Abstract
Aim
This study intended to scrutinize the effect of RFR time on adverse renal outcomes and mortality and try to define the cutoff of early RFR.
Methods
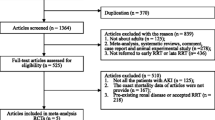
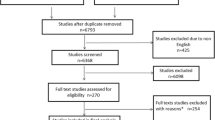
We conducted a literature search from database inception to February 2023. Outcome measures incorporated the progression of CKD, delivery of RRT, incidence of composite renal outcomes, and mortality. And pooled results were depicted as odds ratio (OR) and 95% confidence interval (CI).
Results
A total of 11 studies were finally selected (507,989 patients, mean follow-up, 3.89 years). The results exhibited that the crude mortality was lower in patients with early RFR (OR = 0.39, 95% CI: 0.16–0.95, P = 0.037). In addition, patients with early RFR had a lower incidence of progression to CKD (OR = 0.38, 95% CI: 0.17–0.85, P < 0.018), RRT (OR = 0.37, 95% CI: 0.20–0.71, P = 0.03), and composite renal outcomes (OR = 0.18, 95% CI: 0.15–0.20, P < 0.001). CKD progression-related events were significantly higher in patients whose renal function recovered after 7 days (OR = 0.69, 95% CI: 0.47–1.09, P = 0.112) than in those whose renal function recovered within 7 days (OR = 0.23, 95% CI: 0.06–0.92, P = 0.038), and the risk of RRT was lower in patients who recovered within 7 days (OR = 0.32, 95% CI: 0.15–0.66, P = 0.002) than in those who recovered after 7 days (OR = 0.72, 95% CI: 0.17–3.09, P = 0.654) or longer.
Conclusion
Patients with early RFR had a lower risk of CKD progression, RRT, and composite renal outcomes, as well as lower crude mortality than those without early recovery, despite no marked difference in 30-day, 90-day, and 1-year mortality. We speculated that 7 days may be used as a cutoff for early RFR.





Similar content being viewed by others
References
Kellum JA, Lameire N, KDIGO AKI Guideline Work Group (2013) Diagnosis, evaluation, and management of acute kidney injury: a KDIGO summary (Part 1). Crit Care 17:204. https://doi.org/10.1186/cc11454
Ronco C, Bellomo R, Kellum JA (2019) Acute kidney injury. Lancet 394:1949–1964. https://doi.org/10.1016/S0140-6736(19)32563-2
Hoste EA, Kellum JA, Selby NM et al (2018) Global epidemiology and outcomes of acute kidney injury. Nat Rev Nephrol. https://doi.org/10.1038/s41581-018-0052-0
Ostermann M, Bellomo R, Burdmann EA et al (2020) Controversies in acute kidney injury: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) Conference. Kidney Int 98:294–309. https://doi.org/10.1016/j.kint.2020.04.020
Bihorac A, Yavas S, Subbiah S et al (2009) Long-term risk of mortality and acute kidney injury during hospitalization after major surgery. Ann Surg 249:851–858. https://doi.org/10.1097/SLA.0b013e3181a40a0b
Tain YL, Liu CL, Kuo HC, Hsu CN (2022) Kidney function trajectory within six months after acute kidney injury inpatient care and subsequent adverse kidney outcomes: a retrospective cohort study. J Pers Med 12:1606. https://doi.org/10.3390/jpm12101606
Duarte TTP, Magro MCS (2022) Recovery of renal function in clinical patients with acute kidney injury: impact on mortality. Life (Basel) 12:852. https://doi.org/10.3390/life12060852
Alobaidi R, Anton N, Burkholder S et al (2021) Association between acute kidney injury duration and outcomes in critically ill children. Pediatr Crit Care Med 22:642–650. https://doi.org/10.1097/PCC.0000000000002679
Bhatraju PK, Zelnick LR, Chinchilli VM et al (2020) Association between early recovery of kidney function after acute kidney injury and long-term clinical outcomes. JAMA Netw Open 3:e202682. https://doi.org/10.1001/jamanetworkopen.2020.2682
Chua H-R, Wong W-K, Ong VH et al (2020) Extended mortality and chronic kidney disease after septic acute kidney injury. J Intensive Care Med 35:527–535. https://doi.org/10.1177/0885066618764617
Ozrazgat-Baslanti T, Loftus TJ, Ren Y et al (2021) Association of persistent acute kidney injury and renal recovery with mortality in hospitalised patients. BMJ Health Care Inform 28:e100458. https://doi.org/10.1136/bmjhci-2021-100458
Orieux A, Prezelin-Reydit M, Prevel R et al (2023) Clinical trajectories and impact of acute kidney disease after acute kidney injury in the intensive care unit: a 5-year single-centre cohort study. Nephrol Dial Transplant 38:167–176. https://doi.org/10.1093/ndt/gfac054
Ye N, Xu Y, Bellomo R et al (2020) Effect of nephrology follow-up on long-term outcomes in patients with acute kidney injury: A systematic review and meta-analysis. Nephrology 25:607–615. https://doi.org/10.1111/nep.13698
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Zhou D, Lun Z, Wang B et al (2022) Association between non-recovered contrast-associated acute kidney injury and poor prognosis in patients undergoing coronary angiography. Front Cardiovasc Med 9:823829. https://doi.org/10.3389/fcvm.2022.823829
Fidalgo P, Ahmed M, Meyer SR et al (2014) Association between transient acute kidney injury and morbidity and mortality after lung transplantation: a retrospective cohort study. J Crit Care 29:1028–1034. https://doi.org/10.1016/j.jcrc.2014.07.024
Luo X, Yan P, Zhang N et al (2022) Early recovery status and outcomes after sepsis-associated acute kidney injury in critically ill patients. Zhong Nan Da Xue Xue Bao Yi Xue Ban 47:535–545. https://doi.org/10.11817/j.issn.1672-7347.2022.210368
Jing L, Chen W, Zhao L et al (2021) Acute kidney injury following adult lung transplantation. Chin Med J (Engl) 135:172–180. https://doi.org/10.1097/CM9.0000000000001636
Sawhney S, Marks A, Fluck N et al (2017) Intermediate and long-term outcomes of survivors of acute kidney injury episodes: a large population-based cohort study. Am J Kidney Dis 69:18–28. https://doi.org/10.1053/j.ajkd.2016.05.018
Wang H, Lambourg E, Guthrie B et al (2022) Patient outcomes following AKI and AKD: a population-based cohort study. BMC Med 20:229. https://doi.org/10.1186/s12916-022-02428-8
Singbartl K, Kellum JA (2012) AKI in the ICU: definition, epidemiology, risk stratification, and outcomes. Kidney Int 81:819–825. https://doi.org/10.1038/ki.2011.339
Chawla LS, Bellomo R, Bihorac A et al (2017) Acute kidney disease and renal recovery: consensus report of the Acute Disease Quality Initiative (ADQI) 16 Workgroup. Nat Rev Nephrol 13:241–257. https://doi.org/10.1038/nrneph.2017.2
Pickkers P, Darmon M, Hoste E et al (2021) Acute kidney injury in the critically ill: an updated review on pathophysiology and management. Intensive Care Med 47:835–850. https://doi.org/10.1007/s00134-021-06454-7
Han SS, Kim S, Ahn SY et al (2013) Duration of acute kidney injury and mortality in critically ill patients: a retrospective observational study. BMC Nephrol 14:133. https://doi.org/10.1186/1471-2369-14-133
Kellum JA, Sileanu FE, Bihorac A et al (2017) Recovery after acute kidney injury. Am J Respir Crit Care Med 195:784–791. https://doi.org/10.1164/rccm.201604-0799OC
Heung M, Steffick DE, Zivin K et al (2016) Acute Kidney injury recovery pattern and subsequent risk of CKD: an analysis of veterans health administration data. Am J Kidney Dis 67:742–752. https://doi.org/10.1053/j.ajkd.2015.10.019
Liu Y, Davari-Farid S, Arora P et al (2014) Early versus late initiation of renal replacement therapy in critically ill patients with acute kidney injury after cardiac surgery: a systematic review and meta-analysis. J Cardiothorac Vasc Anesth 28:557–563. https://doi.org/10.1053/j.jvca.2013.12.030
Wang X, Jie Yuan W (2012) Timing of initiation of renal replacement therapy in acute kidney injury: a systematic review and meta-analysis. Ren Fail 34:396–402. https://doi.org/10.3109/0886022X.2011.647371
Yang XM, Tu GW, Zheng JL et al (2017) A comparison of early versus late initiation of renal replacement therapy for acute kidney injury in critically ill patients: an updated systematic review and meta-analysis of randomized controlled trials. BMC Nephrol 18:264. https://doi.org/10.1186/s12882-017-0667-6
Castro I, Relvas M, Gameiro J et al (2022) The impact of early versus late initiation of renal replacement therapy in critically ill patients with acute kidney injury on mortality and clinical outcomes: a meta-analysis. Clin Kidney J 15:1932–1945. https://doi.org/10.1093/ckj/sfac139
Su CC, Chen JY, Chen SY et al (2023) Outcomes associated with acute kidney disease: a systematic review and meta-analysis. EClinicalMedicine 55:101760. https://doi.org/10.1016/j.eclinm.2022.101760
Funding
This work was supported by the Hebei Provincial Specialty Capacity Building and Specialty Leader Training Project [(2018)674], the Hebei Provincial Excellent Talents in Clinical Medicine Training Project [(2019)139], the Hebei province medical technology tracking project (GZ2020013), the Hebei Clinical Medical Research Centre Project (20577701D), the project of the Hebei Provincial Excellent Health Talents and High-Quality Development of Public Hospitals [(2022)180], and the project of Natural Science Foundation of Hebei Province (H2023206385).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Yaling Bai and Yajing Li have contributed to this work equally. The authors state that there is no conflict of interest.
Ethical approval
No ethical approval was required because the data were extracted from previously published articles.
Informed consent
This study did not directly involve human participants or animal subjects.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bai, Y., Li, Y., Jin, J. et al. Effects of early recovery of renal function on adverse renal outcomes and mortality in patients with acute kidney injury: a systematic review and meta-analysis. Int Urol Nephrol (2024). https://doi.org/10.1007/s11255-024-03974-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11255-024-03974-1