Abstract
Purpose
Although dyslipidemia can cause kidney damage, whether it independently contributes to the progression of chronic kidney disease (CKD) remains controversial. The research aims to evaluate the predictive value of serum lipids and their ratios in the progression of CKD.
Methods
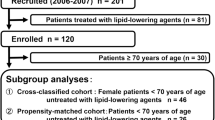
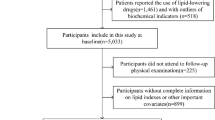
The retrospective, case–control study included 380 adult subjects with CKD stage 3–4 (G3-4) at baseline. The end point of follow-up was the progression of CKD, defined as a composite of renal function rapid decline [an annual estimated glomerular filtration rate (eGFR) decline > 5 mL/min/1.73 m2] or the new-onset end-stage renal disease (ESRD) [eGFR < 15 mL/min/1.73 m2]. Logistic regression analysis was performed to examine the association between CKD progression and lipid parameters. Receiver operating characteristic (ROC) curve analysis was used to evaluate the predictive power of lipid parameters in the progression of CKD.
Results
Over a median follow-up of 3.0 years, 96 participants (25.3%) developed CKD progression. In multivariable logistic regression analysis, logarithm-transformed urinary albumin-to-creatinine ratio (log ACR) [odds ratio (OR) 1.834;95% confidence interval (CI) 1.253–2.685; P = 0.002] and total cholesterol to high-density lipoprotein cholesterol ratio (TC/HDL-C) [OR 1.345; 95% CI 1.079–1.677; P = 0.008] were independently associated with CKD progression. The ROC curve showed the combined predictor of ACR and TC/HDL-C ratio was acceptable for CKD progression diagnosis (area under the ROC curve [AUC] = 0.716, sensitivity 50.0%, specificity 84.2%), and the cut-off value was − 0.98.
Conclusions
The combination of TC/HDL-C ratio and ACR had predictive value in the progression of CKD, and may help identify the high-risk population with CKD.


Similar content being viewed by others
Data availability
All data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Aleksandra Pikula ASB, Wang J (2015) Lipid and lipoprotein measurements and the risk of ischemic vascular events: Framingham Study. Neurology 84(5):472–479
Diamond JR (1991) Analogous pathobiologic mechanisms in glomerulosclerosis and atherosclerosis. Kidney Int Suppl 31:S29-34
Moorhead JF, Chan MK, El-Nahas M (1982) Lipid nephrotoxicity in chronic progressive glomerular and tubulo-interstitial disease. Lancet 2(8311):1309–1311
Merscher S, Pedigo CE, Mendez AJ (2014) Metabolism, energetics, and lipid biology in the podocyte—cellular cholesterol-mediated glomerular injury. Front Endocrinol (Lausanne) 5:169
Johnson AC, Stahl A, Zager RA (2005) Triglyceride accumulation in injured renal tubular cells: alterations in both synthetic and catabolic pathways. Kidney Int 67(6):2196–2209
Trevisan R, Dodesini AR, Lepore G (2006) Lipids and renal disease. J Am Soc Nephrol 17(4 Suppl 2):S145-147
Cachofeiro V, Goicochea M, de Vinuesa SG, Oubina P, Lahera V, Luno J (2008) Oxidative stress and inflammation, a link between chronic kidney disease and cardiovascular disease. Kidney Int Suppl 111:S4-9
Rajendran P, Rengarajan T, Thangavel J et al (2013) The vascular endothelium and human diseases. Int J Biol Sci 9(10):1057–1069
Joles JA, Kunter U, Janssen U et al (2000) Early mechanisms of renal injury in hypercholesterolemic or hypertriglyceridemic rats. J Am Soc Nephrol 11(4):669–683
Blanco S, Vaquero M, Gomez-Guerrero C, Lopez D, Egido J, Romero R (2005) Potential role of angiotensin-converting enzyme inhibitors and statins on early podocyte damage in a model of type 2 diabetes mellitus, obesity, and mild hypertension. Am J Hypertens 18(4 Pt 1):557–565
Rahman M, Yang W, Akkina S et al (2014) Relation of serum lipids and lipoproteins with progression of CKD: the CRIC study. Clin J Am Soc Nephrol 9(7):1190–1198
Nam KH, Chang TI, Joo YS et al (2019) Association between serum high-density lipoprotein cholesterol levels and progression of chronic kidney disease: results from the KNOW-CKD. J Am Heart Assoc 8(6):e011162
Bowe B, Xie Y, Xian H, Balasubramanian S, Al-Aly Z (2016) Low levels of high-density lipoprotein cholesterol increase the risk of incident kidney disease and its progression. Kidney Int 89(4):886–896
Sanchez-Inigo L, Navarro-Gonzalez D, Pastrana-Delgado J, Fernandez-Montero A, Martinez JA (2016) Association of triglycerides and new lipid markers with the incidence of hypertension in a Spanish cohort. J Hypertens 34(7):1257–1265
Edwards MK, Blaha MJ, Loprinzi PD (2017) Atherogenic index of plasma and triglyceride/high-density lipoprotein cholesterol ratio predict mortality risk better than individual cholesterol risk factors, among an older adult population. Mayo Clin Proc 92(4):680–681
Zhang X, Wang B, Yang J et al (2019) Serum lipids and risk of rapid renal function decline in treated hypertensive adults with normal renal function. Am J Hypertens 32(4):393–401
Schaeffner ES, Kurth T, Curhan GC et al (2003) Cholesterol and the risk of renal dysfunction in apparently healthy men. J Am Soc Nephrol 14(8):2084–2091
Zuo PY, Chen XL, Liu YW, Zhang R, He XX, Liu CY (2015) Non-HDL-cholesterol to HDL-cholesterol ratio as an independent risk factor for the development of chronic kidney disease. Nutr Metab Cardiovasc Dis 25(6):582–587
Zhang L, Yuan Z, Chen W et al (2014) Serum lipid profiles, lipid ratios and chronic kidney disease in a Chinese population. Int J Environ Res Public Health 11(8):7622–7635
Bikbov B, Purcell CA, Levey AS et al (2020) Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 395(10225):709–733
Zhang L, Wang F, Wang L et al (2012) Prevalence of chronic kidney disease in China: a cross-sectional survey. Lancet 379(9818):815–822
Huang Y, Gao L, Xie X, Tan SC (2014) Epidemiology of dyslipidemia in Chinese adults: meta-analysis of prevalence, awareness, treatment, and control. Popul Health Metr 12(1):28
Inker LA, Astor BC, Fox CH et al (2014) KDOQI US commentary on the 2012 KDIGO clinical practice guideline for the evaluation and management of CKD. Am J Kidney Dis 63(5):713–735
Levin A, Stevens PE (2014) Summary of KDIGO 2012 CKD guideline: behind the scenes, need for guidance, and a framework for moving forward. Kidney Int 85(1):49–61
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Visconti L, Benvenga S, Lacquaniti A et al (2016) Lipid disorders in patients with renal failure: role in cardiovascular events and progression of chronic kidney disease. J Clin Transl Endocrinol 6:8–14
Kwan BC, Kronenberg F, Beddhu S, Cheung AK (2007) Lipoprotein metabolism and lipid management in chronic kidney disease. J Am Soc Nephrol 18(4):1246–1261
Bulbul MC, Dagel T, Afsar B et al (2018) Disorders of lipid metabolism in chronic kidney disease. Blood Purif 46(2):144–152
Mikolasevic I, Zutelija M, Mavrinac V, Orlic L (2017) Dyslipidemia in patients with chronic kidney disease: etiology and management. Int J Nephrol Renovasc Dis 10:35–45
Vaziri ND (2006) Dyslipidemia of chronic renal failure: the nature, mechanisms, and potential consequences. Am J Physiol Renal Physiol 290(2):F262-272
Kronenberg F (2018) HDL in CKD-the devil is in the detail. J Am Soc Nephrol 29(5):1356–1371
Rysz J, Gluba-Brzozka A, Rysz-Gorzynska M, Franczyk B (2020) The role and function of HDL in patients with chronic kidney disease and the risk of cardiovascular disease. Int J Mol Sci 21(2):601
Ji B, Zhang S, Gong L et al (2013) The risk factors of mild decline in estimated glomerular filtration rate in a community-based population. Clin Biochem 46(9):750–754
Stevens LA, Schmid CH, Greene T et al (2010) Comparative performance of the CKD epidemiology collaboration (CKD-EPI) and the modification of diet in renal disease (MDRD) study equations for estimating GFR levels above 60 mL/min/1.73 m2. Am J Kidney Dis 56(3):486–495
Funding
This work was financially supported by Wuhan Health and Family Planning Commission research projects (No. WX18Q31).
Author information
Authors and Affiliations
Contributions
HW and JD conceived and designed the study. WL screened the abstract and full text, assessed studies and drafted the manuscript. ZD performed statistical analyses. HW revised the manuscript. All authors read the manuscript and approved the final version.
Corresponding authors
Ethics declarations
Conflict of interest
All the authors declared no competing interests.
Ethical approval
This study was performed in accordance with the ethical principles of the Declaration of Helsinki and was approved by the ethics Committee of Wuhan Fourth Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, China (KY2021-0021-01). All participants have written informed consent before the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, W., Du, Z., Wei, H. et al. Total cholesterol to high-density lipoprotein cholesterol ratio is independently associated with CKD progression. Int Urol Nephrol 54, 2057–2063 (2022). https://doi.org/10.1007/s11255-021-03099-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-021-03099-9