Abstract
Purpose
The recent scoring rules of the American Academy of Sleep Medicine (AASM) define hypoventilation in children as a carbon dioxide (CO2) level of >50 mmHg for >25 % of total sleep time (partial pressure of CO2 (PCO2) > 50[>25 %]). As there is no validated level of nocturnal hypoventilation with regard to end-organ damage in children, we evaluated the prevalence of hypoventilation with the AASM definition but also with a lesser degree of elevated CO2 in children with sleep-disordered breathing (SDB).
Methods
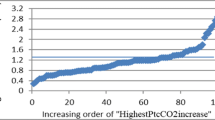
Transcutaneous CO2 (PtcCO2) was recorded during overnight polygraphy (PG). Hypoventilation was defined according to four definitions: the AASM score (PCO2 > 50[>25 %]), the peak value of PtcCO2 > 50 mmHg (PtcCO2 > 50[peak]), a percentage of PtcCO2 > 50 mmHg > 2 % of nighttime recording (PtcCO2 > 50[>2 %]) or a nocturnal PtcCO2 > 10 mmHg above waking baseline level (PtcCO2[>10 mmHg]). PtcCO2 indices were correlated to the apnoea–hypopnoea index (AHI) and oxygenation indices.
Results
PGs from 221 children with suspicion of obstructive sleep apnoea (72 %), neuromuscular diseases (21 %), and lung diseases (7 %) were analysed. The prevalence of hypoventilation according to PCO2 > 50[>25 %], PtcCO2 > 50[peak], PtcCO2 > 50[>2 %] and PtcCO2[>10 mmHg] were 16, 27, 31 and 52 %, respectively, and did not differ between the three diagnostic groups. Significant but weak correlations were observed between hypoventilation and AHI and oxygenation indices.
Conclusions
Nocturnal hypoventilation occurs in a large number of children referred for SDB, independent of the underlying disease, when more stringent criteria than those of the AASM are used. The poor correlation between hypoventilation and AHI or oxygenation indices is in favour of CO2 being a supplemental index of SDB.



Similar content being viewed by others
References
Marcus CL, Brooks LJ, Draper KA, Gozal D, Halbower AC, Jones J, Schechter MS, Ward SD, Sheldon SH, Shiffman RN, Lehmann C, Spruyt K, American Academy of Pediatrics (2012) Diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 130:e714–e755
Arens R, Marcus CL (2004) Pathophysiology of upper airway obstruction: a developmental perspective. Sleep 27:997–1019
American Thoracic Society (1996) Standards and indications for cardiopulmonary sleep studies in children. Am J Respir Crit Care Med 153:866–878
AASM (2005) International classification of sleep disorders: diagnostic and coding manual. American Academy of Sleep Medicine, Westchester
Polat M, Sakinci O, Ersoy B, Sezer RG, Yilmaz H (2012) Assessment of sleep-related breathing disorders in patients with duchenne muscular dystrophy. J Clin Med Res 4:332–337
Iber C, Ancoli-Israel S, Chesson AL, Quan SF, American Academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated events. American Academy of Sleep Medicine, Westchester
Beck SE, Marcus CL (2009) Pediatric polysomnography. Sleep Med Clin 4:393–406
Grigg-Damberger MM (2012) The AASM scoring manual four years later. J Clin Sleep Med 8:323–332
Marcus CL, Omlin KJ, Basinski DJ, Bailey SL, Rachal AB, Von Pechmann WS, Keens TG, Davidson-Ward SL (1992) Normal polysomnographic values for children and adolescents. Am Rev Respir Dis 146:1235–1239
Montgomery-Downs HE, O’Brien LM, Gulliver TE, Gozal D (2006) Polysomnographic characteristics in normal preschool and early school-aged children. Pediatrics 117:741–753
Kirk VG, Batuyong ED, Bohn SG (2006) Transcutaneous carbon dioxide monitoring and capnography during pediatric polysomnography. Sleep 29:1601–1608
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep Medicine (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the sleep apnea definitions task force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Uliel S, Tauman R, Greenfeld M, Sivan Y (2004) Normal polysomnographic respiratory values in children and adolescents. Chest 125:872–878
Sans Capdevila O, Kheirandish-Gozal L, Dayyat E, Gozal D (2008) Pediatric obstructive sleep apnea. Complications, management, and long-term outcomes. Proc Am Thorac Soc 5:274–282
Witmans MB, Keens TG, Davidson Ward SL, Marcus CL (2003) Obstructive hypopneas in children and adolescents: normal values. Am J Respir Crit Care Med 168:1540
de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J (2007) Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ 85:660–667
Ward S, Chatwin M, Heather S, Simonds AK (2005) Randomised controlled trial of non-invasive ventilation (NIV) for nocturnal hypoventilation in neuromuscular and chest wall disease patients with daytime normocapnia. Thorax 60:1019–1024
Paiva R, Krivec U, Aubertin G, Cohen E, Clément A, Fauroux B (2009) Carbon dioxide monitoring during long-term noninvasive respiratory support in children. Intensive Care Med 35:1068–1074
O’Donoghue FJ, Catcheside PG, Ellis EE, Grunstein RR, Pierce RJ, Rowland LS, Collins ER, Rochford SE, McEvoy RD, Australian trial of Noninvasive Ventilation in Chronic Airflow Limitation investigators (2003) Sleep hypoventilation in hypercapnic chronic obstructive pulmonary disease: prevalence and associated factors. Eur Respir J 21:977–984
Morielli A, Desjardins D, Brouillette RT (1993) Transcutaneous and end-tidal carbon dioxide pressures should be measured during pediatric polysomnography. Am Rev Respir Dis 148:1599–1604
Acknowledgments
The research of Brigitte Fauroux is supported by the Association Française contre les Myopathies (AFM); ADEP Assistance, S2A Santé, Vaincre la Mucoviscidose (VLM); Assistance Publique-Hôpitaux de Paris, Inserm and Université Pierre et Marie Curie-Paris6.
Conflict of interest
None of the authors has any conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pautrat, J., Khirani, S., Boulé, M. et al. Carbon dioxide levels during polygraphy in children with sleep-disordered breathing. Sleep Breath 19, 149–157 (2015). https://doi.org/10.1007/s11325-014-0980-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-014-0980-2