Abstract
Purpose
Population studies of patients undergoing radical cystectomy (RC) for bladder cancer (BC) suggest that a more extended lymph node dissection (LND) increases survival. However, information regarding LNDs of patients undergoing RC with a history of radiation therapy for BC is largely unknown. This study aims to define the lymph node yield (LNY) in patients undergoing RC for BC following radiation of the bladder using the surveillance epidemiology and end results (SEER) database.
Methods
Data were collected using SEER 18 registries from 1988 to 2013 to identify patients undergoing RC for BC. Data on extent and yield of LND were obtained. Logistic regression and multivariate Cox proportional hazard regression were done to identify predictors of adequate LND and all-cause mortality, respectively.
Results
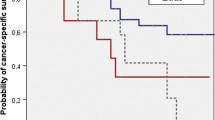
In total, 27,451 patients were identified, of which, 27,362 (99.7%) were radiation naïve and 89 (0.3%) had prior radiation therapy for BC. The average LNY in radiation naïve patients (15, SD [13.5]) was slightly higher than the LNY in patients with prior radiation (12.3 SD [9.2], p = 0.157). Prior radiation was not an independent predictor of overall mortality (HR = 1.3, 95% CI [0.98–1.7]; p = 0.076).
Conclusions
A lower proportion of patients with a history of radiation underwent a LND. The LNYs of radiation naïve patients, and those with a history of radiation, were not statistically different; however, the proportion of irradiated patients was small. Further investigation will be required to elucidate the patient and provider characteristics that contribute to the similar LNYs.

Similar content being viewed by others
References
Konety BR, Joslyn SA, O’Donnell MA (2003) Extent of pelvic lymphadenectomy and its impact on outcome in patients diagnosed with bladder cancer: analysis of data from the Surveillance, Epidemiology and End Results Program data base. J Urol 169(3):946–950
Siemens DR et al (2015) Lymph node counts are valid indicators of the quality of surgical care in bladder cancer: a population-based study. Urol Oncol 33(10):425.e15–425.e23
Hollenbeck BK et al (2008) Hospital lymph node counts and survival after radical cystectomy. Cancer 112(4):806–812
Herr HW et al (2002) Impact of the number of lymph nodes retrieved on outcome in patients with muscle invasive bladder cancer. J Urol 167(3):1295–1298
Herr H et al (2004) Standardization of radical cystectomy and pelvic lymph node dissection for bladder cancer: a collaborative group report. J Urol 171(5):1823–1828 (discussion 1827–1828)
Leissner J et al (2000) Lymphadenectomy in patients with transitional cell carcinoma of the urinary bladder; significance for staging and prognosis. BJU Int 85(7):817–823
Wright JL, Lin DW, Porter MP (2008) The association between extent of lymphadenectomy and survival among patients with lymph node metastases undergoing radical cystectomy. Cancer 112(11):2401–2408
Abdollah F et al (2012) Stage-specific impact of pelvic lymph node dissection on survival in patients with non-metastatic bladder cancer treated with radical cystectomy. BJU Int 109(8):1147–1154
Cole AP et al (2015) Temporal trends in receipt of adequate lymphadenectomy in bladder cancer 1988 to 2010. Urol Oncol 33(12):504.e9–504.e17
Hedgepeth RC et al (2011) Variation in use of lymph node dissection during radical cystectomy for bladder cancer. Urology 77(2):385–390
Ramani VA et al (2010) Differential complication rates following radical cystectomy in the irradiated and nonirradiated pelvis. Eur Urol 57(6):1058–1063
Efstathiou JA et al (2012) Long-term outcomes of selective bladder preservation by combined-modality therapy for invasive bladder cancer: the MGH experience. Eur Urol 61(4):705–711
Nieuwenhuijzen JA et al (2004) Salvage cystectomy after failure of interstitial radiotherapy and external beam radiotherapy for bladder cancer. BJU Int 94(6):793–797
Eisenberg MS et al (2010) Early complications of cystectomy after high dose pelvic radiation. J Urol 184(6):2264–2269
Hellenthal NJ et al (2009) Trends in pelvic lymphadenectomy at the time of radical cystectomy: 1988 to 2004. J Urol 181(6):2490–2495
Herr HW et al (2004) Surgical factors influence bladder cancer outcomes: a cooperative group report. J Clin Oncol 22(14):2781–2789
Skinner EC, Stein JP, Skinner DG (2007) Surgical benchmarks for the treatment of invasive bladder cancer. Urol Oncol 25(1):66–71
National Comprehensive Cancer Network. Bladder cancer (version 1.2017). 2017 January 5, 2017. https://www.nccn.org/professionals/physician_gls/PDF/bladder.pdf
Dorin RP et al (2011) Lymph node dissection technique is more important than lymph node count in identifying nodal metastases in radical cystectomy patients: a comparative mapping study. Eur Urol 60(5):946–952
van de Putte EEF et al (2015) Lymph node count at radical cystectomy does not influence long-term survival if surgeons adhere to a standardized template. Urol Oncol 33(12):504.e19–504.e24
Ghersi D, Stewart LA, Palmar MKB et al. (1999) Neoadjuvant cisplatin, methotrexate, and vinblastine chemotherapy for muscle-invasive bladder cancer: a randomised controlled trial. International collaboration of trialists. Lancet 354(9178):533–540
Mata DA et al (2015) Variability in surgical quality in a phase III clinical trial of radical cystectomy in patients with organ-confined, node-negative urothelial carcinoma of the bladder. J Surg Oncol 111(7):923–928
Stein JP et al (2007) Radical cystectomy with extended lymphadenectomy: evaluating separate package versus en bloc submission for node positive bladder cancer. J Urol 177(3):876–881 (discussion 881–882)
Acknowledgements
This research was supported by the Intramural Research Program of the NIH, National Cancer Institute, Center for Cancer Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Maruf, M., Sidana, A., Purnell, S. et al. Lymph node dissection during radical cystectomy following prior radiation therapy: results from the SEER database. Int Urol Nephrol 50, 257–262 (2018). https://doi.org/10.1007/s11255-017-1751-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-017-1751-3