Abstract
Purpose
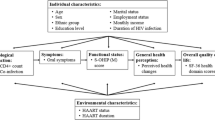
This study compared the Quality of Life (QOL) according to the presence of functional and psychosocial impact of oral disorders and evaluated the convergent validity between the dimensions of the WHOQOL and the OHIP-14 scores among people living with HIV.
Methods
This was a cross-sectional study with patients enrolled in reference centres of a midsize Brazilian city. Interviews were conducted when the participants arrived at the centres seeking services for medical appointments and collecting medicines. The OHIP-14 was used to evaluate the functional and psychosocial impact of oral disorders. QOL was assessed using the general issues and six domains of the WHOQOL-HIV BREF. The Chi square test, Mann–Whitney test, and Spearman correlation analysis were used for analysis.
Results
The sample comprised 422 people living with HIV/AIDS (response rate: 81.2 %). The prevalence of functional and psychosocial impact of oral disorders was 34.0 %. The prevalence of very poor/poor QOL and those who were very dissatisfied/dissatisfied with their health was higher among those with functional and psychosocial impact of oral disorders. There was a negative correlation between the scores on the domains of QOL and the severity of the impact of the oral disorders (r-value ranged from −0.107 to −0.30).
Conclusion
Individuals with functional and psychosocial impact of oral disorders were found to more frequently rate their QOL as poor/very poor, and were more often dissatisfied with health. The correlation between the scores of QOL and functional and psychosocial impact of oral disorders scores was weak, indicating that they represent different constructs. The measures of functional and psychosocial impact of oral disorders should be complemented by general measures of QOL.
Similar content being viewed by others
Reference
Giri, S., Neupane, M., Pant, S., Timalsina, U., Koirala, S., Timalsina, S., et al. (2013). Quality of life among people living with acquired immune deficiency syndrome receiving anti-retroviral therapy: a study from Nepal. HIV AIDS Research and Palliative Care, 5, 277–282.
UNAIDS (2013). Global report: UNAIDS report on the global AIDS epidemic. Switzerland
BRASIL. Ministério da Saúde. Boletim Epidemiológico 2013 http://www.aids.gov.br/pagina/aids-no-brasil
Porter, K., Babiker, A., Bhaskaran, K., Darbyshire, J., Pezzotti, P., Porter, K., et al. (2003). Determinants of survival following HIV-1 soroconversion after introduction of HAART. Lancet, 362(9392), 1267–1274.
Boyd, M. A. (2009). Improvements in antiretroviral therapy outcomes over calendar time. Current Opinion in HIV and AIDS, 4(3), 194–199.
Justice, A. C. (2010). HIV and aging: time for a new paradigm. Curr HIV/AIDS Rep, 7(2), 69–76.
Briongos Figuero, L. S., Bachiller Luque, P., Palacios Martín, T., González Sagrado, M., & Eiros Bouza, J. M. (2011). Assessment of factors influencing health-related quality of life in HIV-infected patients. HIV Medicine, 12(1), 22–30.
Lorentz, K., Cunningham, W. E., Spritzer, K. L., & Hays, R. D. (2006). Changes in symptoms and health-related quality of life in a nationally representative sample of adults in treatment for HIV. Quality of Life Research, 15(6), 951–958.
Rajagopalan, R., Laitinen, D., & Dietz, B. (2008). Impact of lipoatrophy on quality of life in HIV patients receiving anti-retroviral therapy. AIDS Care, 201(10), 1197–1201.
Wig, N., Lekshmi, R., Pal, H., Ahuja, V., Mittal, C. M., & Agarwal, S. K. (2006). The impact of HIV/AIDS on the quality of life: a cross sectional study in North India. Indian Journal of Medical Sciences, 60(1), 3–12.
Rueda, S., Raboud, J., Mustard, C., Bayoumi, A., Lavis, J. N., & Rourke, S. B. (2011). Employment status is associated with both physical and mental health quality of life in people living with HIV. AIDS Care, 23(4), 435–443.
Rajeev, K. H., Yuvaraj, B. Y., Gowda, M. R. N., & Ravikumar, S. M. (2012). Impact of HIV aids on quality of life of people living with HIV aids in Chitradurga District. Karnataba. Indian Journal of Public Health, 56(2), 116–121.
Rai, Y., Dutta, T., & Gulati, A. K. (2010). Quality of life of HIV-infected people across different stages of infection. Journal of Happiness Studies, 11, 61–69.
Weinfut, K. P., Willke, R. J., Glick, H. A., Freimuth, W. W., & Schulman, K. A. (2000). Relationship between CD4 count, viral burden, and quality of life over time in HIV-1 infected patients. Medical Care, 38(4), 404–410.
Tramarin, A., Parise, N., Campostrini, S., Yin, D. D., Postma, M. J., Lyu, R., et al. (2004). Association between diarrhea and quality of life in HIV-infected patients receiving highly active antiretroviral therapy. Quality of Life Research, 13(1), 243–250.
Silva, J., Bunn, K., Bertoni, R. F., Neves, O. A., & Traebert, J. (2013). Quality of life of people living with HIV. AIDS Care, 25(1), 71–76.
Pérez, I. R., Lima, A. O. L., Castillo, L. S., Baño, J. R., Ruz, M. A. L., & Jimenez, A. A. (2009). No differences in quality of life between men and women undergoing HIV antiretroviral treatment. Impact of demographic, clinical and psychosocial factors. AIDS Care, 21(8), 942–952.
Santos, E. C. M., Junior, I. F., & Lopes, F. (2007). Quality of life of people living with HIV AIDS in São Paulo, Brazil. Revista de Saúde Pública, 41, 64–71.
Coulter, I. D., Heslin, K. C., Marcus, M., Hays, R. D., Freed, J., Der-Martirosia, C., et al. (2002). Associations of self-reported oral health with physical and mental health in a nationally representative sample of HIV persons receiving medical care. Quality of Life Research, 11(1), 57–70.
Yengopal, V., & Naidoo, S. (2008). Do oral lesions associated with HIV affect quality of life? Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, 106(1), 66–73.
Liberali, S. A., Coates, E. A., Freeman, A. D., Logan, R. M., Jamieson, L., & Mejia, G. (2013). Oral conditions and their social impact among HIV dental patients, 18 years on. Australian Dental Journal, 58(1), 18–25.
Tomar, S. L., Pereyra, M., & Metsch, L. R. (2011). Oral health-related quality of life among low-income adults living with HIV. Journal of Public Health Dentistry, 71(3), 241–247.
Mulligan, R., Seirawan, H., Alves, M. E., Navazesh, M., Phelan, J. A., Greenspan, D., et al. (2008). Oral health-related quality of life among HIV-infected and at-risk women. Community Dentistry and Oral Epidemiology, 36(6), 549–557.
Jenganathan, S., Batterham, M., Begley, K., Purnomo, J., & Houtzager, L. (2011). Predictors of oral health quality of life in HIV-1 infected patients attending routine care in Australia. Journal of Public Health Dentistry, 71(3), 248–251.
Lawrence, H. P., Thomson, W. M., Broadbent, J. M., & Poulton, R. (2008). Oral health-related quality of life in a birth cohort of 32-year olds. Community Dentistry and Oral Epidemiology, 36(4), 305–316.
Sanders, A. E., Slade, G. D., Lim, S., & Reisine, S. T. (2009). Impact of oral disease on quality of life in the US and Australian populations. Community Dentistry and Oral Epidemiology, 37(2), 171–181.
Locker, D., & Allen, F. (2007). What do measures of oral health related quality of life measure? Community Dentistry and Oral Epidemiology, 35(6), 401–411.
Tsakos, G., Allen, F., Steele, J. G., & Locker, D. (2012). Interpreting oral health-related quality of life data. Community Dentistry and Oral Epidemiology, 40(3), 193–200.
Santos, J. D. P., Silveira, D. V., Oliveira, D. F., & Caiaffa, W. T. (2011). Instrumentos para avaliação do tabagismo: uma revisão sistemática. Ciência & Saúde Coletiva, 16(12), 4707–4720.
Lima, C. T., Freire, A. C., Silva, A. P., Teixeira, R. M., Ferrell, M., & Prince, M. (2005). Concurrent and construct validity of the AUDIT in an urban Brazilian sample. Alcohol and Alcoholism, 40(6), 584–589.
Matsudo, S., Araújo, T., Matsudo, V., Andrade, D., Andrade, E., Oliveira, L. C., et al. (2001). O questionário Internacional de Atividade Física: estudo de validade e reprodutibilidade. Revista Atividade Física e Saúde, 6(2), 5–18.
Who. Departamento de Saúde Mental e Dependência Química. WHOQOL-HIV bref. Versão em Português. 2002. Acesso em 16 jul 2014. Disponível em: http://www.ufrgs.br/psiquiatria/psiq/whoqol_hiv_03.pdf.
Zimpel, R. R., & Fleck, M. P. (2007). Quality of life in HIV-positive Brazilians: application and validation of the WHOQOL-HIV. Brazilian version. AIDS Care, 19(7), 923–930.
WHOQOL-HIV: Sintaxe. Available in: http://www.ufrgs.br/psiquiatria/psiq/whoqol_hiv_04.pdf. Accessed on 09 February 2014
Oliveira, B. H., & Nadanovsky, P. (2005). Psychometric properties of the Brazilian version of the Oral Health Impact Profile-short form. Community Dentistry and Oral Epidemiology, 33(4), 307–314.
Slade, G. D., Nuttall, N., Sanders, A. E., Steele, J. G., Allen, P. F., & Lahti, S. (2005). Impacts of oral disorders in the United Kingdom and Australia. British Dental Journal, 198(8), 489–493.
Huang, I. C., Wu, A. W., & Frangakis, C. (2006). Do the SF-36 and WHOQOL-bref measure the same constructs? Evidence from the Taiwan population. Quality of Life Research, 15(1), 15–24.
Dunbar, H. T., Mueller, C. W., Medina, C., & Wolf, T. (1998). Psychological and spiritual growth in women living with HIV. Social Work, 43(2), 144–154.
Miotto, M. H. M. B., Barcellos, L. A., & Velten, D. B. (2012). Avaliação do impacto na qualidade de vida causado por problemas bucais na população adulta e idosa em município da Região Sudeste. Ciência & Saúde Coletiva, 17(2), 397–406.
Silva, A. E., Demarco, F. F., & Feldens, C. A. (2013). Oral health-related quality of life and associated factors in Southern Brazilian elderly. Gerodontology,. doi:10.1111/ger.1205.
Gonzales-Sullcahuamán, J. A., Ferreira, F. M., de Menezes, J. V., Paiva, S. M., & Fraiz, F. C. (2013). Oral health-related quality of life among Brazilian dental students. Acta Odontol Latinoam, 26(2), 76–83.
Ulinski, K. G., do Nascimento, M. A., Lima, A. M., Benetti, A. R., Poli-Frederico, R. C., Fernandes, K. B., et al. (2013). Factors related to oral health-related quality of life of independent Brazilian elderly. International Journal of Dentistry, 2013, 705047. doi:10.1155/2013/705047.
Santos, M. S., Hugo, F. N., Leal, A. F., & Hilgert, J. B. (2013). Comparison of two assessment instruments of quality of life in older adults. Revista Brasileira de Epidemiologia, 16(2), 328–337.
Locker, D., & Quiñonez, C. (2011). To what extent do oral disorders compromise the quality of life? Community Dentistry and Oral Epidemiology, 39(1), 3–11.
Locker, D. (2008). Research on oral health and the quality of life-a critical overview. Community Dental Health, 25(3), 130–131.
Acknowledgments
To Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) for the financial support (reference 478253/2010-9).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Quadros Coelho, M., Cordeiro, J.M., Vargas, A.M.D. et al. Functional and psychosocial impact of oral disorders and quality of life of people living with HIV/AIDS. Qual Life Res 24, 503–511 (2015). https://doi.org/10.1007/s11136-014-0778-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-014-0778-5