Abstract
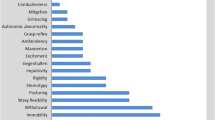
DSM-5 introduced a number of modifications to the catatonic syndrome, which is now closer to Kahlbaum’s original concept. The aim of the present study was to assess residents’ and qualified psychiatrists’ knowledge, experience and views about the treatment of catatonia in acute psychiatric care in Budapest, Hungary. Authors approached all psychiatric units that provide acute psychiatric care (N = 11) in Budapest and invited all psychiatrists and residents, who consented, to participate in the survey, completing a 13 items questionnaire. Ninety-eight fully qualified and trainee psychiatrists completed the questionnaire. Although 84.7% of the participants rated their knowledge of catatonia as moderate or significant, there were a number of obvious mistakes in their answers. Most catatonic signs and symptoms were not identified by almost 50% of the respondents and the frequency of catatonia was also underestimated. The views of the majority of the participants reflected the Kraepelinian concept, in which catatonia is primarily associated with schizophrenia. Although benzodiazepines are widely recommended as a first line treatment for catatonia, only 69.4% of participants chose them as a treatment option. In view of its clinical importance, catatonia deserves more attention in the education and training of medical students and psychiatric residents.


Similar content being viewed by others
References
Kahlbaum KL. Die Katatonie oder das Spannungsirresein. Berlin: Verlag August Hirschwald; 1874.
Dide L, Giraud P, Lafage R. Syndrome parkinsonien dans le demence precoce. Rev Neurol. 1921;28:692–4.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders, Fifth Edition (DSM-5). Arlington: American Psychiatric Publishing; 2013.
Ungvari GS, Gerevich J, Takács R, Gazdag G. Schizophrenia with prominent catatonic features: a selective review. Schizophr Res. 2018;200:77–84.
van der Heijden FM, Tuinier S, Arts NJ, Hoogendoorn ML, Kahn RS, Verhoeven WM. Catatonia: disappeared or under-diagnosed? Psychopathology. 2005;38:3–8.
Smith SL, Grelotti DJ, Fils-Aime R, Uwimana E, Ndikubwimana JS, Therosme T et al. Catatonia in resource-limited settings: a case series and treatment protocol. Gen Hosp Psychiatry. 2015;37(1):89–93.
Cooper JJ, Roiq LJ. Catatonia education: needs assessment and brief online intervention. Acad Psychiatry. 2017;41:360–3.
Bush G, Fink M, Petrides G, Dowling F, Francis A. Catatonia. I. Rating scale and standardized examination. Acta Psychiatr Scand. 1996;93:129–36.
Peralta V, Cuesta MJ. Motor features in psychotic disorders. II. Development of diagnostic criteria for catatonia. Schizophr Res. 2001;47:117–26.
Takács R, Asztalos M, Ungvari GS, Antosik-Wójcińska AZ, Gazdag G. The prevalence of catatonic syndrome in acute psychiatric wards. Psychiatria Polska. 2019;53:1251–60.
Takács R, Rihmer Z. Catatonia in affective disorders. Curr Psychiatr Rev. 2013;9:101–5.
Barnes MP, Saunders M, Walls TJ, Saunders I, Kirk CA. The syndrome of Karl Ludwig Kahlbaum. J Neurol Neurosurg Psychiatry. 1986;49:991–6.
Lee JW, Schwartz DL, Hallmayer J. Catatonia in a psychiatric intensive care facility: incidence and response to benzodiazepines. Ann Clin Psychiatry. 2000;12:89–96.
Ungvari GS, Caroff SN, Gerevich J. The catatonia conundrum: evidence of psychomotor phenomena as a symptom dimension in psychotic disorders. Schizophr Bull. 2010;36:231–8.
Caroff SN, Mann SC, Francis A, Fricchione GL. Catatonia. From psychopathology to neurobiology. Washington, DC: American Psychiatric Publishing Inc; 2004.
Sienaert P, Dhossche DM, Vancampfort D, De Hert M, Gazdag G. A clinical review of the treatment of catatonia. Front Psychiatry. 2014;5:181.
Asztalos M, Ungvari GS, Gazdag G. Changes in electroconvulsive therapy practice in the last 12 years in Hungary. J ECT. 2017;33:260–3.
Gazdag G, Asztalos M, Ungvari GS. Accessibility to electroconvulsive therapy in Hungary. Psychiatr Hung. 2018;33:266–9.
Gazdag G, Ungvari GS. Electroconvulsive therapy: 80 years old and still going strong. World J Psychiatry. 2019;9:1–6.
Fink M, Taylor MA. Catatonia: a Clinician’s guide to diagnosis and treatment. New York: Cambridge University Press; 2003.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Considerations
The study protocol was approved by the Internal Review Board of the Jahn Ferenc South Pest Hospital, Budapest, Hungary.
Declaration of Interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Takács, R., Ungvari, G.S., Antosik-Wójcińska, A.Z. et al. Hungarian Psychiatrists’ Recognition, Knowledge, and Treatment of Catatonia. Psychiatr Q 92, 41–47 (2021). https://doi.org/10.1007/s11126-020-09748-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11126-020-09748-z