Abstract
Purpose
To assess health-related quality of life (HRQOL) among adolescents and young adults (AYAs) with chronic conditions.
Methods
AYAs (N = 872) aged 14–20 years completed NIH’s Patient-Reported Outcomes Measurement Information System® (PROMIS®) measures of physical function, pain interference, fatigue, social health, depression, anxiety, and anger. Latent profile analysis (LPA) was used to group AYAs into HRQOL profiles using PROMIS T-scores. The optimal number of profiles was determined by model fit statistics, likelihood ratio test, and entropy. Multinomial logistic regression models were used to examine how LPA’s HRQOL profile membership was associated with patient demographic and chronic conditions. The model prediction accuracy on profile membership was evaluated using Huberty’s I index with a threshold of 0.35 for good effect.
Results
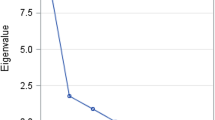
A 4-profile LPA model was selected. A total of 161 (18.5%), 256 (29.4%), 364 (41.7%), and 91 (10.4%) AYAs were classified into Minimal, Mild, Moderate, and Severe HRQOL Impact profiles. AYAs in each profile had distinctive mean scores with over a half standard deviation (5-points in PROMIS T-scores) of difference between profiles across most HRQOL domains. AYAs who were female or had conditions such as mental health condition, hypertension, and self-reported chronic pain were more likely to be in the Severe HRQOL Impact profile. The Huberty’s I index was 0.36.
Conclusions
Approximately half of AYAs with a chronic condition experience moderate to severe HRQOL impact. The availability of risk prediction models for HRQOL impact will help to identify AYAs who are in greatest need of closer clinical care follow-up.


Similar content being viewed by others
Data availability
The study data contain confidential patient information and cannot be deposited to a public repository.
References
Gore, F. M., et al. (2011). Global burden of disease in young people aged 10–24 years: A systematic analysis. The Lancet, 377(9783), 2093–2102.
Yeo, M., & Sawyer, S. (2005). Chronic illness and disability. BMJ, 330(7493), 721–723.
Sprangers, M. A. G. (2002). Quality-of-life assessment in oncology. Acta Oncologica, 41(3), 229–237.
Cella, D. F., & Tulsky, D. S. (1990). Measuring quality of life today: methodological aspects. Oncology (Williston Park, N.Y.), 4(5), 29–38. discussion 69.
Siegrist, J., & Junge, A. (1989). Conceptual and methodological problems in research on the quality of life in clinical medicine. Social Science and Medicine, 29(3), 463–468.
Stewart, A. L., et al. (1989). Functional status and well-being of patients with chronic conditions: Results from the medical outcomes study. JAMA, 262(7), 907–913.
Schlenk, E. A., et al. (1997). Health-related quality of life in chronic disorders: A comparison across studies using the MOS SF-36. Quality of life research, 7(1), 57–65.
Langeveld, N. E., et al. (2002). Quality of life in young adult survivors of childhood cancer. Supportive Care in Cancer, 10(8), 579–600.
Ashing-Giwa, K. T., et al. (2007). Examining predictive models of HRQOL in a population-based, multiethnic sample of women with breast carcinoma. Quality of Life Research, 16(3), 413–428.
Bellizzi, K. M., et al. (2012). Double jeopardy? Age, race, and HRQOL in older adults with cancer. Journal of Cancer Epidemiology, 2012, 1–9.
Clauser, S. B., et al. (2008). Disparities in HRQOL of cancer survivors and non-cancer managed care enrollees. Health Care Financing Review, 29(4), 23.
Deimling, G. T., et al. (2005). The health of older-adult, long-term cancer survivors. Cancer Nursing, 28(6), 415–424.
Varni, J. W., Limbers, C. A., & Burwinkle, T. M. (2007). Impaired health-related quality of life in children and adolescents with chronic conditions: a comparative analysis of 10 disease clusters and 33 disease categories/severities utilizing the PedsQL™ 4.0 Generic Core Scales. Health and Quality of Life Outcomes, 5(1), 43.
Uzark, K., et al. (2008). Quality of life in children with heart disease as perceived by children and parents. Pediatrics, 121(5), e1060–e1067.
Devinsky, O., et al. (1999). Risk factors for poor health-related quality of life in adolescents with epilepsy. Epilepsia, 40(12), 1715–1720.
Hallstrand, T. S., et al. (2003). Quality of life in adolescents with mild asthma. Pediatric Pulmonology, 36(6), 536–543.
Gaspar, T., et al. (2010). Quality of life: differences related to gender, age, socio-economic status and health status, in Portuguese teens. Revista de Psicologia da Criança e do Adolescente, 2, 87–104.
Colver, A., et al. (2015). Self-reported quality of life of adolescents with cerebral palsy: A cross-sectional and longitudinal analysis. The Lancet, 385(9969), 705–716.
Parkinson, K. N., et al. (2015). Influence of adiposity on health-related quality of life in the Gateshead Millennium Study cohort: Longitudinal study at 12 years. Archives of Disease in Childhood, 100(8), 779–783.
Kaczmarek, C., Haller, D. M., & Yaron, M. (2016). Health-related quality of life in adolescents and young adults with polycystic ovary syndrome: A systematic review. Journal of pediatric and adolescent gynecology, 29(6), 551–557.
Kamp-Becker, I., et al. (2010). Health-related quality of life in adolescents and young adults with high functioning autism-spectrum disorder. Psychosocial Medicine. https://doi.org/10.3205/psm000065
Jennes-Coussens, M., Magill-Evans, J., & Koning, C. (2006). The quality of life of young men with Asperger syndrome: A brief report. Autism, 10(4), 403–414.
Jörngården, A., Wettergen, L., & von Essen, L. (2006). Measuring health-related quality of life in adolescents and young adults: Swedish normative data for the SF-36 and the HADS, and the influence of age, gender, and method of administration. Health and Quality of Life Outcomes, 4(1), 1–10.
Smith, A. W., et al. (2013). Health-related quality of life of adolescent and young adult patients with cancer in the United States: The adolescent and young adult health outcomes and patient experience study. Journal of Clinical Oncology, 31(17), 2136–2145.
Nelson, T. D., et al. (2014). Health-related quality of life among adolescents in residential care: Description and correlates. American Journal of Orthopsychiatry, 84(3), 226.
Pemberger, S., et al. (2005). Quality of life in long-term childhood cancer survivors and the relation of late effects and subjective well-being. Supportive Care in Cancer, 13(1), 49–56.
Wang, J., & Lanza, S. T. (2010). Preface of methods and applications of mixture models, special journal issue of advances and applications of statistical sciences. Advances and Applications in Statistical Sciences, 3, 1–6.
Wang, J., & Wang, X. (2012). Structural equation modeling with Mplus: Methods and applications. Wiley.
Buckner, T. W., et al. (2014). Patterns of symptoms and functional impairments in children with cancer. Pediatric Blood & Cancer, 61(7), 1282–1288.
Hinds, P. S., et al. (2021). Subjective toxicity profiles of children in treatment for cancer: A new guide to supportive care? Journal of Pain and Symptom Management, 61(6), 1188-1195.e2.
Barsevick, A. M., & Aktas, A. (2013). Cancer symptom cluster research: New perspectives and tools. Current Opinion in Supportive and Palliative Care, 7(1), 36–37.
Davis, P. J., et al. (2003). Multidimensional subgroups in migraine: Differential treatment outcome to a pain medicine program. Pain Medicine, 4(3), 215–222.
Miaskowski, C., et al. (2006). Online exclusive-subgroups of patients with cancer with different symptom experiences and quality-of-life outcomes: A cluster analysis. Oncology Nursing Forum, 33, E79–E89.
Laursen, B., & Hoff, E. (2006). Person-centered and variable-centered approaches to longitudinal data. Merrill-Palmer Quarterly (1982-), 52, 377–389.
Stewart, D. W. (1981). The application and misapplication of factor analysis in marketing research. Journal of Marketing Research, 18(1), 51–62.
Olaya, B., et al. (2017). Latent class analysis of multimorbidity patterns and associated outcomes in Spanish older adults: A prospective cohort study. BMC Geriatrics, 17, 1–10.
Larsen, F. B., et al. (2017). A latent class analysis of multimorbidity and the relationship to socio-demographic factors and health-related quality of life. A national population-based study of Danish adults. PLoS ONE, 12(1), e0169426.
Garey, L., et al. (2019). Health-related quality of life among homeless smokers: Risk and protective factors of latent class membership. Behavioral Medicine, 45(1), 40–51.
Huang, J., et al. (2023). Health-related quality of life in Chinese medical staff: A latent profile analysis. Frontiers in Public Health. https://doi.org/10.3389/fpubh.2023.1183483
Kenzik, K. M., et al. (2015). Health-related quality of life in lung cancer survivors: Latent class and latent transition analysis. Cancer, 121(9), 1520–1528.
Dyball, S., et al. (2022). Determinants of health-related quality of life across the spectrum of connective tissue diseases using latent profile analysis: Results from the LEAP cohort. Rheumatology. https://doi.org/10.1093/rheumatology/keac680
Grant, R. W., et al. (2020). Use of latent class analysis and k-means clustering to identify complex patient profiles. JAMA Network Open, 3(12), e2029068.
Băjenaru, L., et al. (2022). Latent profile analysis for quality of life in older patients. BMC Geriatrics, 22(1), 1–7.
Michie, S., Miles, J., & Weinman, J. (2003). Patient-centredness in chronic illness: What is it and does it matter? Patient Education and Counseling, 51(3), 197–206.
Wong, A. W., et al. (2023). Use of latent class analysis and patient reported outcome measures to identify distinct long COVID phenotypes: A longitudinal cohort study. PLoS ONE, 18(6), e0286588.
Shoop-Worrall, S. J., et al. (2021). Patient-reported wellbeing and clinical disease measures over time captured by multivariate trajectories of disease activity in individuals with juvenile idiopathic arthritis in the UK: A multicentre prospective longitudinal study. The Lancet Rheumatology, 3(2), e111–e121.
Basch, E., et al. (2022). Effect of electronic symptom monitoring on patient-reported outcomes among patients with metastatic cancer: A randomized clinical trial. JAMA, 327(24), 2413–2422.
Lee, J. J., et al. (2021). Longitudinal analysis of symptom-based clustering in patients with primary Sjogren’s syndrome: A prospective cohort study with a 5-year follow-up period. Journal of Translational Medicine, 19, 1–8.
Lanza, S. T., & Cooper, B. R. (2016). Latent Class Analysis for Developmental Research. Child Development Perspectives, 10(1), 59–64.
Kiresuk, T. J., Smith, A., & Cardillo, J. E. (2014). Goal attainment scaling: Applications, theory, and measurement. Psychology Press.
Cairns, A., et al. (2015). Setting measurable goals with young people: Qualitative feedback from the Goal Attainment Scale in youth mental health. British Journal of Occupational Therapy, 78(4), 253–259.
Reeve, B. B., et al. (2016). Linkage between the PROMIS® pediatric and adult emotional distress measures. Quality of Life Research, 25(4), 823–833.
Neff, J. M., et al. (2002). Identifying and classifying children with chronic conditions using administrative data with the clinical risk group classification system. Ambulatory Pediatrics, 2(1), 71–79.
Bethell, C. D., et al. (2002). Identifying children with special health care needs: Development and evaluation of a short screening instrument. Ambulatory Pediatrics, 2(1), 38–48.
Cella, D., et al. (2019). PROMIS® adult health profiles: Efficient short-form measures of seven health domains. Value in Health, 22(5), 537–544.
PROMIS® Score Cut Points. (2021). [cited 2022 May 2]. Retrieved from https://www.healthmeasures.net/score-and-interpret/interpret-scores/promis/promis-score-cut-points.
Blalock, D. V., et al. (2020). Analysis of differential item functioning in PROMIS® pediatric and adult measures between adolescents and young adults with special health care needs. Psychological Test and Assessment Modeling, 62(4), 417–428.
Bakk, Z., & Kuha, J. (2021). Relating latent class membership to external variables: An overview. British Journal of Mathematical and Statistical Psychology, 74(2), 340–362.
McCutcheon, A. L. (1987). Latent class analysis. Sage.
Spurk, D., et al. (2020). Latent profile analysis: A review and “how to” guide of its application within vocational behavior research. Journal of Vocational Behavior, 120, 103445.
Oberski, D. (2016). Mixture models: Latent profile and latent class analysis. Modern statistical methods for HCI (pp. 275–287). Springer.
Lo, Y. (2001). Testing the number of components in a normal mixture. Biometrika, 88(3), 767–778.
Nylund, K. L., Asparouhov, T., & Muthén, B. O. (2007). Deciding on the number of classes in latent class analysis and growth mixture modeling: A Monte Carlo simulation study. Structural Equation Modeling: A Multidisciplinary Journal, 14(4), 535–569.
Celeux, G., & Soromenho, G. (1996). An entropy criterion for assessing the number of clusters in a mixture model. Journal of Classification, 13(2), 195–212.
Huberty, C. J., & Lowman, L. L. (2000). Group overlap as a basis for effect size. Educational and Psychological Measurement, 60(4), 543–563.
Granado, E. A. (2015). Comparing three effect sizes for latent class analysis. University of North Texas Doctoral Dissertation.
Bakk, Z., & Kuha, J. (2018). Two-step estimation of models between latent classes and external variables. Psychometrika, 83(4), 871–892.
Cohen, J. (2013). Statistical power analysis for the behavioral sciences. Routledge.
Terwee, C. B., et al. (2021). Minimal important change (MIC): A conceptual clarification and systematic review of MIC estimates of PROMIS measures. Quality of Life Research, 30(10), 2729–2754.
Chalkiadis, G. A. (2001). Management of chronic pain in children. Medical Journal of Australia, 175(9), 476–479.
Roth-Isigkeit, A., et al. (2005). Pain among children and adolescents: Restrictions in daily living and triggering factors. Pediatrics, 115(2), e152–e162.
Varni, J. W., et al. (2007). The PedsQL™ as a patient-reported outcome in children and adolescents with fibromyalgia: an analysis of OMERACT domains. Health and Quality of Life Outcomes. https://doi.org/10.1186/1477-7525-5-9
Hunfeld, J. A. M. (2001). Chronic pain and its impact on quality of life in adolescents and their families. Journal of Pediatric Psychology, 26(3), 145–153.
Gold, J. I., et al. (2009). Pediatric chronic pain and health-related quality of life. Journal of Pediatric Nursing, 24(2), 141–150.
Quittner, A. L., et al. (2010). Impact of socioeconomic status, race, and ethnicity on quality of life in patients with cystic fibrosis in the United States. Chest, 137(3), 642–650.
Tulsky, D. S., et al. (2019). Determining a transitional scoring link between PROMIS® pediatric and adult physical health measures. Quality of Life Research, 28(5), 1217–1229.
Acknowledgements
PROMIS® was funded with cooperative agreements from the National Institutes of Health (NIH) Common Fund Initiative U01AR052181. See www.healthmeasures.net for additional information on the PROMIS® initiative. Dr. Suwei Wang is a Measurement and Regulatory Science (MaRS) fellow at Duke University and is funded by Takeda Pharmaceutical. Dr. Cara J. Arizmendi is a MaRS fellow at Duke University and is funded by AstraZeneca.
Funding
PROMIS® was funded with cooperative agreements from the National Institutes of Health (NIH) Common Fund Initiative U01AR052181. See www.nihpromis.org for additional information on the PROMIS® initiative. Dr. Suwei Wang is a Measurement and Regulatory Science (MaRS) fellow at Duke University and is funded by Takeda Pharmaceutical Company. Dr. Cara J. Arizmendi is a MaRS fellow at Duke University and is funded by AstraZeneca.
Author information
Authors and Affiliations
Contributions
Conceptualization, methodology, formal analysis, results interpretation, first draft, draft revision, final draft approval.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. The current study was ruled exempt from IRB review by the Duke University Health System.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
The authors affirm that human research participants provided informed consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, S., Arizmendi, C.J., Blalock, D.V. et al. Health-related quality of life profiles in adolescents and young adults with chronic conditions. Qual Life Res 32, 3171–3183 (2023). https://doi.org/10.1007/s11136-023-03463-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-023-03463-5