Abstract
Purpose
Pregnant women are particularly susceptible to sleep-disordered breathing. Obstructive sleep apnea (OSA) in pregnancy is associated with poor pregnancy and fetal outcomes. Oxidative stress caused by intermittent hypoxemia and reoxygenation may impact pregnancy health. We hypothesize that pregnant women with OSA have a pronounced oxidative stress profile.
Methods
A case-control study was performed to study oxidative stress markers in the serum of pregnant women with or without OSA. Patients with OSA were identified between 2003 and 2009. Contemporaneous controls were pregnant subjects without apnea, gasping, or snoring around the time of delivery. Serum markers of oxidative and carbonyl stress were measured by spectrophotometric/fluorometric methods. Multiple linear regression analysis was used with a model including age, body mass index at delivery, history of diabetes, and gestational age.
Results
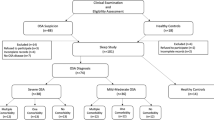
Serum samples from 23 OSA cases and 41 controls were identified. Advanced oxidation protein products, a marker for oxidative stress, and advanced glycation end products (AGEs), a marker for carbonyl stress, were significantly lower in women with OSA than in controls (p value <0.0001). Total antioxidant capacity was higher in women with OSA in comparison to controls (p value <0.0001). The difference in AGEs remained significant even after adjusting for confounders.
Conclusion
Contrary to our hypothesis, the results of this study suggest that pregnant women with OSA have higher antioxidant capacity and lower oxidative and carbonyl stress markers compared to controls, suggesting a possible protective effect of intermittent hypoxia. Whether OSA in pregnancy impacts oxidative stress differently than OSA in the general population remains to be confirmed.


Similar content being viewed by others
References
Punjabi NM, Shahar E, Redline S, Gottlieb DJ, Givelber R, Resnick HE (2004) Sleep-disordered breathing, glucose intolerance, and insulin resistance: the Sleep Heart Health Study. Am J Epidemiol 160(6):521–530. doi:10.1093/aje/kwh261
Gottlieb DJ, Redline S, Nieto FJ, Baldwin CM, Newman AB, Resnick HE et al (2006) Association of usual sleep duration with hypertension: the Sleep Heart Health Study. Sleep 29(8):1009–1014
Redline S, Yenokyan G, Gottlieb DJ, Shahar E, O’Connor GT, Resnick HE et al (2010) Obstructive sleep apnea-hypopnea and incident stroke: the sleep heart health study. Am J Respir Crit Care Med 182(2):269–277. doi:10.1164/rccm.200911-1746OC
Lavie L, Lavie P (2009) Molecular mechanisms of cardiovascular disease in OSAHS: the oxidative stress link. Eur Respir J. 33(6):1467–1484. doi:10.1183/09031936.00086608
Young T, Palta M, Dempsey J, Peppard PE, Nieto FJ, Hla KM (2009) Burden of sleep apnea: rationale, design, and major findings of the Wisconsin Sleep Cohort study. WMJ 108(5):246–249
Bourjeily G, Raker CA, Chalhoub M, Miller MA (2010) Pregnancy and fetal outcomes of symptoms of sleep-disordered breathing. Eur Respir J 36(4):849–855. doi:10.1183/09031936.00021810
O’Brien LM, Bullough AS, Owusu JT, Tremblay KA, Brincat CA, Chames MC et al (2012) Pregnancy-onset habitual snoring, gestational hypertension, and preeclampsia: prospective cohort study. Am J Obstet Gynecol 207(6):487.e1–487.e9. doi:10.1016/j.ajog.2012.08.034
Louis J, Auckley D, Miladinovic B, Shepherd A, Mencin P, Kumar D et al (2012) Perinatal outcomes associated with obstructive sleep apnea in obese pregnant women. Obstet Gynecol 120(5):1085–1092. doi:10.1097/AOG.0b013e31826eb9d8
Reutrakul S, Zaidi N, Wroblewski K, Kay HH, Ismail M, Ehrmann DA et al (2013) Interactions between pregnancy, obstructive sleep apnea, and gestational diabetes mellitus. J Clin Endocrinol Metab 98(10):4195–4202. doi:10.1210/jc.2013-2348
Louis JM, Mogos MF, Salemi JL, Redline S, Salihu HM (2014) Obstructive sleep apnea and severe maternal-infant morbidity/mortality in the United States, 1998-2009. Sleep 37(5):843–849. doi:10.5665/sleep.3644
Jurkovicova I, Celec P, Mucska I, Hodosy J (2003) On the origin of cardiovascular complications of sleep apnea syndrome by the means of molecular interactions. Bratisl Lek Listy 104(4–5):167–173
Ellis EM (2007) Reactive carbonyls and oxidative stress: potential for therapeutic intervention. Pharmacol Ther 115(1):13–24. doi:10.1016/j.pharmthera.2007.03.015
Clerici G, Slavescu C, Fiengo S, Kanninen TT, Romanelli M, Biondi R et al (2012) Oxidative stress in pathological pregnancies. J Obstet Gynaecol 32(2):124–127. doi:10.3109/01443615.2011.637139
Eisele HJ, Markart P, Schulz R (2015) Obstructive sleep apnea, oxidative stress, and cardiovascular disease: evidence from human studies. Oxidative Med Cell Longev 2015:608438. doi:10.1155/2015/608438
Jurkovicova I, Celec P (2004) Sleep apnea syndrome and its complications. Acta Med Austriaca 31(2):45–50
Yamauchi M, Nakano H, Maekawa J, Okamoto Y, Ohnishi Y, Suzuki T et al (2005) Oxidative stress in obstructive sleep apnea. Chest 127(5):1674–1679. doi:10.1378/chest.127.5.1674
Ravishankar S, Bourjeily G, Lambert-Messerlian G, He M, De Paepe ME, Gundogan F (2015) Evidence of placental hypoxia in maternal sleep disordered breathing. Pediatr Dev Pathol 18(5):380–386. doi:10.2350/15-06-1647-OA.1
Celec P, Jurkovicova I, Buchta R, Bartik I, Gardlik R, Palffy R et al (2013) Antioxidant vitamins prevent oxidative and carbonyl stress in an animal model of obstructive sleep apnea. Sleep Breath 17(2):867–871. doi:10.1007/s11325-012-0728-9
Sanchis-Gomar F, Vina J, Lippi G (2012) Intermittent hypobaric hypoxia applicability in myocardial infarction prevention and recovery. J Cell Mol Med 16(5):1150–1154. doi:10.1111/j.1582-4934.2011.01508.x
Vogtel M, Michels A (2010) Role of intermittent hypoxia in the treatment of bronchial asthma and chronic obstructive pulmonary disease. Curr Opin Allergy Clin Immunol 10(3):206–213. doi:10.1097/ACI.0b013e32833903a6
Bourjeily G, Butterfield K, Curran P, Lambert-Messerlian G (2015) Obstructive sleep apnea is associated with alterations in markers of fetoplacental wellbeing. J Matern Fetal Neonatal Med 28(3):262–266. doi:10.3109/14767058.2014.913131
Bourjeily G, Curran P, Butterfield K, Maredia H, Carpenter M, Lambert-Messerlian G (2015) Placenta-secreted circulating markers in pregnant women with obstructive sleep apnea. J Perinat Med 43(1):81–87. doi:10.1515/jpm-2014-0052
Maislin G, Pack AI, Kribbs NB, Smith PL, Schwartz AR, Kline LR et al (1995) A survey screen for prediction of apnea. Sleep 18(3):158–166
Tothova L, Hodosy J, Mucska I, Celec P (2014) Salivary markers of oxidative stress in patients with obstructive sleep apnea treated with continuous positive airway pressure. Sleep Breath 18(3):563–570. doi:10.1007/s11325-013-0919-z
Bourjeily G, Mazer J, Paglia M (2013) Outcomes of sleep disordered breathing in pregnancy. Open Sleep J 6(Suppl 1: M4):28–36. doi:10.2174/1874620901306010028
Izci-Balserak B, Pien GW (2014) The relationship and potential mechanistic pathways between sleep disturbances and maternal hyperglycemia. Curr Diab Rep 14(2):459. doi:10.1007/s11892-013-0459-8
Dikmenoglu N, Ciftci B, Ileri E, Guven SF, Seringec N, Aksoy Y et al (2006) Erythrocyte deformability, plasma viscosity and oxidative status in patients with severe obstructive sleep apnea syndrome. Sleep Med 7(3):255–261. doi:10.1016/j.sleep.2005.12.005
Jordan W, Cohrs S, Degner D, Meier A, Rodenbeck A, Mayer G et al (2006) Evaluation of oxidative stress measurements in obstructive sleep apnea syndrome. J Neural Transm (Vienna) 113(2):239–254. doi:10.1007/s00702-005-0316-2
Selmi C, Montano N, Furlan R, Keen CL, Gershwin ME (2007) Inflammation and oxidative stress in obstructive sleep apnea syndrome. Exp Biol Med (Maywood) 232(11):1409–1413. doi:10.3181/0704-mr-103
Ozkan Y, Firat H, Simsek B, Torun M, Yardim-Akaydin S (2008) Circulating nitric oxide (NO), asymmetric dimethylarginine (ADMA), homocysteine, and oxidative status in obstructive sleep apnea-hypopnea syndrome (OSAHS). Sleep Breath 12(2):149–154. doi:10.1007/s11325-007-0148-4
Qanungo S, Mukherjea M (2000) Ontogenic profile of some antioxidants and lipid peroxidation in human placental and fetal tissues. Mol Cell Biochem 215(1–2):11–19
Fialova L, Malbohan I, Kalousova M, Soukupova J, Krofta L, Stipek S et al (2006) Oxidative stress and inflammation in pregnancy. Scand J Clin Lab Invest 66(2):121–127. doi:10.1080/00365510500375230
Huang QT, Zhong M, Tian JW, Hou FF (2013) Higher plasma AOPP is associated with increased proteinuria excretion and decreased glomerular filtration rate in pre-eclamptic women. Pregnancy Hypertens 3(1):16–20. doi:10.1016/j.preghy.2012.08.001
Karacay O, Sepici-Dincel A, Karcaaltincaba D, Sahin D, Yalvac S, Akyol M et al (2010) A quantitative evaluation of total antioxidant status and oxidative stress markers in preeclampsia and gestational diabetic patients in 24-36 weeks of gestation. Diabetes Res Clin Pract 89(3):231–238. doi:10.1016/j.diabres.2010.04.015
de Ranitz-Greven WL, Bos DC, Poucki WK, Visser GH, Beulens JW, Biesma DH et al (2012) Advanced glycation end products, measured as skin autofluorescence, at diagnosis in gestational diabetes mellitus compared with normal pregnancy. Diabetes Technol Ther 14(1):43–49. doi:10.1089/dia.2011.0105
de Ranitz-Greven WL, Kaasenbrood L, Poucki WK, Hamerling J, Bos DC, Visser GH et al (2012) Advanced glycation end products, measured as skin autofluorescence, during normal pregnancy and pregnancy complicated by diabetes mellitus. Diabetes Technol Ther 14(12):1134–1139. doi:10.1089/dia.2012.0120
Pertynska-Marczewska M, Glowacka E, Sobczak M, Cypryk K, Wilczynski J (2009) Glycation endproducts, soluble receptor for advanced glycation endproducts and cytokines in diabetic and non-diabetic pregnancies. Am J Reprod Immunol 61(2):175–182. doi:10.1111/j.1600-0897.2008.00679.x
Oliver EA, Buhimschi CS, Dulay AT, Baumbusch MA, Abdel-Razeq SS, Lee SY et al (2011) Activation of the receptor for advanced glycation end products system in women with severe preeclampsia. J Clin Endocrinol Metab 96(3):689–698. doi:10.1210/jc.2010-1418
Toescu V, Nuttall SL, Martin U, Nightingale P, Kendall MJ, Brydon P et al (2004) Changes in plasma lipids and markers of oxidative stress in normal pregnancy and pregnancies complicated by diabetes. Clin Sci (Lond) 106(1):93–98. doi:10.1042/cs20030175
Hung TH, Lo LM, Chiu TH, Li MJ, Yeh YL, Chen SF et al (2010) A longitudinal study of oxidative stress and antioxidant status in women with uncomplicated pregnancies throughout gestation. Reprod Sci 17(4):401–409. doi:10.1177/1933719109359704
Garcia-Benavides L, Guzman-Sanchez A, Hernandez-Mora FJ, Muro-Gomez AM, Gomez-Martinez ML, Siller-Lopez FR (2012) PP078. Total antioxidant capacity in patients with pregnancy induced hypertension: its relation to maternal and/or perinatal complications. Pregnancy Hypertens. 2(3):282–283. doi:10.1016/j.preghy.2012.04.189
Christou K, Moulas AN, Pastaka C, Gourgoulianis KI (2003) Antioxidant capacity in obstructive sleep apnea patients. Sleep Med 4(3):225–228
Barcelo A, Miralles C, Barbe F, Vila M, Pons S, Agusti AG (2000) Abnormal lipid peroxidation in patients with sleep apnoea. Eur Respir J. 16(4):644–647
Dyugovskaya L, Lavie P, Lavie L (2002) Increased adhesion molecules expression and production of reactive oxygen species in leukocytes of sleep apnea patients. Am J Respir Crit Care Med 165(7):934–939
Tan KC, Chow WS, Lam JC, Lam B, Bucala R, Betteridge J et al (2006) Advanced glycation endproducts in nondiabetic patients with obstructive sleep apnea. Sleep 29(3):329–333
Lam JC, Tan KC, Lai AY, Lam DC, Ip MS (2012) Increased serum levels of advanced glycation end-products is associated with severity of sleep disordered breathing but not insulin sensitivity in non-diabetic men with obstructive sleep apnoea. Sleep Med 13(1):15–20. doi:10.1016/j.sleep.2011.07.015
Serebrovskaya TV, Swanson RJ, Kolesnikova EE (2003) Intermittent hypoxia: mechanisms of action and some applications to bronchial asthma treatment. J Physiol Pharmacol 54(Suppl 1):35–41
Cai Z, Manalo DJ, Wei G, Rodriguez ER, Fox-Talbot K, Lu H et al (2003) Hearts from rodents exposed to intermittent hypoxia or erythropoietin are protected against ischemia-reperfusion injury. Circulation 108(1):79–85. doi:10.1161/01.cir.0000078635.89229.8a
Paz Y, Mar HL, Hazen SL, Tracy RP, Strohl KP, Auckley D, Bena J et al (2016) Effect of continuous positive airway pressure on cardiovascular biomarkers: the sleep apnea stress randomized controlled trial. Chest 150(1):80–90. doi:10.1016/j.chest.2016.03.002
Duthie GG, Morrice PC, Ventresca PG, McLay JS Effects of storage, iron and time of day on indices of lipid peroxidation in plasma from healthy volunteers. Clin Chim Acta n206(3):207–213
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria, educational grants, participation in speakers’ bureaus, membership, employment, consultancies, stock ownership or other equity interest, and expert testimony or patent-licensing arrangements) or nonfinancial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript. GB received research equipment support from Respironics for a federally funded study; however, Respironics had no role in the current study.
Human and animal rights and informed consent
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants prospectively recruited into the study. Waiver of consent was obtained for the retrospective component of the study. Both were IRB approved.
Funding
GB received funding from NIH R01HL130702 and R01HD078515 and Perkins Charitable Foundation. The Perkins Foundation had no role in study design, conduct, interpretation, or submission of the manuscript.
Rights and permissions
About this article
Cite this article
Khan, N., Lambert-Messerlian, G., Monteiro, J.F. et al. Oxidative and carbonyl stress in pregnant women with obstructive sleep apnea. Sleep Breath 22, 233–240 (2018). https://doi.org/10.1007/s11325-017-1475-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1475-8