Abstract
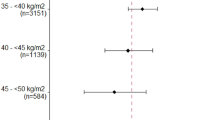
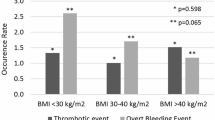
Despite the lack of an optimum dosing strategy in obese patients, warfarin remains the most commonly used anticoagulant. Body mass index (BMI) >30 has been linked to increased time to obtain a therapeutic international normalized ratio on initiation of warfarin as well as higher maintenance dose. Despite higher dosage requirements, few studies have examined the relationship between warfarin and bleeding events in obese individuals. We examined the performance of BMI in predicting the incidence of bleeding at an anticoagulation clinic (ACC) over a 1 year period. Eight hundred and sixty-three patients followed in the ACC over a 1 year period were evaluated for bleeds in relation to BMI [defined as weight (kg)/height (m2)]. Seventy-one of the 863 patients had a bleeding event (8.2 %); mean age 69.5 years and 44 % females. BMI categories were normal weight (21 %), overweight (38 %), obese class I (21 %), II (9 %), and III (11.3 %), respectively. Prevalence of major and minor bleeding events were 4.4 and 3.8 %, respectively. In univariate analyses, hazard ratio (HR) for major bleeding risks increases with higher obesity categories (HR 1.3, 1.85, and 1.93 for classes I, II, III, respectively). In multivariable adjusted model obesity classes II and III significantly increased the risk of major bleeds (HR 1.84, p < 0.001). Bleeding risk is higher in obese compared to normal weight individuals who are on warfarin. These results suggests that BMI plays a role in bleeding events in patients on warfarin.
Similar content being viewed by others
References
Gage BF, Eby C, Johnson JA et al (2000) Management and dosing of warfarin Therapy. Am J Med 109:326–331. doi:10.1038/clpt.2008.10.Use
Lewis JD (1987) The management of the limb in acute venous thrombosis. Blood Rev 1:230–236. doi:10.1016/0268-960X(87)90024-5
Parvizi J, Huang R, Raphael IJ et al (2015) Timing of symptomatic pulmonary embolism with warfarin following arthroplasty. J Arthroplast. doi:10.1016/j.arth.2015.01.004
Arepally GM, Ortel TL (2015) Changing practice of anticoagulation : will target-specific anticoagulants replace warfarin ? Annu Rev Med 66:214–253. doi:10.1146/annurev-med-051113-024633
Kokame GT (2002) Management options for early. Methods 31:118–126
Deykin D (1970) Warfarin therapy (first of two parts). N Engl J Med 283:691–693
Deykin D (1970) Warfarin therapy (second of two parts). N Engl J Med 283:801–803
Thomas IC, Sorrentino MJ (2014) Bleeding risk prediction models in atrial fibrillation. Curr Cardiol Rep 16:1–8. doi:10.1007/s11886-013-0432-9
Loewen P, Dahri K (2011) Risk of bleeding with oral anticoagulants: an updated systematic review and performance analysis of clinical prediction rules. Ann Hematol 90:1191–1200. doi:10.1007/s00277-011-1267-3
Airaksinen KEJ, Suurmunne H, Porela P et al (2010) Usefulness of outpatient bleeding risk index to predict bleeding complications in patients with long-term oral anticoagulation undergoing coronary stenting. Am J Cardiol 106:175–179. doi:10.1016/j.amjcard.2010.03.011
Ruíz-Giménez N, Suárez C, González R et al (2008) Predictive variables for major bleeding events in patients presenting with documented acute venous thromboembolism. Findings from the RIETE Registry. Thromb Haemost 100:26–31. doi:10.1160/TH08-03-0193
Pisters R, Lane DA, Nieuwlaat R et al (2010) A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation: the Euro heart survey. Chest 138:1093–1100. doi:10.1378/chest.10-0134
Lip GYH, Frison L, Halperin JL, Lane DA (2011) Comparative validation of a novel risk score for predicting bleeding risk in anticoagulated patients with atrial fibrillation: the HAS-BLED (hypertension, abnormal renal/liver function, stroke, bleeding history or predisposition, labile INR, elderly, drug). J Am Coll Cardiol 57:173–180. doi:10.1016/j.jacc.2010.09.024
Ciaroni S, Cuenoud L, Bloch A (2000) Clinical study to investigate the predictive parameters for the onset of atrial fibrillation in patients with essential hypertension. Am Heart J 139:814–819
Ashburner JM, Go AS, Reynolds K et al (2015) Comparison of frequency and outcome of major gastrointestinal hemorrhage in patients with atrial fibrillation on versus not receiving warfarin therapy (from the ATRIA and ATRIA-CVRN cohorts). Am J Cardiol 115:40–46. doi:10.1016/j.amjcard.2014.10.006
Mueller JA, Patel T, Halawa A et al (2014) Warfarin dosing and body mass index. Ann Pharmacother 48:584–588. doi:10.1177/1060028013517541
Wallace JL, Reaves AB, Tolley EA et al (2013) Comparison of initial warfarin response in obese patients versus non-obese patients. J Thromb Thrombolysis 36:96–101. doi:10.1007/s11239-012-0811-x
Gurwitz J, Avorn J (1992) Aging and the anticoagulant response to warfarin therapy. Ann Intern Med 116:901–904
Kamali F, Khan TI, King BP et al (2004) Contribution of age, body size, and CYP2C9 genotype to anticoagulant response to warfarin. Clin Pharmacol Ther 75:204–212. doi:10.1016/j.clpt.2003.10.001
Yoo S-H, Nah H-W, Jo M-W et al (2009) Age and body weight adjusted warfarin initiation program for ischaemic stroke patients. Eur J Neurol 16:1100–1105. doi:10.1111/j.1468-1331.2009.02745.x
Gage BF (2008) Use of pharmacogenetics and clinical factors to predict the therapeutic dose of warfarin. Clin Pharmacol Ther 84(3):326–331.
Yuan H-Y, Chen J-J, Lee MTM et al (2005) A novel functional VKCOR1 promoter polymorphism is associated with inter-individual and inter-ethnic differences in warfarin sensitivity. Hum Mol Genet 14:1745–1751. doi:10.1093/hmg/ddi180
Acknowledgments
We would like to thank Pamela Burgwinkle and Ray Stierer for their contributions in conducting this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ogunsua, A.A., Touray, S., Lui, J.K. et al. Body mass index predicts major bleeding risks in patients on warfarin. J Thromb Thrombolysis 40, 494–498 (2015). https://doi.org/10.1007/s11239-015-1226-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-015-1226-2