Abstract
Purpose
Guidelines for atypical small acinar proliferation (ASAP) diagnosed on prostate biopsy recommend repeat biopsy within 3–6 months after diagnosis. We sought to discern the rate of detecting clinically significant prostate cancer on repeat biopsy and predictors associated with progression.
Materials and methods
We performed a retrospective chart review of patients who underwent prostate biopsy at our institution from January 1, 2008, to December 31, 2015. Gleason grade group (GGG) system and D’Amico stratification were used to report pathology and risk stratification, respectively. Logistic and linear regression analyses were performed.
Results
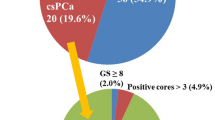
A total of 593 patients underwent transrectal ultrasound-guided prostate biopsy, of which 27 (4.6%) had the diagnosis of ASAP. Of these, 11 (41%) had a repeat biopsy. Median time from diagnosis to repeat biopsy was 147 days (IQR 83.5–247.0). Distribution across the GGG system on repeat biopsy was as follows: 7 (63.6%) benign, 3 (27.3%) GG1, and 1 (9.1%) GG2. ASAP was not associated with subsequent diagnosis of clinically significant prostate cancer (OR 0.46, 95% CI 0.064–3.247, P = 0.432). There was no association between ASAP and high cancer risk (ASAP: β = − 0.12; P = 0.204).
Conclusions
Patients diagnosed with ASAP managed according to guideline recommendations are more likely diagnosed with benign pathology and indolent prostate cancer on repeat biopsy. These findings support prior studies suggesting refinement of guidelines in regard to the appropriateness and timeliness of repeat biopsy among patients diagnosed with ASAP.


Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics, 2017. CA Cancer J Clin 67(1):7–30
Makarov DV, Trock BJ, Humphreys EB et al (2007) Updated nomogram to predict pathologic stage of prostate cancer given prostate-specific antigen level, clinical stage, and biopsy Gleason score (Partin tables) based on cases from 2000 to 2005. Urology 69(6):1095–1101
Lu-Yao GL, Albertsen PC, Moore DF et al (2009) Outcomes of localized prostate cancer following conservative management. JAMA 302(11):1202–1209
Mohler JL, Armstrong AJ, Bahnson RR et al (2016) Prostate cancer, version 1.2016. J Natl Compr Cancer Netw 14(1):19–30
Montironi R, Scattoni V, Mazzucchelli R, Lopez-Beltran A, Bostwick DG, Montorsi F (2006) Atypical foci suspicious but not diagnostic of malignancy in prostate needle biopsies (also referred to as “atypical small acinar proliferation suspicious for but not diagnostic of malignancy”). Eur Urol 50(4):666–674
Borboroglu PG, Comer SW, Riffenburgh RH, Amling CL (2000) Extensive repeat transrectal ultrasound guided prostate biopsy in patients with previous benign sextant biopsies. J Urol 163(1):158–162
Moore CK, Karikehalli S, Nazeer T, Fisher HA, Kaufman RP Jr, Mian BM (2005) Prognostic significance of high grade prostatic intraepithelial neoplasia and atypical small acinar proliferation in the contemporary era. J Urol 173(1):70–72
Warlick C, Feia K, Tomasini J, Iwamoto C, Lindgren B, Risk M (2015) Rate of Gleason 7 or higher prostate cancer on repeat biopsy after a diagnosis of atypical small acinar proliferation. Prostate Cancer Prostatic Dis 18(3):255–259
Leone A, Gershman B, Rotker K et al (2016) Atypical small acinar proliferation (ASAP): is a repeat biopsy necessary ASAP? A multi-institutional review. Prostate Cancer Prostatic Dis 19(1):68–71
Dorin RP, Wiener S, Harris CD, Wagner JR (2015) Prostate atypia: does repeat biopsy detect clinically significant prostate cancer? Prostate 75(7):673–678
Tosoian JJ, Mamawala M, Epstein JI et al (2015) Intermediate and longer-term outcomes from a prospective active-surveillance program for favorable-risk prostate cancer. J Clin Oncol 33(30):3379–3385
Carroll PR, Parsons JK, Andriole G et al (2014) Prostate cancer early detection, version 1.2014. Featured updates to the NCCN guidelines. J Natl Compr Cancer Netw 12(9):1211–1219 (quiz 1219)
Epstein JI, Egevad L, Amin MB, Delahunt B, Srigley JR, Humphrey PA (2016) The 2014 international society of urological pathology (ISUP) consensus conference on Gleason grading of prostatic carcinoma: definition of grading patterns and proposal for a new grading system. Am J Surg Pathol 40(2):244–252
Heidenreich A, Bastian PJ, Bellmunt J et al (2014) EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent-update 2013. Eur Urol 65(1):124–137
van Vugt HA, Roobol MJ, Kranse R et al (2011) Prediction of prostate cancer in unscreened men: external validation of a risk calculator. Eur J Cancer 47(6):903–909
Ankerst DP, Hoefler J, Bock S et al (2014) Prostate cancer prevention trial risk calculator 2.0 for the prediction of low- vs high-grade prostate cancer. Urology 83(6):1362–1367
Hamdy FC, Donovan JL, Lane JA et al (2016) 10-Year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Engl J Med 375(15):1415–1424
Tosoian JJ, Trock BJ, Landis P et al (2011) Active surveillance program for prostate cancer: an update of the Johns Hopkins experience. J Clin Oncol 29(16):2185–2190
Raskolnikov D, Rais-Bahrami S, George AK et al (2015) The role of image guided biopsy targeting in patients with atypical small acinar proliferation. J Urol 193(2):473–478
Cool DW, Romagnoli C, Izawa JI et al (2016) Comparison of prostate MRI-3D transrectal ultrasound fusion biopsy for first-time and repeat biopsy patients with previous atypical small acinar proliferation. Can Urol Assoc J 10(9–10):342–348
Merrick GS, Galbreath RW, Bennett A, Butler WM, Amamovich E (2016) Incidence, grade and distribution of prostate cancer following transperineal template-guided mapping biopsy in patients with atypical small acinar proliferation. World J Urol 35:1009–1013
Kapoor DA, Klimberg IW, Malek GH et al (1998) Single-dose oral ciprofloxacin versus placebo for prophylaxis during transrectal prostate biopsy. Urology 52(4):552–558
Ekwueme DU, Stroud LA, Chen Y (2007) Cost analysis of screening for, diagnosing, and staging prostate cancer based on a systematic review of published studies. Prev Chronic Dis 4(4):A100
Ploussard G, Plennevaux G, Allory Y et al (2009) High-grade prostatic intraepithelial neoplasia and atypical small acinar proliferation on initial 21-core extended biopsy scheme: incidence and implications for patient care and surveillance. World J Urol 27(5):587–592
Aus G, Ahlgren G, Bergdahl S, Hugosson J (1996) Infection after transrectal core biopsies of the prostate—risk factors and antibiotic prophylaxis. Br J Urol 77(6):851–855
Loeb S, van den Heuvel S, Zhu X, Bangma CH, Schroder FH, Roobol MJ (2012) Infectious complications and hospital admissions after prostate biopsy in a European randomized trial. Eur Urol 61(6):1110–1114
Lundstrom KJ, Drevin L, Carlsson S et al (2014) Nationwide population based study of infections after transrectal ultrasound guided prostate biopsy. J Urol 192(4):1116–1122
Loeb S, Carter HB, Berndt SI, Ricker W, Schaeffer EM (2013) Is repeat prostate biopsy associated with a greater risk of hospitalization? Data from SEER-Medicare. J Urol 189(3):867–870
Nam RK, Saskin R, Lee Y et al (2013) Increasing hospital admission rates for urological complications after transrectal ultrasound guided prostate biopsy. J Urol 189(1 Suppl):S12–S17 (discussion S17–18)
Borboroglu PG, Sur RL, Roberts JL, Amling CL (2001) Repeat biopsy strategy in patients with atypical small acinar proliferation or high grade prostatic intraepithelial neoplasia on initial prostate needle biopsy. J Urol 166(3):866–870
Epstein JI, Zelefsky MJ, Sjoberg DD et al (2016) A contemporary prostate cancer grading system: a validated alternative to the Gleason score. Eur Urol 69(3):428–435
Rosenkrantz AB, Verma S, Choyke P et al (2016) Prostate magnetic resonance imaging and magnetic resonance imaging targeted biopsy in patients with a prior negative biopsy: a consensus statement by AUA and SAR. J Urol 196(6):1613–1618
Funding
This study was funded by the Institute for Translational Sciences at the University of Texas Medical Branch, supported in part by a Clinical and Translational Science Award Mentored Career Development (KL2) Award (KL2TR001441) from the National Center for Advancing Translational Sciences, National Institutes of Health (SBW).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was not obtained from individual participants included in the study as the study was a retrospective study which institutional IRB granted waiver for consent.
Rights and permissions
About this article
Cite this article
Ynalvez, L.A., Kosarek, C.D., Kerr, P.S. et al. Atypical small acinar proliferation at index prostate biopsy: rethinking the re-biopsy paradigm. Int Urol Nephrol 50, 1–6 (2018). https://doi.org/10.1007/s11255-017-1714-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-017-1714-8