Abstract
Introduction and aim
Hydrogen sulfide (H2S) is an endogenously produced gas-structure mediator. It is proposed to have antioxidant, anti-inflammatory and antiapoptotic effects. Acetaminophen (N-acetyl-P-aminophenol; APAP) is an antipyretic and analgesic medication known as paracetamol. When taken at therapeutic doses there are few side-effects, but at high doses APAP can cause clear liver and kidney damage in humans and experimental animals. In this study, the effects of the H2S donor of sodium hydrosulfide (NaHS) on acute renal toxicity induced by APAP in rats were researched in comparison with N-acetyl cysteine (NAC).
Method
Rats were divided into six groups (n = 7) as control. APAP, APAP + NAC, APAP + NaHS 25 µmol/kg, NaHS 50 µmol/kg and NaHS 100 µmol/kg. After oral dose of 2 g/kg APAP, NAC and NaHS were administered via the i.p. route for 7 days. In renal homogenates, KIM-1 (Kidney Injury Molecule-1), NGAL (neutrophil gelatinase-associated lipocalin), TNF-α and TGFβ levels were measured with the ELISA method for tissue injury and inflammation. In renal tissue, oxidative stress levels were identified by spectrophotometric measurement of TAS and TOS. Histopathologic investigation of renal tissue used caspase 3 staining for apoptotic changes, Masson trichrome and H&E staining for variations occurring in glomerular and tubular systems.
Results
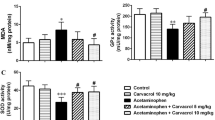
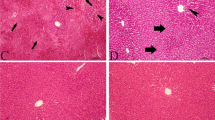
NaHS lowered KIM-1, NGAL, TNF-α, TGF-β and TOS levels elevated in renal tissue linked to APAP and increased TAS values. NaHS prevented apoptosis in the kidney and was identified to ensure histologic amelioration in glomerular and tubular structures. NaHS at 50 µmol/kg dose was more effective, with the effect reduced with 100 µmol/kg dose.
Conclusion
H2S shows protective effect against acute renal injury linked to APAP. This protective effect reduces with high doses of H2S. The anti-inflammatory and antioxidant activity of H2S may play a role in the renoprotective effect.






Similar content being viewed by others
References
Abdel-Hafez SMN, Rifaai RA, Abd Elzaher WY (2017) Mechanism of grape seeds extract protection against paracetamol renal cortical damage in male Albino rats. Bratisl Lek Listy 118(4):233–242. https://doi.org/10.4149/BLL_2017_046
Kennon-McGill S, McGill MR (2018) Extrahepatic toxicity of acetaminophen: critical evaluation of the evidence and proposed mechanisms. J Clin Transl Res. https://doi.org/10.18053/jctres.03.201703.005
Jones AF, Vale JA (1993) Paracetamol poisoning and the kidney. J Clin Pharm Ther 18(1):5–8
Sarumathy KA (2011) Protective effect of Caesalpinia sappan on acetaminophen phen induced nephrotoxicity and oxidative stress in male albino rats. J Pharmacol Toxicol 15(2):598–605
Bessems JG, Vermeulen NP (2001) Paracetamol (acetaminophen)-induced toxicity: molecular and biochemical mechanisms, analogues and protective approaches. Crit Rev Toxicol 31:55–138. https://doi.org/10.1080/20014091111677
Mugford CA, Tarloff JB (1997) The contribution of oxidation and deacetylation to acetaminophen nephrotoxicity in female Sprague-Dawley rats. Toxicol Lett 93:15–22
Li C, Liu J, Saavedra JE, Keefer LK, Waalkes MP (2003) The nitric oxide donor, V-PYRRO/NO, protects against acetaminophen-induced nephrotoxicity in mice. Toxicology 189:173–180
Das J, Ghosh J, Manna P, Sil PC (2010) Taurine protects acetaminophen-induced oxidative damage in mice kidney through APAP urinary excretion and CYP2E1 inactivation. Toxicology 269(1):24–34. https://doi.org/10.1016/j.tox.2010.01.003
Atkuri KR, Mantovani JJ, Herzenberg LA (2007) N-Acetylcysteine, a safe antidote forcysteine/glutathione deficiency. Curr Opin Pharmacol 7:355–359. https://doi.org/10.1016/j.coph.2007.04.005
Heard KJ (2008) Acetylcysteine for acetaminophen poisoning. N Engl J Med 359:285–292. https://doi.org/10.1056/NEJMct0708278
Murad HA, Habib H, Kamel Y, Alsayed S, Shakweer M, Elshal M (2016) Thearubigins protect against acetaminophen-induced hepatic and renal injury in mice: biochemical, histopathological, immunohistochemical, and flow cytometry study. Drug Chem Toxicol 39(2):190–198. https://doi.org/10.3109/01480545.2015.1070170
Hanly LN, Chen N, Aleksa K, Cutler M, Bajcetic M, Palassery R, Regueira O, Turner C, Baw B, Malkin B, Freeman D, Rieder MJ, Vasylyeva TL, Koren G (2012) N-acetylcysteine as a novel prophylactic treatment for ifosfamide-induced nephrotoxicity in children: translational pharmacokinetics. J Clin Pharmacol 52:55–64. https://doi.org/10.1177/0091270010391790
Sen U, Pushpakumar SB, Amin MA, Tyagi SC (2014) Homocysteine in renovascular complications: hydrogen sulfide is a modulator and plausible anaerobic ATP generator. Nitric Oxide 15;41:27–37. https://doi.org/10.1016/j.niox.2014.06.006
Shibuya N, Koike S, Tanaka M, Ishigami-Yuasa M, Kimura Y, Ogasawara Y (2013) A novel pathway for the production of hydrogen sulfide from d-cysteine in mammalian cells. Nat Commun 4:1366. https://doi.org/10.1038/ncomms2371
Chen Y, Jin S, Teng X, Hu Z, Zhang Z, Qiu X, Tian D, Wu Y(2018). Hydrogen sulfide attenuates LPS-induced acute kidney injury by inhibiting inflammation and oxidative stress. Oxid Med Cell Longev 2018: 6717212. https://doi.org/10.1155/2018/6717212
Huang Z, Zhuang X, Xie C, Hu X, Dong X, Guo Y, Li S, Liao X (2016) Exogenous hydrogen sulfide attenuates high glucose-induced cardiotoxicity by inhibiting NLRP3 inflammasome activation by suppressing TLR4/NF-κB pathway in H9C2 cells. Cell Physiol Biochem 40:6;1578–90. https://doi.org/10.1159/000453208
Han SJ, Kim JI, Park JW, Park KM (2015) Hydrogen sulfide accelerates the recovery of kidney tubules after renal ischemia/reperfusion injury. Nephrol Dial Transpl. 30:1497–1506. https://doi.org/10.1093/ndt/gfv226
Dugbartey GJ (2016) Diabetic nephropathy: A potential savior with ‘rotten-egg’ smell. Pharmacol Rep 69(2):331–9. https://doi.org/10.1016/j.pharep.2016.11.004
Dugbartey GJ (2017) H2S as a possible therapeutic alternative for the treatment of hypertensive kidney injury. Nitric Oxide 64:52–60. https://doi.org/10.1016/j.niox.2017.01.002
Dugbartey (2018) The smell of renal protection against chronic kidney disease: hydrogen sulfide offers a potential stinky remedy. Pharmacol Rep 70(2):196–205. https://doi.org/10.1016/j.pharep.2017.10.007
Canayakin D, Bayir Y, Kilic Baygutalp N, Sezen Karaoglan E, Atmaca HT, Kocak Ozgeris FB, Keles MS, Halici Z (2016) Paracetamol-induced nephrotoxicity and oxidative stress in rats: the protective role of Nigella sativa. Pharm Biol 54(10):2082–2091. https://doi.org/10.3109/13880209.2016.1145701
Zeng O, Li F, Li Y, Li L, Xiao T, Chu C, Yang J (2016) Effect of novel gasotransmitter hydrogen sulfide on renal fibrosis and connexins expression in diabetic rats. Bioengineered 7(5):314–320. https://doi.org/10.1080/21655979.2016.1197743
Zhang W, Sha Y, Wei K, Wu C, Ding D, Yang Y, Zhu C, Zhang Y, Ding G, Zhang A, Jia Z, Huang S (2018) Rotenone ameliorates chronic renal injury caused by acute ischemia/reperfusion. Oncotarget 9(36):24199–24208. https://doi.org/10.18632/oncotarget.24733
Hiragi S, Yamada H, Tsukamoto T, Yoshida K, Kondo N, Matsubara T, Yanagita M, Tamura H, Kuroda T (2018) Acetaminophen administration and the risk of acute kidney injury: a self-controlled case series study. Clin Epidemiol 10:265–276. https://doi.org/10.2147/CLEP.S158110
Högestätt ED, Jönsson BA, Ermund A, Andersson DA, Björk H, Alexander JP, Cravatt BF, Basbaum AI, Zygmunt PM (2005) Conversion of acetaminophen to the bioactive N-acylphenolamine AM404 via fatty acid amide hydrolase-dependent arachidonic acid conjugation in the nervous system. J Biol Chem 280(36):31405–31412. https://doi.org/10.1074/jbc.M501489200
RM (2000) Botting. Mechanism of action of acetaminophen: is there a cyclooxygenase 3? Clin Infect Dis 31(suppl 5):S202–S210. https://doi.org/10.1086/317520
Botting R, Ayoub SS (2005) COX-3 and the mechanism of action of paracetamol/acetaminophen. Prostaglandins Leukot Essent Fatty Acids 72(2):85–87. https://doi.org/10.1016/j.plefa.2004.10.005
Mazer M, Perrone J (2008) Acetaminophen-induced nephrotoxicity: pathophysiology, clinical manifestations, and management. J Med Toxicol 4(1):2–6
Prescott LF (1983) Paracetamol overdosage. Pharmacological considerations and clinical management. Drugs 25(3):290–314
Chen YG, Lin CL, Dai MS, Chang PY, Chen JH, Huang TC, Wu YY, Kao CH (2015) Risk of acute kidney injury and long-term outcome in patients with acetaminophen intoxication: a nationwide population-based retrospective cohort study. Medicine 94(46):e2040. https://doi.org/10.1097/MD.0000000000002040
Lei L, Li LP, Zeng Z, Mu JX, Yang X, Zhou C, Wang ZL, Zhang H (2018) Value of urinary KIM-1 and NGAL combined with serum Cys C for predicting acute kidney injury secondary to decompensated cirrhosis. Sci Rep 21(1):7962. https://doi.org/10.1038/s41598-018-26226-6
Bonventre JV (2014) Kidney injury molecule-1: a translational journey. Trans Am Clin Climatol Assoc 125:293–299
Zhang Y, Liu N, Ren Q, Zhang H, Xie X (2013) Sodium hydrosulfide for prevention of kidney damage in rats after amputation. Nan Fang Yi Ke Da Xue Xue Bao 33(8):1146–1150. https://doi.org/10.3969/j.issn.1673-4254.2013.08.10
Lobb I, Davison M, Carter D, Liu W, Haig A, Gunaratnam L, Sener A (2015) Hydrogen sulfide treatment mitigates renal allograft ischemia-reperfusion injury during cold storage and improves early transplant kidney function and survival following allogeneic renal transplantation. J Urol 194(6):1806–1815. https://doi.org/10.1016/j.juro.2015.07.096
Nußbaum BL, Vogt J, Wachter U, McCook O, Wepler M, Matallo J, Calzia E, Gröger M, Georgieff M, Wood ME, Whiteman M, Radermacher P, Hafner S (2017) Metabolic, cardiac, and renal effects of the slow hydrogen sulfide-releasing molecule GYY4137 during resuscitated septic shock in swine with pre-existing coronary artery disease. Shock 48(2):175–184. https://doi.org/10.1097/SHK.0000000000000834
Sekijima M, Sahara H, Miki K, Villani V, Ariyoshi Y, Iwanaga T, Tomita Y, Yamada K (2017) Hydrogen sulfide prevents renal ischemia-reperfusion injury in CLAWN miniature swine. J Surg Res 219:165–172. https://doi.org/10.1016/j.jss.2017.05.123
Ibrahim MY, Aziz NM, Kamel MY, Rifaai RA (2015) Sodium hydrosulphide against renal ischemia/reperfusion and the possible contribution of nitric oxide in adult male Albino rats. Bratisl Lek Listy. 116(11):681–688. https://doi.org/10.4149/BLL_2015_133
Ali FF, Abdel-Hamid HA, Toni ND (2018) H2S attenuates acute lung inflammation induced by administration of lipopolysaccharide in adult male rats. Gen Physiol Biophys. https://doi.org/10.4149/gpb_2018002
Wu D, Gao B, Li M, Yao L, Wang S, Chen M, Li H, Ma C, Ji A, Li Y (2016) Hydrogen sulfide mitigates kidney injury in high fat diet-induced obese mice. Oxid Med Cell Longev 2016:2715718 https://doi.org/10.1155/2016/2715718
Wu D, Luo N, Wang L, Zhao Z, Bu H, Xu G, Yan Y, Che X, Jiao Z, Zhao T, Chen J, Ji A, Li Y, Lee GD (2017) Hydrogen sulfide ameliorates chronic renal failure in rats by inhibiting apoptosis and inflammation through ROS/MAPK and NF-κB signaling pathways. Sci Rep 28;7(1):455. https://doi.org/10.1038/s41598-017-00557-2
Yang R, Liu XF, Ma SF, Gao Q, Li ZH, Jia Q (2016) Protective effect of hydrogen sulfide on kidneys of type 1 diabetic rats. Zhongguo Ying Yong Sheng Li Xue Za Zhi 8(2):181–184. https://doi.org/10.13459/j.cnki.cjap.2016.02.023.
Karimi A, Absalan F, Khorsandi L, Valizadeh A, Mansouri E (2017) Sodium hydrogen sulfide (NaHS) ameliorates alterations caused by cisplatin in filtration slit diaphragm and podocyte cytoskeletal in rat kidney. J Nephropathol 6(3):150–156. https://doi.org/10.15171/jnp.2017.26
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the Dumlupinar University, Animal Experiments Local Ethics Committee at which the studies were conducted (Decision no: 2017.07.01).
Additional information
This Study was carried out in Dumlupinar University, Experimental Animal Laboratory.
Rights and permissions
About this article
Cite this article
Ozatik, F.Y., Teksen, Y., Kadioglu, E. et al. Effects of hydrogen sulfide on acetaminophen-induced acute renal toxicity in rats. Int Urol Nephrol 51, 745–754 (2019). https://doi.org/10.1007/s11255-018-2053-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-2053-0