Abstract
Rationale
Retrospective studies indicate that obstructive sleep apnea occurs often after aneurysmal subarachnoid hemorrhage. We aim to investigate if obstructive sleep apnea is associated with impaired blood pressure control early after subarachnoid hemorrhage.
Methods
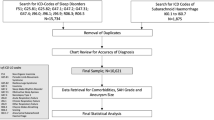
Patients with subarachnoid hemorrhage were recruited and screened for sleep apnea using cardiorespiratory polygraphy within 48 h after intensive care unit admission, and 6 months after hospital discharge at home. Blood pressure was continuously measured using intra-arterial catheter within the first 24 h after admission. Time between hospital admission and first blood pressure below 140 mmHg, and time with elevated blood pressure within the first 24 h after admission were compared between patients with and without obstructive sleep apnea.
Results
Of 60 patients, 55 successfully completed the study. Obstructive sleep apnea (AHI > 5/h) was diagnosed in 32% of men and 24% of women. While the time to reach a blood pressure of 140 mmHg did not differ (60.0 ± 26.2 min vs. 49.7 ± 16.4 min; p = 0.74), obstructive sleep apnea patients spent more time with blood pressure above 140 mmHg (292.0 ± 114.0 vs. 96.9 ± 28.3 min per 24 h; p = 0.025, CI 95 −363.6 to −26.5) within the observational period. Only AHI and diagnosed hypertension were significant predictors for elevated blood pressure (R2 0.42; p = 0.03).
Conclusion
Obstructive sleep apnea is associated in our study with poor blood pressure control early after subarachnoid hemorrhage. These patients may need advanced management for blood pressure including management for OSA following subarachnoid hemorrhage. Screening for sleep apnea in patients with subarachnoid hemorrhage is recommended.
Trial registration
ClincalTrials.gov identifier: NCT02724215, registered on March 31, 2016.



Similar content being viewed by others
References
Rincon F, Rossenwasser RH, Dumont A (2013) The epidemiology of admissions of nontraumatic subarachnoid hemorrhage in the United States. Neurosurgery 73:217–223. https://doi.org/10.1227/01.neu.0000430290.93304.33
Walendy V, Strauss C, Rachinger J, Stang A (2014) Treatment of aneurysmal subarachnoid haemorrhage in Germany: a nationwide analysis of the years 2005-2009. Neuroepidemiology 42:90–97. https://doi.org/10.1159/000355843
Macdonald RL, Schweizer TA (2017) Spontaneous subarachnoid haemorrhage. Lancet. 389:655–666. https://doi.org/10.1016/S0140-6736(16)30668-7
Güresir E, Vatter H, Schuss P, Platz J, Konczalla J, de Rochement RDM, Berkefeld J, Seifert V (2013) Natural history of small unruptured anterior circulation aneurysms: a prospective cohort study. Stroke 44:3027–3031. https://doi.org/10.1161/STROKEAHA.113.001107
Andreasen TH, Bartek J, Andresen M, Springborg JB, Romner B (2013) Modifiable risk factors for aneurysmal subarachnoid hemorrhage. Stroke 44:3607–3612. https://doi.org/10.1161/STROKEAHA.113.001575
Connolly ES, Rabinstein AA, Carhuapoma JR et al (2012) Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 43:1711–1737. https://doi.org/10.1161/STR.0b013e3182587839
Lin QS, Chen P, Lin YX et al (2016) Systolic blood pressure variability is a novel risk factor for rebleeding in acute subarachnoid hemorrhage: a case-control study. Medicine (Baltimore). https://doi.org/10.1097/MD.0000000000003028
Jordan AS, McSharry DG, Malhotra A (2014) Adult obstructive sleep apnoea. Lancet 383:736–747. https://doi.org/10.1016/S0140-6736(13)60734-5
Heinzer R, Vat S, Marques-Vidal P, Marti-Soler H, Andries D, Tobback N, Mooser V, Preisig M, Malhotra A, Waeber G, Vollenweider P, Tafti M, Haba-Rubio J (2015) Prevalence of sleep-disordered breathing in the general population: the HypnoLaus study. Lancet Respir Med 3:310–318. https://doi.org/10.1016/S2213-2600(15)00043-0
Kohler M, Stradling JR (2010) Mechanisms of vascular damage in obstructive sleep apnea. Nat Rev Cardiol 7:677–685. https://doi.org/10.1038/nrcardio.2010.145
Kotikoski S, Huttunen J, Huttunen TJ, Helin K, Frösen J, Koivisto T, Kurki MI, von und zu Fraunberg M, Kunnamo I, Jääskeläinen JE, Lindgren AE (2018) Secondary hypertension in patients with saccular intracranial aneurysm disease: a population based study. PLoS One 13:e0206432
Redline S, Yenokyan G, Gottlieb DJ, Shahar E, O'Connor GT, Resnick HE, Diener-West M, Sanders MH, Wolf PA, Geraghty EM, Ali T, Lebowitz M, Punjabi NM (2010) Obstructive sleep apnea-hypopnea and incident stroke: the sleep heart health study. Am J Respir Crit Care Med 182:269–277. https://doi.org/10.1164/rccm.200911-1746OC
Lisabeth LD, Scheer RV, Li C, Case E, Chervin RD, Zahuranec DB, Morgenstern LB, Garcia NM, Tower S, Brown DL (2018) Intracerebral hemorrhage and sleep-disordered breathing. Sleep Med 46:114–116. https://doi.org/10.1016/j.sleep.2018.03.005
Schuiling WJ, Rinkel GJE, Walchenbach R, De Weerd AW (2005) Disorders of sleep and wake in patients after subarachnoid hemorrhage. Stroke 36:578–582. https://doi.org/10.1161/01.STR.0000154862.33213.73
Alaqeel AM, Almasri SH, Alotaibi NM, Al-Yamany MA, Bahammam AS, Mohammad YM, Sharif MM (2013) Neurosciences (Riyadh) 18(3):248–251
Zaremba S, Albus L, Schuss P, Vatter H, Klockgether T, Güresir E (2019) Increased risk for subarachnoid hemorrhage in patients with sleep apnea. J Neurol. https://doi.org/10.1007/s00415-019-09265-5
Zaremba S, Güresir E (2019; published online Feb) Is there a causal relationship between obstructive sleep apnea and the pathophysiology of intracranial aneurysm? Somnologie. https://doi.org/10.1007/s11818-019-0191-y
Martynowicz H, Porębska I, Poręba R, Mazur G, Brzecka A (2016) Nocturnal blood pressure variability in patients with obstructive sleep apnea syndrome. In: Pokorski M (ed) Advancements in clinical research. Advances in Experimental Medicine and Biology, vol 952. Springer, Cham.
Bir SC, Nanda A, Cuellar H, Sun H, Guthikonda B, Liendo C, Minagar A, Chernyshev OY (2017) Coexistence of obstructive sleep apnea worsens the overall outcome of intracranial aneurysm: a pioneer study. J Neurosurg 128:735–746. https://doi.org/10.3171/2016.10.JNS162316
Brown RD, Broderick JP (2014) Unruptured intracranial aneurysms: epidemiology, natural history, management options, and familial screening. Lancet Neurol 13:393–404. https://doi.org/10.1016/S1474-4422(14)70015-8
Walia HK, Li H, Rueschman M, Bhatt DL, Patel SR, Quan SF, Gottlieb DJ, Punjabi NM, Redline S, Mehra R (2014) Association of severe obstructive sleep apnea and elevated blood pressure despite antihypertensive medication use. J Clin Sleep Med 10:835–843. https://doi.org/10.5664/jcsm.3946
Somers VK, Dyken ME, Clary MP, Abboud FM (1995) Sympathetic neural mechanisms in obstructive sleep apnea. J Clin Invest 96:1897–1904. https://doi.org/10.1172/JCI118235
Phillips BG, Narkiewicz K, Pesek CA, Haynes WG, Dyken ME, Somers VK (1999) Effects of obstructive sleep apnea on endothelin-1 and blood pressure. J Hypertens 17:61–66. https://doi.org/10.1097/00004872-199917010-00010
Kourembanas S, Marsden PA, McQuillan LP, Faller DV (1991) Hypoxia induces endothelin gene expression and secretion in cultured human endothelium. J Clin Invest 88:1054–1057. https://doi.org/10.1172/JCI115367
Gjørup PH, Sadauskiene L, Wessels J, Nyvad O, Strunge B, Pedersen EB (2007) Abnormally increased endothelin-1 in plasma during the night in obstructive sleep apnea: relation to blood pressure and severity of disease. Am J Hypertens 20:44–52. https://doi.org/10.1016/j.amjhyper.2006.05.021
Moussouttas M, Lai EW, Huynh TT, James J, Stocks-Dietz C, Dombrowski K, Khoury J, Pacak K (2014) Association between acute sympathetic response, early onset vasospasm, and delayed vasospasm following spontaneous subarachnoid hemorrhage. J Clin Neurosci 21:256–262. https://doi.org/10.1016/j.jocn.2013.03.036
Ma Y, Sun S, Peng CK, Fang Y, Thomas RJ (2017) Ambulatory blood pressure monitoring in Chinese patients with obstructive sleep apnea. J Clin Sleep Med 13:433–439. https://doi.org/10.5664/jcsm.6498
Zaremba S, Shin CH, Hutter MM, Malviya SA, Grabitz SD, MacDonald T, Diaz-Gil D, Ramachandran SK, Hess D, Malhotra A, Eikermann M (2016) Continuous positive airway pressure mitigates opioid-induced worsening of sleep-disordered breathing early after bariatric surgery. Anesthesiology 125:92–104. https://doi.org/10.1097/ALN.0000000000001160
Martínez-García MÁ, Capote F, Campos-Rodríguez F, Lloberes P, Díaz de Atauri MJ, Somoza M, Masa JF, González M, Sacristán L, Barbé F, Durán-Cantolla J, Aizpuru F, Mañas E, Barreiro B, Mosteiro M, Cebrián JJ, de la Peña M, García-Río F, Maimó A, Zapater J, Hernández C, Grau SanMarti N, Montserrat JM, Spanish Sleep Network (2013) Effect of CPAP on blood pressure in patients with obstructive sleep apnea and resistant hypertension: the HIPARCO randomized clinical trial. JAMA 310:2407–2415. https://doi.org/10.1001/jama.2013.281250
Kepplinger J, Barlinn K, Albright KC, Schrempf W, Boehme AK, Pallesen LP, Schwanebeck U, Graehlert X, Storch A, Reichmann H, Alexandrov AV, Bodechtel U (2013) Early sleep apnea screening on a stroke unit is feasible in patients with acute cerebral ischemia. J Neurol 260:1343–1350. https://doi.org/10.1007/s00415-012-6803-0
Timm FP, Zaremba S, Grabitz SD, Farhan HN, Zaremba S, Siliski E, Shin CH, Muse S, Friedrich S, Mojica JE, Kurth T, Ramachandran SK, Eikermann M (2018) Effects of opioids given to facilitate mechanical ventilation on sleep apnea after extubation in the intensive care unit. Sleep 41. https://doi.org/10.1093/sleep/zsx191
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zaremba, S., Albus, L., Vatter, H. et al. Poor blood pressure control following subarachnoid hemorrhage in patients with sleep apnea. Sleep Breath 25, 777–785 (2021). https://doi.org/10.1007/s11325-020-02184-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02184-0