Abstract
Purpose
Paraoxonase-1 (PON-1) is a high-density lipoprotein-associated (HDL) enzyme, which has been shown to reduce susceptibility to low-density lipoprotein (LDL) peroxidation. Epicardial adipose tissue (EAT) is a marker of atherosclerosis. The aim of this study was to determine the relationship between PON-1 activity and EAT in hemodialysis (HD) patients.
Methods
This is a cross-sectional study conducted on 72 (43 males) HD patients with end-stage renal disease. Serum levels for lipid profiles, C-reactive protein, calcium, phosphate, and parathyroid hormone were measured. PON-1 activity was also measured and compared to the rate of enzymatic hydrolysis of paraoxon to p-nitrophenol. Echocardiography was used to measure EAT thickness (EATT). The correlation between PON-1 and EATT was assessed, while independent predictors of EATT in HD patients were similarly assessed using multivariate regression analysis.
Results
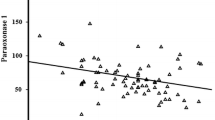
There was a significant low mean value of PON-1 activity in HD patients compared with the control group (82.1 ± 31.6 vs. 164.3 ± 61.5 U/l, p = 0.0001) and significant high mean value of EATT in HD patients, compared with controls (6.2 ± 1.7 vs. 3.9 ± 1.1 mm, p = 0.0001). In addition, there was a significant negative correlation between PON-1 activity and EATT (r = −0.484, p = 0.0001) and a significant positive correlation between PON-1 activity and HDL-C (r = 0.417, p = 0.0003). PON-1, total cholesterol, triglycerides, LDL, HDL, age, and body mass index were found to be independent predictors of EATT.
Conclusion
Our study demonstrated that PON-1 activity was significantly lower in HD patients compared with healthy controls and that PON-1 activity was inversely correlated with EATT in this population.


Similar content being viewed by others
References
Hou FF, Jiang JP, Chen J, Yu X, Zhou Q, Chen P, Mei C, Xiong F, Shi W, Zhou W, Liu X, Sun S, Xie D, Liu J, Zhang P, Yang X, Zhang Y, Zhang Y, Liang X, Zhang Z, Lin Q, Yu Y, Wu S, Xu X (2012) China collaborative study on dialysis: a multi-centers cohort study on cardiovascular diseases in patients on maintenance dialysis. BMC Nephrol 13(1):94–102
Kosaka T, Yamaguchi M, Motomura T, Mizuno K (2005) Investigation of the relationship between atherosclerosis and paraoxonase or homocysteine thiolactonase activity in patients with type 2 diabetes mellitus using a commercially available assay. Clin Chim Acta 359:156–162
Dantoine TF, Debord J, Charmes JP, Merle L, Marquet P, Lachatre G, Leroux-Robert C (1998) Decrease of serum paraoxonase activity in chronic renal failure. J Am Soc Nephrol 9(11):2082–2088
Beltowski J, Wójcicka G, Jamroz A (2003) Leptin decreases plasma paraoxonase 1 (PON1) activity and induces oxidative stress: the possible novel mechanism for proatherogenic effect of chronic hyperleptinemia. Atherosclerosis 170:21–29
Senti M, Tomás M, Elosual R, Sala J (2002) The paraoxonase-1 codon 192 polymorphism is associated with fasting total cholesterol and LDL-cholesterol concentrations only in postmenopausal women. The REGICOR study. Clin Chem Lab Med 40:677–683
Iacobellis G, Corradi D, Sharma AM (2005) Epicardial adipose tissue: anatomic, biomolecular and clinical relationships with the heart. Nat Clin Pract Cardiovasc Med 2:536–543
Corradi D, Maestri R, Callegari S, Pastori P, Goldoni M, Luong TV, Bordi C (2004) The ventricular epicardial fat is related to the myocardial mass in normal, ischemic and hypertrophic hearts. Cardiovasc Pathol 13:313–316
Rabkin SW (2014) The relationship between epicardial fat and indices of obesity and the metabolic syndrome: a systematic review and meta-analysis. Metab Syndr Relat Disord 12(1):31–42
Turan MN, Gungor O, Asci G, Kircelli F, Acar T, Yaprak M, Ceylan N, Demirci MS, Bayraktaroglu S, Toz H, Ozkahya M, Ok E (2013) Epicardial adipose tissue volume and cardiovascular disease in hemodialysis patients. Atherosclerosis 226(1):129–133
Turkmen K, Ozbek O, Kayrak M, Samur C, Guler I, Tonbul HZ (2013) Peri-aortic fat tissue thickness in peritoneal dialysis patients. Perit Dial Int 33(3):316–324
Spencer K (1986) Analytical reviews in clinical biochemistry: the estimation of creatinine. Ann Clin Biochem 23:1–25
Zein N, Ganuza C, Kushner I (1979) Significance of C-reactive protein elevation in patients with SLE. Arthritis Rheum 22:7–12
Suchocka Z, Swatowska J, Pachecka J, Suchocka P (2006) RP-HPLC determination of paraoxonase activity in human blood serum. J Pharm Biomed Anal 42:113–119
Bertaso AG, Bertol D, Duncan BB, Foppa M (2013) Epicardial fat definition, measurements and systematic review of main outcomes. Arq Bras Cardiol 101(1):e18–e28
Nusair MB, Rajpurohit N, Alpert MA (2012) Chronic inflammation and coronary atherosclerosis in patients with end-stage renal disease. Cardiorenal Med 2:117–124
Moradi H, Pahl MV, Elahimehr R, Vaziri ND (2009) Impaired antioxidant activity of high-density lipoprotein in chronic kidney disease. Transl Res 153:77–85
Pahl MV, Ni Z, Sepassi L, Moradi H, Vaziri ND (2009) Plasma phospholipid transfer protein, cholesteryl ester transfer protein and lecithin:cholesterol acyltransferase in end-stage renal disease (ESRD). Nephrol Dial Transplant 24:2541–2546
Moradi H, Said HM, Vaziri ND (2013) Post-transcriptional nature of uremia-induced downregulation of hepatic apolipoprotein A-I production. Transl Res 161:477–485
Çolak H, Kilicarslan B, Tekce H, Tanrisev M, Tugmen C, Aktas G, Kursat S (2015) Relationship between epicardial adipose tissue, inflammation and volume markers in hemodialysis and transplant patients. Ther Apher Dial 19(1):56–62
Dirican M, Akca R, Sarandol E, Dilek K (2004) Serum paraoxonase activity in uremic predialysis and hemodialysis patients. J Nephrol 17(6):813–818
Saeed SA, Elsharkawy M, Elsaeed K, Fooda O (2008) Paraoxonase-1 (PON1) activity as a risk factor for atherosclerosis in chronic renal failure patients. Hemodial Int 12(4):471–479
Sztanek F, Seres I, Harangi M, Lo′′csey L, Padra J, Paragh GJR, Asztalos L, Paragh G (2012) Decreased paraoxonase 1 (PON1) lactonase activity in hemodialyzed and renal transplanted patients. A novel cardiovascular biomarker in end-stage renal disease. Nephrol Dial Transplant 27(7):2866–2872
Sumegová K, Blažíček P, Fuhrman B, Waczulíková I, Ďuračková Z (2006) Paraoxonase 1 (PON1) and its relationship to lipid variables, age and gender in healthy volunteers. Biologia 61(6):699–704
Hasselwander O, Dorothy MM, Fogarty DG, Maxwell AP, Nicholls DP, Young IS (1998) Serum Paraoxonase1 (PON1) and platelet activating factor acetylhydrolase in chronic renal failure. Clin Chem 44:179–181
Gugliucci A, Kinugasa E, Kotani K, Caccavello R, Kimura S (2011) Serum paraoxonase 1 (PON1) lactonase activity is lower in end-stage renal disease patients than in healthy control subjects and increases after hemodialysis. Clin Chem Lab Med 49:61–67
Altun B, Tasolar H, Eren N, Binnetoğlu E, Altun M, Temiz A, Gazi E, Barutcu A, Altunoren O, Colkesen Y, Uysal F (2014) Epicardial adipose tissue thickness in hemodialysis patients. Echocardiography 31(8):941–946
Macunluoglu B, Atakan A, Ari E, Kaya Y, Kaspar C, Demir H, Alp HH (2014) Epicardial fat tissue thickness is correlated with diminished levels of co-enzyme Q10, a major antioxidant molecule among hemodialysis patients. Clin Biochem 47(13–14):1231–1234
Atakan A, Macunluoglu B, Kaya Y, Ari E, Demir H, Asicioglu E, Kaspar C (2014) Epicardial fat thickness is associated with impaired coronary flow reserve in hemodialysis patients. Hemodial Int 18(1):62–69
Graham-Brown MPM, McCann GP, Burton JO (2015) Epicardial adipose tissue in patients with end-stage renal disease on haemodialysis. Curr Opin Nephrol Hypertens 24(6):517–524
Turan MN, Gungor O, Asci G, Kircelli F, Acar T, Yaprak M, Ceylan N, Demirci MS, Bayraktaroglu S, Toz H, Ozkahya M, Ercan OK (2013) Epicardial adipose tissue volume and cardiovascular disease in hemodialysis patients. Atherosclerosis 226(1):129–133
Rozenberg O, Rosenblat M, Coleman R, Shih DM, Aviram M (2003) Paraoxonase (PON1) deficiency is associated with increased macrophage oxidative stress: studies in PON1-knockout mice. Free Radic Biol Med 34(6):774–784
Demir B, Demir E, Acıksarı G, Uygun T, Utku IK, Gedikbasi A, Caglar IM, Pirhan O, Tureli HO, Oflar E, Ungan I, Ciftci S, Karakaya O (2014) The association between the epicardial adipose tissue thickness and oxidative stress parameters in isolated metabolic syndrome patients: a multimarker approach. Int J Endocrinol 2014:1–9
Rector RS, Warner SO, Liu Y, Hinton PS, Sun GY, Cox RH, Stump CS, Laughlin MH, Dellsperger KC, Thomas TR (2007) Exercise and diet induced weight loss improves measures of oxidative stress and insulin sensitivity in adults with characteristics of the metabolic syndrome. Am J Physiol Endocrinol Metab 293:E500–E506
Eroglu E, Kocyigit I, Unal A, Korkar H, Karakukcu C, Orscelik O, Sipahioglu MH, Tokgoz B, Oymak O (2015) Serum paraoxonase activity is associated with epicardial fat tissue in renal transplant recipients. Int Urol Nephrol 47(8):1409–1414
Saruhan E, Olgun A, Oztürk K, Akman S, Erbil MK (2007) Age-related paraoxonase activity changes in Turkish population. Ann N Y Acad Sci 1100:218–222
Acknowledgements
Many thanks to Dr. Amna Metwaly, professor of cardiology, Intensive Care Unit, Theodor Bilharz Research Institute, Cairo, Egypt, for her help in study concept and design, acquisition of echocardiographic data, analysis and interpretation of data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was performed in accordance with the Declaration of Helsinki, and the study protocol was approved by the Institute Ethics Committee.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Abstract accepted as a poster presentation in ERA-EDTA, Vienna, Austria, May 21st–24th, 2016.
Rights and permissions
About this article
Cite this article
Abdallah, E., El-Shishtawy, S., Sherif, N. et al. Assessment of the relationship between serum paraoxonase activity and epicardial adipose tissue in hemodialysis patients. Int Urol Nephrol 49, 329–335 (2017). https://doi.org/10.1007/s11255-016-1465-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-016-1465-y