Abstract
Purpose
Traditional cutoff values of urinary albumin-to-creatinine ratio (UACR) for predicting mortality have recently been challenged. In this study, we investigated the optimal threshold of UACR for predicting long-term cardiovascular and non-cardiovascular mortality in the general population.
Methods
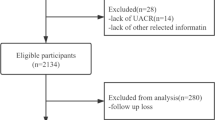
Data for 25,302 adults were extracted from the National Health and Nutrition Examination Survey (2005–2014). Receiver operating characteristic (ROC) curve analysis was performed to assess the predictive value of UACR for cardiovascular and non-cardiovascular mortality. A Cox regression model was established to examine the association between UACR and cardiovascular and non-cardiovascular mortality. X-tile was used to estimate the optimal cutoff of UACR.
Results
The UACR had acceptable predictive value for both cardiovascular (AUC (95% CI) for 1-year, 3-year and 5-year mortality, respectively: 0.769 (0.711–0.828), 0.764 (0.722–0.805) and 0.763 (0.730–0.795)) and non-cardiovascular (AUC (95% CI) for 1-year, 3-year and 5-year mortality, respectively: 0.772 (0.681–0.764), 0.708 (0.686–0.731) and 0.708 (0.690–0.725)) mortality. The optimal cutoff values were 16 and 30 mg/g for predicting long-term cardiovascular and non-cardiovascular mortality, respectively. Both cutoffs of UACR had acceptable specificity (0.785–0.891) in predicting long-term mortality, while the new proposed cutoff (16 mg/g) had higher sensitivity. The adjusted hazard ratios of cardiovascular and non-cardiovascular mortality for the high-risk group were 2.50 (95% CI 1.96–3.18, P < 0.001) and 1.92 (95% CI 1.70–2.17, P < 0.001), respectively.
Conclusions
Compared to the traditional cutoff value (30 mg/g), a UACR cutoff of 16 mg/g may be more sensitive for identifying patients at high risk for cardiovascular mortality in the general population.




Similar content being viewed by others
Data availability
Data are from Centers for Disease Control and Prevention, National Center for Health Statistics. National health and nutrition examination survey data. Available at: https://www.cdc.gov/nchs/nhanes/
References
Hillege HL, Fidler V, Diercks GF, van Gilst WH, de Zeeuw D, van Veldhuisen DJ, Gans RO, Janssen WM, Grobbee DE, de Jong PE (2002) Urinary albumin excretion predicts cardiovascular and noncardiovascular mortality in general population. Circulation 106(14):1777–1782. https://doi.org/10.1161/01.cir.0000031732.78052.81
da Silva MD, de Santa Rosa RG, Gomes CP, Cardoso Berensztejn A, Pinto MV, Pinto LF, Cruz MW (2019) Albumin/creatinine (uACR) and protein/creatinine (uPCR) ratios in spot urine samples can be used to evaluate albuminuria and proteinuria in hereditary transthyretin amyloidosis patients. Amyloid 26(sup1):41–42. https://doi.org/10.1080/13506129.2019.1582506
Roth GA, Johnson C, Abajobir A, Abd-Allah F, Abera SF, Abyu G, Ahmed M, Aksut B, Alam T, Alam K, Alla F, Alvis-Guzman N, Amrock S, Ansari H, Ärnlöv J, Asayesh H, Atey TM, Avila-Burgos L, Awasthi A, Banerjee A, Barac A, Bärnighausen T, Barregard L, Bedi N, Belay Ketema E, Bennett D, Berhe G, Bhutta Z, Bitew S, Carapetis J, Carrero JJ, Malta DC, Castañeda-Orjuela CA, Castillo-Rivas J, Catalá-López F, Choi JY, Christensen H, Cirillo M, Cooper L Jr, Criqui M, Cundiff D, Damasceno A, Dandona L, Dandona R, Davletov K, Dharmaratne S, Dorairaj P, Dubey M, Ehrenkranz R, El Sayed ZM, Faraon EJA, Esteghamati A, Farid T, Farvid M, Feigin V, Ding EL, Fowkes G, Gebrehiwot T, Gillum R, Gold A, Gona P, Gupta R, Habtewold TD, Hafezi-Nejad N, Hailu T, Hailu GB, Hankey G, Hassen HY, Abate KH, Havmoeller R, Hay SI, Horino M, Hotez PJ, Jacobsen K, James S, Javanbakht M, Jeemon P, John D, Jonas J, Kalkonde Y, Karimkhani C, Kasaeian A, Khader Y, Khan A, Khang YH, Khera S, Khoja AT, Khubchandani J, Kim D, Kolte D, Kosen S, Krohn KJ, Kumar GA, Kwan GF, Lal DK, Larsson A, Linn S, Lopez A, Lotufo PA, El Razek HMA, Malekzadeh R, Mazidi M, Meier T, Meles KG, Mensah G, Meretoja A, Mezgebe H, Miller T, Mirrakhimov E, Mohammed S, Moran AE, Musa KI, Narula J, Neal B, Ngalesoni F, Nguyen G, Obermeyer CM, Owolabi M, Patton G, Pedro J, Qato D, Qorbani M, Rahimi K, Rai RK, Rawaf S, Ribeiro A, Safiri S, Salomon JA, Santos I, Santric Milicevic M, Sartorius B, Schutte A, Sepanlou S, Shaikh MA, Shin MJ, Shishehbor M, Shore H, Silva DAS, Sobngwi E, Stranges S, Swaminathan S, Tabarés-Seisdedos R, Tadele Atnafu N, Tesfay F, Thakur JS, Thrift A, Topor-Madry R, Truelsen T, Tyrovolas S, Ukwaja KN, Uthman O, Vasankari T, Vlassov V, Vollset SE, Wakayo T, Watkins D, Weintraub R, Werdecker A, Westerman R, Wiysonge CS, Wolfe C, Workicho A, Xu G, Yano Y, Yip P, Yonemoto N, Younis M, Yu C, Vos T, Naghavi M, Murray C (2017) Global, regional, and national burden of cardiovascular diseases for 10 causes, 1990 to 2015. J Am Coll Cardiol 70(1):1–25. https://doi.org/10.1016/j.jacc.2017.04.052
Ruilope LM, Rodríguez-Sánchez E, Ruiz-Hurtado G (2019) The endless story of markers of renal function and cardiovascular risk. Eur Heart J 40(42):3494–3495. https://doi.org/10.1093/eurheartj/ehz489
American Diabetes Association. Microvascular Complications and Foot Care (2016). Diabetes Care 39 Suppl 1:S72-80. https://doi.org/10.2337/dc16-S012
Garimella PS, Lee AK, Ambrosius WT, Bhatt U, Cheung AK, Chonchol M, Craven T, Hawfield AT, Jotwani V, Killeen A, Punzi H, Sarnak MJ, Wall BM, Ix JH, Shlipak MG (2019) Markers of kidney tubule function and risk of cardiovascular disease events and mortality in the SPRINT trial. Eur Heart J 40(42):3486–3493. https://doi.org/10.1093/eurheartj/ehz392
Matsushita K, van der Velde M, Astor BC, Woodward M, Levey AS, de Jong PE, Coresh J, Gansevoort RT (2010) Association of estimated glomerular filtration rate and albuminuria with all-cause and cardiovascular mortality in general population cohorts: a collaborative meta-analysis. Lancet 375(9731):2073–2081. https://doi.org/10.1016/s0140-6736(10)60674-5
Visram A, Al Saleh A, Parmar H, McDonald J, Lieske J, Vaxman I, Muchtar E, Hobbs M, Fonder A, Hwa Y, Buadi F, Dingli D, Lacy M, Dispenzieri A, Kapoor P, Hayman S, Warsame R, Kourelis T, Siddiqui M, Gonsalves W, Lust J, Kyle R, Vincent Rajkumar S, Gertz M, Kumar S, Leung N(2020) Correlation between urine ACR and 24-h proteinuria in a real-world cohort of systemic AL amyloidosis patients. Blood Cancer J 10(12):124. https://doi.org/10.1038/s41408-020-00391-2
Scirica BM, Mosenzon O, Bhatt DL, Udell JA, Steg PG, McGuire DK, Im K, Kanevsky E, Stahre C, Sjöstrand M, Raz I, Braunwald E (2018) Cardiovascular outcomes according to urinary albumin and kidney disease in patients with Type 2 diabetes at high cardiovascular risk: observations from the SAVOR-TIMI 53 trial. JAMA Cardiol 3(2):155–163. https://doi.org/10.1001/jamacardio.2017.4228
Ohkuma T, Jun M, Chalmers J, Cooper ME, Hamet P, Harrap S, Zoungas S, Perkovic V, Woodward M (2019) Combination of changes in estimated GFR and albuminuria and the risk of major clinical outcomes. Clin J Am Soc Nephrol 14(6):862–872. https://doi.org/10.2215/CJN.13391118
Sung K-C, Ryu S, Lee J-Y, Lee SH, Cheong E, Hyun Y-Y, Lee K-B, Kim H, Byrne CD (2016) Urine albumin/creatinine ratio below 30 mg/g is a predictor of incident hypertension and cardiovascular mortality. J Am Heart Assoc. https://doi.org/10.1161/JAHA.116.003245
Blecker S, Matsushita K, Köttgen A, Loehr LR, Bertoni AG, Boulware LE, Coresh J (2011) High-normal albuminuria and risk of heart failure in the community. Am J Kidney Dis 58(1):47–55. https://doi.org/10.1053/j.ajkd.2011.02.391
Mosenzon O, Bain SC, Heerspink HJL, Idorn T, Mann JFE, Persson F, Pratley RE, Rasmussen S, Rossing P, von Scholten BJ, Raz I (2020) Cardiovascular and renal outcomes by baseline albuminuria status and renal function: results from the LEADER randomized trial. Diabetes Obes Metab 22(11):2077–2088. https://doi.org/10.1111/dom.14126
Kovesdy CP, Lott EH, Lu JL, Malakauskas SM, Ma JZ, Molnar MZ, Kalantar-Zadeh K (2013) Outcomes associated with microalbuminuria: effect modification by chronic kidney disease. J Am Coll Cardiol 61(15):1626–1633. https://doi.org/10.1016/j.jacc.2012.11.071
Inoue K, Streja E, Tsujimoto T, Kobayashi H (2021) Urinary albumin-to-creatinine ratio within normal range and all-cause or cardiovascular mortality among US adults enrolled in the NHANES during 1999–2015. Ann Epidemiol 55:15–23. https://doi.org/10.1016/j.annepidem.2020.12.004
Warnock DG, Muntner P, McCullough PA, Zhang X, McClure LA, Zakai N, Cushman M, Newsome BB, Kewalramani R, Steffes MW, Howard G, McClellan WM (2010) Kidney function, albuminuria, and all-cause mortality in the REGARDS (reasons for geographic and racial differences in stroke) study. Am J Kidney Dis 56(5):861–871. https://doi.org/10.1053/j.ajkd.2010.05.017
Centers for Disease Control and Prevention, National Center for Health Statistics. National health and nutrition examination survey data. Available at: https://www.cdc.gov/nchs/nhanes/. Accessed 1 Sep 2020
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612. https://doi.org/10.7326/0003-4819-150-9-200905050-00006
Camp RL, Dolled-Filhart M, Rimm DL (2004) X-tile: a new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization. Clinical Cancer Res 10(21):7252–7259. https://doi.org/10.1158/1078-0432.Ccr-04-0713
Yang S, Ma C, Wu H, Zhang H, Yuan F, Yang G, Yang Q, Jia L, Liang Z, Kang L (2020) Tectorigenin attenuates diabetic nephropathy by improving vascular endothelium dysfunction through activating AdipoR1/2 pathway. Pharmacol Res 153:104678. https://doi.org/10.1016/j.phrs.2020.104678
Webster AC, Nagler EV, Morton RL, Masson P (2017) Chronic kidney disease. Lancet (London, England) 389(10075):1238–1252. https://doi.org/10.1016/s0140-6736(16)32064-5
He FF, Gong Y, Li ZQ, Wu L, Jiang HJ, Su H, Zhang C, Wang YM (2018) A new pathogenesis of albuminuria: role of transcytosis. Cellular Physiol Biochem 47(3):1274–1286. https://doi.org/10.1159/000490223
Kibel A, Lukinac AM, Dambic V, Juric I, Relatic KS (2020) Oxidative stress in ischemic heart disease. Oxid Med Cell Longev 2020:6627144. https://doi.org/10.1155/2020/6627144
Scurt FG, Menne J, Brandt S, Bernhardt A, Mertens PR, Haller H, Chatzikyrkou C (2019) Systemic inflammation precedes microalbuminuria in diabetes. Kidney Int Rep 4(10):1373–1386. https://doi.org/10.1016/j.ekir.2019.06.005
Sangoi MB, de Carvalho JA, Tatsch E, Hausen BS, Bollick YS, Londero SW, Duarte T, Scolari R, Duarte MM, Premaor MO, Comim FV, Moretto MB, Moresco RN (2016) Urinary inflammatory cytokines as indicators of kidney damage in type 2 diabetic patients. Int J Clin Chem 460:178–183. https://doi.org/10.1016/j.cca.2016.06.028
Stewart MH, Lavie CJ, Shah S, Englert J, Gilliland Y, Qamruddin S, Dinshaw H, Cash M, Ventura H, Milani R (2018) Prognostic implications of left ventricular hypertrophy. Prog Cardiovasc Dis 61(5–6):446–455. https://doi.org/10.1016/j.pcad.2018.11.002
Dekkers IA, de Mutsert R, de Vries APJ, Rosendaal FR, Cannegieter SC, Jukema JW, le Cessie S, Rabelink TJ, Lamb HJ, Lijfering WM (2018) Determinants of impaired renal and vascular function are associated with elevated levels of procoagulant factors in the general population. J Thromb Haemost 16(3):519–528. https://doi.org/10.1111/jth.13935
Wendelboe AM, Raskob GE (2016) Global burden of thrombosis: epidemiologic aspects. Circ Res 118(9):1340–1347. https://doi.org/10.1161/circresaha.115.306841
Rabelink TJ, de Zeeuw D (2015) The glycocalyx–linking albuminuria with renal and cardiovascular disease. Nat Rev Nephrol 11(11):667–676. https://doi.org/10.1038/nrneph.2015.162
Xin Z, Liu S, Niu J, Xu M, Wang T, Lu J, Chen Y, Wang W, Ning G, Bi Y, Xu Y, Li M, Zhao Z (2021) The association of low-grade albuminuria with incident non-alcoholic fatty liver disease and non-invasive markers of liver fibrosis by glycaemia status. Liver Int 41(1):101–109. https://doi.org/10.1111/liv.14649
Huxley RR, Peters SA, Mishra GD, Woodward M (2015) Risk of all-cause mortality and vascular events in women versus men with type 1 diabetes: a systematic review and meta-analysis. Lancet Diabetes Endocrinol 3(3):198–206. https://doi.org/10.1016/s2213-8587(14)70248-7
Vlek AL, van der Graaf Y, Spiering W, Algra A, Visseren FL (2008) Cardiovascular events and all-cause mortality by albuminuria and decreased glomerular filtration rate in patients with vascular disease. J Intern Med 264(4):351–360. https://doi.org/10.1111/j.1365-2796.2008.01970.x
Ekinci EI, Barr ELM, Barzi F, Hughes JT, Lawton PD, Jones GRD, Hoy W, Cass A, Thomas M, Sinha A, Jerums G, O’Dea K, MacIsaac RJ, Maple-Brown LJ (2019) Is hyperfiltration associated with higher urine albumin-to-creatinine ratio at follow up among Indigenous Australians? The eGFR follow-up study. J Diabetes Complicat 33(5):343–349. https://doi.org/10.1016/j.jdiacomp.2019.02.005
Park M, Yoon E, Lim YH, Kim H, Choi J, Yoon HJ (2015) Renal hyperfiltration as a novel marker of all-cause mortality. J Am Soc Nephrol 26(6):1426–1433. https://doi.org/10.1681/asn.2014010115
Lin YS, Chiu FC, Lin JW, Hwang JJ, Caffrey JL (2010) Association of albuminuria and cancer mortality. Cancer Epidemiol Biomark Prev 19(11):2950–2957. https://doi.org/10.1158/1055-9965.Epi-10-0617
Charokopos A, Griffin M, Rao VS, Inker L, Sury K, Asher J, Turner J, Mahoney D, Cox ZL, Wilson FP, Testani JM (2019) Serum and urine albumin and response to loop diuretics in heart failure. Clin J Am Soc Nephrol 14(5):712–718. https://doi.org/10.2215/cjn.11600918
Funding
National Natural Science Foundation of China (grant no. 82002014), Natural Science Foundation of Guangdong Province (grant no. 2021A1515010107), the Project of Administration of Traditional Chinese Medicine of Guangdong Province of China (20221003), Science and Technology Projects of Guangzhou (grant no. 201903010097), Guangdong Provincial Key Laboratory of Coronary Heart Disease Prevention (Y0120220151). The funders had no role in the study design, data collection and analysis, decision to publish, nor preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
ZWY, WXB and YDQ contributed to the conception or design of the study. ZWY, YBF, JLH, BQF, GRZ contributed to the acquisition, analyses, and interpretation of data. ZWY, YBF, WXB drafted the manuscript. YDQ revised the manuscript critically. YDQ had all access to the data and is responsible for the overall content as guarantor. All authors contributed to refinement of the study protocol and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
All NHANES study protocols survey protocol was approved by the Ethics Review Committee of NCHS of the Centers for Disease Control and Prevention.
Consent to participate
All participants had provided written, informed consent for the use of their data. All procedures in this study were conducted in accordance with all the relevant guidelines.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, Zw., Fu, Yb., Wei, Xb. et al. Optimal threshold of urinary albumin-to-creatinine ratio (UACR) for predicting long-term cardiovascular and noncardiovascular mortality. Int Urol Nephrol 55, 1811–1819 (2023). https://doi.org/10.1007/s11255-023-03499-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03499-z