Abstract
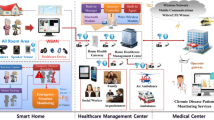
Dental caries is a complex, multifactorial, transmissible biofilm-initiated oral disease, which results in loss of tooth structure. Oral microbial flora, pH of biofilm, consumption of carbohydrates, and oral hygiene are few of those major factors, which cause dental caries. However, it is possible to monitor those cariogenic factors with the help of new technology, and that will result in the prevention and early detection of dental caries. Internet of Dental Things (IoDT) is an advanced cloud-based digital technology, which could be successfully used in this area. Our goal is to generate such a technology-based model. This paper proposes a novel innovative model, which is based on Internet of Dental Things, intraoral wireless sensors and tele dentistry, which will achieve prevention and detection of dental caries in its initial stages.









Similar content being viewed by others
References
Selwitz, R. H., Ismail, A. I., & Pitts, N. B. (2007). Dental caries. Lancet, 369(9555), 51–59. https://doi.org/10.1016/S0140-6736(07)60031-2 PMID: 17208642.
Dental Diseases and Oral Health—World health organization https://www.who.int/oral_health/publications/en/orh_fact_sheet.pdf
Rechmann, P., Kinsel, R., & Featherstone, J. D. B. (2018). Integrating caries management by risk assessment (CAMBRA) and prevention strategies into the contemporary dental practice. Compendium of Continuing Education in Dentistry, 39(4), 226–233. quiz 234, PMID: 29600870.
Bagramian, R. A., Garcia-Godoy, F., & Volpe, A. P. (2009). The global increase in dental caries. A pending public health crisis. American Journal of Dentistry, 22, 3–8.
Oral Health in America: A report of the surgeon General, Department of Health and Human Services, U.S. Public Health Service, https://www.nidcr.nih.gov/sites/default/files/201710/hck1ocv.%40www.surgeon.fullrpt.pdf
Kaur, P., Singh, S., Mathur, A., Makkar, D. K., Aggarwal, V. P., Batra, M., Sharma, A., & Goyal, N. (2017). Impact of dental disorders and its influence on self esteem levels among adolescents. Journal of Clinical and Diagnostic Research, 11(4), ZC05–ZC08. https://doi.org/10.7860/JCDR/2017/23362.9515 Published online 2017.
Giacaman, R. A. (2018). Sugars and beyond. The role of sugars and the other nutrients and their potential impact on caries. Oral Diseases, 24(7), 1185–1197. https://doi.org/10.1111/odi.12778 Epub 2017 Oct 6.
Harel-Raviv, M., Laskaris, M., & Chu, K. S. (1996). Dental caries and sugar consumption into the 21st century. American Journal of Dentistry, 9(5), 184–190. PMID: 9545901.
Maltz, M., Alves, L. S., & Zenkner, J. E. D. A. (2017). Biofilm control and oral hygiene practices. Monographs in Oral Science, 26, 76–82. https://doi.org/10.1159/000479348 Epub 2017 Oct 19.
Krzyściak, W., Jurczak, A., Kościelniak, D., Bystrowska, B., & Skalniak, A. (2014). The virulence of Streptococcus mutans and the ability to form biofilms. European Journal of Clinical Microbiology & Infectious Diseases, 33(4), 499–515. https://doi.org/10.1007/s10096-013-1993-7 Epub 2013 Oct 24.
Twetman, S. (2018). Prevention of dental caries as a non-communicable disease. European Journal of Oral Sciences, 126(Suppl 1), 19–25. https://doi.org/10.1111/eos.12528
Kutsch, V. K. (2014). Dental caries: An updated medical model of risk assessment. Journal of Prosthetic Dentistry, 111(4), 280–285. https://doi.org/10.1016/j.prosdent.2013.07.014 Epub 2013 Dec 10 PMID: 24331852.
Clarke, J. L., Scott Bourn, R. N., Skoufalos, A., Beck, E. H., & Castillo, D. J. (2017). An innovative approach to health care delivery for patients with chronic conditions. Population Health Management, 20(1), 23–30. https://doi.org/10.1089/pop.2016.0076 Published online 2017.
Marcenes, W., Kassebaum, N. J., Bernabé, E., Flaxman, A., Naghavi, M., Lopez, A., & Murray, C. J. (2013). Global burden of oral conditions in 1990–2010: A systematic analysis. Journal of Dental Research, 92(7), 592–7.
Nithila, A., Bourgeois, D., Barmes, D. E., & Murtomaa, H. (1998). WHO global oral data bank, 1986–96: An overview of oral health surveys at 12 years of age. Bulletin of the World Health Organization, 76(3), 237–244.
Ladewig, N. M., Camargo, L. B., Tedesco, T. K., Floriano, I., Gimenez, T., Imparato, J. C. P., Mendes, F. M., Braga, M. M., & Raggio, D. P. (2018). Management of dental caries among children: A look at the cost-effectiveness. Expert Review of Pharmacoeconomics & Outcomes Research, 18(2), 127–134. https://doi.org/10.1080/14737167.2018.1414602 Epub 2017 Dec 9.
Young, D. A., & Featherstone, J. D. (2013). Caries management by risk assessment. Community Dentistry and Oral Epidemiology, 41(1), e53-63. https://doi.org/10.1111/cdoe.12031
Konstantinidis, E. I., Bamparopoulos, G., Billis, A., Bamidis, P. D., et al. (2015). Internet of things for an age-friendly healthcare. Studies in Health Technology and Informatics, 210, 587–591.
Dimitrov, D. V. (2016). Medical internet of things and big data in healthcare. Healthcare Informatics Research, 22(3), 156–163. https://doi.org/10.4258/hir.2016.22.3.156
Salagare, S., & Prasad, R. (2020). An overview of internet of dental things: New frontier in advanced dentistry. Wireless Personal Communications, 110, 1345–1371. https://doi.org/10.1007/s11277-019-06790-4
Lopez-Barbosa, N., Gamarra, J. D., Osma, J. F., et al. (2016). The future point-of-care detection of disease and its data capture and handling. Analytical and Bioanalytical Chemistry, 408(11), 2827–37. https://doi.org/10.1007/s00216-015-9249-2 Epub 2016 Jan 15.
Basatneh, R., Najafi, B., Armstrong, D. G., et al. (2018). Health sensors, smart home devices, and the internet of medical things: An opportunity for dramatic improvement in care for the lower extremity complications of diabetes. Journal of Diabetes Science and Technology, 12(3), 577–586.
Pasluosta, C. F., Gassner, H., Winkler, J., Klucken, J., Eskofier, B. M., et al. (2015). An emerging era in the management of Parkinson’s disease: Wearable technologies and the internet of things. IEEE Journal of Biomedical and Health Informatics, 19(6), 1873–1881. https://doi.org/10.1109/jbhi.2015.2461555
Rovini, E., Maremmani, C., Cavallo, F., et al. (2018). Automated systems based on wearable sensors for the management of Parkinson’s disease at home: A systematic review. Telemedicine Journal E-Health. https://doi.org/10.1089/tmj.2018.0035
Naranjo-Hernández, D., Talaminos-Barroso, A., Reina-Tosina, J., Roa, L. M., Barbarov-Rostan, G., Cejudo-Ramos, P., et al. (2018). Smart vest for respiratory rate monitoring of COPD patients based on non-contact capacitive sensing. Sensors (Basel), 18, 2144.
Choi, J. E., Lyons, K. M., Kieser, J. A., & Waddell, N. J. (2017). Diurnal variation of intraoral pH and temperature. BDJ Open, 30(3), 17015. https://doi.org/10.1038/bdjopen.2017.15 PMID:29607085; PMCID:PMC5842828.
Sun, J., Guo, Y., Wang, X., Zeng, Q., et al. (2016). mHealth For Aging China Opportunities and challenges. Aging Disease, 7(1), 53–67. https://doi.org/10.14336/ad.2015.1011 (eCollection 2016 Jan).
Deng, Y. Y., Chen, C. L., Tsaur, W. J., Tang, Y. W., Chen, J. H., et al. (2017). Internet of things (IoT) based design of a secure and lightweight body area network (BAN) healthcare system. Sensors (Basel), 17(12), E2919. https://doi.org/10.3390/s17122919
Jampani, N. D., Nutalapati, R., Dontula, B. S. K., Boyapati, R., et al. (2011). Applications of teledentistry: A literature review and update. Journal of International Society of Preventive and Community Dentistry, 1(2), 37–44.
Estai, M., Bunt, S., Kanagasingam, Y., Kruger, E., Tennant, M., et al. (2016). Diagnostic accuracy of teledentistry in the detection of dental caries: A systematic review. Journal of Evidence Based Dental Practice, 16(3), 161–172. https://doi.org/10.1016/j.jebdp.2016.08.003 Epub 2016 Sep 7.
Irving, M., Stewart, R., Spallek, H., Blinkhorn, A., et al. (2018). Using teledentistry in clinical practice as an enabler to improve access to clinical care: A qualitative systematic review. Journal of Telemedicine and Telecare, 24(3), 129–146. https://doi.org/10.1177/1357633X16686776 Epub 2017 Jan 16.
Duka, M., Mihailović, B., Miladinović, M., Janković, A., Vujicić, B., et al. (2009). Evaluation of telemedicine systems for impacted third molars diagnosis. Vojnosanitetski Pregled, 66(12), 985–91.
Arora, S. (2020). IoMT (internet of medical things) reducing cost while improving patient care. IEEE Pulse, 11(5), 24–27. https://doi.org/10.1109/MPULS.2020.3022143 PMID: 33064641.
Funding
This research was self-supported.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Smita Salagare. The first draft of the manuscript was written by Smita Salagare and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.)
Corresponding author
Ethics declarations
Conflicts of interest
This research was supported by Department of Business Development and Technology, CTIF Global Capsule, Aarhus University, Herning, Denmark.)
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Salagare, S., Prasad, R. Internet of Dental Things (IoDT), Intraoral Wireless Sensors, and Teledentistry: A Novel Model for Prevention of Dental Caries. Wireless Pers Commun 123, 3263–3274 (2022). https://doi.org/10.1007/s11277-021-09287-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11277-021-09287-1