Abstract
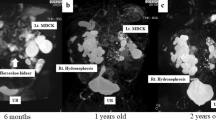
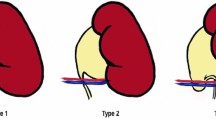
Aberrant vessels is the most common cause of extriensic uretero–pelvic junction (UPJ) obstruction. Due to the left flank pain, 18-year-old male patient with UPJ obstruction due to aberrant vessels in left malrotated kidney and right renal cross ectopia without fusion, had been operated. Ureter was reconstructed and anastomosed anterior to the aberrant vessels after the Double-J-Stent has been placed. At the postoperative period there were improvements in the clinical symptoms and renal function. So, even in the later childhood surgical choice is still the acceptable treatment modality in such cases. To the best of our knowledge, although there are some papers about aberrant vessels which cause UPJ obstruction, there is no such a case with ipsilateral renal hydronephrosis due to aberrant vessels associated with contralateral renal cross ectopia without fusion.
Similar content being viewed by others
References
HH. Nixon (1953) ArticleTitleHydronephrosis in children: a clinical study of seventy-eight cases with special reference to the role of aberrant renal vessels and the reult of conservative operations Br J Surg 40 601 Occurrence Handle13059346
HP. Lee (1949) ArticleTitleCrossed unfused renal ectopia with tumor J Urol 61 333
JW. Ductkett (1993) ArticleTitleWhen to operate on neonatal hydronephrosis Urology 42 617 Occurrence Handle10.1016/0090-4295(93)90522-C Occurrence Handle8256392
JR. Woodard (1993) ArticleTitleHydronephrosis in the neonate Urology 42 620 Occurrence Handle10.1016/0090-4295(93)90523-D Occurrence Handle8256393
RM Parker TG Rudd RK Wonderly JS. Ansel (1981) ArticleTitleUreteropelvic junction obstruction in infants and children: functional evaluation of the obstructed kidney preoperatively and post- operatively J Urol 126 509 Occurrence Handle7288942
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mustafa, M., Alkan, E. Aberrant Vessels in Ipsilateral Malrotated Kidney Associated with Contralateral Cross Ectopia without Fusion. Int Urol Nephrol 37, 39–41 (2005). https://doi.org/10.1007/s11255-004-6075-4
Issue Date:
DOI: https://doi.org/10.1007/s11255-004-6075-4