Abstract
Purpose
Although polysomnography (PSG) is the gold standard for monitoring sleep, it has many limitations. We aimed to prospectively determine the validity of wearable sleep-tracking devices and smartphone applications by comparing the data to that of PSGs.
Methods
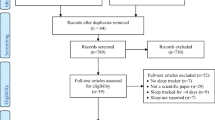
Patients who underwent one night of attended PSG at a single institution from January, 2015 to July 2019 were recruited. Either a sleep application or wearable device was used simultaneously while undergoing PSG. Nine smartphone applications and three wearable devices were assessed.
Results
We analyzed the results of 495 cases of smartphone applications and 170 cases of wearables by comparing each against PSG. None of the tested applications were able to show a statistically significant correlation between sleep efficiency, durations of wake time, light sleep or deep sleep with PSG. Snore time correlated well in both of the two applications which provided such information. Deep sleep duration and WASO measured by two of the three wearable devices correlated significantly with PSG. Even after controlling for transition count and moving count, the correlation indices of the wearables did not increase, suggesting that the algorithms used by the wearables were not largely affected by tossing and turning.
Conclusions
Most of the applications tested in this study showed poor validity, while wearable devices mildly correlated with PSG. An effective use for these devices may be as a tool to identify the change seen in an individual’s sleep patterns on a day-to-day basis, instead of as a method of detecting absolute measurements.



Similar content being viewed by others
References
Luyster FS, Strollo PJ, Jr., Zee PC, Walsh JK, Boards of Directors of the American Academy of Sleep M, the Sleep Research S (2012) Sleep: a health imperative. Sleep 35(6):727–734
Watson NF, Badr MS, Belenky G, Bliwise DL, Buxton OM, Buysse D, Dinges DF, Gangwisch J, Grandner MA, Kushida C, Malhotra RK, Martin JL, Patel SR, Quan SF, Tasali E (2015) Recommended Amount of Sleep for a Healthy Adult: A Joint Consensus Statement of the American Academy of Sleep Medicine and Sleep Research Society. Sleep 38(6):843–844
Kryger MH, Roth T, Dement WC (2017) Principles and practice of sleep medicine, Sixth, edition. Elsevier, Philadelphia, PA
Baron KG, Duffecy J, Berendsen MA, Cheung Mason I, Lattie EG, Manalo NC (2018) Feeling validated yet? A scoping review of the use of consumer-targeted wearable and mobile technology to measure and improve sleep. Sleep Med Rev 40:151–159
Khosla S, Deak MC, Gault D, Goldstein CA, Hwang D, Kwon Y, O’Hearn D, Schutte-Rodin S, Yurcheshen M, Rosen IM, Kirsch DB, Chervin RD, Carden KA, Ramar K, Aurora RN, Kristo DA, Malhotra RK, Martin JL, Olson EJ, Rosen CL, Rowley JA, Academy American, of Sleep Medicine Board of D, (2018) Consumer Sleep Technology: An American Academy of Sleep Medicine Position Statement. J Clin Sleep Med 14(5):877–880
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep M (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8(5):597-619
Fino E, Plazzi G, Filardi M, Marzocchi M, Pizza F, Vandi S, Mazzetti M (2020) (Not so) Smart sleep tracking through the phone: Findings from a polysomnography study testing the reliability of four sleep applications. J Sleep Res 29(1):e12935
Choi YK, Demiris G, Lin SY, Iribarren SJ, Landis CA, Thompson HJ, McCurry SM, Heitkemper MM, Ward TM (2018) Smartphone Applications to Support Sleep Self-Management: Review and Evaluation. J Clin Sleep Med 14(10):1783–1790
Fino E, Mazzetti M (2019) Monitoring healthy and disturbed sleep through smartphone applications: a review of experimental evidence. Sleep Breath 23(1):13–24
Lee-Tobin PA, Ogeil RP, Savic M, Lubman DI (2017) Rate My Sleep: Examining the Information, Function, and Basis in Empirical Evidence Within Sleep Applications for Mobile Devices. J Clin Sleep Med 13(11):1349–1354
Bhat S, Ferraris A, Gupta D, Mozafarian M, DeBari VA, Gushway-Henry N, Gowda SP, Polos PG, Rubinstein M, Seidu H, Chokroverty S (2015) Is There a Clinical Role For Smartphone Sleep Apps? Comparison of Sleep Cycle Detection by a Smartphone Application to Polysomnography. J Clin Sleep Med 11(7):709–715
Kazikdas KC (2019) The Perioperative Utilization of Sleep Monitoring Applications on Smart Phones in Habitual Snorers With Isolated Inferior Turbinate Hypertrophy. Ear Nose Throat J 98(1):32–36
Kang SG, Kang JM, Ko KP, Park SC, Mariani S, Weng J (2017) Validity of a commercial wearable sleep tracker in adult insomnia disorder patients and good sleepers. J Psychosom Res 97:38–44
Kahawage P, Jumabhoy R, Hamill K, de Zambotti M, Drummond SPA (2020) Validity, potential clinical utility, and comparison of consumer and research-grade activity trackers in Insomnia Disorder I: In-lab validation against polysomnography. J Sleep Res 29(1):e12931
de Zambotti M, Goldstone A, Claudatos S, Colrain IM, Baker FC (2018) A validation study of Fitbit Charge 2 compared with polysomnography in adults. Chronobiol Int 35(4):465–476
Gruwez A, Bruyneel AV, Bruyneel M (2019) The validity of two commercially-available sleep trackers and actigraphy for assessment of sleep parameters in obstructive sleep apnea patients. PLoS One 14(1):e0210569
Ameen MS, Cheung LM, Hauser T, Hahn MA, Schabus M (2019) About the Accuracy and Problems of Consumer Devices in the Assessment of Sleep. Sensors (Basel) 19(19)
Degroote L, Hamerlinck G, Poels K, Maher C, Crombez G, De Bourdeaudhuij I, Vandendriessche A, Curtis RG, DeSmet A (2020) Low-Cost Consumer-Based Trackers to Measure Physical Activity and Sleep Duration Among Adults in Free-Living Conditions: Validation Study. JMIR Mhealth Uhealth 8(5):e16674
Xu ZF, Luo X, Shi J, Lai Y (2019) Quality analysis of smart phone sleep apps in China: can apps be used to conveniently screen for obstructive sleep apnea at home? BMC Med Inform Decis Mak 19(1):224
Funding
This research was supported by a National Research Foundation of Korea grant funded by the Korean Government (2017R1E1A1A01074543) and the Korean Health Technology R&D Project, Ministry of Health & Welfare, Republic of Korea (HC15C3415).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the institutional IRB (AJIRB-MED-MDB-17-328, AJIRB-DEV-DEO-14-293).
Conflict of interest
The authors do not have any financial or nonfinancial conflicts of interest to disclose.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, K., Park, DY., Song, Y.J. et al. Consumer-grade sleep trackers are still not up to par compared to polysomnography. Sleep Breath 26, 1573–1582 (2022). https://doi.org/10.1007/s11325-021-02493-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02493-y