Abstract
Background
Nephrotic syndrome (NS) is an immune-mediated disorder associated with hyperlipidemia. NS has been proposed to be mediated through CD80-related T cell immune response, which could be blocked using soluble cytotoxic T lymphocyte-associated s(CTLA)-4. Although ghrelin is a hormone-modulating lipid metabolism and suppressing immune system, the precise role of ghrelin in NS is not well established.
Methods
We evaluated the levels of ghrelin, soluble CD80 (sCD80) and sCTLA4 in serum and urine in doxorubicin-induced NS in rats. We also investigated the relation between their levels and the levels of serum total cholesterol (TC), triglyceride, albumin and urine protein.
Results
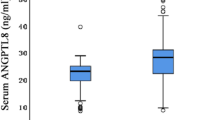
While urinary ghrelin levels were significantly lower in the nephrotic rats compared to the control group, serum ghrelin levels were comparable in the nephrotic and control rats. In contrast, serum and urinary sCD80 and sCTLA4 levels were higher in the nephrotic rats than the controls. The urinary ghrelin levels were negatively correlated with the levels of serum triglyceride, TC and urine protein, sCD80 and sCTLA4. The urine sCD80 levels were positively correlated with the TC, urine protein and urine sCTLA4 levels, and negatively correlated with the serum albumin. The urine sCTLA4 levels were positively correlated with the TC and urine protein levels and negatively correlated with the serum albumin levels. In regression analysis, the urine ghrelin levels significantly relate to urine sCD80 levels. Besides, hyperlipidemia in NS did not appear to be related to serum ghrelin levels.
Conclusion
Low urine ghrelin levels might be relevant to pathogenesis of doxorubicin-induced NS. The reduction in urine ghrelin levels might also be associated with increased levels of urine sCTLA4 and sCD80 which reflect proteinuria.






Similar content being viewed by others
References
Hosoda H, Kojima M, Kangawa K (2006) Biological, physiological, and pharmacological aspects of ghrelin. J Pharmacol Sci 100:398–410
Verhulst PJ, Depoortere I (2012) Ghrelin’s second life: from appetite stimulator to glucose regulator. World J Gastroenterol 18:3183–3195
Kojima M, Kangawa K (2005) Ghrelin: structure and function. Physiol Rev 85:495–522
Lim CT, Kola B, Korbonits M (2011) The ghrelin/GOAT/GHS-R system and energy metabolism. Rev Endocr Metab Disord 12:173–186
Nogueiras R, Wiedmer P, Perez-Tilve D, Veyrat-Durebex C, Keogh JM, Sutton GM, Pfluger PT, Castaneda TR, Neschen S, Hofmann SM et al (2007) The central melanocortin system directly controls peripheral lipid metabolism. J Clin Investig 117:3475–3488
Andrews ZB, Erion DM, Beiler R, Choi CS, Shulman GI, Horvath TL (2010) Uncoupling protein-2 decreases the lipogenic actions of ghrelin. Endocrinology 151:2078–2086
Perez-Tilve D, Hofmann SM, Basford J, Nogueiras R, Pfluger PT, Patterson JT, Grant E, Wilson-Perez HE, Granholm NA, Arnold M, Trevaskis JL, Butler AA, Davidson WS, Woods SC, Benoit SC, Sleeman MW, DiMarchi RD, Hui DY, Tschöp MH (2010) Melanocortin signaling in the CNS directly regulates circulating cholesterol. Nat Neurosci 13:877–882
Cheyuo C, Jacob A, Wang P (2012) Ghrelin-mediated sympathoinhibition and suppression of inflammation in sepsis. Am J Physiol Endocrinol Metab 1(302):E265–E272
Granado M, Priego T, Martin AI, Villanua MA, Lopez-Calderon A (2005) Anti-inflammatory effect of the ghrelin agonist growth hormone-releasing peptide-2 (GHRP-2) in arthritic rats. Am J Physiol Endocrinol Metab 288:486–492
Souza-Moreira L, Campos-Salinas J, Caro M, Gonzalez-Rey E (2011) Neuropeptides as pleiotropic modulators of the immune response. Neuroendocrinology 94:89–100
Rajan D, Wu R, Shah KG, Jacob A, Coppa GF, Wang P (2012) Human ghrelin protects animals from renal ischemia-reperfusion injury through the vagus nerve. Surgery 151:37–47
Khowailed A, Younan SM, Ashour H, Kamel AE, Sharawy N (2015) Effects of ghrelin on sepsis induced acute kidney injury: one step forward. Clin Exp Nephrol 19:419–426
Baatar D, Patel K, Taub DD (2011) The effects of ghrelin on inflammation and the immune system. Mol Cell Endocrinol 20(340):44–58
Elie V, Fakhoury M, Deschênes G, Jacqz-Aigrain E (2012) Physiopathology of idiopathic nephrotic syndrome: lessons from glucocorticoids and epigenetic perspectives. Pediatr Nephrol 27:1249–1256
Shimada M, Araya C, Rivard C, Ishimoto T, Johnson RJ, Garin EH (2011) Minimal change disease: a“two-hit”podocyte immune disorder? Pediatr Nephrol 26:645–649
Cara-Fuentes G, Wasserfall CH, Wang H, Johnson RJ, Garin EH (2014) Minimal change disease: a dysregulation of the podocyte CD80-CTLA-4 axis? Pediatr Nephrol 29:2333–2340
Ling C, Liu X, Shen Y, Chen Z, Fan J, Jiang Y, Meng Q (2015) Urinary CD80 levels as a diagnostic biomarker of minimal change disease. Pediatr Nephrol 30:309–316
Bour-Jordan H, Esensten JH, Martinez-Llordella M, Penaranda C, Stumpf M, Bluestone JA (2011) Intrinsic and extrinsic control of peripheral T-cell tolerance by costimulatory molecules of the CD28/ B7 family. Immunol Rev 241:180–205
Ishimoto T, Shimada M, Araya CE, Huskey J, Garin EH, Johnson RJ (2011) Minimal change disease: a CD80 podocytopathy? Semin Nephrol 31:320–325
Lee VW, Harris DC (2011) Adriamycin nephropathy: a model of focal segmental glomerulosclerosis. Nephrology 16:30–38
Ebal E, Cavalié H, Michaux O, Lac G (2007) Effect of a lipid-enriched diet on body composition and some regulatory hormones of food intake in growing rats. Ann Endocrinol (Paris) 68:366–371
Zhang Z, Li Q, Liu F, Sun Y, Zhang J (2010) Prevention of diet-induced obesity by safflower oil: insights at the levels of PPARalpha, orexin, and ghrelin gene expression of adipocytes in mice. Acta Biochim Biophys Sin (Shanghai) 15(42):202–208
Aydin S, Sahin I, Ozkan Y, Dag E, Gunay A, Guzel SP, Catak Z, Ozercan MR (2012) Examination of the tissue ghrelin expression of rats with diet-induced obesity using radioimmunoassay and immunohistochemical methods. Mol Cell Biochem 365:165–173
Saverino Daniele, Simone Rita, Bagnasco Marcello, Pesce Giampaola (2010) The soluble CTLA-4 receptor and its role in autoimmune diseases: an update. Autoimmun Highlights 1:73–81
Taub DD (2008) Novel connections between the neuroendocrine and immune systems: the ghrelin immunoregulatory network. Vitam Hormon 77:325–346
Cheyuo C, Wu R, Zhou M, Jacob A, Coppa G, Wang P (2011) Ghrelin suppresses inflammation and neuronal nitric oxide synthase in focal cerebral ischemia via the vagus nerve. Shock 35:258–265
Taub DD, Longo DL (2005) Insights into thymic aging and regeneration. Immunol Rev 205:72–93
Garin EH, Diaz LN, Mu W, Wasserfall C, Araya C, Segal M, Johnson RJ (2009) Urinary CD80 excretion increases in idiopathic minimal-change disease. J Am Soc Nephrol 20:260–266
Sakthivel P, Wermeling F, Elmgren A, Hulthe J, Kakoulidou M, Lefvert AK, Lind L (2010) Circulating soluble CTLA-4 is related to inflammatory markers in the 70 year old population. Scand J Clin Lab Investig 70:237–243
Li JY, Yong TY, Michael MZ, Gleadle JM (2010) Review: the role of microRNAs in kidney disease. Nephrology (Carlton) 15:599–608
Luo Y, Wang C, Chen X, Zhong T, Cai X, Chen S, Shi Y, Hu J, Guan X, Xia Z, Wang J, Zen K, Zhang CY, Zhang C (2013) Increased serum and urinary microRNAs in children with idiopathic nephrotic syndrome. Clin Chem 59:658–666
Khella HW, Bakhet M, Lichner Z, Romaschin AD, Jewett MA, Yousef GM (2013) MicroRNAs in kidney disease: an emerging understanding. Am J Kidney Dis 61:798–808
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Duygu Ozkorucu, Nuran Cetin, Nadide Melike Sav and Bilal Yildiz declare that they have no conflict of interest.
Human and animal rights
All applicable international, national and institutional guidelines for the care and use of animals were followed. All animal experiments were approved by the Committee for Animal Experiments of the Eskisehir Osmangazi University (Number: 32/186-1).
Rights and permissions
About this article
Cite this article
Ozkorucu, D., Cetin, N., Sav, N.M. et al. Urine and serum ghrelin, sCD80 and sCTLA-4 levels in doxorubicin-induced experimental nephrotic syndrome. Int Urol Nephrol 48, 1187–1196 (2016). https://doi.org/10.1007/s11255-016-1249-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-016-1249-4