Abstract
Antiplatelet agents and statin therapies are widely used in patients with known cardiovascular disease. Plaque rupture (PR) and plaque erosion (PE) are the most frequent underlying mechanisms of acute coronary syndromes (ACS). The conditions and medications that are associated with ST-segment elevation myocardial infarction (STEMI) following PR or PE have not been systematically studied. A total of 838 ACS patients (494 with STEMI, 344 with NSTE-ACS) who were diagnosed with PR or PE by optical coherence tomography were included. The patients were categorized into two groups based on underlying pathology, and the baseline characteristics and culprit plaque morphology associated with STEMI were investigated within each group. Among 838 patients, 467 (55.7%) had PR, and 371 (44.3%) were diagnosed with PE. Among patients with PR, older age, hyperlipidemia, no antiplatelet therapy, higher level of low-density lipoprotein cholesterol, and greater lipid burden and macrophage infiltration were associated with increased probability of STEMI. Among patients with PE, no dual antiplatelet therapy and no statin therapy were associated with increased probability of STEMI. The incidence of STEMI caused by PR was significantly lower on antiplatelet therapy (P < 0.001), and the incidence of STEMI caused by PE was significantly lower on antiplatelet therapy (P < 0.001) or on statin therapy (P < 0.001). Antiplatelet therapy is associated with lower probability of STEMI, regardless of underlying pathology, and statin therapy is associated with lower probability of STEMI in PE as clinical presentation of ACS.
Graphic Abstract
Statin therapy prior to the onset of acute coronary syndromes (ACS) may reduce the probability of plaque rupture. Antiplatelet therapy prior to the onset of ACS is associated with reduced probability of ST-segment elevation myocardial infarction (STEMI) following both plaque rupture and plaque erosion, and dual antiplatelet therapy offers additional protection compared to a single antiplatelet agent in plaque erosion. The combination of statin and antiplatelet therapy may have an additive effect on reducing the probability of STEMI caused by plaque erosion.
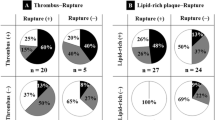
Yellow: lipid pool(necrotic core); red: fibrin-rich thrombus; gray; platelet-rich thrombus



Similar content being viewed by others
References
Davies MJ (2000) The pathophysiology of acute coronary syndromes. Heart 83:361–366. https://doi.org/10.1136/heart.83.3.361
Bentzon JF, Otsuka F, Virmani R, Falk E (2014) Mechanisms of plaque formation and rupture. Circ Res 114:1852–1866. https://doi.org/10.1161/CIRCRESAHA.114.302721
Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, Prescott E, Storey RF, Deaton C, Cuisset T, Agewall S, Dickstein K, Edvardsen T, Escaned J, Gersh BJ, Svitil P, Gilard M, Hasdai D, Hatala R, Mahfoud F, Masip J, Muneretto C, Valgimigli M, Achenbach S, Bax JJ, Group ESCSD (2020) 2019 ESC guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J 41:407–477. https://doi.org/10.1093/eurheartj/ehz425
Rich JD, Cannon CP, Murphy SA, Qin J, Giugliano RP, Braunwald E (2010) Prior aspirin use and outcomes in acute coronary syndromes. J Am Coll Cardiol 56:1376–1385. https://doi.org/10.1016/j.jacc.2010.06.028
Spencer FA, Allegrone J, Goldberg RJ, Gore JM, Fox KA, Granger CB, Mehta RH, Brieger D, Investigators G (2004) Association of statin therapy with outcomes of acute coronary syndromes: the GRACE study. Ann Intern Med 140:857–866. https://doi.org/10.7326/0003-4819-140-11-200406010-00006
Jia H, Abtahian F, Aguirre AD, Lee S, Chia S, Lowe H, Kato K, Yonetsu T, Vergallo R, Hu S, Tian J, Lee H, Park SJ, Jang YS, Raffel OC, Mizuno K, Uemura S, Itoh T, Kakuta T, Choi SY, Dauerman HL, Prasad A, Toma C, McNulty I, Zhang S, Yu B, Fuster V, Narula J, Virmani R, Jang IK (2013) In vivo diagnosis of plaque erosion and calcified nodule in patients with acute coronary syndrome by intravascular optical coherence tomography. J Am Coll Cardiol 62:1748–1758. https://doi.org/10.1016/j.jacc.2013.05.071
Kolodgie FD, Burke AP, Wight TN, Virmani R (2004) The accumulation of specific types of proteoglycans in eroded plaques: a role in coronary thrombosis in the absence of rupture. Curr Opin Lipidol 15:575–582. https://doi.org/10.1097/00041433-200410000-00012
Sato Y, Hatakeyama K, Yamashita A, Marutsuka K, Sumiyoshi A, Asada Y (2005) Proportion of fibrin and platelets differs in thrombi on ruptured and eroded coronary atherosclerotic plaques in humans. Heart 91:526–530. https://doi.org/10.1136/hrt.2004.034058
Damman P, de Winter RJ (2017) Timing of revascularisation for acute coronary syndrome. Lancet 390:717–718. https://doi.org/10.1016/S0140-6736(17)31632-X
Ino Y, Kubo T, Tanaka A, Kuroi A, Tsujioka H, Ikejima H, Okouchi K, Kashiwagi M, Takarada S, Kitabata H, Tanimoto T, Komukai K, Ishibashi K, Kimura K, Hirata K, Mizukoshi M, Imanishi T, Akasaka T (2011) Difference of culprit lesion morphologies between st-segment elevation myocardial infarction and non-st-segment elevation acute coronary syndrome: an optical coherence tomography study. JACC Cardiovasc Interv 4:76–82. https://doi.org/10.1016/j.jcin.2010.09.022
Yonetsu T, Lee T, Murai T, Kanno Y, Hamaya R, Ichijo S, Niida T, Hada M, Araki M, Matsuda J, Usui E, Hoshino M, Kanaji Y, Kakuta T (2017) Association between prior aspirin use and morphological features of culprit lesions at first presentation of acute coronary syndrome assessed by optical coherence tomography. Circ J 81:511–519. https://doi.org/10.1253/circj.CJ-16-0957
Amabile N, Hammas S, Fradi S, Souteyrand G, Veugeois A, Belle L, Motreff P, Caussin C (2015) Intra-coronary thrombus evolution during acute coronary syndrome: regression assessment by serial optical coherence tomography analyses. Eur Heart J Cardiovasc Imaging 16:433–440. https://doi.org/10.1093/ehjci/jeu228
Barrabes JA, Galian L (2010) Endogenous thrombolysis: a hidden player in acute coronary syndromes? J Am Coll Cardiol 55:2116–2117. https://doi.org/10.1016/j.jacc.2010.01.034
Baigent C, Blackwell L, Collins R, Emberson J, Godwin J, Peto R, Buring J, Hennekens C, Kearney P, Meade T, Patrono C, Roncaglioni MC, Zanchetti A (2009) Aspirin in the primary and secondary prevention of vascular disease: collaborative meta-analysis of individual participant data from randomised trials. Lancet 373:1849–1860. https://doi.org/10.1016/S0140-6736(09)60503-1
Hurlen M, Abdelnoor M, Smith P, Erikssen J, Arnesen H (2002) Warfarin, aspirin, or both after myocardial infarction. N Engl J Med 347:969–974. https://doi.org/10.1056/NEJMoa020496
Jia H, Dai J, Hou J, Xing L, Ma L, Liu H, Xu M, Yao Y, Hu S, Yamamoto E, Lee H, Zhang S, Yu B, Jang IK (2017) Effective anti-thrombotic therapy without stenting: Intravascular optical coherence tomography-based management in plaque erosion (the erosion study). Eur Heart J 38:792–800. https://doi.org/10.1093/eurheartj/ehw381
Sugiyama T, Xing L, Yamamoto E, Fracassi F, Lee H, Yu B, Jang IK (2018) Thrombus resolution with tirofiban in the conservative management of patients presenting with plaque erosion. Coron Artery Dis 29:301–308. https://doi.org/10.1097/MCA.0000000000000614
Schartl M, Bocksch W, Koschyk DH, Voelker W, Karsch KR, Kreuzer J, Hausmann D, Beckmann S, Gross M (2001) Use of intravascular ultrasound to compare effects of different strategies of lipid-lowering therapy on plaque volume and composition in patients with coronary artery disease. Circulation 104:387–392. https://doi.org/10.1161/hc2901.093188
Komukai K, Kubo T, Kitabata H, Matsuo Y, Ozaki Y, Takarada S, Okumoto Y, Shiono Y, Orii M, Shimamura K, Ueno S, Yamano T, Tanimoto T, Ino Y, Yamaguchi T, Kumiko H, Tanaka A, Imanishi T, Akagi H, Akasaka T (2014) Effect of atorvastatin therapy on fibrous cap thickness in coronary atherosclerotic plaque as assessed by optical coherence tomography: The easy-fit study. J Am Coll Cardiol 64:2207–2217. https://doi.org/10.1016/j.jacc.2014.08.045
von Birgelen C, Klinkhart W, Mintz GS, Wieneke H, Baumgart D, Haude M, Bartel T, Sack S, Ge J, Erbel R (2000) Size of emptied plaque cavity following spontaneous rupture is related to coronary dimensions, not to the degree of lumen narrowing. A study with intravascular ultrasound in vivo. Heart 84:483–488. https://doi.org/10.1136/heart.84.5.483
Raffel OC, Merchant FM, Tearney GJ, Chia S, Gauthier DD, Pomerantsev E, Mizuno K, Bouma BE, Jang IK (2008) In vivo association between positive coronary artery remodelling and coronary plaque characteristics assessed by intravascular optical coherence tomography. Eur Heart J 29:1721–1728. https://doi.org/10.1093/eurheartj/ehn286
Scalone G, Niccoli G, Refaat H, Vergallo R, Porto I, Leone AM, Burzotta F, D'Amario D, Liuzzo G, Fracassi F, Trani C, Crea F (2017) Not all plaque ruptures are born equal: an optical coherence tomography study. Eur Heart J Cardiovasc Imaging 18:1271–1277. https://doi.org/10.1093/ehjci/jew208
Libby P, Pasterkamp G, Crea F, Jang IK (2019) Reassessing the mechanisms of acute coronary syndromes. Circ Res 124:150–160. https://doi.org/10.1161/CIRCRESAHA.118.311098
Ferrante G, Nakano M, Prati F, Niccoli G, Mallus MT, Ramazzotti V, Montone RA, Kolodgie FD, Virmani R, Crea F (2010) High levels of systemic myeloperoxidase are associated with coronary plaque erosion in patients with acute coronary syndromes: a clinicopathological study. Circulation 122:2505–2513. https://doi.org/10.1161/CIRCULATIONAHA.110.955302
Kessinger CW, Kim JW, Henke PK, Thompson B, McCarthy JR, Hara T, Sillesen M, Margey RJ, Libby P, Weissleder R, Lin CP, Jaffer FA (2015) Statins improve the resolution of established murine venous thrombosis: Reductions in thrombus burden and vein wall scarring. PLoS ONE 10:e0116621. https://doi.org/10.1371/journal.pone.0116621
Mayyas F, Baydoun D, Ibdah R, Ibrahim K (2018) Atorvastatin reduces plasma inflammatory and oxidant biomarkers in patients with risk of atherosclerotic cardiovascular disease. J Cardiovasc Pharmacol Ther 23:216–225. https://doi.org/10.1177/1074248417753677
Kimura K, Kimura T, Ishihara M, Nakagawa Y, Nakao K, Miyauchi K, Sakamoto T, Tsujita K, Hagiwara N, Miyazaki S, Ako J, Arai H, Ishii H, Origuchi H, Shimizu W, Takemura H, Tahara Y, Morino Y, Iino K, Itoh T, Iwanaga Y, Uchida K, Endo H, Kongoji K, Sakamoto K, Shiomi H, Shimohama T, Suzuki A, Takahashi J, Takeuchi I, Tanaka A, Tamura T, Nakashima T, Noguchi T, Fukamachi D, Mizuno T, Yamaguchi J, Yodogawa K, Kosuge M, Kohsaka S, Yoshino H, Yasuda S, Shimokawa H, Hirayama A, Akasaka T, Haze K, Ogawa H, Tsutsui H, Yamazaki T (2019) JCS 2018 guideline on diagnosis and treatment of acute coronary syndrome. Circ J 83:1085–1196. https://doi.org/10.1253/circj.CJ-19-0133
Yamamoto E, Yonetsu T, Kakuta T, Soeda T, Saito Y, Yan BP, Kurihara O, Takano M, Niccoli G, Higuma T, Kimura S, Minami Y, Ako J, Adriaenssens T, Boeder NF, Nef HM, Fracassi F, Sugiyama T, Lee H, Crea F, Kimura T, Fujimoto JG, Fuster V, Jang IK (2019) Clinical and laboratory predictors for plaque erosion in patients with acute coronary syndromes. J Am Heart Assoc 8:e012322. https://doi.org/10.1161/JAHA.119.012322
Zheng SL, Roddick AJ (2019) Association of aspirin use for primary prevention with cardiovascular events and bleeding events: a systematic review and meta-analysis. JAMA 321:277–287. https://doi.org/10.1001/jama.2018.20578
Wascher TC (2003) Long-term statin safety and efficacy in secondary prevention: can combination therapy improve outcomes? Atheroscler Suppl 4:11–16. https://doi.org/10.1016/s1567-5688(03)90002-x
Hennekens CH, Sacks FM, Tonkin A, Jukema JW, Byington RP, Pitt B, Berry DA, Berry SM, Ford NF, Walker AJ, Natarajan K, Sheng-Lin C, Fiedorek FT, Belder R (2004) Additive benefits of pravastatin and aspirin to decrease risks of cardiovascular disease: randomized and observational comparisons of secondary prevention trials and their meta-analyses. Arch Intern Med 164:40–44. https://doi.org/10.1001/archinte.164.1.40
Acknowledgements
Dr. Jang’s research was supported by Mr. and Mrs. Allan and Gill Gray and by Mr. and Mrs. Michael and Kathryn Park.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Dr. Jang has received educational grants from Abbott Vascular and a consulting fee from Svelte Medical Systems. They had no role in the design or conduct of this research. All other authors have reported that they have no relationships relevant to the contents of this paper to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kurihara, O., Takano, M., Kakuta, T. et al. Determinants of ST-segment elevation myocardial infarction as clinical presentation of acute coronary syndrome. J Thromb Thrombolysis 51, 1026–1035 (2021). https://doi.org/10.1007/s11239-020-02281-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-020-02281-7