Abstract
Cutaneous melanoma is a complex pathology that still has only treatments that lack efficiency and offer many adverse effects. Due to this scenario emerges the need to analyze other possible treatments against this disease, such as the effect of phenolic compounds. These substances have proven antitumor effects, but still have not been fully explored as a form of therapy to combat melanoma. Also, the purinergic receptors, along with its system molecules, take part in the formation of tumors from many pathways, such as the actions of ectoenzymes and receptors activity, especially P2Rs family, and are formed by structures that can be modulated by the phenolic compounds. Therefore, more studies have to be made with the aim of explaining the purinergic system activity in carcinogenesis of cutaneous melanoma and the effects of its modulation by phenolic compound, in order to enable the development of new therapies to combat this aggressive and feared cancer.
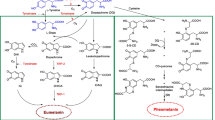
Graphical Abstract




Similar content being viewed by others
Data Availability
Not applicable.
Abbreviations
- Ado :
-
Adenosine
- ADP :
-
Adenosine diphosphate
- AMP :
-
Adenosine monophosphate
- ATP :
-
Adenosine triphosphate
- Ang-2 :
-
Angiopoietin-2
- CA :
-
Caffeic acid
- CM :
-
Cutaneous melanoma
- COX-2 :
-
Cyclooxygenase 2
- Enos :
-
Endothelial nitric oxide synthase
- EMT :
-
Epithelial-mesenchymal transition
- bFGF :
-
Fibroblastic growth factor
- HB-EGF :
-
Heparin-binding EGF-like growth factor
- HBV :
-
Hepatitis B virus
- HBx :
-
Hepatitis B x protein
- HIF :
-
Hypoxia induction factor
- ELISA :
-
Immunoenzymatic assay
- IME :
-
Inflammatory microenvironment
- IFN :
-
Interferon
- IL :
-
Interleukin
- M-CSF :
-
Macrophage colony-stimulating factor
- MDI :
-
Macrophage colony-stimulating factor, dexamethasone, and IL-4
- mRNA :
-
Messenger RNA
- miRNAs :
-
MicroRNAs
- MEK :
-
Mitogen-Activated Protein Kinase
- BRAF :
-
Murine Viral Sarcoma
- NK :
-
Natural killer
- NRas :
-
Neuroblastoma Viral Oncogene
- PDGF :
-
Platelet-derived growth factor
- P2R :
-
P2 receptors
- P2XR :
-
P2X receptors
- P2X7R :
-
P2X7 receptor
- P2YR :
-
P2Y receptors
- P2Y11R :
-
P2Y11 receptor
- P2Y12R :
-
P2Y12 receptor
- ROS :
-
Reactive oxygen species
- RTK :
-
Receptor tyrosine kinase
- RA :
-
Rosmarinic acid
- Th17 :
-
T helper lymphocytes type 17
- Treg :
-
T regulator lymphocytes
- TGF :
-
Transforming growth factor
- TILs :
-
Tumor infiltrating in T cells
- TME :
-
Tumor microenvironment
- TNF :
-
Tumor necrosis factor
- UDP :
-
Uridine diphosphate
- UTP :
-
Uridine triphosphate
- UV :
-
Ultraviolet
- VEGF :
-
Vascular endothelial growth factor
References
Lopes A, Chammas R, Iyeyasu H (2013) Oncologia para a graduação. Lemar, São Paulo
Leonardi G, Falzone L, Salemi R, Zangh� A, Spandidos D, Mccubrey J, et al. Cutaneous melanoma: from pathogenesis to therapy (Review). Int J Oncol 2018. https://doi.org/10.3892/ijo.2018.4287
Garbe C, Amaral T, Peris K, Hauschild A, Arenberger P, Basset-Seguin N et al (2022) European consensus-based interdisciplinary guideline for melanoma. Part 1: diagnostics: Update 2022. Eur J Cancer 170:236–55. https://doi.org/10.1016/j.ejca.2022.03.008
da Silva GB, Yamauchi MA, Zanini D, Bagatini MD (2022) Novel possibility for cutaneous melanoma treatment by means of rosmarinic acid action on purinergic signaling. Purinergic Signal 18:61–81. https://doi.org/10.1007/s11302-021-09821-7
Baloghová J, Michalková R, Baranová Z, Mojžišová G, Fedáková Z, Mojžiš J (2023) Spice-derived phenolic compounds: potential for skin cancer prevention and therapy. Molecules 28:6251. https://doi.org/10.3390/molecules28176251
Murai T, Matsuda S (2023) The chemopreventive effects of chlorogenic acids, phenolic compounds in coffee, against inflammation, cancer, and neurological diseases. Molecules 28:2381. https://doi.org/10.3390/molecules28052381
Mahmoud MA, Okda TM, Omran GA, Abd-Alhaseeb MM (2021) Rosmarinic acid suppresses inflammation, angiogenesis, and improves paclitaxel induced apoptosis in a breast cancer model via NF3 κB-p53-caspase-3 pathways modulation. J Appl Biomed 19:202–9. https://doi.org/10.32725/jab.2021.024
Messeha SS, Zarmouh NO, Asiri A, Soliman KFA (2020) Rosmarinic acid-induced apoptosis and cell cycle arrest in triple-negative breast cancer cells. Eur J Pharmacol 885:173419. https://doi.org/10.1016/j.ejphar.2020.173419
Abdelwahab T, Abdelhamed R, Ali E, Mansour N, Abdalla M (2021) Evaluation of silver nanoparticles caffeic acid complex compound as new potential therapeutic agent against cancer incidence in mice. Asian Pacific J Cancer Prev 22:3189–201. https://doi.org/10.31557/APJCP.2021.22.10.3189
Tseng J-C, Wang B-J, Wang Y-P, Kuo Y-Y, Chen J-K, Hour T-C et al (2023) Caffeic acid phenethyl ester suppresses EGFR/FAK/Akt signaling, migration, and tumor growth of prostate cancer cells. Phytomedicine 116:154860. https://doi.org/10.1016/j.phymed.2023.154860
Chen C, Kuo Y-H, Lin C-C, Chao C-Y, Pai M-H, Chiang EPI et al (2020) Decyl caffeic acid inhibits the proliferation of colorectal cancer cells in an autophagy-dependent manner in vitro and in vivo. PLoS One 15:e0232832. https://doi.org/10.1371/journal.pone.0232832
Caetano AR, Oliveira RD, Celeiro SP, Freitas AS, Cardoso SM, Gonçalves MST et al (2023) Phenolic compounds contribution to portuguese propolis anti-melanoma activity. Molecules 28:3107. https://doi.org/10.3390/molecules28073107
Kichina JV, Maslov A, Kandel ES (2023) PAK1 and therapy resistance in melanoma. Cells 12:2373. https://doi.org/10.3390/cells12192373
Kepp O, Bezu L, Yamazaki T, Di Virgilio F, Smyth MJ, Kroemer G, et al. ATP and cancer immunosurveillance. EMBO J 2021;40. https://doi.org/10.15252/embj.2021108130.
Vultaggio-Poma V, Falzoni S, Salvi G, Giuliani AL, Di Virgilio F (2022) Signalling by extracellular nucleotides in health and disease. Biochimica et Biophysica Acta (BBA) Mol Cell Res 1869:119237. https://doi.org/10.1016/j.bbamcr.2022.119237
Savio LEB, Leite-Aguiar R, Alves VS, Coutinho-Silva R, Wyse ATS (2021) Purinergic signaling in the modulation of redox biology. Redox Biol 47:102137. https://doi.org/10.1016/j.redox.2021.102137
Nakamura H, Takada K (2021) Reactive oxygen species in cancer: current findings and future directions. Cancer Sci 112:3945–3952. https://doi.org/10.1111/cas.15068
da Silva JLG, Viana AR, Passos DF, Krause LMF, Miron VV, Schetinger MRC et al (2023) Istradefylline modulates purinergic enzymes and reduces malignancy-associated factors in B16F10 melanoma cells. Purinergic Signal 19:633–650. https://doi.org/10.1007/s11302-022-09909-8
Ijaz S, Iqbal J, Abbasi BA, Ullah Z, Yaseen T, Kanwal S et al (2023) Rosmarinic acid and its derivatives: current insights on anticancer potential and other biomedical applications. Biomed Pharmacother 162:114687. https://doi.org/10.1016/j.biopha.2023.114687
Azhar MDK, Anwar S, Hasan GM, Shamsi A, Islam A, Parvez S et al (2023) Comprehensive insights into biological roles of rosmarinic acid: implications in diabetes, cancer and neurodegenerative diseases. Nutrients 15:4297. https://doi.org/10.3390/nu15194297
Osakabe N (2003) Rosmarinic acid inhibits epidermal inflammatory responses: anticarcinogenic effect of Perilla frutescens extract in the murine two-stage skin model. Carcinogenesis 25:549–557. https://doi.org/10.1093/carcin/bgh034
Huang L, Chen J, Quan J, Xiang D (2021) Rosmarinic acid inhibits proliferation and migration, promotes apoptosis and enhances cisplatin sensitivity of melanoma cells through inhibiting ADAM17/EGFR/AKT/GSK3β axis. Bioengineered 12:3065–3076. https://doi.org/10.1080/21655979.2021.1941699
Di Virgilio F, Dal Ben D, Sarti AC, Giuliani AL, Falzoni S (2017) The P2X7 receptor in infection and inflammation. Immunity 47:15–31. https://doi.org/10.1016/j.immuni.2017.06.020
Strassheim D, Verin A, Batori R, Nijmeh H, Burns N, Kovacs-Kasa A et al (2020) P2Y purinergic receptors, endothelial dysfunction, and cardiovascular diseases. Int J Mol Sci 21:6855. https://doi.org/10.3390/ijms21186855
Alam M, Ahmed S, Elasbali AM, Adnan M, Alam S, Hassan MdI, et al. Therapeutic implications of caffeic acid in cancer and neurological diseases. Front Oncol 2022;12. https://doi.org/10.3389/fonc.2022.860508.
Kudugunti SK, Vad NM, Whiteside AJ, Naik BU, Yusuf MohdA, Srivenugopal KS et al (2010) Biochemical mechanism of caffeic acid phenylethyl ester (CAPE) selective toxicity towards melanoma cell lines. Chem Biol Interact 188:1–14. https://doi.org/10.1016/j.cbi.2010.05.018
Pelinson LP, Assmann CE, Palma TV, da Cruz IBM, Pillat MM, Mânica A et al (2019) Antiproliferative and apoptotic effects of caffeic acid on SK-Mel-28 human melanoma cancer cells. Mol Biol Rep 46:2085–2092. https://doi.org/10.1007/s11033-019-04658-1
Kimsa-Dudek M, Synowiec-Wojtarowicz A, Krawczyk A, Kosowska A, Kimsa-Furdzik M, Francuz T (2022) The apoptotic effect of caffeic or chlorogenic acid on the C32 cells that have simultaneously been exposed to a static magnetic field. Int J Mol Sci 23:3859. https://doi.org/10.3390/ijms23073859
Anwar J, Spanevello RM, Pimentel VC, Gutierres J, Thomé G, Cardoso A et al (2013) Caffeic acid treatment alters the extracellular adenine nucleotide hydrolysis in platelets and lymphocytes of adult rats. Food Chem Toxicol 56:459–466. https://doi.org/10.1016/j.fct.2013.02.030
Tao DL, Tassi Yunga S, Williams CD, McCarty OJT (2021) Aspirin and antiplatelet treatments in cancer. Blood 137:3201–3211. https://doi.org/10.1182/blood.2019003977
Castro MFV, Stefanello N, Assmann CE, Baldissarelli J, Bagatini MD, da Silva AD et al (2021) Modulatory effects of caffeic acid on purinergic and cholinergic systems and oxi-inflammatory parameters of streptozotocin-induced diabetic rats. Life Sci 277:119421. https://doi.org/10.1016/j.lfs.2021.119421
Valdespino-Gómez VM, Valdespino-Castillo PM, Valdespino-Castillo VE (2015) Interacción de las vías de señalización intracelulares participantes en la proliferación celular: potencial blanco de intervencionismo terapéutico. Cir Cir 83:165–174. https://doi.org/10.1016/j.circir.2015.04.015
Pegoraro A, De Marchi E, Ferracin M, Orioli E, Zanoni M, Bassi C et al (2021) P2X7 promotes metastatic spreading and triggers release of miRNA-containing exosomes and microvesicles from melanoma cells. Cell Death Dis 12:1088. https://doi.org/10.1038/s41419-021-04378-0
Lara R, Adinolfi E, Harwood CA, Philpott M, Barden JA, Di Virgilio F, et al. P2X7 in cancer: from molecular mechanisms to therapeutics. Front Pharmacol 2020;11. https://doi.org/10.3389/fphar.2020.00793.
De Marchi E, Orioli E, Pegoraro A, Sangaletti S, Portararo P, Curti A et al (2019) The P2X7 receptor modulates immune cells infiltration, ectonucleotidases expression and extracellular ATP levels in the tumor microenvironment. Oncogene 38:3636–3650. https://doi.org/10.1038/s41388-019-0684-y
Chen L, Heikkinen L, Wang C, Yang Y, Sun H, Wong G (2019) Trends in the development of miRNA bioinformatics tools. Brief Bioinform 20:1836–1852. https://doi.org/10.1093/bib/bby054
Tucci M, Mannavola F, Passarelli A, Stucci LS, Cives M, Silvestris F (2018) Exosomes in melanoma: a role in tumor progression, metastasis and impaired immune system activity. Oncotarget 9:20826–37. https://doi.org/10.18632/oncotarget.24846
Rotondo JC, Mazziotta C, Lanzillotti C, Stefani C, Badiale G, Campione G et al (2022) The role of purinergic P2X7 receptor in inflammation and cancer: novel molecular insights and clinical applications. Cancers (Basel) 14:1116. https://doi.org/10.3390/cancers14051116
Savio LEB, de Andrade Mello P, da Silva CG, Coutinho-Silva R. The P2X7 receptor in inflammatory diseases: angel or demon? Front Pharmacol 2018;9. https://doi.org/10.3389/fphar.2018.00052.
Romagnani A, Rottoli E, Mazza EMC, Rezzonico-Jost T, De Ponte CB, Proietti M et al (2020) P2X7 receptor activity limits accumulation of T cells within tumors. Cancer Res 80:3906–3919. https://doi.org/10.1158/0008-5472.CAN-19-3807
Lei C, Fan Y, Peng X, Gong X, Shao L (2019) P2Y11R regulates cytotoxicity of HBV X protein (HBx) in human normal hepatocytes. Am J Transl Res 11:2765–2774
Yang C, Lei L, Collins JWM, Briones M, Ma L, Sturdevant GL et al (2021) Chlamydia evasion of neutrophil host defense results in NLRP3 dependent myeloid-mediated sterile inflammation through the purinergic P2X7 receptor. Nat Commun 12:5454. https://doi.org/10.1038/s41467-021-25749-3
Snelgrove RJ, Gregory LG, Peiró T, Akthar S, Campbell GA, Walker SA et al (2014) Alternaria-derived serine protease activity drives IL-33–mediated asthma exacerbations. J Allergy Clin Immunol 134:583-592.e6. https://doi.org/10.1016/j.jaci.2014.02.002
Quan J-H, Huang R, Wang Z, Huang S, Choi I-W, Zhou Y et al (2018) P2X7 receptor mediates NLRP3-dependent IL-1β secretion and parasite proliferation in Toxoplasma gondii-infected human small intestinal epithelial cells. Parasit Vectors 11:1. https://doi.org/10.1186/s13071-017-2573-y
Kloss L, Dollt C, Schledzewski K, Krewer A, Melchers S, Manta C et al (2019) ADP secreted by dying melanoma cells mediates chemotaxis and chemokine secretion of macrophages via the purinergic receptor P2Y12. Cell Death Dis 10:760. https://doi.org/10.1038/s41419-019-2010-6
Malavasi F, Deaglio S, Funaro A, Ferrero E, Horenstein AL, Ortolan E et al (2008) Evolution and function of the ADP ribosyl cyclase/CD38 gene family in physiology and pathology. Physiol Rev 88:841–886. https://doi.org/10.1152/physrev.00035.2007
Morandi F, Morandi B, Horenstein AL, Chillemi A, Quarona V, Zaccarello G et al (2015) A non-canonical adenosinergic pathway led by CD38 in human melanoma cells induces suppression of T cell proliferation. Oncotarget 6:25602–18. https://doi.org/10.18632/oncotarget.4693
Chen L, Diao L, Yang Y, Yi X, Rodriguez BL, Li Y et al (2018) CD38-mediated immunosuppression as a mechanism of tumor cell escape from PD-1/PD-L1 blockade. Cancer Discov 8:1156–1175. https://doi.org/10.1158/2159-8290.CD-17-1033
Moesta AK, Li X-Y, Smyth MJ (2020) Targeting CD39 in cancer. Nat Rev Immunol 20:739–755. https://doi.org/10.1038/s41577-020-0376-4
Timperi E, Barnaba V (2021) CD39 regulation and functions in T cells. Int J Mol Sci 22:8068. https://doi.org/10.3390/ijms22158068
Noble A, Mehta H, Lovell A, Papaioannou E, Fairbanks L (2016) IL-12 and IL-4 activate a CD39-dependent intrinsic peripheral tolerance mechanism in CD8 + T cells. Eur J Immunol 46:1438–1448. https://doi.org/10.1002/eji.201545939
Bastid J, Regairaz A, Bonnefoy N, Déjou C, Giustiniani J, Laheurte C et al (2015) Inhibition of CD39 enzymatic function at the surface of tumor cells alleviates their immunosuppressive activity. Cancer Immunol Res 3:254–265. https://doi.org/10.1158/2326-6066.CIR-14-0018
Simoni Y, Becht E, Fehlings M, Loh CY, Koo S-L, Teng KWW et al (2018) Bystander CD8+ T cells are abundant and phenotypically distinct in human tumour infiltrates. Nature 557:575–579. https://doi.org/10.1038/s41586-018-0130-2
Young A, Ngiow SF, Barkauskas DS, Sult E, Hay C, Blake SJ et al (2016) Co-inhibition of CD73 and A2AR adenosine signaling improves anti-tumor immune responses. Cancer Cell 30:391–403. https://doi.org/10.1016/j.ccell.2016.06.025
Chen S, Akdemir I, Fan J, Linden J, Zhang B, Cekic C (2020) The expression of adenosine A2B receptor on antigen-presenting cells suppresses CD8+ T-cell responses and promotes tumor growth. Cancer Immunol Res 8:1064–1074. https://doi.org/10.1158/2326-6066.CIR-19-0833
Ohta A, Gorelik E, Prasad SJ, Ronchese F, Lukashev D, Wong MKK et al (2006) A2A adenosine receptor protects tumors from antitumor T cells. Proc Natl Acad Sci 103:13132–13137. https://doi.org/10.1073/pnas.0605251103
JanhoDitHreich S, Benzaquen J, Hofman P, Vouret-Craviari V (2021) To inhibit or to boost the ATP/P2RX7 pathway to fight cancer—that is the question. Purinergic Signal 17:619–31. https://doi.org/10.1007/s11302-021-09811-9
Gan P, Liu C, Wu H, Dong Xin-Tong, Ke J, Chen F (2021) The role of HIF-VEGF-Ang-2 signal transduction-mediated synovial angiogenesis in rheumatoid arthritis / 药学学报. Acta Pharmaceutica Sinica 12:1246–52
Tammela T, Enholm B, Alitalo K, Paavonen K (2005) The biology of vascular endothelial growth factors. Cardiovasc Res 65:550–563. https://doi.org/10.1016/j.cardiores.2004.12.002
Romagnoli GG (2007) Fatores de crescimento e citocinas envolvidos na angiogênese de melanoma em animais selecionados pela intensidade da resposta inflamatória aguda. Dissertation, Universidade Estadual Paulista (UNESP)
Acknowledgements
GCB is grateful to the Federal University of Fronteira Sul for the research grant that promotes the production of this and other publications. All figures were made with Biorender.
Funding
MDB acknowledges grant support from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) (CNPq proj. No 404256/2021–0 and 310606/2021–7).
Author information
Authors and Affiliations
Contributions
GCB had the idea for the article. GCB, JVC, VCM, BBL, and MDB performed the literature search and data analysis, drafted, and critically revised the work.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
An informed consent and a consent to publish were obtained from each of the participants.
Research involving human participants and/or animals
Not applicable.
Informed consent
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
• Cutaneous melanoma is one of the types of cancer with higher rates of migration and development, resulting in low survival rates.
• Cutaneous melanoma has only a few options of treatment, being most of them not effective enough to combat the disease and with many adverse effects.
• The purinergic system and its molecules influence in the development of cutaneous melanoma.
• Phenolic compound therapy has demonstrated effective results against carcinogenic processes in researches.
• Phenolic compounds are able to modulate purinoreceptors.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Carvalho Braga, G., Coiado, J.V., de Melo, V.C. et al. Cutaneous melanoma and purinergic modulation by phenolic compounds. Purinergic Signalling (2024). https://doi.org/10.1007/s11302-024-10002-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11302-024-10002-5