Abstract
Purpose
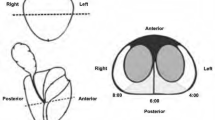
Although numerous studies have observed an inverse relationship between the size of benign prostate hypertrophy (BPH) and the incidence of prostate cancer (PCa), few studies have explored specific mechanisms by which BPH and PCa may influence one another. In a recent study, one possibility has been brought up that growth in the transition zone due to BPH may cause pressure-induced fibrotic changes in the peripheral zone, an area where 80% of cancer occurs, leading to gland atrophy and the thickening of the prostatic capsule. To shed more light on this phenomenon, we conducted a pilot study examining the quantitative and qualitative histo-anatomical changes that occur in the peripheral zone associated with BPH.
Methods
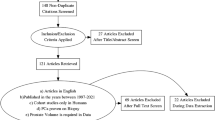
Thirty-nine prostate specimens of various sizes were selected from patients who had undergone radical prostatectomies. Each prostate was evaluated in six different locations along the dorsal aspect of the peripheral zone by measuring the thickness of the peripheral fibrotic zone (prostate capsule) and its association with gland atrophy. Multiple regression analysis was performed to determine the relationship between prostate size and the average thickness of the prostate capsule.
Results
Multiple regression analysis revealed a strong, positive relationship between prostate size and average capsule thickness with a Pearson coefficient of 0.707 (p < 0.05). Fibrotic histo-anatomical changes were spatially associated with gland atrophy: glands found within the peripheral fibrotic zone appeared elongated and atrophic.
Conclusion
The results suggest that BPH may be associated with the development of fibrotic material and atrophy of glands within the peripheral zone. Because this atrophy involves glands where 80% of prostate cancer originates, this potentially explains the inverse relationship between PCa and BPH.




Similar content being viewed by others
Abbreviations
- BPH:
-
Benign prostate hypertrophy
- Cz:
-
Central zone
- PCa:
-
Prostate cancer
- Pz:
-
Peripheral zone
- Tz:
-
Transitional zone
References
Alcaraz A, Hammerer P, Tubaro A, Schroder FH, Castro R (2009) Is there evidence of a relationship between benign prostatic hyperplasia and prostate cancer? Findings of a literature review. Eur Urol 55(4):864–873
Briganti A, Chun FK, Suardi N et al (2007) Prostate volume and adverse prostate cancer features: fact not artifact. Eur J Cancer 43(18):2669–2677
Chen ME, Troncoso P, Johnston D, Tang K, Babaian RJ (1999) Prostate cancer detection: relationship to prostate size. Urology 53(4):764–768
de Gorski A, Roupret M, Peyronnet B et al (2015) Accuracy of magnetic resonance imaging/ultrasound fusion targeted biopsies to diagnose clinically significant prostate cancer in enlarged compared to smaller prostates. J Urol 194(3):669–673
Filson CP, Natarajan S, Margolis DJ et al (2016) Prostate cancer detection with magnetic resonance-ultrasound fusion biopsy: the role of systematic and targeted biopsies. Cancer 122(6):884–892
Hong SK, Poon BY, Sjoberg DD, Scardino PT, Eastham JA (2014) Prostate size and adverse pathologic features in men undergoing radical prostatectomy. Urology 84(1):153–157
Kim JS, Ryu JG, Kim JW et al (2015) Prostate-specific antigen fluctuation: what does it mean in diagnosis of prostate cancer? Int Braz J Urol 41(2):258–264
Kozminski MA, Palapattu GS, Mehra R et al (2014) Understanding the relationship between tumor size, gland size, and disease aggressiveness in men with prostate cancer. Urology 84(2):373–378
Levine MA, Ittman M, Melamed J, Lepor H (1998) Two consecutive sets of transrectal ultrasound guided sextant biopsies of the prostate for the detection of prostate cancer. J Urol 159(2):471–475 (discussion 475–476)
Ung JO, San Francisco IF, Regan MM, DeWolf WC, Olumi AF (2003) The relationship of prostate gland volume to extended needle biopsy on prostate cancer detection. J Urol 169(1):130–135
Werahera PN, Sullivan K, La Rosa FG et al (2012) Optimization of prostate cancer diagnosis by increasing the number of core biopsies based on gland volume. Int J Clin Exp Pathol 5(9):892–899
Yoon BI, Shin TS, Cho HJ et al (2012) Is it effective to perform two more prostate biopsies according to prostate-specific antigen level and prostate volume in detecting prostate cancer? Prospective study of 10-core and 12-core prostate biopsy. Urol J 9(2):491–497
Fine S, Reuter V (2012) Anatomy of the prostate revisited: implications for prostate biopsy and zonal origins of prostate cancer. Histopathology 60(1):142–152
Strasser H, Janetschek G, Reissigl A, Bartsch (1996) Prostate zones in three-dimensional transrectal ultrasound. Adult Urol 47(4):485–490
Ayala AG, Ro JY, Babaian R, Troncoso P, Grignon DJ (1989) The prostatic capsule: does it exist? Its importance in the staging and treatment of prostatic carcinoma. Am J Surg Pathol 13(1):21–27
Semple J (1963) Surgical capsule of the benign enlargement of the prostate its development and action. BMJ 1:1640–1643
McNeal JE (1992) Prostate. In: Sternberg SS (ed) Histology for pathologists, vol 1, 2nd edn. Raven Press, New York, p 751
Rosenkrantz A, Taneja S (2014) Radiatolgist, be aware: tend pitfalls that confound the interpretation of multi-parametric prostate mri. AJR 202:109–120
Guzman J, Sharma P, Smith L, Buie J, de Riese W (2019) Histological changes of the peripheral zone in small and large prostates and possible clinical implications. Res Rep Urol 11:77–81
Guillermo L, Hughes T, Dominguez-Frojan O, Reali A, Gomez H (2019) Computer simulations suggest that prostate enlargement due to benign prostatic hyperplasia mechanically impedes prostate cancer growth. Natl Acad Sci 116(4):1152–1161
Lepor H (2004) Pathophysiology, epidemiology, and natural history of benign prostatic hyperplasia. Rev Urol 6(Suppl 9):S3–S10
Al-Khalil S, Ibilibor C, Cammack JT, de Riese W (2016) Association of prostate volume with incidence and aggressiveness of prostate cancer. Res Rep Urol 8:201–205
Oh JJ, Jeong SJ, Jeong CW et al (2013) Is there any association between the severity of lower urinary tract symptoms and the risk of biopsy-detectable prostate cancer in patients with PSA level below 20 ng/ml in multi-core prostate biopsy? Prostate 73(1):42–47
Acknowledgements
The authors wish to acknowledge the contribution of the Texas Tech University Health Sciences Center Clinical Research Institute for their assistance with the statistical analysis of the data in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial relationships or conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Frost, J.M., Smith, L.A., Sharma, P. et al. Possible clinical implications of peripheral zone changes depending on prostate size. Int Urol Nephrol 51, 1721–1726 (2019). https://doi.org/10.1007/s11255-019-02221-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-019-02221-2