Abstract
Purpose
To assess whether the preoperative 1-h pad test could predict postoperative urinary incontinence and quality of life after robot-assisted radical prostatectomy.
Methods
A total of 329 patients who underwent robot-assisted radical prostatectomy between 2013 and 2016 were prospectively enrolled in this study. These patients were divided into the preoperative urinary continence group and the preoperative urinary incontinence group according to the 1-h pad test. The time to achieve urinary continence, lower urinary tract function evaluated by uroflowmetry and post-voided residual urine volume, and quality of life evaluated by King’s Health Questionnaire and International Consultation on Incontinence Questionnaire-Short Form were compared between these two groups.
Results
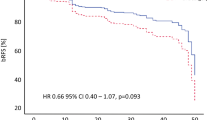
There were 190 patients (58%) in the preoperative urinary continence group (1-h pad test ≤ 2 g) and 139 patients (42%) in the preoperative urinary incontinence group (1-h pad test > 2 g). In the preoperative urinary continence/incontinence groups, 83%/76% of patients achieved continence within 12 months, respectively, and urinary incontinence remained significantly longer in the preoperative incontinence group than in the preoperative continence group (P = 0.042). Although there were no significant differences in all quality of life items between the two groups before surgery, several items were significantly higher in the preoperative urinary continence group.
Conclusion
Achievement of urinary continence and improvement of urinary quality of life are delayed in patients with preoperative urinary incontinence assessed by the 1-h pad test. The preoperative 1-h pad test could be a useful predictor of prolonged urinary incontinence and poor quality of life after robot-assisted radical prostatectomy.







Similar content being viewed by others
References
Patel VR, Sivaraman A, Coelho RF, Chauhan S, Palmer KJ, Orvieto MA, Camacho I, Coughlin G, Rocco B (2011) Pentafecta: a new concept for reporting outcomes of robot-assisted laparoscopic radical prostatectomy. Eur Urol 59(5):702–707. https://doi.org/10.1016/j.eururo.2011.01.032
Jereczek-Fossa BA, Zerini D, Fodor C, Santoro L, Maucieri A, Gerardi MA, Vischioni B, Cambria R, Garibaldi C, Cattani F, Vavassori A, Matei DV, Musi G, De Cobelli O, Orecchia R (2014) Reporting combined outcomes with Trifecta and survival, continence, and potency (SCP) classification in 337 patients with prostate cancer treated with image-guided hypofractionated radiotherapy. BJU Int 114(6b):E3–E10. https://doi.org/10.1111/bju.12530
Van Kampen M, Geraerts I, De Weerdt W, Van Poppel H (2009) An easy prediction of urinary incontinence duration after retropubic radical prostatectomy based on urine loss the first day after catheter withdrawal. J Urol 181(6):2641–2646. https://doi.org/10.1016/j.juro.2009.02.025
Murphy G, Haddock P, Doak H, Jackson M, Dorin R, Meraney A, Kesler S, Staff I, Wagner JR (2015) Urinary bother as a predictor of postsurgical changes in urinary function after robotic radical prostatectomy. Urology 86(4):817–823. https://doi.org/10.1016/j.urology.2015.04.041
Nguyen L, Jhaveri J, Tewari A (2008) Surgical technique to overcome anatomical shortcoming: balancing post-prostatectomy continence outcomes of urethral sphincter lengths on preoperative magnetic resonance imaging. J Urol 179(5):1907–1911. https://doi.org/10.1016/j.juro.2008.01.036
Tan HJ, Xiong S, Laviana AA, Chuang RJ, Treat E, Walsh PC, Hu JC (2016) Technique and outcomes of bladder neck intussusception during robot-assisted laparoscopic prostatectomy: A parallel comparative trial. Urol Oncol 34(12):529.e521–529.e527. https://doi.org/10.1016/j.urolonc.2015.01.012
You YC, Kim TH, Sung GT (2012) Effect of bladder neck preservation and posterior urethral reconstruction during robot-assisted laparoscopic radical prostatectomy for urinary continence. Korean J Urol 53(1):29–33. https://doi.org/10.4111/kju.2012.53.1.29
Lavigueur-Blouin H, Noriega AC, Valdivieso R, Hueber PA, Bienz M, Alhathal N, Latour M, Trinh QD, El-Hakim A, Zorn KC (2015) Predictors of early continence following robot-assisted radical prostatectomy. Can Urol Assoc J 9(1–2):e93–97. https://doi.org/10.5489/cuaj.2086
Kim JJ, Ha YS, Kim JH, Jeon SS, Lee DH, Kim WJ, Kim IY (2012) Independent predictors of recovery of continence 3 months after robot-assisted laparoscopic radical prostatectomy. J Endourol 26(10):1290–1295. https://doi.org/10.1089/end.2012.0117
Bahler CD, Sundaram CP, Kella N, Lucas SM, Boger MA, Gardner TA, Koch MO (2016) A parallel randomized clinical trial examining the return of urinary continence after robot-assisted radical prostatectomy with or without a small intestinal submucosa bladder neck sling. J Urol 196(1):179–184. https://doi.org/10.1016/j.juro.2016.01.010
Kumar A, Samavedi S, Bates AS, Coelho RF, Rocco B, Palmer K, Patel VR (2015) Continence outcomes of robot-assisted radical prostatectomy in patients with adverse urinary continence risk factors. BJU Int 116(5):764–770. https://doi.org/10.1111/bju.13106
Van Velthoven RF, Ahlering TE, Peltier A, Skarecky DW, Clayman RV (2003) Technique for laparoscopic running urethrovesical anastomosis:the single knot method. Urology 61(4):699–702. https://doi.org/10.1016/s0090-4295(02)02543-8
Rocco F, Carmignani L, Acquati P, Gadda F, Dell’Orto P, Rocco B, Bozzini G, Gazzano G, Morabito A (2006) Restoration of posterior aspect of rhabdosphincter shortens continence time after radical retropubic prostatectomy. J Urol 175(6):2201–2206. https://doi.org/10.1016/s0022-5347(06)00262-x
O’Sullivan R, Karantanis E, Stevermuer TL, Allen W, Moore KH (2004) Definition of mild, moderate and severe incontinence on the 24-hour pad test. BJOG 111(8):859–862. https://doi.org/10.1111/j.1471-0528.2004.00211.x
Haga N, Aikawa K, Hoshi S, Yabe M, Akaihata H, Hata J, Satoh Y, Ogawa S, Ishibashi K, Kojima Y (2016) Postoperative urinary incontinence exacerbates nocturia-specific quality of life after robot-assisted radical prostatectomy. Int J Urol 23(10):873–878. https://doi.org/10.1111/iju.13163
Haga N, Hata J, Matsuoka K, Koguchi T, Akaihata H, Kataoka M, Sato Y, Ogawa S, Ishibashi K, Kojima Y (2018) The impact of nerve-sparing robot-assisted radical prostatectomy on lower urinary tract function: prospective assessment of patient-reported outcomes and frequency volume charts. Neurourol Urodyn 37(1):322–330. https://doi.org/10.1002/nau.23297
Kaiho Y, Masuda H, Takei M, Hirayama T, Mitsui T, Yokoyama M, Kitta T, Kawamorita N, Nakagawa H, Iwamura M, Arai Y (2018) Surgical and patient reported outcomes of artificial urinary sphincter implantation: a multicenter, prospective, observational study. J Urol 199(1):245–250. https://doi.org/10.1016/j.juro.2017.08.077
Wei JT, Dunn RL, Marcovich R, Montie JE, Sanda MG (2000) Prospective assessment of patient reported urinary continence after radical prostatectomy. J Urol 164(3 Pt 1):744–748
Moore K, Allen M, Voaklander DC (2004) Pad tests and self-reports of continence in men awaiting radical prostatectomy: establishing baseline norms for males. Neurourol Urodyn 23(7):623–626. https://doi.org/10.1002/nau.20067
Kadono Y, Nohara T, Kadomoto S, Nakashima K, Iijima M, Shigehara K, Narimoto K, Izumi K, Mizokami A (2016) Investigating urinary conditions prior to robot-assisted radical prostatectomy in search of a desirable method for evaluating post-prostatectomy incontinence. Anticancer Res 36(8):4293–4298
von Bodman C, Matsushita K, Savage C, Matikainen MP, Eastham JA, Scardino PT, Rabbani F, Akin O, Sandhu JS (2012) Recovery of urinary function after radical prostatectomy: predictors of urinary function on preoperative prostate magnetic resonance imaging. J Urol 187(3):945–950. https://doi.org/10.1016/j.juro.2011.10.143
Kadono Y, Ueno S, Iwamoto D, Takezawa Y, Nohara T, Izumi K, Mizokami A, Namiki M (2015) Chronological urodynamic evaluation of changing bladder and urethral functions after robot-assisted radical prostatectomy. Urology 85(6):1441–1447. https://doi.org/10.1016/j.urology.2015.02.029
Matsukawa Y, Hattori R, Yoshikawa Y, Ono Y, Gotoh M (2009) Laparoscopic versus open radical prostatectomy: urodynamic evaluation of vesicourethral function. Int J Urol 16(4):393–396
Schroeck FR, Krupski TL, Sun L, Albala DM, Price MM, Polascik TJ, Robertson CN, Tewari AK, Moul JW (2008) Satisfaction and regret after open retropubic or robot-assisted laparoscopic radical prostatectomy. Eur Urol 54(4):785–793. https://doi.org/10.1016/j.eururo.2008.06.063
Schroeck FR, Krupski TL, Stewart SB, Banez LL, Gerber L, Albala DM, Moul JW (2012) Pretreatment expectations of patients undergoing robotic assisted laparoscopic or open retropubic radical prostatectomy. J Urol 187(3):894–898. https://doi.org/10.1016/j.juro.2011.10.135
Kakehi Y, Kamoto T, Shiraishi T, Ogawa O, Suzukamo Y, Fukuhara S, Saito Y, Tobisu K, Kakizoe T, Shibata T, Fukuda H, Akakura K, Suzuki H, Shinohara N, Egawa S, Irie A, Sato T, Maeda O, Meguro N, Sumiyoshi Y, Suzuki T, Shimizu N, Arai Y, Terai A, Kato T, Habuchi T, Fujimoto H, Niwakawa M (2008) Prospective evaluation of selection criteria for active surveillance in Japanese patients with stage T1cN0M0 prostate cancer. Jpn J Clin Oncol 38(2):122–128. https://doi.org/10.1093/jjco/hym161
Kelleher CJ, Cardozo LD, Khullar V, Salvatore S (1997) A new questionnaire to assess the quality of life of urinary incontinent women. Br J Obstet Gynaecol 104(12):1374–1379. https://doi.org/10.1111/j.1471-0528.1997.tb11006.x
Hunskaar S, Burgio K, Diokno A, Herzog AR, Hjälmås K, Lapitan MC (2003) Epidemiology and natural history of urinary incontinence in women. Urology 62(4):16–23. https://doi.org/10.1016/s0090-4295(03)00755-6
Haga N, Ogawa S, Yabe M, Akaihata H, Hata J, Sato Y, Ishibashi K, Hasegawa O, Kikuchi K, Shishido F, Kojima Y (2015) Factors contributing to early recovery of urinary continence analyzed by pre- and postoperative pelvic anatomical features at robot-assisted laparoscopic radical prostatectomy. J Endourol 29(6):683–690. https://doi.org/10.1089/end.2014.0708
Haga N, Ogawa S, Yabe M, Akaihata H, Hata J, Sato Y, Ishibashi K, Hasegawa O, Kikuchi K, Shishido F, Kojima Y (2014) Association between postoperative pelvic anatomic features on magnetic resonance imaging and lower tract urinary symptoms after radical prostatectomy. Urology 84(3):642–649. https://doi.org/10.1016/j.urology.2014.04.044
Basto MY, Vidyasagar C, te Marvelde L, Freeborn H, Birch E, Landau A, Murphy DG, Moon D (2014) Early urinary continence recovery after robot-assisted radical prostatectomy in older Australian men. BJU Int 114(Suppl 1):29–33. https://doi.org/10.1111/bju.12800
Novara G, Ficarra V, D’Elia C, Secco S, Cioffi A, Cavalleri S, Artibani W (2010) Evaluating urinary continence and preoperative predictors of urinary continence after robot assisted laparoscopic radical prostatectomy. J Urol 184(3):1028–1033. https://doi.org/10.1016/j.juro.2010.04.069
Shao IH, Chang YH, Hou CM, Lin ZF, Wu CT (2018) Predictors of short-term and long-term incontinence after robot-assisted radical prostatectomy. J Int Med Res 46(1):421–429. https://doi.org/10.1177/0300060517715396
Lee JK, Assel M, Thong AE, Sjoberg DD, Mulhall JP, Sandhu J, Vickers AJ, Ehdaie B (2015) Unexpected long-term improvements in urinary and erectile function in a large cohort of men with self-reported outcomes following radical prostatectomy. Eur Urol 68(5):899–905. https://doi.org/10.1016/j.eururo.2015.07.074
Acknowledgements
The authors would like to thank everyone involved in this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to report.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kurimura, Y., Haga, N., Yanagida, T. et al. The preoperative pad test as a predictor of urinary incontinence and quality of life after robot-assisted radical prostatectomy: a prospective, observational, clinical study. Int Urol Nephrol 52, 67–76 (2020). https://doi.org/10.1007/s11255-019-02301-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-019-02301-3