Abstract
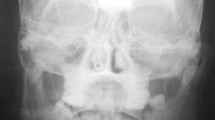
Some difficulties have been described in the diagnosis of a number of reported cases of central superior mandibular condyle dislocation, which involves intracranial penetration of the mandibular condyle. Given that radiology plays an important role in detecting this condition, we herein propose an imaging diagnostic protocol for the management of suspicious superior mandibular condyle dislocation to identify this condition and properly evaluate the damaged tissues. We make reference to the case of a 13-year-old girl, who presented at the age of 7 years with a superior dislocation of the left condyle, which was clinically diagnosed as a probable temporomandibular joint ankylosis.



Similar content being viewed by others
References
Radhakrishna S, Ramesh B. Rare case of superolateral dislocation of the condyle. Oral Maxillofac Surg. 2013;17:59–61.
Da Fonseca GD. Experimental study on fractures of the mandibular condylar process. Int J Oral Surg. 1974;3:89–101.
Spanio S, Baciliero U, Fornezza U, Pinna V, Toffanin A, Padula E. Intracranial dislocation of the mandibular condyle: report of two cases and review of the literature. Br J Oral Maxillofac Surg. 2002;40:253–5.
Melugin MB, Indresano AT, Clemens SP. Glenoid fossa fracture and condylar penetration into the middle cranial fossa: report of a case and review of the literature. J Oral Maxillofac Surg. 1997;55:1342–7.
Van Der Linden WJ. Dislocation of the mandibular condyle into the middle cranial fossa: report of a case with 5 year CT follow-up. Int J Oral Maxillofac Surg. 2003;32:215–8.
Struewer J, Kiriazidis I, Figiel J, Dukatz T, Frangen T, Ziring E. Dislocation of the mandibular condyle into the middle cranial fossa causing an epidural haematoma. J Craniomaxillofac Surg. 2012;40:396–9.
Barron RP, Kainulainen VT, Gusenbauer AW, Hollenberg R, Sándor GK. Fracture of glenoid fossa and traumatic dislocation of mandibular condyle into middle cranial fossa. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;93:640–2.
Rushton V, Rout J. Panoramic radiology. London: Quintessence Publishing Co., Ltd.; 2006.
Scarfe WC, Farman AG. What is cone-beam CT and how does it work? Dent Clin North Am. 2008;52:707–30.
Bushong SC. Magnetic resonance imaging: physical and biological principles. 3rd ed. St Louis: Mosby; 2003.
Scarfe WC, Li Z, Aboelmaaty W, Scott SA, Farman AG. Maxillofacial cone beam computed tomography: essence, elements and steps to interpretation. Aust Dent J. 2012;57:46–60.
Jacobs MA, Ibrahim TS, Ouwerkerk R. AAPM/RSNA physics tutorials for residents: MR imaging: brief overview and emerging applications. Radiographics. 2007;27:1213–29.
Mikla VI, Mikla VV. Medical imaging technology. 1st ed. Philadelphia: Elsevier; 2013.
Bushberg JT, Seibert JA, Leidholdt EM, Boone JM. The essential physics of medical imaging. 3rd ed. Philadelphia: Lippincott Williams & Wilkins; 2012.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Jorge Pinares Toledo and Ricardo Urzúa Novoa declare that they have no conflict of interest.
Human rights statements and informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions. Informed consent was obtained from all patients for being included in the study.
Rights and permissions
About this article
Cite this article
Pinares, J., Urzúa, R. Proposed radiographic protocol for central superior mandibular condyle dislocation into the middle cranial fossa: apropos of a case. Oral Radiol 32, 191–194 (2016). https://doi.org/10.1007/s11282-015-0229-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-015-0229-1