Abstract
Purpose
This study aimed to investigate pharyngeal paraesthesia symptoms in patients with obstructive sleep apnoea (OSA).
Material and methods
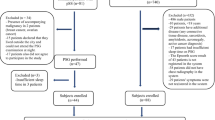
Patients with snoring and suspected OSA as well as age-matched controls were recruited. All participants underwent nocturnal polysomnography (PSG) and pharyngeal paraesthesia assessment using the Glasgow-Edinburgh throat scale (GETS). The incidence and severity of pharyngeal paraesthesia symptoms were compared between the groups.
Results
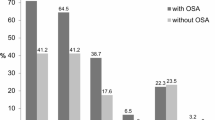
A total of 280 patients who snored or were suspected of having OSA and 35 healthy, age-matched controls were recruited. The total pharyngeal paraesthesia symptom score was significantly higher in the OSA group than in the healthy group (12 [5, 23] vs. 3 [0, 9]; p < 0.001). The most frequent pharyngeal paraesthesia symptoms in the snore patients were Q7 (catarrh down the throat) and Q3 (discomfort/irritation in the throat), which are related to the irritability of the throat. The incidence of Q7 (OSA, 58% vs. controls, 14%; χ2 = 23.66; p < 0.001), Q3 (OSA, 46% vs. controls, 3%; χ2 = 23.07; p < 0.001), Q1 (feeling of something stuck in the throat; OSA, 33% vs. controls, 6%; χ2 = 11.00; p = 0.001), Q6 (swelling in the throat; OSA, 31% vs. controls, 0%; χ2 = 14.53; p < 0.001), Q9 (want to swallow all the time; OSA, 20% vs. controls, 6%; χ2 = 6.28; p = 0.012), Q5 (throat closing off; OSA, 24% vs. controls, 6%; χ2 = 6.16; p = 0.013), and Q2 (pain in the throat; OSA, 23% vs. controls, 6%; χ2 = 5.32; p = 0.021) was significantly higher in the OSA group than in the controls
Conclusions
Patients with obstructive sleep apnoea have higher pharyngeal paraesthesia symptoms scores and tend to have irritated throats compared to healthy controls.
Clinical trial registration
ClinicalTrials.gov identifier: NCT03506178.



Similar content being viewed by others
References
Ryan S, Arnaud C, Fitzpatrick SF, Gaucher J, Tamisier R (2019) Adipose tissue as a key player in obstructive sleep apnoea. 28(152). https://doi.org/10.1183/16000617.0006-2019
Li C, Zhang Y, Chen Y, Su T, Zhao Y, Shi S (2020) Cell-autonomous autophagy protects against chronic intermittent hypoxia induced sensory nerves and endothelial dysfunction of the soft palate. Med Sci Monit 26:e920878. https://doi.org/10.12659/msm.920878
Patel J, Ray B, Fernandez-Salvador C, Gouveia C, Zaghi S, Camacho M (2018) Neuromuscular function of the soft palate and uvula in snoring and obstructive sleep apnea: a systematic review. Am J Otolaryngol 39(3):327–337. https://doi.org/10.1016/j.amjoto.2018.03.006
Larsson H, Carlsson-Nordlander B, Lindblad LE, Norbeck O, Svanborg E (1992) Temperature thresholds in the oropharynx of patients with obstructive sleep apnea syndrome. Am Rev Respir Dis 146(5 Pt 1):1246–1249. https://doi.org/10.1164/ajrccm/146.5_Pt_1.1246
Kimoff RJ, Sforza E, Champagne V, Ofiara L, Gendron D (2001) Upper airway sensation in snoring and obstructive sleep apnea. Am J Respir Crit Care Med 164(2):250–255. https://doi.org/10.1164/ajrccm.164.2.2010012
Guilleminault C, Li K, Chen NH, Poyares D (2002) Two-point palatal discrimination in patients with upper airway resistance syndrome, obstructive sleep apnea syndrome, and normal control subjects. Chest 122(3):866–870
Hagander L, Harlid R, Svanborg E (2009) Quantitative sensory testing in the oropharynx: a means of showing nervous lesions in patients with obstructive sleep apnea and snoring. Chest 136(2):481–489. https://doi.org/10.1378/chest.08-2747
Kim SW, Park HW, Won SJ, Jeon SY, Jin HR, Lee SJ, Chang DY, Kim DW (2013) Palatal sensory threshold reflects nocturnal hypoxemia and airway occlusion in snorers and obstructive sleep apnea patients. J Clin Sleep Med 9(11):1179–1186. https://doi.org/10.5664/jcsm.3164
Jeong KH, Yang Y, Choi HR, Cho JH, Kim GT, Kim JK (2016) Assessment of change in palatal sensation in obstructive sleep apnea patients by using two-point palatal discrimination. Clin Exp Otorhinolaryngol 9(3):226–232. https://doi.org/10.21053/ceo.2015.01375
Heiser C, Zimmermann I, Sommer JU, Hormann K, Herr RM, Stuck BA (2013) Pharyngeal chemosensitivity in patients with obstructive sleep apnea and healthy subjects. Chem Senses 38(7):595–603. https://doi.org/10.1093/chemse/bjt031
An Y, Li Y, Chang W, Gao F, Ding X, Xu W, Han D (2019) Quantitative evaluation of the function of the sensory nerve fibers of the palate in patients with obstructive sleep apnea. J Clin Sleep Med 15(9):1347–1353. https://doi.org/10.5664/jcsm.7756
Deary IJ, Wilson JA, Harris MB, MacDougall G (1995) Globus pharyngis: development of a symptom assessment scale. J Psychosom Res 39(2):203–213
Tang B, Cai HD, Xie HL, Chen DY, Jiang SM, Jia L (2016) Epidemiology of globus symptoms and associated psychological factors in China. J Dig Dis 17(5):319–324. https://doi.org/10.1111/1751-2980.12354
Nam SW, Lim DH, Cho KY, Kim HS, Kim K, Chung TY (2018) Risk factors of presenile nuclear cataract in health screening study. BMC Ophthalmol 18(1):263. https://doi.org/10.1186/s12886-018-0928-6
Sunnergren O, Brostrom A, Svanborg E (2011) Soft palate sensory neuropathy in the pathogenesis of obstructive sleep apnea. Laryngoscope 121(2):451–456. https://doi.org/10.1002/lary.21371
Senaratna CV, Perret JL, Lodge CJ, Lowe AJ, Campbell BE, Matheson MC, Hamilton GS, Dharmage SC (2017) Prevalence of obstructive sleep apnea in the general population: a systematic review. Sleep Med Rev 34:70–81. https://doi.org/10.1016/j.smrv.2016.07.002
Singh M, Liao P, Kobah S, Wijeysundera DN, Shapiro C, Chung F (2013) Proportion of surgical patients with undiagnosed obstructive sleep apnoea. Br J Anaesth 110(4):629–636. https://doi.org/10.1093/bja/aes465
Gamaldo C, Buenaver L, Chernyshev O, Derose S, Mehra R, Vana K, Walia HK, Gonzalez V, Gurubhagavatula I (2018) Evaluation of clinical tools to screen and assess for obstructive sleep apnea. J Clin Sleep Med 14(7):1239–1244. https://doi.org/10.5664/jcsm.7232
Tapia IE, Bandla P, Traylor J, Karamessinis L, Huang J, Marcus CL (2010) Upper airway sensory function in children with obstructive sleep apnea syndrome. Sleep 33(7):968–972
Alsubie HS, BaHammam AS (2017) Obstructive sleep apnoea: children are not little adults. Paediatr Respir Rev 21:72–79. https://doi.org/10.1016/j.prrv.2016.02.003
Martinez-Garcia MA, Campos-Rodriguez F, Barbé F, Gozal D, Agustí A (2019) Precision medicine in obstructive sleep apnoea. Lancet Respir Med 7(5):456–464. https://doi.org/10.1016/s2213-2600(19)30044-x
Funding
This was not an industry-supported study. An Yunsong is supported by Medical Science and Technology Research Foundation of Guangdong Province (A2020018) and Science and Technology Special Fund of Guangdong Provincial People’s Hospital (2020bq01).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
An, Y., Gao, F., Su, X. et al. Characteristics of pharyngeal paraesthesia symptoms in patients with obstructive sleep apnoea. Sleep Breath 25, 2163–2169 (2021). https://doi.org/10.1007/s11325-021-02325-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02325-z