Abstract
Rationale
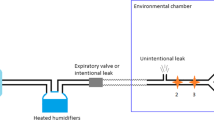
Water condensate in the humidifier tubing can affect bi-level ventilation by narrowing tube diameter and increasing airflow resistance. We investigated room temperature and tubing type as ways to reduce condensate and its effect on bi-level triggering and pressure delivery. In this bench study, the aim was to test the hypothesis that a relationship exists between room temperature and tubing condensate.
Methods
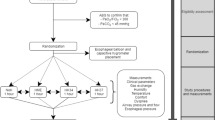
Using a patient simulator, a Res-med bi-level device was set to 18/8 cm H2O and run for 6 h at room temperatures of 16°C, 18°C and 20°C. The built-in humidifier was set to a low, medium or high setting while using unheated or insulated tubing or replaced with a humidifier using heated tubing. Humidifier output, condensate, mask pressure and triggering delay of the bi-level were measured at 1 and 6 h using an infrared hygrometer, metric weights, Honeywell pressure transducer and TSI pneumotach.
Results
When humidity output exceeded 17.5 mg H2O/L, inspiratory pressure fell by 2–15 cm H2O and triggering was delayed by 0.2–0.9 s. Heating the tubing avoided any such ventilatory effect whereas warmer room temperatures or insulating the tubing were of marginal benefit.
Conclusions
Users of bi-level ventilators need to be aware of this problem and its solution. Bi-level humidifier tubing may need to be heated to ensure correct humidification, pressure delivery and triggering.



Similar content being viewed by others
References
British Thoracic Society Standards of Care Committee (2002) Non-invasive ventilation in acute respiratory failure. Thorax 57(3):192–211
Massie CA, Hart RW, Peralez K, Richards GN (1999) Effects of humidification on nasal symptoms and compliance in sleep apnea patients using continuous positive airway pressure. Chest 116(2):403–408
Nishida T, Nishimura M, Fujino Y, Mashimo T (2001) Performance of heated humidifiers with a heated wire according to ventilatory settings. J Aerosol Med 14(1):43–51
Wiest GH, Fuchs FS, Brueckl WM, Nusko G, Harsch IA, Hahn EG, Ficker JH (2000) In vivo efficacy of heated and non-heated humidifiers during nasal continuous positive airway pressure (nCPAP)-therapy for obstructive sleep apnoea. Respir Med 94(4):364–368
Bacon JP, Farney RJ, Jensen RL, Walker JM, Cloward TV (2000) Nasal continuous positive airway pressure devices do not maintain the set pressure dynamically when tested under simulated clinical conditions. Chest 118:1441–1449
Louis B, Leroux K, Boucherie M, Isabey D, Grillier-Lanoir V, Fauroux B, Lofaso F (2010) Pressure stability with CPAP devices: a bench evaluation. Sleep Medicine 11
Nilius G, Domansk U, Franke KJ, Ruhle KH (2008) Impact of a controlled heated breathing tube humidifier on sleep quality during CPAP therapy in a cool sleeping environment. Eur Respir J 31:830–836
Miyao H, Hirokawa T, Miyasaka K, Kawazoe T (1992) Relative humidity, not absolute humidity, is of great importance when using a humidifier with a heating wire. Crit Care Med 20(5):674–679
Holland AE, Denehy L, Buchan CA, Wilson JW (2007) Efficacy of a heated passover humidifier during noninvasive ventilation: a bench study. Respiratory Care 52 NO 1
Gilmour IJ, Boyle MJ, Rozenberg A, Palahniuk RJ (1994) The effect of heated wire circuits on humidification of inspired gases. Anesth Analg 79(1):160–164
Mador MJ, Krauza M, Pervez A, Pierce D, Braun M (2005) Effect of heated humidification on compliance and quality of life in patients with sleep apnea using nasal continuous positive airway pressure. Chest 128:2151–2158
Krachman SL, Quaranta AJ, Berger TJ, Criner GJ (1997) Effects of noninvasive positive pressure ventilation on gas exchange and sleep in COPD patients. Chest 112:623–628
Ozsacak A, D’Ambrosio C, Hill NS (2008) Nocturnal noninvasive ventilation. Chest 133:1275–1286
Howden-Chapman P, Viggers H, Chapman R, O'Dea D, Free S, O'Sullivan K (2009) Warm homes: drivers of the demand for heating in the residential sector in New Zealand. Energy Policy:3387-3399
Conflict of Interest
Diana Hart received travel funding from Fisher & Paykel Healthcare.
Author information
Authors and Affiliations
Corresponding author
Additional information
Clinical Trial Registration number N/A
The study was sponsored by Fisher & Paykel Healthcare
Diana E Hart received travel funding from Fisher & Paykel.
Rights and permissions
About this article
Cite this article
Hart, D.E., Forman, M. & Veale, A.G. Effect of tubing condensate on non-invasive positive pressure ventilators tested under simulated clinical conditions. Sleep Breath 15, 535–541 (2011). https://doi.org/10.1007/s11325-010-0397-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-010-0397-5