Abstract
Background
Tandem occlusions exist in 17–32% of large vessel occlusion (LVO) strokes. A significant concern is bleeding when carotid stenting is performed in tandem with thrombectomy due the administration of antiplatelet agents such as glycoprotein IIb/IIIa inhibitors (GP2b3aI) after receiving rtPA, but data are limited in this setting.
Methods
A mutlicenter, retrospective chart review was conducted at two comprehensive stroke centers to assess the safety and efficacy of using GP2b3aI to facilitate carotid stent placement simultaneously with endovascular thrombectomy in patients who have received rtPA.
Results
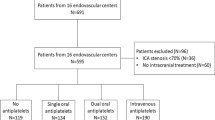
Overall, 32 patients were included in this study, with average age of 66.3 ± 10.4 years and predominantly male (87.5%). The cause of stroke was mostly large artery atherosclerosis (59.4%) and the thrombectomy target vessels were typically first- or second segment middle cerebral artery (37.5% and 31.3%). Time from symptom onset to rtPA bolus was 1.8 h [interquartile range (IQR) 1.5–2.7], rtPA bolus to first pass was 2 h [IQR 1.5–3.1], rtPA bolus to GP2b3aI bolus was 2 h [IQR 1.6–3.5], and rtPA bolus to aspirin and clopidogrel administration was 4.3 h [IQR 2.6–8.9] and 6.6 h [IQR 4.5–11.6] respectively. No patients had acute in-stent thrombosis or post-op bleeding from the access site. Two patients (6.3%) had significant hemorrhagic conversion.
Conclusion
The use of GP2b3aI in the setting of tandem occlusions that required emergent stent placement post-rtPA appears safe and effective. Given the small sample size, these findings should be interpreted cautiously, and need to be confirmed in a larger patient population.

Similar content being viewed by others
References
National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group (1995) Tissue plasminogen activator for acute ischemic stroke. N Engl J Med 333(24):1581–1588. https://doi.org/10.1056/NEJM199512143332401
Gong L, Liu M, Zeng T et al (2015) Crystal structure of the Michaelis complex between tissue-type plasminogen activator and plasminogen activators inhibitor-1. J Biol Chem. https://doi.org/10.1074/jbc.M115.677567
Khan IA, Gowda RM (2003) Clinical perspectives and therapeutics of thrombolysis. Int J Cardiol 91(2–3):115–127. https://doi.org/10.1016/s0167-5273(03)00019-6
Stangl K, Laule M, Tenckhoff B et al (1998) Fibrinogen breakdown, long-lasting systemic fibrinolysis, and procoagulant activation during alteplase double-bolus regimen in acute myocardial infarction. Am J Cardiol. https://doi.org/10.1016/S0002-9149(98)00018-6
Collen D, Lijnen H (1994) Fibrinolysis and the control of hemostasis. In: Stamatoyannopoulos G (ed) The molecular basis of blood disease, 2nd edn. W.B Saunders, pp 662–688
Berkhemer OA, Fransen PSS, Beumer D et al (2014) A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med 372(1):11–20. https://doi.org/10.1056/NEJMoa1411587
Saver JL, Goyal M, Bonafe A et al (2015) Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med. https://doi.org/10.1056/nejmoa1415061
Campbell BCV, Mitchell PJ, Kleinig TJ et al (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med. https://doi.org/10.1056/nejmoa1414792
Goyal M, Demchuk AM, Menon BK et al (2015) Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med. https://doi.org/10.1056/nejmoa1414905
Jovin TG, Chamorro A, Cobo E et al (2015) Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med. https://doi.org/10.1056/nejmoa1503780
Nogueira RG, Jadhav AP, Haussen DC et al (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med. https://doi.org/10.1056/nejmoa1706442
Albers GW, Marks MP, Kemp S et al (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med. https://doi.org/10.1056/nejmoa1713973
Sacco RL, Adams R, Albers G et al (2006) Guidelines for prevention of stroke in patients with ischemic stroke or transient ischemic attack: a statement for healthcare professionals from the American Heart Association/American Stroke Association council on stroke—Council on Cardiovascular Radiology and Intervention: the American Academy of Neurology affirms the value of this guideline. Stroke. https://doi.org/10.1161/01.STR.0000199147.30016.74
Kim KS, Fraser JF, Grupke S, Cook AM (2018) Management of antiplatelet therapy in patients undergoing neuroendovascular procedures. J Neurosurg. https://doi.org/10.3171/2017.5.JNS162307
Barra ME, Berger K, Tesoro EP, Brophy GM (2019) Periprocedural neuroendovascular antiplatelet strategies for thrombosis prevention in clopidogrel-hyporesponsive patients. Pharmacotherapy. https://doi.org/10.1002/phar.2228
Dornbos D, Katz JS, Youssef P, Powers CJ, Nimjee SM (2018) Glycoprotein IIb/IIIa inhibitors in prevention and rescue treatment of thromboembolic complications during endovascular embolization of intracranial aneurysms. Clin Neurosurg. https://doi.org/10.1093/neuros/nyx170
Jadhav AP, Zaidat OO, Liebeskind DS et al (2019) Emergent management of tandem lesions in acute ischemic stroke. Stroke. https://doi.org/10.1161/strokeaha.118.021893
Behme D, Mpotsaris A, Zeyen P et al (2015) Emergency stenting of the extracranial internal carotid artery in combination with anterior circulation thrombectomy in acute ischemic stroke: a retrospective multicenter study. AJNR Am J Neuroradiol 36(12):2340–2345. https://doi.org/10.3174/ajnr.A4459
Assis Z, Menon BK, Goyal M et al (2018) Acute ischemic stroke with tandem lesions: technical endovascular management and clinical outcomes from the ESCAPE trial. J Neurointervent Surg 10(5):429–433. https://doi.org/10.1136/neurintsurg-2017-013316
Yaghi S, Willey JZ, Cucchiara B et al (2017) Treatment and outcome of hemorrhagic transformation after intravenous alteplase in acute ischemic stroke a scientific statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. https://doi.org/10.1161/STR.0000000000000152
Sabatine MS, Morrow DA, Giugliano RP et al (2005) Association of hemoglobin levels with clinical outcomes in acute coronary syndromes. Circulation. https://doi.org/10.1161/01.CIR.0000162477.70955.5F
Mehran R, Rao SV, Bhatt DL et al (2011) Standardized bleeding definitions for cardiovascular clinical trials: a consensus report from the bleeding academic research consortium. Circulation. https://doi.org/10.1161/CIRCULATIONAHA.110.009449
Wahlgren N, Ahmed N, Dávalos A et al (2007) Thrombolysis with alteplase for acute ischaemic stroke in the Safe Implementation of Thrombolysis in Stroke-Monitoring Study (SITS-MOST): an observational study. Lancet (Lond, Engl) 369(9558):275–282. https://doi.org/10.1016/S0140-6736(07)60149-4
Jacquin G, Poppe AY, Labrie M et al (2019) Lack of consensus among stroke experts on the optimal management of patients with acute tandem occlusion. Stroke. https://doi.org/10.1161/STROKEAHA.118.023758
Heck DV, Brown MD (2015) Carotid stenting and intracranial thrombectomy for treatment of acute stroke due to tandem occlusions with aggressive antiplatelet therapy may be associated with a high incidence of intracranial hemorrhage. J Neurointervent Surg 7(3):170–175. https://doi.org/10.1136/neurintsurg-2014-011224
Steglich-Arnholm H, Holtmannspötter M, Kondziella D et al (2015) Thrombectomy assisted by carotid stenting in acute ischemic stroke management: benefits and harms. J Neurol 262(12):2668–2675. https://doi.org/10.1007/s00415-015-7895-0
Papanagiotou P, Roth C, Walter S et al (2011) Carotid artery stenting in acute stroke. J Am Coll Cardiol 58(23):2363–2369. https://doi.org/10.1016/j.jacc.2011.08.044
Funding
No funding was obtained for the conduction of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors of this study have no direct or indirect conflicts of interest to disclose.
Ethical approval
Ethical approval was waived by the local Ethics Committee of The Ohio State University in view of the retrospective nature of the study and all the procedures being performed were part of the routine care.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Smetana, K.S., Zakeri, A., Dolia, J. et al. Management of tandem occlusions in patients who receive rtPA. J Thromb Thrombolysis 52, 1182–1186 (2021). https://doi.org/10.1007/s11239-021-02510-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-021-02510-7