Abstract
Purpose
Arteriovenous fistula (AVF) is the preferred vascular access for hemodialysis. The impact of vascular calcification process on AVF survival remains unclear and results of several studies about this issue are controversial. In the light of the new knowledge about the different susceptibility for calcification process in different blood vessels, the aim of our study was to analyze whether the calcification of AVF-blood vessels may have an impact on AVF longevity.
Methods
The study included 90 patients, 49 males and 41 females, all of them Caucasians, with a mean age 62 ± 11 years, on regular hemodialysis for more than 1 year with patent primary AVFs. Vascular calcification in AVF-blood vessels or in the anastomotic region was detected using X-ray examination.
Results
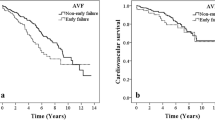
Calcification in AVF-blood vessels was found in 62% of patients. Binary logistic regression analysis demonstrated that male gender, presence of diabetes mellitus and longer duration of AVF before calcification determination were associated with calcification of AVF-blood vessels. Using a Cox proportional hazard model adjusted for these standardized predicted values revealed that patients with present AVF-blood vessels calcification had increased risk to develop AVF failure with a hazard rate of 3.42 (95% confidence interval 1.00–11.67; P = 0.049).
Conclusions
Calcifications of AVF-blood vessels are found frequently among dialysis patients and may jeopardize the survival of native AVF. We suggested the local X-ray as simple and valid method for detection of patients that are at risk for AVFs failure which should be monitored more closely.


Similar content being viewed by others
References
Vascular Access 2006 Work Group (2006) Clinical practice guidelines for vascular access. Am J Kidney Dis 48(Suppl 1):S176–S247
Allon M, Robbin ML (2002) Increasing arteriovenous fistulas in hemodialysis patients: problems and solutions. Kidney Int 62:1109–1124
Gallieni M, Martini A, Mezzina N (2009) Dialysis access: an increasingly important clinical issue. Int J Artif Organs 32:851–856
Campos RP, Do Nascimento MM, Chula DC, Do Nascimento DE, Riella MC (2006) Stenosis in hemodialysis arteriovenous fistula: evaluation and treatment. Hemodial Int 10:152–161
Feddersen MA, Roger SD (2012) Arteriovenous fistula surveillance: everyone’s responsibility. Port J Nephrol Hypert 26:255–265
Kumbar L, Karim J, Besarab A. (2012) Surveillance and monitoring of dialysis access. Int J Nephrol 649735
Igata M, Motoshima H, Tsuruzoe K, Kojima K, Matsumura T, Kondo T, Taguchi T, Nakamaru K, Yano M, Kukidome D, Matsumoto K, Toyonaga T, Asano T, Nishikawa T, Araki E (2005) Adenosine monophosphate-activated protein kinase suppresses vascular smooth muscle cell proliferation through the inhibition of cell cycle progression. Circ Res 97(8):837–844
MacAskill MG, Watson DG, Ewart MA, Wadsworth R, Jackson A, Aitken E, MacKenzie G, Kingsmore D, Currie S, Coats P (2015) Improving arteriovenous fistula patency: transdermal delivery of diclofenac reduces cannulation-dependent neointimal hyperplasia via AMPK activation. Vascul Pharmacol 71:108–115
Krönung G (1984) Plastic deformation of cimino fistula by repeated puncture. Dial Transplant. 13:635–638
Lobo C, Stockler-Pinto MB, da Nóbrega ACL, Carraro-Eduardo JC, Mafra D (2013) Is there association between uric acid and inflammation in hemodialysis patients? Ren Fail 35:361–366
De Graaf R, Kloppenburg G, Kitslaar PJHM, Bruggemana C, Stassen F (2006) Human heat shock protein 60 stimulates vascular smooth muscle cell proliferation through toll-like receptors 2 and 4. Microbes Infect 8:1859–1865
Simard T, Hibbert B, Ramirez FD, Froeschl M, Chen YX, O’Brien ER (2014) The evolution of coronary stents: a brief review. Can J Cardiol 30:35–45
Leivaditis K, Panagoutsos S, Roumeliotis A, Liakopoulos V, Vargemezis V (2014) Vascular access for hemodialysis: postoperative evaluation and function monitoring. Int Urol Nephrol 46:403–409
Jankovic A, Damjanovic T, Djuric Z, Marinkovic J, Schlieper G, Tosic-Dragovic J, Djuric P, Popovic J, Floege J, Dimkovic N (2015) Impact of vascular calcifications on arteriovenous fistula survival in hemodialysis patients: a five-year follow-up. Nephron. 129:247–252
Choi SJ, Yoon HE, Kim YS, Yoon SA, Yang CW, Kim YS, Kim YS, Park SC, Kim YO (2015) Pre-existing arterial micro-calcification predicts primary unassisted arteriovenous fistula failure in incident hemodialysis patients. Semin Dial 28(6):665–669
Allon M, Robbin M, Umphrey HR, Young CJ, Deierhoi MH, Goodman J, Hanaway M, Lockhart ME, Barker-Finkel J, Litovsky S (2015) Preoperative arterial microcalcification and clinical outcomes of arteriovenous fistulas for hemodialysis. Am J Kidney Dis 66(1):84–90
Georgiadis GS, Georgakarakos EI, Antoniou GA, Panagoutsos S, Argyriou C, Mourvati E, Passadakis P, Lazarides MK (2014) Correlation of pre-existing radial artery macrocalcifications with late patency of primary radiocephalic fistulas in diabetic hemodialysis patients. J Vasc Surg 60(2):462–470
London GM (2012) Bone-vascular cross-talk. J Nephrol 25:619–625
Schlieper G, Schurgers L, Brandenburg V, Reutelingsperger C, Floege J (2016) Vascular calcification in chronic kidney disease: an update. Nephrol Dial Transplant 31(1):31–39
Schlieper G, Krüger T, Djuric Z, Damjanovic T, Markovic N, Schurgers LJ, Brandenburg VM, Westenfeld R, Dimkovic S, Ketteler M, Grootendorst DC, Dekker FW, Floege J, Dimkovic N (2008) Vascular access calcification predicts mortality in hemodialysis patients. Kidney Int 74:1582–1587
Jankovic A, Donfrid B, Adam J, Ilic M, Djuric Z, Damjanovic T, Popovic J, Popovic G, Radojicic Z, Dimkovic N (2013) Arteriovenous fistula aneurysm in patients on regular hemodialysis: prevalence and risk factors. Nephron Clin Pract 124:94–98
Kidney Disease: Improving Global Outcomes (KDIGO) CKD-MBD Work Group (2009) KDIGO clinical practice guideline for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD). Kidney Int Suppl 113:S1–S130
Tordoir J, Canaud B, Haage P, Konner K, Basci A, Fouque D, Kooman J, Martin-Malo A, Pedrini L, Pizzarelli F, Tattersall J, Vennegoor M, Wanner C, ter Wee P, Vanholder R (2007) EBPG on vascular access. Nephrol Dial Transplant 22(2):88–117
Ravani P, Brunori G, Mandolfo S, Cancarini G, Imbasciati E, Marcelli D, Malberti F (2004) Cardiovascular comorbidity and late referral impact arteriovenous fistula survival: a prospective multicenter study. J Am Soc Nephrol 15:204–209
Rayner HC, Pisoni RL, Gillespie BW, Goodkin DA, Akiba T, Akizawa T, Saito A, Young EW, Port FK; Dialysis Outcomes and Practice Patterns Study (2003) Dialysis outcomes and practice patterns study: creation, cannulation and survival of arteriovenous fistulae: data from the dialysis outcomes and practice patterns study. Kidney Int 63:323–330
Yamamoto K, Protack CD, Kuwahara G, Tsuneki M, Hashimoto T, Hall MR, Assi R, Brownson KE, Foster TR, Bai H, Wang M, Madri JA, Dardik A (2015) Disturbed shear stress reduces Klf2 expression in arterial-venous fistulae in vivo. Physiol Rep 3(3):e12348
Adragao T, Pires A, Lucas C, Birne R, Magalhaes L, Gonçalves M, Negrao AP (2004) A simple vascular calcification score predicts cardiovascular risk in haemodialysis patients. Nephrol Dial Transplant 19:1480–1488
Lehoux S, Castier Y, Tedgui A (2006) Molecular mechanisms of the vascular responses to haemodynamic forces. J Intern Med 259:381–392
McCue S, Noria S, Langille BL (2004) Shear-induced reorganization of endothelial cell cytoskeleton and adhesion complexes. Trends Cardiovasc Med 14:143–151
Gimbrone MA Jr (1999) Endothelial dysfunction, hemodynamic forces, and atherosclerosis. Thromb Haemost 82:722–726
Nayak L, Lin Z, Jain MK (2011) “Go with the flow”: how Kruppel-like factor 2 regulates the vasoprotective effects of shear stress. Antioxid Redox Signal 15:1449–1461
Bjorck HM, Renner J, Maleki S, Nilsson SF, Kihlberg J, Folkersen L, Karlsson M, Ebbers T, Eriksson P, Länne T (2012) Characterization of shear-sensitive genes in the normal rat aorta identifies Hand2 as a major flow-responsive transcription factor. PLoS One 7(12):e52227
Chiu JJ, Chien S (2011) Effects of disturbed flow on vascular endothelium: pathophysiological basis and clinical perspectives. Physiol Rev 91:327–387
Davies PF, Civelek M, Fang Y, Fleming I (2013) The atherosusceptible endothelium: endothelial phenotypes in complex haemodynamic shear stress regions in vivo. Cardiovasc Res 99:315–327
Noordzij M, Cranenburg EM, Engelsman LF, Hermans MM, Boeschoten EW, Brandenburg VM, Bos WJ, Kooman JP, Dekker FW, Ketteler M, Schurgers LJ, Krediet RT, Korevaar JC; NECOSAD Study Group (2011) Progression of aortic calcification is associated with disorders of mineral metabolism and mortality in chronic dialysis patients. Nephrol Dial Transplant 26(5):1662–1669
Kröger K (2006) Epidemiology of peripheral arterial disease in Germany. What is evident, what remains unclear? Hamostaseologie 26(3):193–196
Lanzer P, Boehm M, Sorribas V, Thiriet M, Janzen J, Zeller T, St Hilaire C, Shanahan C (2014) Medial vascular calcification revisited: review and perspectives. Eur Heart J 35:1515–1525
Prischl FC, Kirchgatterer A, Brandstätter E, Wallner M, Baldinger C, Roithinger FX, Kramar R (1995) Parameters of prognostic relevance to the patency of vascular access in hemodialysis patients. J Am Soc Nephrol 6(6):1613–1618
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Jankovic, A., Damjanovic, T., Djuric, Z. et al. Calcification in arteriovenous fistula blood vessels may predict arteriovenous fistula failure: a 5-year follow-up study. Int Urol Nephrol 49, 881–887 (2017). https://doi.org/10.1007/s11255-017-1515-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-017-1515-0