Abstract
Objective
To assess the quality of life (QOL) with rivaroxaban in patients with non-valvular atrial fibrilation (NVAF) related to therapeutic compliance.
Methods
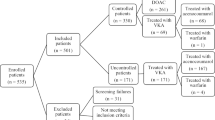
Prospective, longitudinal, multicenter study was developed in 160 Spanish primary or specialized care centers. We included 412 patients treated with rivaroxaban, prescribed for stroke prevention. Three visits were conducted: baseline, 6 and 12 months. Compliance was measured by electronic monitoring systems. QOL was measured by a specific questionnaire. We calculated the percentage of compliance means, the percentage of daily compliers and the score of QOL.
Results
Three hundred and seventy patients finished the study (mean age 75.19 SD: 7.5 years). Daily compliance was 83.5% (CI 78.53–88.57%) (n = 309) and 80% (CI 74.65–85.35%) at 6 and 12 months, respectively. Average QOL rating was 112.85 (SD 29.31) in non-compliant and 111.80 (SD 29.31) in the compliant group (p = Not significant), and after 12 months of 124.67 (SD 30.78) and 83.47 (SD 26.44), respectively (p < 0.0001), with a decrease in the score compliers (p < 0.01) and an increase in non-compliant group (p < 0.05). A higher number of drugs consumed, as well as the number of diseases/conditions suffered, the older age of the patients and having been previously treated with VKA were associated with a higher overall score (worse QOL).
Conclusions
QOL in NVAF patients treated with rivaroxaban improved significantly over the study group at the expense of compliers. A worse QOL was associated with pluripathology, polymedication, older patients and previous treatment with VKA.
Similar content being viewed by others
References
Mani, H., & Lindhoff-Last, E. (2014). New oral anticoagulants in patients with nonvalvular atrial fibrillation: a review of pharmacokinetics, safety, efficacy, quality of life, and cost effectiveness. Drug Design Development and Therapy, 8, 789–798.
Potpara, T. S., Jokic, V., Medic, B., Prostran, M., & Lip, G. Y. (2015). An update on atrial fibrillation: focus on stroke risk reduction strategies. Minerva Medica, 106, 259–273.
Hernández Olmedo, M., & Suárez, Fernández C. (2015). Progress of anticoagulation therapy in atrial fibrillation. Medicina Clinica (BARC), 145, 124–130.
de Andrés-Nogales, F., Oyagüez, I., Betegón-Nicolás, L., Canal-Fontcuberta, C., & Soto-Álvarez, J. (2015). Status of oral anticoagulant treatment in patients with nonvalvular atrial fibrillation in Spain. REACT-AF Study. Rev Clin Esp, 215, 73–82.
Camm, A. J., Lip, G. Y., de Caterina, R., Savelieva, I., Atar, D., Hohnloser, S. H., et al (2012). 2012 focused update of the ESC Guidelines for the management of atrial fibrillation: an update of the 2010 ESC Guidelines for the management of atrial fibrillation. Developed with the special contribution of the European Heart Rhythm Association. Europace, 14, 1385–413.
Hernández Olmedo, M., & Suárez, Fernández C. (2015). Progress of anticoagulation therapy in atrial fibrillation. Medicina Clinica (BARC), 145, 124–130.
Miller, C. S., Grandi, S. M., Shimony, A., Filion, K. B., & Eisenberg, M. J. (2012). Meta-analysis of efficacy and safety of new oral anticoagulants (dabigatran, rivaroxaban, apixaban) versus warfarin in patients with atrial fibrillation. The American Journal of Cardiology, 110, 453–460.
Newby, L. K., LaPointe, N. M., Chen, A. Y., Kramer, J. M., Hammill, B. G., DeLong, E. R., et al. (2006). Long-term adherence to evidence-based secondary prevention therapies in coronary artery disease. Circulation, 113, 203–212.
Amin, A., & Marrs, J. C. (2016). Direct oral anticoagulants for the management of thromboembolic disorders: The importance of adherence and persistence in achieving beneficial outcomes. Clin Appl Thromb Hemost, 22, 605–616.
Martinez, C., Katholing, A., Wallenhorst, C., & Freedman, S. B. (2016). Therapy persistence in newly diagnosed non-valvular atrial fibrillation treated with warfarin or NOAC. A cohort study. Thromb Haemost, 115, 31–39.
Gusmai Lde, F., Novato Tde, S., & Nogueira, Lde S. (2015). The influence of quality of life in treatment adherence of diabetic patients: a systematic review. Revista da Escola Enfermagem da USP, 49, 839–846.
Miller, C. S., Grandi, S. M., Shimony, A., Filion, K. B., & Eisenberg, M. J. (2012). Meta-analysis of efficacy and safety of new oral anticoagulants (dabigatran, rivaroxaban, apixaban) versus warfarin in patients with atrial fibrillation. The American Journal of Cardiology, 110, 453–460.
Patel, M. R., Mahaffey, K. W., Garg, J., Pan, G., Singer, D. E., Hacke, W., et al. (2011). Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. New England Journal of Medicine, 365, 883–891.
Camm, A. J., Amarenco, P., Haas, S., Hess, S., Kirchhof, P., Kuhls, S., et al. (2016). XANTUS: A real-world, prospective, observational study of patients treated with rivaroxaban for stroke prevention in atrial fibrillation. Europe Heart Journal, 37, 1145–1153.
Fox, K. A. A., Piccini, J. P., Wojdyla, D., Becker, R. C., Halperin, J. L., Nessel, C. C., et al. (2011). Prevention of stroke and systemic embolism with rivaroxaban compared with warfarin in patients with non-valvular atrial fibrillation and moderate renal impairment. Europe Heart Journal, 32, 2387–2394.
Sawicki, P. T. (1999). A structured teaching and self-management program for patients receiving oral anticoagulation: a randomized controlled trial. Working group for the Study of Patient Self-Management of Oral Anticoagulation. JAMA, 281, 145–150.
Sánchez González, R., Yanes Baonza, M., Cabrera Majada, A., Ferrer García-Borrás, J. M., Alvarez Nido, R., & Barrera, Linares E. (2004). Adaptación transcultural de un cuestionario para medir la calidad de vida de los pacientes con anticoagulación oral. Atención Primaria, 34, 353–359.
Gadisseur, A. P., Kaptein, A. A., Breukink-Engbers, W. G., de Mol, B. J., Prins, M. H., Hutten, B. A., et al. (2004). Patient self-management of oral anticoagulant care vs. management by specialized anticoagulation clinics: Positive effects on quality of life. Journal of Thrombosis and Haemostasis, 2, 584–591.
Siebenhofer, A., Hemkens, L. G., Rakovac, I., Spat, S., & Didjurgeit, U. (2012). Self-management of oral anticoagulation in elderly patients—effects on treatment-related quality of life. Thromb Res, 130, e60–e66.
Alegret, J. M., Viñolas, X., Arias, M. A., Martínez-Rubio, A., Rebollo, P., Ràfols, C., et al. (2014). New oral anticoagulants vs vitamin K antagonists: benefits for health-related quality of life in patients with atrial fibrillation. International Journal Medical Sciences, 11, 680–684.
Yanes Baonza, M., Cabrera Majada, A., Ferrer García-Borrás, J. M., & Sánchez, González R. (2005). Quality of life of patients treated with oral anticoagulants. Atencion Primaria, 36, 224–225.
De Schryver, E. L., van Gijn, J., Kappelle, L. J., Koudstaal, P. J., Algra, A., Dutch, T. I. A., et al. (2005). Non-adherence to aspirin or oral anticoagulants in secondary prevention after ischaemic stroke. Journal of Neurology, 252, 1316–1321.
Nelson, W. W., Song, X., Thomson, E., Smith, D. M., Coleman, C. I., Damaraju, C. V., et al. (2015). Medication persistence and discontinuation of rivaroxaban and dabigatran etexilate among patients with non-valvular atrial fibrilation. Current Medical Resarch and Opinion, 31, 1831–1840.
Crivera, C., Nelson, W. W., Bookhart, B., Martin, S., Germain, G., Laliberté, F., et al. (2015). Pharmacy quality alliance measure: adherence to non-warfarin oral anticoagulant medications. Current Medicine Resarch and Opinion, 31, 1889–1895.
Ynsaurriaga, F. A., Peinado, R. P., & Ormaetxe Merodio, J. M. (2014). Atrial fibrillation and quality of life related to disease and treatment: focus on anticoagulation. Future Cardiology, 10, 381–393.
Cromheecke, M. E., Levi, M., Colly, L. P., De Mol, B. J. M., Prins, M. H., Hutten, B. A., et al. (2000). Oral anticoagulation self-management and management by a specialist anticoagulation clinic: a randomised cross-over comparison. The Lancet, 356, 97–102.
Sawicki, P. T., Gläser, B., Kleespies, C., Stubbe, J., Schmitz, N., Kaiser, T., et al. (2003). Self-management of oral anticoagulation: long-term results. Journal of Internal Medicine, 254, 515–516.
Hasan, S. S., Teh, K. M., Ahmed, S. I., Chong, D. W., Ong, H. C., & Naina, B. (2015). Quality of life (QoL) and international normalized ratio (INR) control of patients attending anticoagulation clinics. Public Health, 129, 954–962.
Fareau, S., Baumstarck, K., Farcet, A., Molines, C., Auquier, P., & Retornaz, F. (2015). Quality of life of elderly people on oral anticoagulant for atrial fibrillation: VKA versus direct oral anticoagulants. Geriatrie et Psychologie Neuropsychiatrie du Vieillissement, 13, 45–54.
Freeman, J. V., Simon, D. N., Go, A. S., Spertus, J., Fonarow, G. C., Gersh, B. J., et al. (2015). Association between atrial fibrillation symptoms, quality of life, and patient outcomes: results from the outcomes registry for better informed treatment of atrial fibrillation (ORBIT-AF). Circulation Cardiovascular Quality and Outcomes, 8, 393–402.
de Almeida, G., Noblat Lde, A., Passos, L. C., & do Nascimento, H. F. (2011). Quality of life analysis of patients in chronic use of oral anticoagulant: an observational study. Health Quality Life Outcomes, 9, 91.
Acknowledgements
We would like to thank all the researchers of the CUMRIVAFA and the rest of the team of the SHE-LEHLA Compliance Study Group for their work. We thank to Bayer Hispania SL for their sponsorship in this study.
Funding
This study was funded by Bayer Healthcare (Grant 01-2014). Bayer gave a grant to the Association Medical Group Onuba, Huelva (Spain). This association was the promoter of the study.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest existed. The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Clinical Ethics Committee of Andalucía, Elda and Jordi Gol i Gurina Foundation.
Informed consent
Informed consent was obtained from all individual participants included in the study. File attached informed consent.
Rights and permissions
About this article
Cite this article
Márquez-Contreras, E., Martell-Claros, N., Gil-Guillén, V. et al. Quality of life with rivaroxaban in patients with non-valvular atrial fibrilation by therapeutic compliance. Qual Life Res 26, 647–654 (2017). https://doi.org/10.1007/s11136-016-1489-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-016-1489-x