Abstract
Background
Recently, low serum estradiol levels have been associated with increased cardiovascular risk and mortality in non-uremic patient populations. We investigated the predictive value of serum estradiol levels for mortality in female hemodialysis patients.
Methods
One hundred and forty-seven prevalent female hemodialysis patients were included in March 2005 and followed up for 32 ± 16 months. Serum estradiol levels were determined by ELISA at baseline and studied in relation to cardiovascular and overall mortality.
Results
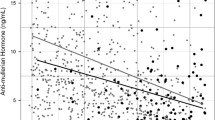
Mean serum estradiol level was 28.6 ± 15.4 pg/ml (5.7–81.3). Patients in the higher estradiol tertile were likely to be more often diabetic and to have more cardiovascular diseases and higher body mass index (BMI). Serum estradiol was inversely correlated with age and urea reduction rate and positively correlated with postdialysis body weight, BMI and hs-CRP levels. During the follow-up period, 52 (35.6 %) patients died. Patients who died were older, had shorter dialysis vintage, were more likely to have a history of diabetes and cardiovascular disease, and lower serum creatinine, albumin, hemoglobin, and higher hs-CRP levels than those who survived. In Cox regression analysis, estradiol levels, in a bimodal (U-shaped) distribution, along with diabetes, low serum albumin and high hs-CRP levels, were predictors for overall mortality.
Conclusions
A U-shaped association between serum estradiol levels and cardiovascular and overall mortality was found in postmenopausal hemodialysis patients.


Similar content being viewed by others
References
Tauchmanovà L, Carrano R, Sabbatini M et al (2004) Hypothalamic-pituitary-gonadal axis function after successful kidney transplantation in men and women. Hum Reprod 19:867–873
Bellinghieri G, Santoro D, Mallamace A, Savica V (2008) Sexual dysfunction in chronic renal failure. J Nephrol 13:113–117
Vanholder R, Massy Z, Argiles A, Spasovski G, Verbeke F, Lameire N (2005) Chronic kidney disease as cause of cardiovascular morbidity and mortality. Nephrol Dial Transplant 20:1048–1056
Shabsigh R, Katz M, Yan G, Makhsida N (2005) Cardiovascular issues in hypogonadism and testosterone therapy. Am J Cardiol 96:67–72
Carrero JJ, Qureshi AR, Parini P et al (2009) Low serum testosterone increase mortality risk among male dialysis patients. J Am Soc Nephrol 20:613–620
Gungor O, Kircelli F, Carrero JJ et al (2010) Endogenous testosterone and mortality in male hemodialysis patients: is it the result of aging? Clin J Am Soc Nephrol 5:2018–2023
Gorton T (1964) Blood pressure of adults by age and sex: United States 1960–1962. Vital Health Stat 11:1–40
Ginsburg ES, Walsh B, Greenberg L, Price D, Chertow GM, Owen WF Jr (1998) Effects of estrogen replacement therapy on the lipoprotein profile in postmenopausal women with ESRD. Kidney Int 54:1344–1350
Seely EW, Walsh BW, Gerhard MD, Williams GH (1999) Estradiol with or without progesterone and ambulatory blood pressure in postmenopausal women. Hypertension 335:1190–1194
Laughlin GA, Ix JH, Cummins K, Allison MA, Daniels LB (2011) Extremes of an aromatase index predict increased 25-year risk of cardiovascular mortality in older women. Clin Endocrinol (Oxf). doi:10.1111/j.1365-2265.2011.04287.x
Rexrode KM, Manson JE, Lee IM et al (2003) Sex hormone levels and risk of cardiovascular events in postmenopausal women. Circulation 108:1688–1693
Stampfer MJ, Colditz GA, Willett WC et al (1991) Postmenopausal estrogen therapy and cardiovascular disease. Ten-year follow-up from the nurses’ health study. N Engl J Med 325:756–762
Wilson PWF, Garrison RJ, Castelli WP (1985) Postmenopausal estrogen use, cigarette smoking, and cardiovascular morbidity in women over 50: the Framingham Study. N Engl J Med 313:1038–1043
Stampfer MJ, Willett WC, Colditz GA, Rosner B, Speizer FE, Hennekens CH (1985) A prospective study of postmenopausal estrogen therapy and coronary heart disease. N Engl J Med 313:1044–1049
Song YS, Yang HJ, Song ES, Han DC, Moon C, Ku JH (2008) Sexual function and quality of life in Korean women with chronic renal failure on hemodialysis: case-control study. Urology 71:243–246
Sugiya N, Nakashima A, Takasugi N et al (2011) Endogenous estrogen may prevent bone loss in postmenopausal hemodialysis patients throughout life. Osteoporos Int 22:1573–1579
Kramer HM, Curhan G, Singh A, HELP Study Group (2003) Hemodialysis and estrogen levels in postmenopausal (HELP) patients: the multicenter HELP study. Am J Kidney Dis 41:1240–1246
McKinlay SM, Brambilla DJ, Posner JG (2008) The normal menopause transition. Maturitas 61:4–16
Nakamura S, Yoshimura M, Nakayama M et al (2004) Possible association of heart failure status with synthetic balance between aldosterone and dehydroepiandrosterone in human heart. Circulation 110:1787–1793
Patten RD, Pourati I, Aronovitz MJ et al (2004) 17 beta-estradiol reduces cardiomyocyte apoptosis in vivo and in vitro via activation of phospho-inositide-3 kinase/Akt signaling. Circ Res 95:692–699
Heine PA, Taylor JA, Iwamoto GA, Lubahn DB, Cooke PS (2000) Increased adipose tissue in male and female estrogen receptor-alpha knockout mice. Proc Natl Acad Sci USA 97:12729–12734
Ohlsson C, Hellberg N, Parini P et al (2000) Obesity and disturbed lipoprotein profile in estrogen receptor-alpha-deficient male mice. Biochem Biophys Res Commun 278:640–645
Barrett-Connor E, Khaw KT (1988) Endogenous sex hormones and cardiovascular disease in men: a prospective population-based study. Circulation 78:539–545
Fukai S, Akishita M, Yamada S et al (2011) Plasma sex hormone levels and mortality in disabled older men and women. Geriatr Gerontol Int 112:196–203
Saltiki K, Papageorgiou G, Voidonikola P et al (2010) Endogenous estrogen levels are associated with endothelial function in males independently of lipid levels. Endocrine 37:329–335
Salpeter SR, Walsh JM, Greyber E, Ormiston TM, Salpeter EE (2004) Mortality associated with hormone replacement therapy in younger and older women: a meta-analysis. J Gen Intern Med 19:791–804
Jankowska EA, Rozentryt P, Ponikowska B et al (2009) Circulating estradiol and mortality in men with systolic chronic heart failure. JAMA 301:1892–1901
Karas RH, Hodgin JB, Kwoun M et al (1999) Estrogen inhibits the vascular injury response in estrogen receptor beta-deficient female mice. Proc Natl Acad Sci USA 96:15133–15136
Cushman M, Legault C, Barrett-Connor E et al (1999) Effect of postmenopausal hormones on inflammation-sensitive proteins: the postmenopausal estrogen/progestin interventions (PEPI) study. Circulation 100:717–722
Nakagami F, Nakagami H, Osako MK et al (2010) Estrogen attenuates vascular remodeling in Lp(a) transgenic mice. Atherosclerosis 211:41–47
Karpuzoglu E, Ahmed SA (2006) Estrogen regulation of nitric oxide and inducible nitric oxide synthase (iNOS) in immune cells: implications for immunity, autoimmune diseases, and apoptosis. Nitric Oxide 15:177–186
Krolner B (1979) Serum levels of testosterone and luteinizing hormone in patients with chronic renal disease. Acta Med Scand 205:623–627
Carrero JJ, Cordeiro AC, Lindholm B, Stenvinkel P (2010) The emerging pleiotrophic role of adipokines in the uremic phenotype. Curr Opin Nephrol Hypertens 19:37–42
Ricks J, Molnar MZ, Kovesdy CP et al (2011) Racial and ethnic differences in the association of body mass index and survival in maintenance hemodialysis patients. Am J Kidney Dis 58:574–582
Ding EL, Song Y, Malik VS, Liu S (2006) Sex differences of endogenous sex hormones and risk of type 2 diabetes: a systematic review and meta-analysis. JAMA 295:1288–1299
Goodman-Gruen D, Barrett-Connor E (2000) Sex differences in the association of endogenous sex hormone levels and glucose tolerance status in older men and women. Diabetes Care 23:912–918
Golden SH, Dobs AS, Vaidya D et al (2007) Endogenous sex hormones and glucose tolerance status in postmenopausal women. J Clin Endocrinol Metab 92:1289–1295
Maggio M, Ceda GP, Lauretani F et al (2009) Relationship between higher estradiol levels and 9-year mortality in older women: the Invecchiare in Chianti study. J Am Geriatr Soc 57:1810–1815
Barros RP, Machado UF, Warner M, Gustafsson JA (2006) Muscle GLUT4 regulation by estrogen receptors ERbeta and ERalpha. Proc Natl Acad Sci USA 31:1605–1608
Acknowledgments
The authors would like to thank all staff of the participating hemodialysis centers for their help and support.
Conflict of interest
The study was supported by Fresenius Medical Care, Turkey with an unrestricted grant. M.T. has worked as a physician at a Fresenius Medical Care Clinic in the last 2 years, and EO is a member of the scientific advisory board of Fresenius Medical Care, Turkey.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tanrisev, M., Asci, G., Gungor, O. et al. Relation between serum estradiol levels and mortality in postmenopausal female hemodialysis patients. Int Urol Nephrol 45, 503–510 (2013). https://doi.org/10.1007/s11255-012-0171-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-012-0171-7