Abstract
Purpose
To evaluate the test–retest reliability of a device that measures urinary sensation during cystometry, and to use that device to determine whether treatment of overactive bladder syndrome (OAB) with solifenacin is associated with a change in urinary sensation.
Methods
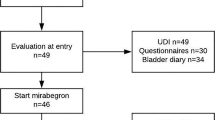
Overall 15 women were recruited for this study, ten women with OAB and urodynamically demonstrated detrusor overactivity and five controls without OAB underwent filling cystometry twice with contemporaneous, continuous recording of urinary sensation. Women with OAB received solifenacin 10 mg daily during the weeks between testing. We compared the areas under the initial and repeat sensation-volume curves.
Results
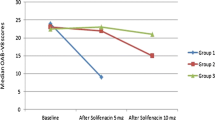
While taking solifenacin, the maximum cystometric capacity increased from 329 ± 168 ml to 464 ± 123 ml (P < 0.002), and the area under the bladder volume-sensation curve decreased (P < 0.0001). Untreated controls did not exhibit these changes.
Conclusion
We present psychometric data demonstrating improved bladder sensation during the treatment of OAB with solifenacin. If clinical correlations are confirmed by future study, such urinary sensation measures may prove useful as assessment, treatment predictor, or outcome measures in OAB research and/or clinical care.



Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM et al (2010) An International urogynecological association (IUGA)/International continence society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J Pelvic Floor Dysfunct 21:5–26
Oliver S, Fowler C, Mundy A, Craggs M (2003) Measuring the sensations of urge and bladder filling during cystometry in urge incontinence and the effects of neuromodulation. Neurourol Urodyn 22:7–16
Lowenstein L, FitzGerald MP, Kenton K, Brubaker L, Gruenwald I, Papier I, Durazo-Arvizu RA, Elliot C, Mueller ER, Vardi Y (2008) Validation of a real-time urodynamic measure of urinary sensation. Am J Obstet Gynecol 198(6):661.e1-4; discussion 661.e4-5
Uebersax JS, Wyman JF, Shumaker SA, McClish DK, Fantl JA (1995) Short forms to assess life quality and symptom distress for urinary incontinence in women: the incontinence impact questionnaire and the urogenital distress inventory. Continence program for women research group. Neurourol Urodyn 14:131–139
Herzog AR, Diokno AC, Brown MB, Normolle DP, Brock BM (1990) Two-year incidence, remission, and change patterns of urinary incontinence in noninstitutionalized older adults. J Gerontol 45:M67–M74
Andersson KE, Yoshida M (2003) Antimuscarinics and the overactive detrusor—which is the main mechanism of action? Eur Urol 43:1–5
Abrams P, Andersson KE, Buccafusco JJ et al (2006) Muscarinic receptors: their distribution and function in body systems, and the implications for treating overactive bladder. Br J Pharmacol 148:565–578
De Laet K, De Wachter S, Wyndaele JJ (2006) Systemic oxybutynin decreases afferent activity of the pelvic nerve of the rat: new insights into the working mechanism of antimuscarinics. Neurourol Urodyn 25:156–161
De Wachter S, De Laet K, Wyndaele JJ (2006) Does the cystometric filling rate affect the afferent bladder response pattern? A study on single fibre pelvic nerve afferents in the rat urinary bladder. Neurourol Urodyn 25:162–167
Kenton K, Lowenstein L, Simmons J, Brubaker L (2007) Aging and overactive bladder may be associated with loss of urethral sensation in women. Neurourol Urodyn 26:981–984
Andersson KE, Chapple CR (2001) Oxybutynin and the overactive bladder. World J Urol 19:319–323
Santos JC, Telo ER (2010) Solifenacin: scientific evidence in the treatment of overactive bladder. Arch Esp Urol 63:197–213
Vardy MD, Mitcheson HD, Samuels TA et al (2009) Effects of solifenacin on overactive bladder symptoms, symptom bother and other patient-reported outcomes: results from VIBRANT—a double-blind, placebo-controlled trial. Int J Clin Pract 63:1702–1714
Acknowledgments
This study was supported by a research grant from Astellas Pharma.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lowenstein, L., Kenton, K., Mueller, E.R. et al. Solifenacin objectively decreases urinary sensation in women with overactive bladder syndrome. Int Urol Nephrol 44, 425–429 (2012). https://doi.org/10.1007/s11255-011-0059-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-011-0059-y