Abstract
Background
Airborne particulate matter may induce health risk with inhalation. Special concerns exist for deployed military personnel with inhaled particulate matter in desert environments. Continuous positive airway pressure (CPAP) used in obstructive sleep apnea may facilitate inhalation of particulate matter. We evaluated the ability of commercial CPAP filter systems to eliminate inhalation of particulate matter.
Methods
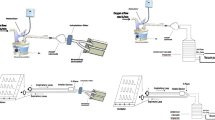
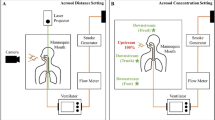
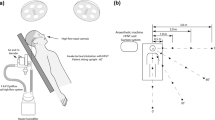
An ultrasonic medical nebulizer (DeVilbliss Ultraneb, DeVilbliss, Somerset, PA) atomized liquid producing “respirable” aerosol. Technetium-99m diethylene triamine pentaacetic acid dissolved in water was also aerosolized to quantify aerosol inhalation. A high efficiency particulate air (HEPA) filter placed at the patient–hose connection port in the bilevel positive airway pressure (BPAP) device captured the aerosol inbound to the patient. The HEPA filter provided a means to quantify aerosol dose delivered to a simulated patient. Commercial foam and ultrafine filters were assessed with aerosol to determine the simulated patient exposure.
Results
Foam and ultrafine filters used together allowed 1.5% or less of aerosol volume to pass through the BPAP system. Foam filters alone allowed an average of 18.9% of aerosol delivered to pass through the BPAP system.
Conclusions
Foam and ultrafine filters used together in BPAP systems provide excellent aerosol filtration in this laboratory simulation of BPAP use.


Similar content being viewed by others
References
National heart, lung, and blood institute. Who is at risk for sleep apnea? September 16, 2010 http://www.nhlbi.nih.gov/health/dci/Diseases/SleepApnea/SleepApnea_WhoIsAtRisk.html. accessed.
Doherty DE MB (2006) Education review manual in pulmonary disease, 2nd edn. Castle Connolly Graduate Medical Publishing, Ltd, New York
Babin S, Burkom H, Holtry R, Tabernero N, Davies-Cole J, Stokes L, Dehaan K, Lee D (2008) Medicaid patient asthma-related acute care visits and their associations with ozone and particulates in Washington, DC, from 1994-2005. Int J Environ Health Res 18(3):209–221
Dominici F, Peng RD, Bell ML, Pham L, McDermott A, Zeger SL, Samet JM (2006) Fine particulate air pollution and hospital admission for cardiovascular and respiratory diseases. Jama 295(10):1127–1134
Simkhovich BZ, Kleinman MT, Kloner RA (2008) Air pollution and cardiovascular injury epidemiology, toxicology, and mechanisms. J Am Coll Cardiol 52(9):719–726
Heyder J, Gebhardt J, Rudolf G, Schiller CF, Stahlhofen W (1986) Deposition of particles in the human respiratory tract in the size range of 0.005–15 μm. J Aerosol Sci 17(5):811–825
Jiang R, Bell ML (2008) A comparison of particulate matter from biomass-burning rural and non-biomass-burning urban households in northeastern China. Environ Health Perspect 116(7):907–914
Abu-Allaban M, Gillies JA, Gertler AW, Clayton R, Proffitt D (2007) Motor vehicle contributions to ambient PM10 and PM2.5 at selected urban areas in the USA. Environ Monit Assess 132(1-3):155–163
Eftim SE, Samet JM, Janes H, McDermott A, Dominici F (2008) Fine particulate matter and mortality: a comparison of the six cities and American Cancer Society cohorts with a medicare cohort. Epidemiology 19(2):209–216
Lipsett MJ, F T, Roger L, Woo M, Ostro BD (2006) Coarse particles and heart rate variability among older adults with coronary artery disease in the Coachella Valley, California. Environ Health Perspect 114:1215–1220
Draxler RR, Dale GA, Kirkpatrick JS, Heller J (2001) Estimating PM10 air concentrations from dust storms in Iraq, Kuwait, and Saudi Arabia. Atmos Environ 35:4315–4330
Polymenakou PN, Mandalakis M, Stephanou EG, Tselepides A (2008) Particle size distribution of airborne microorganisms and pathogens during an intense African dust event in the Eastern Mediterranean. Environ Health Perspect 116:292–296
McDonald E, Todd C (2004) Geochemical and physical characteristics of Iraqi dust and soil samples. Desert Research Institute, Yuma Proving Ground
Corcoran TE, Venkataramanan R, Mihelc KM, Marcinkowski AL, Ou J, McCook BM, Weber L, Carey ME, Paterson DL, Pilewski JM, McCurry KR, Husain S (2006) Aerosol deposition of lipid complex amphotericin-B (Abelcet) in lung transplant recipients. Am J Transplant 6(11):2765–2773
British Standards Institution 1969. BS4400—Method for sodium chloride particulate test for respirator filters.
Acknowledgement
This research was supported financially by United States Air Force School of Aerospace Medicine (USAFSAM).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kristo, D., Corcoran, T., O’Connell, N. et al. The potential for delivery of particulate matter through positive airway pressure devices (CPAP/BPAP). Sleep Breath 16, 193–198 (2012). https://doi.org/10.1007/s11325-010-0475-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-010-0475-8