Abstract
Purpose
There is a paucity of data regarding urology involvement in the management of lower urinary tract injuries (LUTI). We seek to analyze the incidence and epidemiology of LUTI with special attention to trends in urology consultation.
Methods
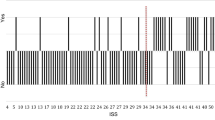
A retrospective review was conducted of patients presenting to our Level I trauma center with LUTI from 2002 to 2016. Demographics, mechanism of injury, associated injuries, injury severity score (ISS), American Association for the Surgery of Trauma (AAST) injury scales, and clinical hospital course were analyzed.
Results
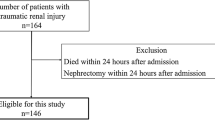
A total of 140 patients (0.47% of all trauma patients) were identified with LUTI, with 72.1% of these presenting with blunt trauma. Bladder injuries were more common than urethral injuries (79% vs. 14%) with 6% of patients having both. In-hospital mortality was 9.2% (13/140). Among patients with LUTI, 115 patients (82%) received urology consultation. There was no significant difference in sex, age, or LOS (hospital and ICU) between the groups. The consult group had a lower mean ISS (21.7 vs 27.9, p = 0.034), but a higher mean AAST bladder injury scale (2.57 vs 2.00, p = 0.016), than the non-consult group. There was a statistically significant difference in the diagnosis methods between the two groups (χ2 test of independence, p = 0.002).
Conclusion
Urology service is important in the management of LUTI with high AAST injury scale. While further study is needed to look at degree of urology service involvement in the management of LUTI, we recommend a consultation for severe LUTI or when the management of injuries is out of the comfort zone of the trauma surgeons. Whether consultation is obtained or not, there is room for improvement in appropriate work up of lower urinary tract injury.

Similar content being viewed by others
References
Johnsen NV, Dmochowski RR, Young JB et al (2017) Epidemiology of blunt lower urinary tract trauma with and without pelvic fracture. Urology 102:234–239
Kong JP, Bultitude MF, Royce P, Gruen RL, Cato A, Corcoran NM (2011) Lower urinary tract injuries following blunt trauma: a review of contemporary management. Rev Urol 13(3):119–130
Zaid UB, Bayne DB, Harris CR et al (2015) Penetrating trauma to the ureter, bladder, and urethra. Curr Trauma Rep 1(2):119–124
Lumen N, Kuehhas FE, Djakovic N et al (2015) Review of the current management of lower urinary tract injuries by the EAU trauma guidelines panel. Eur Urol 67(5):925–929
Johnsen NV, Young JB, Reynolds WS, Kaufman MR, Milam DF, Guillamondegui OD, Dmochowski RR (2016) Evaluating the role of operative repair of extraperitoneal bladder rupture following blunt pelvic trauma. J Urol 195(3):661–665. https://doi.org/10.1016/j.juro.2015.08.081
Morey AF, Hernandez J, McAninch JW (1999) Reconstructive surgery for trauma of the lower urinary tract. Urol Clin N A 26(1):49–60
Gomez RG, Ceballos L, Coburn M et al (2004) Consensus statement on bladder injuries. BJU Int 94:27–32
Udekwu PO, Gurkin B, Oller DW (1996) The use of computed tomography in blunt abdominal injuries. Am Surg 62:56–59
Corriere JN, Sandler CM (1986) Management of the ruptured bladder: seven years of experience with 111 cases. J Trauma 26:830–833
Cass A, Luxenberg M (1987) Features of 164 bladder ruptures. J Urol 138(4 Part 1):743–745
Bjurlin MA, Fantus RJ, Mellett MM, Goble SM (2009) Genitourinary injuries in pelvic fracture morbidity and mortality using the National Trauma Data Bank. J Trauma 67:1033–1039
Sandler CM, Goldman SM, Kawashima A (1998) Lower urinary tract trauma. World J Urol 16(1):69–75
Morey AF, Iverson AJ, Swan A, Harmon WJ, Spore SS, Bhayani S, Brandes SB (2001) Bladder rupture after blunt trauma: guidelines for diagnostic imaging. J Trauma Acute Care Surg 51(4):683–686
Auerbach AD, Rasic MA, Sehgal N, Ide B, Stone B, Maselli J (2007) Opportunity missed. Arch Intern Med 167(21):2338
Andrich DE, Day AC, Mundy AR (2007) Proposed mechanisms of lower urinary tract injury in fractures of the pelvic ring. BJU Int 100:567–573
Morshed S, Knops S, Jurkovich GJ, Wang J, MacKenzie E, Rivara FP (2015) The impact of trauma-center care on mortality and function following pelvic ring and acetabular injuries. JBJS 97(4):265–272
Horiguchi A, Shinchi M, Masunaga A, Okubo K, Kawamura K, Ojima K, Azuma R (2017) Primary realignment for pelvic fracture urethral injury is associated with prolonged time to urethroplasty and increased stenosis complexity. Urology 108:184–189
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Michael Ernst, Amanda Sherman, Teresa Danforth, and W. Alan Guo declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ernst, M., Sherman, A., Danforth, T. et al. Lower urinary tract injury: is urology consultation necessary?. Int Urol Nephrol 52, 489–494 (2020). https://doi.org/10.1007/s11255-019-02326-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-019-02326-8