindra A, Jachymova M, Kvasnicka J, Horky K, Aschermann M (2002) Circulating intercellular cell adhesion molecule-1, endothelin-1 and von Willebrand factor-markers of endothelial dysfunction in uncomplicated essential hypertension: the effect of treatment with ACE inhibitors. J Hum Hypertens 16(8):557–562. https://doi.org/10.1038/sj.jhh.1001403
Pilkauskaite G, Miliauskas S, Vitkauskiene A, Sakalauskas R (2014) Vascular adhesion molecules in men with obstructive sleep apnea: associations with obesity and metabolic syndrome. Sleep Breath 18(4):869–874. https://doi.org/10.1007/s11325-014-0958-0
Kaczmarek E, Bakker JP, Clarke DN, Csizmadia E, Kocher O, Veves A, Tecilazich F, O’Donnell CP, Ferran C, Malhotra A (2013) Molecular biomarkers of vascular dysfunction in obstructive sleep apnea. PLoS ONE 8(7):e70559. https://doi.org/10.1371/journal.pone.0070559
Hung MW, Kravtsov GM, Lau CF, Poon AM, Tipoe GL, Fung ML (2013) Melatonin ameliorates endothelial dysfunction, vascular inflammation, and systemic hypertension in rats with chronic intermittent hypoxia. J Pineal Res 55(3):247–256. https://doi.org/10.1111/jpi.12067
Jiang Y, Jiang L-LI, Maimaitirexiati X-MZY, Zhang Y, Wu L (2015) Irbesartan attenuates TNF-α-induced ICAM-1, VCAM-1, and E-selectin expression through suppression of NF-κB pathway in HUVECs. Eur Rev Med Pharmacol Sc 19(17):3295–3302
Kent BD, Ryan S, McNicholas WT (2011) Obstructive sleep apnea and inflammation: relationship to cardiovascular co-morbidity. Respir Physiol Neurobiol 178(3):475–481. https://doi.org/10.1016/j.resp.2011.03.015
Ramar K, Caples SM (2011) Vascular changes, cardiovascular disease and obstructive sleep apnea. Future Cardiol 7(2):241–249. https://doi.org/10.2217/fca.10.123
Zhao H, Zhao Y, Li X, Xu L, Jiang F, Hou W, Dong L, Cao J (2018) Effects of Antioxidant Tempol on Systematic Inflammation and Endothelial Apoptosis in Emphysematous Rats Exposed to Intermittent Hypoxia. Yonsei Med J 59(9):1079–1087. https://doi.org/10.3349/ymj.2018.59.9.1079
Funding
This work was supported by the National Natural Science Foundation of China (No. 81670084, 81970084).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the Animal Ethical and Welfare committee of Tianjin Medical University guidelines for the care and use of animals.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, J., Wang, L., Hu, J. et al. Polymorphonuclear neutrophils promote endothelial apoptosis by enhancing adhesion upon stimulation by intermittent hypoxia. Sleep Breath 26, 1173–1180 (2022). https://doi.org/10.1007/s11325-021-02503-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02503-z