Abstract
Study objectives
We prospectively investigated the effects of continuous positive airway pressure (CPAP) on long-term cognitive and psychomotor performances, and excessive daytime sleepiness in severe obstructive sleep apnea (OSA) patients.
Methods
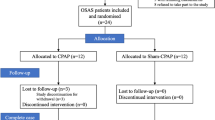
A total of 40 patients were recruited and 23 patients with severe OSA fully completed the study protocol to investigate the effects of CPAP therapy on psychomotor performance at 1, 3, and 6 months and 1 year following initiation of the therapy. Psychomotor CRD-series tests measuring reaction times of light stimulus perception, solving simple arithmetic operations, and complex psychomotor limb coordination, were used in this study. The data collected following CPAP therapy were compared to baseline values prior to the CPAP treatment for each patient.
Results
All of the measured variables improved following CPAP treatment. However, the most pronounced effect was observed in improvement of reaction times to complex psychomotor limb coordination test (p < 0.05). Self-reported evaluation of excessive daytime sleepiness measured by Epworth Sleepiness Scale (ESS) showed significant decrease from 10.0 ± 1.1 before to 3.5 ± 0.5 (p < 0.001), after 1 year on CPAP therapy.
Conclusions
The CPAP therapy improved cognitive and psychomotor performance on CRD-series tests with the most significant improvement observed in complex psychomotor limb coordination of severe OSA patients.



Similar content being viewed by others
References
American Academy of Sleep Medicine Aiawt, SOCIETY ESR, RESEARCH JSOS, SOCIETY LAS (2014) International Classification of Sleep Disorders – Third Edition (ICSD-3)
Decary A, Rouleau I, Montplaisir J (2000) Cognitive deficits associated with sleep apnea syndrome: a proposed neuropsychological test battery. Sleep 23(3):369–381
Aloia MS, Ilniczky N, Di Dio P, Perlis ML, Greenblatt DW, Giles DE (2003) Neuropsychological changes and treatment compliance in older adults with sleep apnea. J Psychosom Res 54(1):71–76
Aloia MS, Arnedt JT, Davis JD, Riggs RL, Byrd D (2004) Neuropsychological sequelae of obstructive sleep apnea-hypopnea syndrome: a critical review. J Int Neuropsychol Soc : JINS 10(5):772–785. https://doi.org/10.1017/S1355617704105134
Engleman HM, Douglas NJ (2004) Sleep. 4: sleepiness, cognitive function, and quality of life in obstructive sleep apnoea/hypopnoea syndrome. Thorax 59(7):618–622
Bucks RS, Olaithe M, Eastwood P (2013) Neurocognitive function in obstructive sleep apnoea: a meta-review. Respirology 18(1):61–70. https://doi.org/10.1111/j.1440-1843.2012.02255.x
Stranks EK, Crowe SF (2016) The cognitive effects of obstructive sleep apnea: an updated meta-analysis. Arch Clin Neuropsychol 31(2):186–193. https://doi.org/10.1093/arclin/acv087
Knoepke CAM (2009) Proposed mechanism of cognitive dysfunction in obstructive sleep apnea. Primary Psychiatry 16(10):51–66
Verstraeten E, Cluydts R, Pevernagie D, Hoffmann G (2004) Executive function in sleep apnea: controlling for attentional capacity in assessing executive attention. Sleep 27(4):685–693
Grigg-Damberger M, Ralls F (2012) Cognitive dysfunction and obstructive sleep apnea: from cradle to tomb. Curr Opin Pulm Med 18(6):580–587. https://doi.org/10.1097/MCP.0b013e328358be18
Kylstra WA, Aaronson JA, Hofman WF, Schmand BA (2013) Neuropsychological functioning after CPAP treatment in obstructive sleep apnea: a meta-analysis. Sleep Med Rev 17(5):341–347. https://doi.org/10.1016/j.smrv.2012.09.002
Landry S, O'Driscoll DM, Hamilton GS, Conduit R (2016) Overnight motor skill learning outcomes in obstructive sleep apnea: effect of continuous positive airway pressure. J Clin Sleep Med : JCSM : Off Publ Am Acad Sleep Med 12(5):681–688. https://doi.org/10.5664/jcsm.5794
Karanovic N, Carev M, Kardum G, Pecotic R, Valic M, Karanovic S, Ujevic A, Dogas Z (2009) The impact of a single 24 h working day on cognitive and psychomotor performance in staff anaesthesiologists. Eur J Anaesthesiol 26(10):825–832. https://doi.org/10.1097/EJA.0b013e32832bb6e4
Petri NM, Dropulic N, Kardum G (2006) Effects of voluntary fluid intake deprivation on mental and psychomotor performance. Croat Med J 47(6):855–861
Radic J, Ljutic D, Radic M, Kovacic V, Sain M, Dodig-Curkovic K (2011) Is there differences in cognitive and motor functioning between hemodialysis and peritoneal dialysis patients? Ren Fail 33(6):641–649. https://doi.org/10.3109/0886022X.2011.586480
Galic T, Bozic J, Pecotic R, Ivkovic N, Valic M, Dogas Z (2016) Improvement of cognitive and psychomotor performance in patients with mild to moderate obstructive sleep apnea treated with mandibular advancement device: a prospective 1-year study. J Clin Sleep Med : JCSM : Off Publ Am Acad Sleep Med 12(2):177–186. https://doi.org/10.5664/jcsm.5480
Epstein LJ, Kristo D, Strollo PJ, Jr., Friedman N, Malhotra A, Patil SP, Ramar K, Rogers R, Schwab RJ, Weaver EM, Weinstein MD (2009) Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J Clin Sleep Med 5 (3):263–276
Pecotic R, Dodig IP, Valic M, Ivkovic N, Dogas Z (2012) The evaluation of the Croatian version of the Epworth Sleepiness Scale and STOP questionnaire as screening tools for obstructive sleep apnea syndrome. Sleep Breath 16(3):793–802. https://doi.org/10.1007/s11325-011-0578-x
Kushida CA, Littner MR, Morgenthaler T, Alessi CA, Bailey D, Coleman J, Jr., Friedman L, Hirshkowitz M, Kapen S, Kramer M, Lee-Chiong T, Loube DL, Owens J, Pancer JP, Wise M (2005) Practice parameters for the indications for polysomnography and related procedures: an update for 2005. Sleep 28 (4):499–521
Drenovac M (2001) An analysis of some attributes of the dynamics of mental processing. Rev Psychol 8:61–67
Quan SF, Wright R, Baldwin CM, Kaemingk KL, Goodwin JL, Kuo TF, Kaszniak A, Boland LL, Caccappolo E, Bootzin RR (2006) Obstructive sleep apnea-hypopnea and neurocognitive functioning in the sleep heart health study. Sleep Med 7(6):498–507. https://doi.org/10.1016/j.sleep.2006.02.005
Sforza E, Roche F (2012) Sleep apnea syndrome and cognition. Front Neurol 3:87. https://doi.org/10.3389/fneur.2012.00087
Beebe DW, Gozal D (2002) Obstructive sleep apnea and the prefrontal cortex: towards a comprehensive model linking nocturnal upper airway obstruction to daytime cognitive and behavioral deficits. J Sleep Res 11(1):1–16
Ferini-Strambi L, Marelli S, Galbiati A, Castronovo C (2013) Effects of continuous positive airway pressure on cognition and neuroimaging data in sleep apnea. Int J Psychophysiol : Off J Int Org Psychophysiol 89(2):203–212. https://doi.org/10.1016/j.ijpsycho.2013.03.022
Olaithe M, Bucks RS (2013) Executive dysfunction in OSA before and after treatment: a meta-analysis. Sleep 36(9):1297–1305. https://doi.org/10.5665/sleep.2950
Ohayon MM, Carskadon MA, Guilleminault C, Vitiello MV (2004) Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals: developing normative sleep values across the human lifespan. Sleep 27(7):1255–1273
George CF, Boudreau AC, Smiley A (1997) Effects of nasal CPAP on simulated driving performance in patients with obstructive sleep apnoea. Thorax 52(7):648–653
Kushida CA, Nichols DA, Holmes TH, Quan SF, Walsh JK, Gottlieb DJ, Simon RD, Jr., Guilleminault C, White DP, Goodwin JL, Schweitzer PK, Leary EB, Hyde PR, Hirshkowitz M, Green S, McEvoy LK, Chan C, Gevins A, Kay GG, Bloch DA, Crabtree T, Dement WC (2012) Effects of continuous positive airway pressure on neurocognitive function in obstructive sleep apnea patients: the apnea positive pressure long-term efficacy study (APPLES). Sleep 35 (12):1593–1602. doi:https://doi.org/10.5665/sleep.2226
Munoz A, Mayoralas LR, Barbe F, Pericas J, Agusti AG (2000) Long-term effects of CPAP on daytime functioning in patients with sleep apnoea syndrome. Eur Respir J 15(4):676–681
Landry S, Anderson C, Andrewartha P, Sasse A, Conduit R (2014) The impact of obstructive sleep apnea on motor skill acquisition and consolidation. J Clin Sleep Med : JCSM : Off Publ Am Acad Sleep Med 10(5):491–496. https://doi.org/10.5664/jcsm.3692
Mihalj M, Lusic L, Dogas Z (2016) Reduced evoked motor and sensory potential amplitudes in obstructive sleep apnea patients. J Sleep Res 25(3):287–295. https://doi.org/10.1111/jsr.12368
Acknowledgments
The authors wish to thank Jelena Baricevic and Dijana Radanovic bacc. med. techn. for their technical assistance.
Funding
Croatian Science Foundation provided financial support in the form of grant #IP-11-2013-5935 funding.
The sponsor had no role in the design or conduct of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (Ethics Committee of the University of Split School of Medicine (USSM)) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Pecotic, R., Dodig, I.P., Valic, M. et al. Effects of CPAP therapy on cognitive and psychomotor performances in patients with severe obstructive sleep apnea: a prospective 1-year study. Sleep Breath 23, 41–48 (2019). https://doi.org/10.1007/s11325-018-1642-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-018-1642-6