Abstract
Purpose
Active Ageing (AA), as described by the WHO (Active Ageing: a policy framework. World Health Organisation, Geneva 5), is an important concept in gerontology. Since the AA-concept has not been examined in the context of residential long-term care facilities, our study addresses this gap by describing the determinants of AA within this setting.
Methods
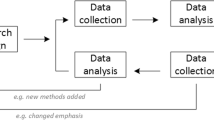
A qualitative study with semi-structured focus groups, followed by a thematic analysis, was conducted. Through purposive sampling, four focus groups of either residents of long-term care facilities (n = 8), children of residents (n = 8), community-dwelling older people (n = 8) and gerontologists (n = 6) were formed.
Results
The thematic analysis yielded nine determinants of AA. Seven correspond to those identified by the WHO: Culture, Behaviour, Psychological Factors, Physical Environment, Social Environment, Economic Characteristics and Health and Social Care. Two new determinants were identified: Meaningful Leisure and Participation. The determinant Participation is seen as crucial to AA in residential care.
Conclusion
This study points to a more extensive set of determinants of AA than those identified by the WHO (Active Ageing: a policy framework. World Health Organisation, Geneva 5). Staff of long-term care facilities can make use of these determinants to promote AA in their residents.
Similar content being viewed by others
Abbreviations
- AA:
-
Active Ageing
- WHO:
-
World Health Organisation
- QoL:
-
Quality of life
- RLTC:
-
Residential long-term care facilities
- R-RLTC:
-
Residents of residential long-term care facilities
- C-RLTC:
-
Children of residents of residential long-term care facilities
- CD:
-
Community-Dwelling older people
- EG:
-
Experts/Gerontologists
References
Commission of the European Communities. (1999). Towards a Europe for all ages. Promoting prosperity and intergenerational solidarity.
Walker, A. (2002). A strategy for active ageing. International Social Security Review, 55, 121–139.
World Health Organisation. (1998). Statement developed by WHO. Geneva: Quality of Life Working Group.
Bowling, A. (2009). Perceptions of active ageing in Britain: Divergences between minority ethnic and whole population samples. Age and Ageing, 38(6), 703–710.
World Health Organisation. (2002). Active ageing: A policy framework. Geneva: World Health Organisation.
Bowling, A. (2008). Enhancing later life: How older people perceive active ageing? Aging Ment Health, 12(3), 293–301.
World Health Organization. (2001). Active ageing: from evidence to action. Geneva: WHO.
World Health Organisation. (2001). Health and ageing. A discussion paper. Geneva: World Health Organisation.
O’Shea, E. (2006). Developing a healthy ageing policy for Ireland: The view from below. Health Policy, 76(1), 93–105.
Stenner, P., McFarquhar, T., & Bowling, A. (2011). Older people and ‘active ageing’: Subjective aspects of ageing actively. Journal of Health Psychology, 16(3), 467–477.
Edmondson, R., & Von Kondratowitz, H.-J. (2009). Valuing older people. A humanist approach to ageing. Bristol: The Policy Press.
Buys, L., Boulton-Lewis, G., Tedman-Jones, J., Edwards, H., Knox, M., & Bigby, C. (2008). Issues of active ageing: Perceptions of older people with lifelong intellectual disability. Australasian Journal on Ageing, 27(2), 67–71.
Cloos, P., Allen, C. F., Alvarado, B. E., Zunzunegui, M. V., Simeon, D. T., & Eldemire-Shearer, D. (2010). ‘Active ageing’: A qualitative study in six Carribean countries. Ageing and society, 30, 79–101.
Chong, A. M., Sink-Hung, N. G., Woo, J., & Kwan, A. Y. (2006). Positive Ageing: The views of middle-aged and older adults in Hong-Kong. Ageing and society, 26, 243–265.
Martinez-Maldonado, M. L., Correa-Munoz, E., & Mendoza-Nunez, V. M. (2007). Program of active aging in a rural Mexican community: A qualitative approach. BMC Public Health, 7, 276–285.
Michael, Y. L., Green, M. K., & Farquhar, S. A. (2006). Neighborhood design and active aging. Health Place, 12(4), 734–740.
Clarke, A., & Warren, L. (2007). Hopes, fears and expectations about the future; What do older people’s stories tell us about active ageing? Ageing and society, 27, 465–488.
Minichiello, V., Browne, J., & Kendig, H. (2000). Perceptions and consequences of ageism: Views of older people. Ageing and Society, 20, 253–278.
Soar, J., & Seo, Y. (2007). Health and aged care enabled by information technology. Annals of the New York Academy of Sciences, 1114, 154–161.
Vlaams Parlement (Flemish Parliament). (2009). Het ontwerp van woonzorgdecreet (The concept of the Decree on residential and home care). from http://www.vvsg.be/Welzijnsvoorzieningen/woonzorg/Documents/Woonzorgdecreet/Ontwerp%20van%20woonzorgdecreet.pdf.
Gorus, E., Van Puyvelde, K., Corremans, V., & Mets, T. (2011). The use of acetyl cholinesterase inhibitors and memantine in nursing home residents. Acta Clinica Belgica, 66(5), 361–366.
Wadensten, B., & Carlsson, M. (2003). Theory-driven guidelines for practical care of older people, based on the theory of gerotranscendence. Journal of Advanced Nursing, 41(5), 462–470.
McLafferty, I. (2004). Focus group interviews as a data collecting strategy. Journal of Advanced Nursing, 48(2), 187–194.
McEwan, M. J., Espie, C. A., Metcalfe, J., Brodie, M. J., & Wilson, M. T. (2004). Quality of life and psychosocial development in adolescents with epilepsy: A qualitative investigation using focus group methods. Seizure, 13(1), 15–31.
Holloway, I., & Wheeler, S. (2010). Qualitative research in nursing and health care (3rd ed.). West-Sussex: Wiley-Blackwell.
Newman, D. K. (2007). Northern hospitality: Creating a hospitality culture in a nursing home setting, by the staff of Northern Services Group, Inc. Nursing Homes, 56(4), 26–35.
McCabe, B. W., Hertzog, M., Grasser, C. M., & Walker, S. N. (2005). Practice of health-promoting behaviors by nursing home residents. Western Journal of Nursing Research, 27(8), 1000–1016. discussion 1017–1022.
Plouffe, L., & Kalache, A. (2010). Towards global age-friendly cities: Determinang urban features that promote active aging. Journal of Urban Health: Bulletin of the New York Academy of Medicine, 87(5), 733–739.
Adler, J. (2008). A home, not a hospital. Planning, 74(6), 24–25.
Federale Overheidsdienst Economie (Federal State Service Economy). (2009). Sectorstudie Rusthuizen (Sector study Insitutional Long Term Care Facilities). from http://statbel.fgov.be/nl/binaries/studie_rusthuissector_tcm325-96287.pdf.
Buckley, C., & McCarthy, G. (2009). An exploration of social connectedness as perceived by older adults in a long-term care setting in Ireland. Geriatric Nursing, 30(6), 390–396.
Nayak, R., Buys, L., & Lovie-Kitchin, J. (2006). Influencing factors in achieving active ageing. In Proceedings 6th IEEE international conference on data mining—workshops, pp. 858–862.
Isola, A., Backman, K., Voutilainen, P., & Rautsiala, T. (2008). Quality of institutional care of older people as evaluated by nursing staff. Journal of Clinical Nursing, 17(18), 2480–2489.
Mion, L., Odegard, P. S., Resnick, B., & Segal-Galan, F. (2006). Interdisciplinary care for older adults with complex needs: American Geriatrics Society position statement. Journal of the American Geriatrics Society, 54(5), 849–852.
Van’t Leven, N., & Jonsson, H. (2002). Doing and being in the atmosphere of the doing: Environmental influences on occupational performance in a nursing home. Scandinavian Journal of Occupational Therapy, 9, 148–155.
Blair, C. E. (1999). Effect of self-care ADLs on self-esteem of intact nursing home residents. Issues in Mental Health Nursing, 20(6), 559–570.
Kari, N., & Michels, P. (1991). The Lazarus Project: The politics of empowerment. American Journal of Occupational Therapy, 45(8), 719–725.
Lie, M., Baines, S., & Wheelock, J. (2009). Citizenship, volunteering and active ageing. Social Policy and Administration, 43(7), 702–718.
World Health Organisation. (2001). International classification of functioning, disability and health (ICF). Geneva: World Health Organisation.
Whiteneck, G. (2005). Conceptual models of disability: past, present, & future. In M. J. Field, A. M. Jette, & L. Martin (Eds.), Workshop on disability in America. Washington DC: National Academics Press.
Yi, Z., Yuzhi, L., & George, L. K. (2003). Gender differentials of the oldest old in China. Research on Aging, 25, 65–80.
Van Malderen, L., Mets, T., & Gorus, E. (2012). Interventions to enhance the quality of life of older people in residential long-term care: a systematic review. Ageing Research Reviews: Accepted for publication.
Whittemore, R., Chase, S. K., & Mandle, C. L. (2001). Validity in qualitative research. Qualitative Health Research, 11(4), 522–537.
Acknowledgments
We thank all the participants of the four focus groups, the nursing homes and the Flemish elderly council for the cooperation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Malderen, L., Mets, T., De Vriendt, P. et al. The Active Ageing–concept translated to the residential long-term care. Qual Life Res 22, 929–937 (2013). https://doi.org/10.1007/s11136-012-0216-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-012-0216-5