Abstract
Purpose
Adipose distribution and sarcopenia could better assess kidney transplantation outcomes than body mass index (BMI) and have been poorly evaluated among obese and overweight recipients. We aimed to evaluate morphometric radiologic markers to predict post-operative dialysis within this population.
Methods
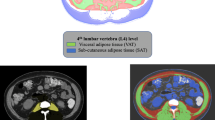
We conducted a retrospective study including patients with a BMI > 25 kg/m2 undergoing kidney transplantation during 5 years. Subcutaneous adipose tissue surface (SAT), visceral adipose tissue surface (VAT), and psoas surface were measured on CT scans sections. A model predictive of post-transplantation dialysis was elaborated through a multivariable logistic regression and was compared to a model including only BMI.
Results
Overall, 248 patients were included whom mean (SD) BMI and age were, respectively, 29.7 kg/m2 (3.6) and 56 years (12.7). Of them, 83 (33.5%) needed dialysis: 14 (5.7%) for primary kidney failure and 69 (27.8%) for delayed kidney function. On multivariable analysis, SAT, VAT and deceased donor were significantly associated with post-operative dialysis (respectively, OR [95%CI]:1.6 [1.1–2.6], 1.6[1.1–2.6], and 7.5 [1.6–56]). The area under the curve of this predictive model was 0.70 versus 0.64 for a BMI-based model.
Conclusion
High VAT and SAT were associated with post-transplantation dialysis. A predictive model based on these morphometrics could provide a better appreciation of graft recovery after transplantation among obese and overweight recipients. External validation is needed.


Similar content being viewed by others
Data availability
Data are available.
Code availability
Not applicable.
References
World Health Organization (WHO) Obesity and overweight. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
Jha V, Garcia-Garcia G, Iseki K, Li Z, Naicker S, Plattner B, Saran R, Wang AY-M, Yang C-W (2013) Chronic kidney disease: global dimension and perspectives. Lancet Lond Engl 382:260–272
Hill CJ, Courtney AE, Cardwell CR et al (2015) Recipient obesity and outcomes after kidney transplantation: a systematic review and meta-analysis. Nephrol Dial Transpl Off Publ Eur Dial Transpl Assoc - Eur Ren Assoc 30:1403–1411
Lynch RJ, Ranney DN, Shijie C, Lee DS, Samala N, Englesbe MJ (2009) Obesity, surgical site infection, and outcome following renal transplantation. Ann Surg 250:1014–1020
Røine E, Bjørk IT, Oyen O (2010) Targeting risk factors for impaired wound healing and wound complications after kidney transplantation. Transpl Proc 42:2542–2546
Meier-Kriesche H-U, Arndorfer JA, Kaplan B (2002) The impact of body mass index on renal transplant outcomes: a significant independent risk factor for graft failure and patient death. Transplantation 73:70–74
Aalten J, Christiaans MH, de Fijter H, Hené R, van der Heijde JH, Roodnat J, Surachno J, Hoitsma A (2006) The influence of obesity on short- and long-term graft and patient survival after renal transplantation. Transpl Int Off J Eur Soc Organ Transpl 19:901–907
Chang SH, Coates PTH, McDonald SP (2007) Effects of body mass index at transplant on outcomes of kidney transplantation. Transplantation 84:981–987
Scherer PE (2006) Adipose tissue: from lipid storage compartment to endocrine organ. Diabetes 55:1537–1545
Lemieux S, Després JP (1994) Metabolic complications of visceral obesity: contribution to the aetiology of type 2 diabetes and implications for prevention and treatment. Diabete Metab 20:375–393
Bergstrom RW, Newell-Morris LL, Leonetti DL, Shuman WP, Wahl PW, Fujimoto WY (1990) Association of elevated fasting C-peptide level and increased intra-abdominal fat distribution with development of NIDDM in Japanese-American men. Diabetes 39:104–111
Dobbelsteyn CJ, Joffres MR, MacLean DR, Flowerdew G (2001) A comparative evaluation of waist circumference, waist-to-hip ratio and body mass index as indicators of cardiovascular risk factors. The Canadian heart health surveys. Int J Obes Relat Metab Disord J Int Assoc Study Obes 25:652–661
Kuk JL, Katzmarzyk PT, Nichaman MZ, Church TS, Blair SN, Ross R (2006) Visceral fat is an independent predictor of all-cause mortality in men. Obes Silver Spring Md 14:336–341
Mitsui Y, Sadahira T, Araki M, Maruyama Y, Wada K, Tanimoto R, Kobayashi Y, Watanabe M, Watanabe T, Nasu Y (2018) Clinical impact of abdominal fat distribution measured by 3-D computed tomography volumetry on post-transplant renal function in recipients after living kidney transplantation: a retrospective study. Clin Exp Nephrol. https://doi.org/10.1007/s10157-018-1643-6
Cruz-Jentoft AJ, Bahat G, Bauer J et al (2019) Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing. https://doi.org/10.1093/ageing/afz046
Pereira RA, Cordeiro AC, Avesani CM, Carrero JJ, Lindholm B, Amparo FC, Amodeo C, Cuppari L, Kamimura MA (2015) Sarcopenia in chronic kidney disease on conservative therapy: prevalence and association with mortality. Nephrol Dial Transpl Off Publ Eur Dial Transpl Assoc - Eur Ren Assoc 30:1718–1725
de Souza VA, Oliveira D, Barbosa SR, Corrêa JO, do A, Colugnati FAB, Mansur HN, Fernandes NM da S, Bastos MG, (2017) Sarcopenia in patients with chronic kidney disease not yet on dialysis: analysis of the prevalence and associated factors. PLoS ONE 12:e0176230
Fang H, Berg E, Cheng X, Shen W (2018) How to best assess abdominal obesity. Curr Opin Clin Nutr Metab Care 21:360–365
Pinar U, Renard Y, Bedretdinova D, Parier B, Hammoudi Y, Irani J, Bessede T (2020) Temporary contraindication of obese recipients in kidney transplantation: a new morphometric tool for decision support. Clin Transpl 34:e13829
Fearon K, Strasser F, Anker SD et al (2011) Definition and classification of cancer cachexia: an international consensus. Lancet Oncol 12:489–495
Irish WD, Ilsley JN, Schnitzler MA, Feng S, Brennan DC (2010) A risk prediction model for delayed graft function in the current era of deceased donor renal transplantation. Am J Transplant Off J Am Soc Transpl Am Soc Transpl Surg 10:2279–2286
Carroll JF, Fulda KG, Chiapa AL, Rodriquez M, Phelps DR, Cardarelli KM, Vishwanatha JK, Cardarelli R (2009) Impact of race/ethnicity on the relationship between visceral fat and inflammatory biomarkers. Obes Silver Spring Md 17:1420–1427
Lee HH, Kang SK, Yoon YE, Huh KH, Kim MS, Kim SI, Kim YS, Han WK (2017) Impact of the ratio of visceral to subcutaneous adipose tissue in donor nephrectomy patients. Transpl Proc 49:940–943
Pek GXW, Ngoh CLY, Teo BW, Vathsala A, Goh BYS, Yong CHR, Raman L, Tiong HY (2018) Visceral obesity in Asian living kidney donors significantly impacts early renal function after donor nephrectomy. World J Urol. https://doi.org/10.1007/s00345-018-2566-2
Hori S, Miyake M, Morizawa Y et al (2018) Impact of preoperative abdominal visceral adipose tissue area and nutritional status on renal function after donor nephrectomy in Japanese living donors for renal transplantation. Ann Transpl 23:364–376
Ibrahim MM (2010) Subcutaneous and visceral adipose tissue: structural and functional differences. Obes Rev Off J Int Assoc Study Obes 11:11–18
Item F, Konrad D (2012) Visceral fat and metabolic inflammation: the portal theory revisited. Obes Rev Off J Int Assoc Study Obes 13(Suppl 2):30–39
Fain JN, Madan AK, Hiler ML, Cheema P, Bahouth SW (2004) Comparison of the release of adipokines by adipose tissue, adipose tissue matrix, and adipocytes from visceral and subcutaneous abdominal adipose tissues of obese humans. Endocrinology 145:2273–2282
Yu J-Y, Choi W-J, Lee H-S, Lee J-W (2019) Relationship between inflammatory markers and visceral obesity in obese and overweight Korean adults: an observational study. Medicine (Baltimore) 98:e14740
von Düring ME, Jenssen T, Bollerslev J, Godang K, Hartmann A, Åsberg A (2018) Arterial stiffness is associated with visceral fat mass in kidney transplanted patients-a nationwide cohort study. Clin Transpl 32:e13341
Toto-Moukouo JJ, Achimastos A, Asmar RG, Hugues CJ, Safar ME (1986) Pulse wave velocity in patients with obesity and hypertension. Am Heart J 112:136–140
Blacher J, Pannier B, Guerin AP, Marchais SJ, Safar ME (1979) London GM (1998) Carotid arterial stiffness as a predictor of cardiovascular and all-cause mortality in end-stage renal disease. Hypertens Dallas Tex 32:570–574
Freedland ES (2004) Role of a critical visceral adipose tissue threshold (CVATT) in metabolic syndrome: implications for controlling dietary carbohydrates: a review. Nutr Metab 1:12
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Contributions
UP: participated in research design, data collection, writing of the paper, performance of the research, data analysis. AM: participated in research design, writing of the paper, performance of the research, data analysis. YR: participated in research design and data analysis. XR: participated in research design and data analysis. CL: participated in research design, writing of the paper and data collection. BB: participated in writing of the paper and data collection. MZ: participated in writing of the paper and data collection. JI: participated in research design, writing of the paper and data collection. TB: participated in research design, writing of the paper, performance of the research, data analysis.
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest to declare.
Informed consent
For this study, oral and written consent was obtained for every patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pinar, U., Mageau, A., Renard, Y. et al. Pre-transplant morphometry by computed tomography scan and post-transplant dialysis risk in overweight or obese kidney transplant recipients. Int Urol Nephrol 53, 2469–2475 (2021). https://doi.org/10.1007/s11255-021-02995-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-021-02995-4