Abstract
Purpose
The main purpose of this study is to determine the correlation between the serum IGF-1 concentration and certain cardiac indexes in hemodialysis patients.
Methods
The study was conducted at the Clinical Center of Montenegro and three regional hemodialysis centers. The echocardiographic studies were performed the day after the hemodialysis sessions. Blood samples were taken before dialysis for the measurement of IGF1 and PTH.
Results
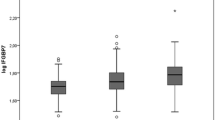
A total of 102 patients were divided into two groups according to their left-ventricular ejection fraction (EF). Patients in the group with the higher EF had higher IGF-1 concentration (p = 0.024). IGF-1 was positively correlated with EF (ρ = 0.251, p = 0.012), and negatively correlated with LVMI (ρ = − 0.621, p < 0.001), SW (ρ = − 0.632, p < 0.001), and LW (ρ = − 0.632, p < 0.001). Multiple linear regression analysis was performed to determine the possible independent association between the EF and IGF-1 and the clinical data. The age of patients, their gender, and smoking habits did not have any combined influence on EF, but IGF-1 had a strong influence and was independently associated with the ejection fraction.
Conclusion
Our results may indicate the possible protective role of IGF-1 in the maintenance of heart structure and function in hemodialysis patients.

Similar content being viewed by others
References
Alani H et al (2014) Cardiovascular co-morbidity in chronic kidney disease: current knowledge and future research needs. World J Nephrol 3(4):156–168
Borges MCC et al (2017) Malnutrition Inflammation Score cut-off predicting mortality in maintenance hemodialysis patients. Clin Nutr 17(4):63–67
Sun J et al (2016) Biomarkers and cardiovascular disease and mortality risk in patients with advanced CKD. Clin J Am SocNephrol 11(9):1163–1172
Sood MM et al (2008) Left ventricular dysfunction in hemodialysis population. NDT Plus 4(6):199–205
Momeni A et al (2016) Reduction of left ventricular ejection fraction after a 12-month follow-up in hemodialysis patients. J Ren Inj Prev 5(1):8–11
Menon V, Gul A, Sarnak MJ (2005) Cardiovascular risk factors in chronic kidney disease. Kidney Int 68(5):1413–1418
Conti E et al (2004) Insulin like growth factor-1 as a vascular protective factor. Circulation 110(5):2260–2265
Torella D, Rota M, Nurzynska D et al (2004) Cardiac stem cell and myocyte aging, heart failure, and insulin-like growth factor-1 overexpression. Circ Res 94(10):514–524
Youngman O (2012) The insulin-like growth factor system in chronic kidney disease: pathophysiology and therapeutic opportunities. Kidney Res ClinPract 31(11):26–37
Burgers AMG et al (2011) IGF-I and mortality: a meta-analysis. J Clin Endocrinol Metab 96(9):2912–2920
Kamenicky P et al (2014) Growth hormone, insulin-like growth factor-1, and the kidney: pathophysiological and clinical implications. Endocr Rev 35(47):234–281
Andreassen M et al (2009) IGF1 as predictor of all cause mortality and cardiovascular disease in an elderly population. Eur J Endoc 160(6):25–31
Zand L, Kumar R (2016) Serum parathyroid hormone concentrations and clinical outcomes in ESRD: a call for targeted clinical trials. Semin Dial 29(3):184–188
Levin A, Stevens PE, Bilous RW, Coresh J, De Francisco ALM, De Jong PE, Griffith KE, Hemmelgarn BR, Iseki K, Lamb EJ, Levey AS, Riella MC, Shlipak MG, Wang H, White CT, Winearls CG, Kidney disease: Improving global outcomes (KDIGO) CKD work group (2013) KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl 3(1):1–150
Mitchell C et al (2019) Guidelines for performing a comprehensive transthoracic echocardiographic examination in adults: recommendations from the American Society of echocardiography. J Am Soc Echocardiogr 32(1):1–64
Ponikowski P et al (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 37:2129–2200
Jia T, Gama Axelsson T, Heimbürger O et al (2014) IGF1 and survival in ESRD. Clin J Am Soc Nephrol 9(7):120–127
Nilsson E et al (2016) A cohort study of insulin-like growth factor 1 and mortality in hemodialysis patients. Clin Kidney J 9(4):148–152
Bleyer AJ, Tell GS et al (2006) Characteristics of sudden death in hemodialysis patients. Kidney Int 69(5):2268–2273
Yamada S et al (2010) Prognostic value of reduced left ventricular ejection fraction at start of hemodialysis therapy on cardiovascular and all-cause mortality in end-stage renal disease patients. Clin J Am Soc Nephrol. https://doi.org/10.2215/CJN.00050110
Zoccali C, Benedetto FA, Mallamaci F, Tripepi G, Giacone G, Cataliotti A, Seminara G, Stancanelli B, Malatino LS (2004) Prognostic value of echocardiographic indicators of leftventricular systolic function in asymptomatic dialysis patients. J Am Soc Nephrol. 15(8):1029–1037
Ganda A, Weiner SD, Chudasama NL, Valeri AM, Jadoon A, Shimbo D et al (2012) Echocardiographic changes following hemodialysis initiation in patients with advanced chronic kidney disease and symptomatic heart failure with reduced ejection fraction. Clin Nephrol 77(9):366–375
Ritz E, Bommer J (2009) Cardiovascular problems on hemodialysis: current deficits and potential improvement. Clin J Am Soc Nephrol 4(7):71–78
Adrian DS (2012) Exploring metabolic dysfunction in chronic kidney disease. Nutr Metab 98(1):36
Abdulle AM, Gillett MP, Abouchacra S, Sabri SM, Rukhaimi MA, Obineche EN, Singh J (2007) Low IGF1 levels are associated with cardiovascular risk factors in haemodialysis patients. Mol Cell Biochem 302(6):195–201
Rees L (2016) Growth hormone therapy in children with CKD after more than two decades of practice. Pediatr Nephrol 31(14):1421–1435
Acknowledgements
This research was supported by the technical and medical staff of the Clinic for Nephrology and the Centre for Laboratory Diagnostic of the Clinical Centre of Montenegro.
Funding
There are no grants or other funding for the conducted survey.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interests.
Ethics approval
This study was approved by the Ethical Committee of the Clinical Centre of Montenegro, and was performed in accordance with the relevant ethical standards and the Declaration of Helsinki.
Consent to participate
All patients gave their informed consent to participate in the study.
Consent for publication
All authors declare their consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Prelevic, V., Antunovic, T., Radunovic, D. et al. Decreased insulin-like growth factor-1 (IGF-1) concentration correlates with reduced left-ventricle ejection fraction (LVEF) in hemodialysis patients. Int Urol Nephrol 52, 2385–2391 (2020). https://doi.org/10.1007/s11255-020-02595-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-020-02595-8