Abstract
Purpose
SARS-CoV-2 had a significant impact on public health since its declaration as a pandemic. It is linked to a high rate of multiple organ dysfunction syndrome (MODS) and a slew of long-term symptoms that are yet to be thoroughly investigated. Among these, genitourinary symptoms of an overactive bladder (increased frequency, urgency, and nocturia) have recently been identified and labeled as COVID-associated cystitis (CAC). This current research is performed to review this phenomenon.
Methods
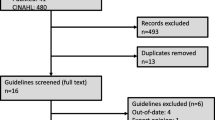
A literature search was performed in MEDLINE, Cochrane, and Google Scholar databases and 185 articles were obtained in total, including reviews and trials involving CAC, which were screened using various methods, and 42 articles were gathered for the review.
Results
Among its multitude of symptoms, overactive bladder (OAB) leads to poorer outcomes. The inflammatory mediator-based theory and the ACE-2 receptor-based theory are two probable theories for how it harms the bladder urothelium. The expression of ACE-2 receptors during the pathogenesis of CAC warrants further investigation as ACE modulation may reveal more information about COVID-19 complications. Other comorbidities, immunocompromised patients, or patients with a history of urinary tract infections can also exacerbate this condition.
Conclusion
The scarce literature collected related to CAC gives us an insight into the symptomatology, pathophysiology, and possible treatment plans. Treatment choices are diverse among COVID-19-afflicted and unaffected patients for treating urinary symptoms which highlights the importance to distinguish between the two. CAC shows greater prevalence and morbidity when linked to other conditions, thereby warranting future developments in it.

Similar content being viewed by others
Data Availability
The authors confirm that the data supporting the findings of this study are available within the article and its supplementary materials.
References
Shen Q, Li J, Zhang Z et al (2022) COVID-19: systemic pathology and its implications for therapy. Int J Biol Sci 18(1):386–408. https://doi.org/10.7150/ijbs.65911
Ebner B, Volz Y, Mumm JN, Stief CG, Magistro G (2022) The COVID-19 pandemic—what have urologists learned? Nat Rev Urol 19(6):344–356. https://doi.org/10.1038/s41585-022-00586-1
Lamb LE, Dhar N, Timar R, Wills M, Dhar S, Chancellor MB (2020) COVID-19 inflammation results in urine cytokine elevation and causes COVID-19 associated cystitis (CAC). Med Hypotheses 145:110375. https://doi.org/10.1016/j.mehy.2020.110375
Cheema M, Aghazadeh H, Nazarali S et al (2020) Keratoconjunctivitis as the initial medical presentation of the novel coronavirus disease 2019 (COVID-19). Can J Ophthalmol 55(4):e125–e129. https://doi.org/10.1016/j.jcjo.2020.03.003
Iacobucci G (2021) Covid-19: runny nose, headache, and fatigue are commonest symptoms of omicron, early data show. BMJ 375:n3103. https://doi.org/10.1136/bmj.n3103
Raveendran AV, Jayadevan R, Sashidharan S (2022) Long COVID: an overview [published correction appears in]. Diabetes Metab Syndr 16(5):102504. https://doi.org/10.1016/j.dsx.2021.04.007
Carfì A, Bernabei R, Landi F (2020) Gemelli against COVID-19 post-acute care study group: persistent symptoms in patients after acute COVID-19. JAMA 324(6):603–605. https://doi.org/10.1001/jama.2020.12603
Greenhalgh T, Knight M, A’Court C, Buxton M, Husain L (2020) Management of post-acute covid-19 in primary care. BMJ 370:m3026. https://doi.org/10.1136/bmj.m3026
Gu J, Gong E, Zhang B et al (2005) Multiple organ infection and the pathogenesis of SARS. J Exp Med 202(3):415–424. https://doi.org/10.1084/jem.20050828
Liu K, Chen X, Ren X, Wu Y, Ren S, Qin C (2021) SARS-CoV-2 effects in the genitourinary system and prospects of sex hormone therapy. Asian J Urol 8(3):303–314. https://doi.org/10.1016/j.ajur.2020.11.004
Connelly ZM, Whitaker D, Dullea A, Ramasamy R (2022) SARS-CoV-2 effects on the male genitourinary system. Am J Clin Exp Urol. 10(4):199–209
Zou X, Chen K, Zou J, Han P, Hao J, Han Z (2020) Single-cell RNA-seq data analysis on the receptor ACE2 expression reveals the potential risk of different human organs vulnerable to 2019-nCoV infection. Front Med 14(2):185–192. https://doi.org/10.1007/s11684-020-0754-0
Peerapornratana S, Manrique-Caballero CL, Gómez H, Kellum JA (2019) Acute kidney injury from sepsis: current concepts, epidemiology, pathophysiology, prevention and treatment. Kidney Int 96(5):1083–1099. https://doi.org/10.1016/j.kint.2019.05.026
Gabarre P, Dumas G, Dupont T, Darmon M, Azoulay E, Zafrani L (2020) Acute kidney injury in critically ill patients with COVID-19. Intensive Care Med 46(7):1339–1348. https://doi.org/10.1007/s00134-020-06153-9
Zhang H, Chen Y, Yuan Q et al (2020) Identification of kidney transplant recipients with coronavirus disease. Eur Urol 77(6):742–747. https://doi.org/10.1016/j.eururo.2020.03.030
Lamb LE, Timar R, Wills M et al (2022) Long COVID and COVID-19-associated cystitis (CAC). Int Urol Nephrol 54(1):17–21. https://doi.org/10.1007/s11255-021-03030-2
Creta M, Sagnelli C, Celentano G et al (2021) SARS-CoV-2 infection affects the lower urinary tract and male genital system: a systematic review. J Med Virol 93(5):3133–3142. https://doi.org/10.1002/jmv.26883
Aboudounya MM, Heads RJ (2021) COVID-19 and toll-like receptor 4 (TLR4): SARS-CoV-2 may bind and activate TLR4 to increase ACE2 expression, facilitating entry and causing hyperinflammation. Mediat Inflamm 2021:8874339. https://doi.org/10.1155/2021/8874339
Mumm JN, Osterman A, Ruzicka M et al (2020) Urinary frequency as a possibly overlooked symptom in COVID-19 patients: does SARS-CoV-2 cause viral cystitis? Eur Urol 78(4):624–628. https://doi.org/10.1016/j.eururo.2020.05.013
Varga Z, Flammer AJ, Steiger P et al (2020) Endothelial cell infection and endotheliitis in COVID-19. Lancet Lond Engl 395(10234):1417–1418. https://doi.org/10.1016/S0140-6736(20)30937-5
Grover S, Srivastava A, Lee R, Tewari AK, Te AE (2011) Role of inflammation in bladder function and interstitial cystitis. Ther Adv Urol 3(1):19–33. https://doi.org/10.1177/1756287211398255
Jiang YH, Jhang JF, Hsu YH, Ho HC, Wu YH, Kuo HC (2020) Urine cytokines as biomarkers for diagnosing interstitial cystitis/bladder pain syndrome and mapping its clinical characteristics. Am J Physiol Ren Physiol 318(6):F1391–F1399. https://doi.org/10.1152/ajprenal.00051.2020
Shie JH, Kuo HC (2011) Higher levels of cell apoptosis and abnormal E-cadherin expression in the urothelium are associated with inflammation in patients with interstitial cystitis/painful bladder syndrome. BJU Int 108(2 pt 2):136–141. https://doi.org/10.1111/j.1464-410X.2010.09911.x
Zhang Z, Ai G, Chen L et al (2021) Associations of immunological features with COVID-19 severity: a systematic review and meta-analysis. BMC Infect Dis 21(1):738. https://doi.org/10.1186/s12879-021-06457-1
Sant GR, Kempuraj D, Marchand JE, Theoharides TC (2007) The mast cell in interstitial cystitis: role in pathophysiology and pathogenesis. Urology 69(4 Suppl):34–40. https://doi.org/10.1016/j.urology.2006.08.1109
Sant GR, Theoharides TC (1994) The role of the mast cell in interstitial cystitis. Urol Clin N Am 21(1):41–53
Fry CH, Vahabi B (2016) The role of the mucosa in normal and abnormal bladder function. Basic Clin Pharmacol Toxicol 119(Suppl 3):57–62. https://doi.org/10.1111/bcpt.12626
Dhar N, Dhar S, Timar R, Lucas S, Lamb LE, Chancellor MB (2020) De novo urinary symptoms associated with COVID-19: COVID-19-associated cystitis. J Clin Med Res 12(10):681–682. https://doi.org/10.14740/jocmr4294
Kaya Y, Kaya C, Kartal T, Tahta T, Tokgöz VY (2021) Could LUTS be early symptoms of COVID-19. Int J Clin Pract 75(3):e13850. https://doi.org/10.1016/j.eururo.2020.06.006
Luciani LG, Gallo F, Malossini G (2020) Re: Jan-Niclas Mumm, Andreas Osterman, Michael Ruzicka, Et Al: urinary frequency as a possible overlooked symptom in COVID-19 patients: does SARS-CoV-2 cause viral cystitis? Eur Urol In Press 78(3):e129–e130. https://doi.org/10.1016/J.Eururo.2020.05
Tiryaki S, Egil O, Birbilen AZ, Buyukcam A (2022) COVID-19 associated lower urinary tract symptoms in children. J Pediatr Urol 18(5):680.e1-680.e7. https://doi.org/10.1016/j.jpurol.2022.08.018
Haghpanah A, Masjedi F, Salehipour M, Hosseinpour A, Roozbeh J, Dehghani A (2022) Is COVID-19 a risk factor for progression of benign prostatic hyperplasia and exacerbation of its related symptoms? A systematic review. Prostate Cancer Prostatic Dis 25(1):27–38. https://doi.org/10.1038/s41391-021-00388-3
Hsu LN, Hu JC, Chen PY, Lee WC, Chuang YC (2022) Metabolic syndrome and overactive bladder syndrome may share common pathophysiologies. Biomedicines 10(8):1957. https://doi.org/10.3390/biomedicines10081957
New survey finds COVID-19 significantly worsens IC symptoms—interstitial cystitis network [Internet] (2022). https://www.ic-network.com/new-survey-finds-covid-19-significantly-worsens-ic-symptoms/. Accessed 19 Dec 2022
Welk B, Richard L, Braschi E, Averbeck MA (2021) Is coronavirus disease 2019 associated with indicators of long-term bladder dysfunction? Neurourol Urodyn 40(5):1200–1206. https://doi.org/10.1002/nau.24682
Bernikov AN, Kupriyanov AA, Stroganov RV, Khodyreva LA, Zaitsev AV (2021) Lower urinary tract symptoms and COVID-19. Urologiia 5:78–83
Ohannessian R, Duong TA, Odone A (2020) Global telemedicine implementation and integration within health systems to fight the COVID-19 pandemic: a call to action. JMIR Public Health Surveill 6(2):e18810. https://doi.org/10.2196/18810
Bertini S, Alekseeva A, Elli S et al (2022) Pentosan polysulfate inhibits attachment and infection by SARS-CoV-2 in vitro: insights into structural requirements for binding. Thromb Haemost 122(6):984–997. https://doi.org/10.1055/a-1807-0168
Kumar R, Rathi H, Haq A, Wimalawansa SJ, Sharma A (2021) Putative roles of vitamin D in modulating immune response and immunopathology associated with COVID-19. Virus Res 292:198235. https://doi.org/10.1016/j.virusres.2020.198235
Willis-Gray MG, Dieter AA, Geller EJ (2016) Evaluation and management of overactive bladder: strategies for optimizing care. Res Rep Urol 8:113–122. https://doi.org/10.2147/RRU.S93636
Hoang Roberts L, Zwaans BMM, Peters KM, Chancellor M, Padmanabhan P (2022) Incidence of new or worsening overactive bladder among patients with a prior SARS-CoV-2 infection: a cohort study. Eur Urol Open Sci 46:68–74. https://doi.org/10.1016/j.euros.2022.10.001
Chancellor MB, Wills M, Timar R et al (2021) COVID-19 associated cystitis (CAC): increased urinary symptoms and biomarkers of inflammation in urine in patients with acute COVID-19. J Urol. https://doi.org/10.1097/JU.0000000000002026.15
Zheng Y, Liu X, Le W et al (2020) A human circulating immune cell landscape in aging and COVID-19. Protein Cell 11(10):740–770. https://doi.org/10.1007/s13238-020-00762-2
Author information
Authors and Affiliations
Contributions
Conceptualization: AD, RG; methodology: AD, RG, YK; validation: AD, RG; formal analysis and investigation: AD, RG; data curation: RG, AD; writing—original draft: AD, RG, PD, YK, GG, SNA, SM, AN, ATB; visualization: AD, RG, YK, SNA; writing—review and editing: AD, RG, GG, YK, AN, PD, KP, AS, SNA, SM, ATB; editing: ATB, PD, KP, AS; supervision and project administration: MA.
Corresponding author
Ethics declarations
Conflict of interest
There are no funding sources or conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Ananya Dhawan and Rohit Ganduboina have equally contributed to the paper and deserve 1st authorship.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dhawan, A., Ganduboina, R., Dutta, P. et al. COVID-associated cystitis: the culprit behind the bladder woes post-COVID infection? A review. Int Urol Nephrol 55, 2367–2372 (2023). https://doi.org/10.1007/s11255-023-03700-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03700-3