Abstract
Purpose
Chronic kidney disease (CKD) is associated with a high incidence of obstructive sleep apnea (OSA). We assessed the effect of continuous positive airway pressure (CPAP) on renal function in patients with CKD and OSA.
Methods
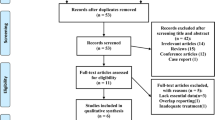
In this retrospective cohort study, 42 patients with Stage 3–5 CKD and OSA were stratified into two groups: patients who use CPAP more (average >4 h/night on >70 % of nights) and patients who use CPAP less (average ≤4 h/night on ≤70 % of nights). Median follow-up time was 2.3 (1.6–2.9) years for greater and 2.0 (0.6–3.5) years for lesser CPAP users. Chart reviews were carried out to record clinical characteristics, proteinuria measurements by urine dipstick, and eGFR values calculated by CKD–EPI equations. Univariate analyses were performed using Wilcoxon rank-sum and Kruskal–Wallis tests. Multivariate logistic regression models were applied to assess eGFR decline after CPAP prescription.
Results
Twelve (29 %) of the 42 subjects used CPAP more. Groups were similar with respect to age, body mass index, blood pressure, Charlson Comorbidity Index, and baseline eGFR and proteinuria. The median rate of decline of eGFR was significantly slower at −0.07 mL/min/1.73 m2/year (range −30 to 13) in those who used more CPAP compared to those who used it less at −3.15 mL/min/1.73 m2/year (range −27 to 7) (p = 0.027).Greater use of CPAP was also associated with a significantly reduced level of proteinuria at 0.15 (range 0.0–3.0) versus 0.70 g/L (range 0.0–3.0) (p = 0.046). Less compliant CPAP users were more likely to have progressive decline of eGFR (decline >3 mL/min/1.73 m2/year), with unadjusted OR 5.0 (95 % CI 0.93–26.8) and adjusted OR 8.9 (95 % CI 1.1–72.8), adjusting for CCI and baseline eGFR.
Conclusions
Compliance to CPAP therapy is associated with a slower rate of progression of CKD in patients with CKD and OSA.

Similar content being viewed by others
References
Turek NF, Ricardo AC, Lash JP (2012) Sleep disturbances as non-traditional risk factors for development and progression of CKD: review of the evidence. Am J Kidney Dis 60(5):823–833
Ozkok A, Kanbay A, Odabas AR et al (2014) Obstructive sleep apnea syndrome and chronic kidney disease: a new cardiorenal risk factor. Clin Exp Hypertens 36(4):211–216
Hanly PJ, Ahmed SB (2014) Sleep apnea and the kidney: is sleep apnea a risk factor for chronic kidney disease? Chest 146(4):1114–1122
Kanbay A, Buyukoglan H, Ozdogan N et al (2012) Obstructive sleep apnea syndrome is related to the progression of chronic kidney disease. Int Urol Nephrol 44(2):535–539
Sim JJ, Rasgon SA, Derose SF (2010) Review article: managing sleep apnoea in kidney diseases. Nephrology 15(2):146–152
Giles TL, Lasserson TJ, Smith BJ (2006) Continuous positive airways pressure for obstructive sleep apnoea in adults. Cochrane Database Syst Rev 25(1):CD001106
Koga S, Ikeda S, Yasunaga T et al (2013) Effects of nasal continuous positive airway pressure on the glomerular filtration rate in patients with obstructive sleep apnea syndrome. Intern Med 52(3):345–349
Kinebuchi S, Kazama JJ, Satoh M et al (2004) Short-term use of continuous positive airway pressure ameliorates glomerular hyperfiltration in patients with obstructive sleep apnoea syndrome. Clin Sci 107(3):317–322
Tahrani AA, Ali A, Raymond NT et al (2013) Obstructive sleep apnea and diabetic nephropathy: a cohort study. Diabetes Care 36(11):3718–3725
Owada T, Yoshihisa A, Yamauchi H et al (2013) Adaptive servoventilation improves cardiorenal function and prognosis in heart failure patients with chronic kidney disease and sleep-disordered breathing. J Card Fail 19(4):225–232
Koyama T, Watanabe H, Terada S et al (2011) Adaptive servo-ventilation improves renal function in patients with heart failure. Respir Med 105(12):1946–1953
Yaşar ZA, Ucar ZZ, Demir AU et al (2014) Does CPAP therapy alter urinary albumin level in adult patients with severe obstructive sleep apnea syndrome? Sleep Breath 18(3):525–532
Kidney Disease Improving Global Outcomes (KDIGO) (2012) Clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int 3(1):19–62
The Report of an American Academy of Sleep Medicine Task Force (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. Sleep 22(5):667–689
Weaver TE, Grunstein RR (2008) Adherence tocontinuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc 5(2):173–178
Collen J, Lettieri C, Kelly W et al (2009) Clinical and polysomnographic predictors of short-term continuous positive airway pressure compliance. Chest 135(3):704–709
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Beecroft JM, Pierratos A, Hanly PJ (2009) Clinical presentation of obstructive sleep apnea in patients with end-stage renal disease. J Clin Sleep Med 5(2):115–121
Elias RM, Bradley TD, Kasai T et al (2012) Rostral overnight fluid shift in end-stage renal disease: relationship with obstructive sleep apnea. Nephrol Dial Transpl 27:1569–1573
Nicholl DD, Hanly PJ, Poulin MJ et al (2014) Evaluation of continuous positive airway pressure therapy on renin-angiotensin system activity in obstructive sleep apnea. Am J Respir Crit Care Med 190(5):572–580
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare they have no conflict of interest, and no disclosure of grants or funding to make. The research protocol was approved by the institutional Research Ethics Board and designed and conducted in accordance with the Declaration of Helsinki. For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Puckrin, R., Iqbal, S., Zidulka, A. et al. Renoprotective effects of continuous positive airway pressure in chronic kidney disease patients with sleep apnea. Int Urol Nephrol 47, 1839–1845 (2015). https://doi.org/10.1007/s11255-015-1113-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-1113-y