Abstract
Purpose
The aim of this study was to evaluate the diaphragm thickness in patients with obstructive sleep apnea syndrome (OSAS).
Methods
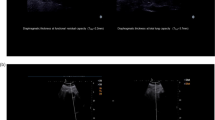
This prospective study included patients who underwent polysomnography evaluation for the first time with a clinical suspicion of OSAS. All patients underwent polysomnographic evaluation with a 55-channel Alice 6 computerized system (Respironics; Philips, IL). Diaphragm thickness was measured as the distance between the peritoneum and the pleura using electronic calipers with a 7–12-MHz linear probe (PHILIPS EPIQ 5G).
Results
A total of 108 patients (67 males, 41 females) were enrolled in the current study. The mean age of the patients was 48.92 ± 11.47 years. The diaphragm thicknesses were significantly higher in OSAS patients both at end-inspirium and end-expirium compared with the normal group (p < 0.05). No significant difference was observed regarding the change level and thickening ratio (%) (p > 0.05). When the patients were allocated into OSAS subtypes; diaphragm thicknesses at the end of inspirium and expirium on both sides were significantly higher in the severe OSAS group and OSAS+OHS group compared with the other groups of normal, mild OSAS, and moderate OSAS subgroups (p < 0.05 for all). There was no significant difference between the groups regarding the thickening ratio (p > 0.05 for all). There was a positive correlation between the severity of OSAS and diaphragm thickness.
Conclusion
Diaphragm thickness seems to be increased in OSAS patients and the thickness correlates with the severity of OSAS. However, the thickness ratio of OSAS patients does not differ from that of normal subjects.


Similar content being viewed by others
References
Pazarli AC, Ekiz T, İnönü Köseoğlu H (2018) Association between 25-hydroxyvitamin D and bone mineral density in people with obstructive sleep apnea syndrome. J Clin Densitom 22(1):39–46. https://doi.org/10.1016/j.jocd.2018.10.001
Epstein LJ, Kristo D, Strollo PJ Jr, Friedman N, Malhotra A, Patil SP, Ramar K, Rogers R, Schwab RJ, Weaver EM, Weinstein MD (2009) Adult Obstructive Sleep ApneaTask Force of the American Academy of Sleep Medicine. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J Clin Sleep Med 5(3):263–276
Matziaras G, Vlami K, Antaraki A, Papastefanou A, Balafas V, Kostomitsopoulos N, Papiris S, Kostakis A (2011) Ultrasound evaluation of diaphragmatic function in obstructive sleep apnea. Eur Respir J 38(Suppl 55):2219
El-Kabir DR, Polkey MI, Lyall RA, Williams AJ, Moxham J (2003) The effect of treatment on diaphragm contractility in obstructive sleep apnea syndrome. Respir Med 97(9):1021–1026. https://doi.org/10.1016/S0954-6111(03)00132-X
Wilcox PG, Paré PD, Road JD, Fleetham JA (1990) Respiratory muscle function during obstructive sleep apnea. Am Rev Respir Dis 142(3):533–539
Crimi C, Heffler E, Augelletti T, Campisi R, Noto A, Vancheri C, Crimi N (2018) Utility of ultrasound assessment of diaphragmatic function before and after pulmonary rehabilitation in COPD patients. Int J Chron Obstruct Pulmon Dis 13:3131–3139. https://doi.org/10.2147/COPD.S171134
de Bruin PF, Ueki J, Watson A, Pride NB (1997) Size and strength of the respiratory and quadriceps muscles in patients with chronic asthma. Eur Respir J 10(1):59–64
O’Gorman CM, O’Brien TG, Boon AJ (2017) Utility of diaphragm ultrasound in myopathy. Muscle Nerve 55(3):427–429. https://doi.org/10.1002/mus.25429
Fayssoil A, Behin A, Ogna A, Mompoint D, Amthor H, Clair B, Laforet P, Mansart A, Prigent H, Orlikowski D, Stojkovic T, Vinit S, Carlier R, Eymard B, Lofaso F, Annane D (2018) Diaphragm: pathophysiology and ultrasound imaging in neuromuscular disorders. J Neuromuscul Dis 5(1):1–10. https://doi.org/10.3233/JND-170276
Jung JH, Kim NS (2017) The correlation between diaphragm thickness, diaphragmatic excursion, and pulmonary function in patients with chronic stroke. J Phys Ther Sci 29(12):2176–2179. https://doi.org/10.1589/jpts.29.2176
Llamas-Álvarez AM, Tenza-Lozano EM, Latour-Pérez J (2017) Diaphragm and lung ultrasound to predict weaning outcome: systematic review and meta-analysis. Chest 152(6):1140–1150
Hudgel DW (2016) Sleep apnea severity classification - revisited. Sleep 39(5):1165–1166. https://doi.org/10.5665/sleep.5776
Dubé B, Dres M (2016) Diaphragm dysfunction: diagnostic approaches and management strategies. J Clin Med 5(12):113. https://doi.org/10.3390/jcm5120113
Khurana J, Gartner SC, Naik L, Tsui BCH (2018) Ultrasound identification of diaphragm by novices using ABCDE technique. Reg Anesth Pain Med 43(2):161–165. https://doi.org/10.1097/AAP.0000000000000718
Goligher EC, Laghi F, Detsky ME, Farias P, Murray A, Brace D, Brochard LJ, Bolz SS, Rubenfeld G, Kavanagh BP et al (2015) Measuring diaphragm thickness with ultrasound in mechanically ventilated patients: feasibility, reproducibility and validity. Intensive Care Med 41:642–649. https://doi.org/10.1007/s00134-015-3687-3
Malas FÜ, Köseoğlu F, Kara M, Ece H, Aytekin M, Öztürk GT, Özçakar L, Ulaşlı AM (2019) Diaphragm ultrasonography and pulmonary function tests in patients with spinal cord injury. Spinal Cord 57(8):679–683. https://doi.org/10.1038/s41393-019-0275-3
Dempsey JA, Veasey SC, Morgan BJ, O’Donnell CP (2010) Pathophysiology of sleep apnea. Physiol Rev 90(1):47–112
Horner RL (2009) Emerging principles and neural substrates underlying tonic sleep-state-dependent influences on respiratory motor activity. Philos Trans R Soc Lond Ser B Biol Sci 364(1529):2553–2564. https://doi.org/10.1098/rstb.2009.0065
Fitts RH, Riley DR, Widrick JJ (2001) Functional and structural adaptations of skeletal muscle to microgravity. J Exp Biol 204(Pt 18):3201–3208
Noda Y, Sekiguchi K, Kohara N, Kanda F, Toda T (2016) Ultrasonographic diaphragm thickness correlates with compound muscle action potential amplitude and forced vital capacity. Muscle Nerve 53(4):522–527. https://doi.org/10.1002/mus.24902
Gottesman E, McCool FD (1997) Ultrasound evaluation of the paralyzed diaphragm. Am J Respir Crit Care Med 155(5):1570–1574
De Bruin PF, Ueki J, Bush A, Khan Y, Watson A, Pride NB (1997) Diaphragm thickness and inspiratory strength in patients with Duchenne muscular dystrophy. Thorax 52(5):472–475
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pazarlı, A.C., Özmen, Z., İnönü Köseoğlu, H. et al. Ultrasonographic measurement of the diaphragm thickness in patients with obstructive sleep apnea syndrome. Sleep Breath 24, 89–94 (2020). https://doi.org/10.1007/s11325-019-01931-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01931-2