Abstract
Background
The rehabilitation of post-prostatectomy urinary incontinence has traditionally focused on pelvic floor strengthening exercise. The goal of this study was to determine whether an individualized pelvic physical therapy (PT) program aimed at normalizing both underactive and overactive pelvic floor dysfunction (PFD) can result in improvement in post-prostatectomy stress urinary incontinence (SUI) and pelvic pain.
Methods
A retrospective chart review of 136 patients with post-prostatectomy SUI and treated with pelvic PT. Patients were identified as having either underactive, overactive, or mixed-type PFD and treated accordingly with a tailored program to normalize pelvic floor function. Outcomes including decrease in SUI as measured in pad usage per day and pain rated on the numeric pain rating scale.
Results
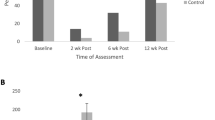
Twenty five patients were found to have underactive PFD and were treated with strengthening. Thirteen patients had overactive PFD and were treated with relaxation training. Ninety eight patients had mixed-type PFD and were treated with a combination of relaxation training followed by strengthening. Patients demonstrated statistically significant decrease in pad usage per day (p < 0.001), decreased pelvic pain (p < 0.001), and increased pelvic floor strength (p = 0.049), even in patients who received predominantly pelvic floor relaxation training to normalize pelvic floor overactivity.
Conclusions
A majority of post-prostatectomy men with SUI have pelvic floor overactivity in addition to pelvic floor underactivity. An individualized pelvic PT program aimed at normalizing pelvic floor function (as opposed to a pure Kegel strengthening program) can be helpful in reducing SUI and pelvic pain.
Similar content being viewed by others
References
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U et al (2003) The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn 21(2):167–178
Reynolds WS, Ahikavoc SA, Katz MH, Zagaja GP, Shalhav AL, Zorn KC (2010) Analysis of continence rates following robot-assisted radical prostatectomy strict leak-free and pad-free continence. Urology 75(2):431–438
Bauer RM, Gozzi C, Hubner W, Nitti VW, Novara G, Peterson A et al (2011) Contemporary management of postprostatectomy incontinence. Eur Urol 59(6):985–996
Anderson CA, Omar MI, Campbell SE, Hunter KF, Cody JD, Glazener CM (2015) Conservative management for postprostatectomy urinary incontinence. Cochrane Database Syst Rev 1:CD001843. https://doi.org/10.1002/14651858.CD001843.pub5
Dorey G, Glazener C, Buckley B, Cochran C, Moore K (2009) Developing a pelvic floor muscle training regimen for use in a trial intervention. Physiotherapy 95(3):199–209
Goode PS, Burgio K, Johnson TM, Clay OJ, Markland AD, Burkhardt JH et al (2011) Behavioral therapy with or without biofeedback and pelvic floor electrical stimulation for persistent postprostatectomy incontinence: a randomized controlled trial. JAMA 305(2):151–159
Manassero F, Traversi C, Ales V, Pistolesi D, Panicucci E, Valent F et al (2007) Contribution of early intensive prolonged pelvic floor exercises on urinary continence recovery after bladder neck-sparing radical prostatectomy: results of a prospective controlled randomized trial. Neurourol Urodyn 26(7):985–989
Overgard M, Angelsen A, Lydersen S, Morkved S (2008) Does physiotherapist-guided pelvic floor muscle training reduce urinary incontinence after radical prostatectomy? A randomised controlled trial. Eur Urol 54(2):438–448
Chen YC, Lin PH, Jou YY, Lin VC (2017) Surgical treatment for urinary incontinence after prostatectomy: a meta-analysis and systematic review. PLoS One 12(5):1–19
Davis NF, Kheradmand F, Creagh T (2013) Injectable biomaterials for the treatment of stress urinary incontinence: their potential and pitfalls as urethral bulking agents. Int Urogynecol J 24(6):913–919
Chughtai B, Lee R, Sandhu J, Te A, Kaplan S (2013) Conservative treatment for postprostatectomy incontinence. Rev Urol 15(2):61–66
Bradley MH, Rawlins A, Brinker CA (2017) Physical therapy treatment of pelvic pain. Phys Med Rehabil Clin N Am 28:589–601
Messelink B, Benson T, Berghmans B, Bo K, Corcos J, Fowler C et al (2005) Standardization of terminology of pelvic floor muscle function and dysfunction: report from the pelvic floor clinical assessment group of the International Continence Society. Neurourol Urodyn 24(4):374–380
Miller J, Sampselle CM, Ashton-Miller JA, Hong GR, DeLancey JO (2008) Clarification and confirmation of the effect of volitional pelvic floor muscle contraction to preempt urine loss (The Knack Maneuver) in stress incontinent women. Int Urogynecol J Pelvic Floor Dysfunct 19(6):773–782
FitzGerald MP, Kotarinos R (2003) Rehabilitation of the short pelvic floor II: treatment of the patient with the short pelvic floor. Int Urogynecol J Pelvic Floor Dysfunct 13(4):269–275
Acknowledgements
This work was supported by a grant from the David M. Crowley Foundation to the Department of Urology at UT Southwestern Medical Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors report financial conflicts of interest with this work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Scott, K.M., Gosai, E., Bradley, M.H. et al. Individualized pelvic physical therapy for the treatment of post-prostatectomy stress urinary incontinence and pelvic pain. Int Urol Nephrol 52, 655–659 (2020). https://doi.org/10.1007/s11255-019-02343-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-019-02343-7