Abstract
Background
Previous studies have reported that selective serotonin reuptake inhibitors (SSRIs) might improve sleep-related breathing disorders (SRBDs). However, the effects of SSRIs on breathing are not evaluated in subjects without moderate-to-severe SRBDs. Further, many symptoms of depression and SRBDs overlap, and so, it is interesting whether there are interactions between breathing and psychopathologic symptoms during SSRI treatment for depression.
Methods
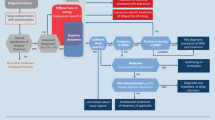
Data were taken from an open-label 8-week trial of sertraline in depressed patients with insomnia (n = 31). The depressed patients were administered 50 mg sertraline at 8 AM on the first day, and the dosage was subsequently titrated up to a maximum of 200 mg/day during the 8-week trial. All the patients were tested by repeated polysomnography (PSG) (baseline, 1st day, 14th day, 28th day, and 56th day). Sleep-disordered breathing events were categorized as apneas, hypopneas, and respiratory event-related arousals (RERAs).
Results
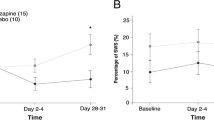
The clinical responses and PSG characteristics improved continuously during the 8-week trial. From the 14th day on, the RERA index during all-night and non-rapid eye movement (NREM) sleep became stable and significantly higher than baseline and the first day (RERA index 7.3 ± 2.2 at baseline, 7.3 ± 2.5 on the 1st day, 4.4 ± 1.9 on the 14th day, 3.9 ± 1.3 on the 28th day, 4.2 ± 2.0 on the 56th day, F = 5.71, P = 0.02; NREM-RERA index 6.2 ± 2.0 at baseline, 6.3 ± 2.3 on the 1st day, 3.2 ± 1.5 on the 14th day, 3.5 ± 0.9 on the 28th day, 3.2 ± 1.7 on the 56th day, F = 4.92, P = 0.03). Additionally, the NREM-apnea index showed a similar pattern to that of the RERA index and reached a significant difference between baseline (1.0 ± 0.5) and the 14th day (0.5 ± 0.4) (KW = 4.28, P = 0.047). Compared to the no-improvement group, the improvement group with a decreasing score rate of the respiratory disturbance index (RDI) greater than or equal to −50 % had a more positive decreasing score rate of slow wave sleep (SWS) (439.0 ± 78.2 vs 373.2 ± 77.9 %, T = 3.46, P = 0.04) and a more negative decreasing score rate on the arousal index (−43.7 ± 16.7 vs −26.6 ± 9.7 %, T = 9.16, P = 0.01), Pittsburgh Sleep Quality Index (PSQI) scores (−65.1 ± 33.7 vs −49.6 ± 21.4 %, T = 4.74, P = 0.05), and Epworth Sleepiness Scale (ESS) scores (−55.7 ± 21.3 vs −36.4 ± 17.5 %, T = 6.44, P = 0.02).
Discussion
This research indicates that SRBDs could be improved to some extent by sertraline treatment, which might be more common in patients with relatively more severe sleep-disordered breathing (e.g., RDI ≥ 10 in the current study). Although the sertraline-induced SRBD improvement seems not to have a significant clinical effect, the SRBD improvement group with decreasing score rate of RDI greater than or equal to −50 % has better subjective and objective sleep aspects than the no-improvement group. Thus, the fact that the SRBDs’ improvement was related to SSRIs might have a potential clinical benefit in the antidepressant treatment.


Similar content being viewed by others
References
Jordan AS, McSharry DG, Malhotra A (2014) Adult obstructive sleep apnoea. Lancet 383(9918):736–747
Zozula R, Rosen R (2001) Compliance with continuous positive airway pressure therapy: assessing and improving treatment outcomes. Curr Opin Pulm Med 7(6):391–398
Morgenthaler TI, Kapen S, Lee-Chiong T, Alessi C, Boehlecke B et al (2006) Practice parameters for the medical therapy of obstructive sleep apnea. Sleep 29(8):1031–1035
Behan M, Moeser AE, Thomas CF, Russell JA, Wang H et al (2012) The effect of tongue exercise on serotonergic input to the hypoglossal nucleus in young and old rats. J Speech Lang Hear Res 55(3):919–929
Kubin L, Tojima H, Davies RO, Pack AI (1992) Serotonergic excitatory drive to hypoglossal motoneurons in the decerebrate cat. Neurosci Lett 139(2):243–248
Carley DW, Radulovacki M (1999) Role of peripheral serotonin in the regulation of central sleep apneas in rats. Chest 115(5):1397–1401
Radulovacki M, Trbovic SM, Carley DW (1998) Serotonin 5-HT3-receptor antagonist GR 38032 F suppresses sleep apneas in rats. Sleep 21(2):131–136
Yue W, Liu H, Zhang J, Zhang X, Wang X et al (2008) Association study of serotonin transporter gene polymorphisms with obstructive sleep apnea syndrome in Chinese Han population. Sleep 31(11):1535–1541
Kraiczi H, Hedner J, Dahlof P, Ejnell H, Carlson J (1999) Effect of serotonin uptake inhibition on breathing during sleep and daytime symptoms in obstructive sleep apnea. Sleep 22(1):61–67
Hanzel DA, Proia NG, Hudgel DW (1991) Response of obstructive sleep apnea to fluoxetine and protriptyline. Chest 100(2):416–421
Berry RB, Yamaura EM, Gill K, Reist C (1999) Acute effects of paroxetine on genioglossus activity in obstructive sleep apnea. Sleep 22(8):1087–1092
Prasad B, Radulovacki M, Olopade C, Herdegen JJ, Logan T et al (2010) Prospective trial of efficacy and safety of ondansetron and fluoxetine in patients with obstructive sleep apnea syndrome. Sleep 33(7):982–989
Nieto FJ, Young TB, Lind BK, Shahar E, Samet JM et al (2000) Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. JAMA 283(14):1829–1836
Harris M, Glozier N, Ratnavadivel R, Grunstein RR (2009) Obstructive sleep apnea and depression. Sleep Med Rev 13(6):437–444
First MB SR, Williams JBW, Gibbon M, Williams JWB (1996) User's Guide for the Structured Clinical Interview for DSM-IV Axis I Disorders: SCID-II Clinician Version: American Psychiatric Association
Hamilton M (1960) A rating scale for depression. J Neurol Neurosurg Psychiatry 23:56–62
Guy W (1976) ECDEU assessment manual for psychopharmacology, revised. DEW, USA: Rockville, pp 341–350
Johns MW (1992) Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep 15(4):376–381
Buysse DJ, Reynolds CF 3rd, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28(2):193–213
Weidong Wang XW, Hong MA (1999) Handbook of mental health questionnaires. Chinese Mental Health Journal, Bei Jing
Kohler M, Stradling JR (2010) Mechanisms of vascular damage in obstructive sleep apnea. Nat Rev Cardiol 7(12):677–685
Zhang B, Hao Y, Jia F, Li X, Ren Y et al (2013) Sertraline and periodic limb movements during sleep: an 8-week open-label study in depressed patients with insomnia. Sleep Med 14(12):1405–1412
Iber C A-IS, Cheeson A, and Quan SF for the academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester, Illinois
Carskadon MA, Dement WC, Mitler MM, Roth T, Westbrook PR et al (1986) Guidelines for the multiple sleep latency test (MSLT): a standard measure of sleepiness. Sleep 9(4):519–524
Barnes NM, Sharp T (1999) A review of central 5-HT receptors and their function. Neuropharmacology 38(8):1083–1152
Veasey SC (2003) Serotonin agonists and antagonists in obstructive sleep apnea: therapeutic potential. Am J Respir Med 2(1):21–29
Heym J, Koe BK (1988) Pharmacology of sertraline: a review. J Clin Psychiatry; 49 Suppl: 40–5
Richmonds CR, Hudgel DW (1996) Hypoglossal and phrenic motoneuron responses to serotonergic active agents in rats. Respir Physiol 106(2):153–160
Veasey SC, Chachkes J, Fenik P, Hendricks JC (2001) The effects of ondansetron on sleep-disordered breathing in the English bulldog. Sleep 24(2):155–160
Veasey SC, Guilleminault C, Strohl KP, Sanders MH, Ballard RD et al (2006) Medical therapy for obstructive sleep apnea: a review by the Medical Therapy for Obstructive Sleep Apnea Task Force of the Standards of Practice Committee of the American Academy of Sleep Medicine. Sleep 29(8):1036–1044
Ratnavadivel R, Chau N, Stadler D, Yeo A, McEvoy RD et al (2009) Marked reduction in obstructive sleep apnea severity in slow wave sleep. J Clin Sleep Med 5(6):519–524
Sallanon M, Janin M, Buda C, Jouvet M (1983) Serotoninergic mechanisms and sleep rebound. Brain Res 268(1):95–104
Cartwright R, Baehr E, Kirkby J, Pandi-Perumal SR, Kabat J (2003) REM sleep reduction, mood regulation and remission in untreated depression. Psychiatry Res 121(2):159–167
Blackwell T, Yaffe K, Ancoli-Israel S, Redline S, Ensrud KE et al (2011) Associations between sleep architecture and sleep-disordered breathing and cognition in older community-dwelling men: the Osteoporotic Fractures in Men Sleep Study. J Am Geriatr Soc 59(12):2217–2225
Ondze B, Espa F, Dauvilliers Y, Billiard M, Besset A (2003) Sleep architecture, slow wave activity and sleep spindles in mild sleep disordered breathing. Clin Neurophysiol 114(5):867–874
Younes M (2004) Role of arousals in the pathogenesis of obstructive sleep apnea. Am J Respir Crit Care Med 169(5):623–633
Berry RB, Bonnet MH, Light RW (1992) Effect of ethanol on the arousal response to airway occlusion during sleep in normal subjects. Am Rev Respir Dis 145(2 Pt 1):445–452
Baglioni C, Battagliese G, Feige B, Spiegelhalder K, Nissen C et al (2011) Insomnia as a predictor of depression: a meta-analytic evaluation of longitudinal epidemiological studies. J Affect Disord 135(1–3):10–19
Burcusa SL, Iacono WG (2007) Risk for recurrence in depression. Clin Psychol Rev 27(8):959–985
Acknowledgments
The work was supported by the Investigator-Initiated Research (IIR) from Pfizer Pharma, (study code WS458774) to BZ and the Science and Technology Project Foundation of Science and Technology Department of Guangdong Province (grant no. 2013B021800045) to BZ. The other authors have nothing to disclose.
Conflict of interest
The authors have declared that no competing interests exist.
Author information
Authors and Affiliations
Corresponding author
Additional information
Clinical trial registry
An 8-week, open-label study to evaluate the effect of sertraline on the polysomnogram of depressed patients with insomnia (http://clinicaltrials.gov/ct2/show/NCT01032434). Registry identifier: NCT01032434
Bin Zhang and Yanli Hao contributed equally to this work.
Rights and permissions
About this article
Cite this article
Zhang, B., Hao, Y., Jia, F. et al. Effect of sertraline on breathing in depressed patients without moderate-to-severe sleep-related breathing disorders. Sleep Breath 19, 1377–1386 (2015). https://doi.org/10.1007/s11325-015-1152-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1152-8