Abstract
Purpose
Mandibular advancement splints (MAS) can effectively treat obstructive sleep apnea (OSA); however, treatment response is variable, and the mechanisms behind differences in treatment outcomes are still not well understood. The aims of this study were (1) to assess the effects of MAS on tongue shape and (2) to compare tongue shape changes with MAS between treatment responders and nonresponders.
Methods
Sixty-eight adults with symptomatic mild to severe OSA were included. A custom-made MAS was provided to patients, and treatment outcome was determined by polysomnography. Two-dimensional tongue measurements were evaluated using sagittal and axial MRI image slices without and with MAS in situ. Tongue measurements of height, length, width, area, and shape (height/length) were collected. Additional measurements of surrounding upper airway structures, soft palate length width and area and upper airway area, length and minimum width were measured on sagittal image slices.
Results
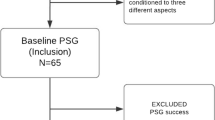
Based on polysomnography with MAS in situ, 47 patients were classified as responders (≥50 % reduction in apnea-hypopnea index [AHI] from baseline), and 21 were nonresponders (<50 % AHI reduction). There was no change in sagittal tongue area with insertion of MAS, although there was a change in most of parameters of tongue shape. Responders showed a greater decrease in tongue length with MAS in situ compared to nonresponders (−0.64 ± 0.46 vs −0.32 ± 0.51 cm, p = 0.016).
Conclusion
This study reports a detailed two-dimensional analysis of tongue dimensions as well as assessment of adjacentsoft palate shape and upper airway structures without and with MAS treatment for OSA. Our finding suggests that MAS does induce changes in tongue shape. MAS treatment responders showed a greater decrease in tongue length (between the tongue tip and hyoid bone) with MAS in situ; whether differences in alteration of tongue position with MAS explain differences in treatment response requires further investigation.



Similar content being viewed by others
References
American Academy of Sleep Medicine Task Force (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. Sleep 22:667–689
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014
Cistulli PA, Gotsopoulos H, Marklund M, Lowe AA (2004) Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances. Sleep Med Rev 8:443–457
Giles TL, Lasserson TJ, Smith BJ, White J, Wright J, Cates CJ (2006) Continuous positive airways pressure for obstructive sleep apnea in adults. Cochrane Database Syst Rev 25, CD001106
Hoffstein V (2007) Review of oral appliances for treatment of sleep-disordered breathing. Sleep Breath 11:1–22
Sutherland K, Cistulli P (2011) Mandibular advancement splints for the treatment of sleep apnea syndrome. Swiss Med Wkly 141:w13276. doi:10.4414/smw.2011.13276
Watanabe T, Isono S, Tanaka A, Tanzawa H, Nishino T (2002) Contribution of body habitus and craniofacial characteristics to segmental closing pressures of the passive pharynx in patients with sleep-disordered breathing. Am J Respir Crit Care Med 165:260–265
Mostafiz W, Dalci O, Sutherland K, Malhotra A, Srinivasan V, Darendeliler MA, Cistulli PA (2011) Influence of oral and craniofacial dimensions on mandibular advancement splint treatment outcome in patients with obstructive sleep apnea. Chest 139:1331–1339
Chan AS, Sutherland K, Schwab RJ, Zeng B, Petocz P, Lee RW, Darendeliler MA, Cistulli PA (2010) The effect of mandibular advancement on upper airway structure in obstructive sleep apnoea. Thorax 65:726–732
Almeida FR, Tsuiki S, Hattori Y, Takei Y, Inoue Y, Lowe AA (2011) Dose-dependent effects of mandibular protrusion on genioglossus activity in sleep apnoea. Eur Respir J 37:209–212
Johal A, Gill G, Ferman A, McLaughlin K (2007) The effect of mandibular advancement appliances on awake upper airway and masticatory muscle activity in patients with obstructive sleep apnoea. Clin Physiol Funct Imaging 27:47–53
Tsuiki S, Ono T, Kuroda T (2000) Mandibular advancement modulates respiratory-related genioglossus electromyographic activity. Sleep Breath 4:53–58
Shen HL, Wen YW, Chen NH, Liao YF (2012) Craniofacial morphologic predictors of oral appliance outcomes in patients with obstructive sleep apnea. J Am Dent Assoc 43:1209–1217
Poon KH, Chay SH, Chiong KF (2008) Airway and craniofacial changes with mandibular advancement device in Chinese with obstructive sleep apnoea. Ann Acad Med Singapore 37:637–644
Menn SJ, Loube DI, Morgan TD, Mitler MM, Berger JS, Erman MK (1996) The mandibular repositioning device: role in the treatment of obstructive sleep apnea. Sleep 9:794–800
Do KL, Ferreyra H, Healy JF, Davidson TM (2000) Does tongue size differ between patients with and without sleep-disoreded breathing? Laryngoscope 110:1552–1555
Lowe AA, Fleetham JA, Adachi S, Ryan CF (1995) Cephalometric and computed tomographic predictors of obstructive sleep apnea severity. Am J Orthod Dentofacial Orthop 107:589–595
Iida-Kondo C, Yoshino N, Kurabayashi T, Mataki S, Hasegawa M, Kurosaki N (2006) Comparison of tongue volume/oral cavity volume ratio between obstructive sleep apnea syndrome patients and normal adults using magnetic response imaging. J Med Dent Sci 53:119–126
Okubo M, Suzuki M, Horiuchi A et al (2006) Morphologic analyses of mandible and upper airway soft tissue by MRI of patients with obstructive sleep apnea hypopnea syndrome. Sleep 29:909–915
Pae EK, Lowe AA (1999) Tongue shape in obstructive sleep apnea patients. Angle Orthod 69:147–150
Zeng B, Ng AT, Darendeliler MA, Petocz P, Cistulli PA (2007) Use of flow-volume curves to predict oral appliance treatment outcome in obstructive sleep apnea. Am J Respir Crit Care Med 175:726–730
Zeng B, Ng AT, Qian J, Petocz P, Darendeliler MA, Cistulli PA (2008) Influence of nasal resistance on oral appliance treatment outcome in obstructive sleep apnea. Sleep 31:543–547
Kumar P, Parkash H, Bhargava A, Gupta S, Bagga DK (2013) Reliability of anatomic reference planes in establishing the occlusal plane in different jaw relationships: a cephalometric study. J Indian Prosthodont Soc 13:571–577
Furuhashi A, Yamada S, Shiomi T, Sasanabe R, Aoki Y, Yamada Y, Kazaoka Y (2013) Effective three-dimensional evaluation analysis of upper airway form during oral appliance therapy in patients with obstructive sleep apnoea. J Oral Rehabil 40:582–589
Kato T, Yamaguchi T, Okura K, Abe S, Lavigne GJ (2013) Sleep less and bite more: sleep disorders associated with occlusal loads during sleep. J Prosthodont Res 57:69–81
Pouderoux P, Kahrilas PJ (1995) Deglutitive tongue force modulation by volition, volume, and viscosity in humans. Gastroenterology 108:1418–1426
Liu ZJ, Shcherbatyy V, Perkins JA (2008) Functional loads of the tongue and consequences of volume reduction. J Oral Maxillofac Surg 66:1351–1361
Brown EC, Cheng S, McKenzie DK (2013) Tongue and lateral upper airway movement with mandibular advancement. Sleep 36:397–404
Kyung SH, Park YC, Pae EK (2005) Obstructive sleep apnea patients with the oral appliance experience pharyngeal size and shape changes in three dimensions. Angle Orthod 75:15–22
Choi JK, Hur YK, Lee JM, Clark GT (2010) Effects of mandibular advancement on upper airway dimension and collapsibility in patients with obstructive sleep apnea using dynamic upper airway imaging during sleep. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109:712–719
Acknowledgments
We would like to thank Dr Biao Zeng, Dr Jin Qian, Dr Andrew Ng, Dr Belinda Liu, and the sleep laboratory staff at St George and Royal North Shore Hospitals for their assistance, and Dr. Saeed Jafari from the Division of Orthodontic Dentistry, Tohoku University Graduate School of Dentistry for his support.
Funding
National Health and Medical Research Council of Australia. SomnoMed provided the oral appliances for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Toru Ogawa and Jianlan Long contributed equally to this work
Rights and permissions
About this article
Cite this article
Ogawa, T., Long, J., Sutherland, K. et al. Effect of mandibular advancement splint treatment on tongue shape in obstructive sleep apnea. Sleep Breath 19, 857–863 (2015). https://doi.org/10.1007/s11325-014-1101-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-014-1101-y