Abstract
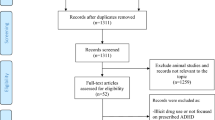
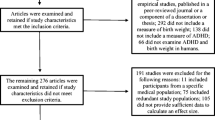
Previous studies have shown mixed results on the relationship between prenatal, birth, and postnatal (“pregnancy-related”) risk factors and attention-deficit/hyperactivity disorder (ADHD). We conducted meta-analyses to identify potentially modifiable pregnancy-related factors associated with ADHD. A comprehensive search of PubMed, Web of Science, and EMBASE in 2014, followed by an updated search in January 2021, identified 69 articles published in English on pregnancy-related risk factors and ADHD for inclusion. Risk factors were included in the meta-analysis if at least three effect sizes with clear pregnancy-related risk factor exposure were identified. Pooled effect sizes were calculated for ADHD overall, ADHD diagnosis, inattention, and hyperactivity/impulsivity. Odds ratios (OR) were calculated for dichotomous measures and correlation coefficients (CC) for continuous measures. Prenatal factors (pre-pregnancy weight, preeclampsia, pregnancy complications, elevated testosterone exposure), and postnatal factors (Apgar score, neonatal illness, no breastfeeding) were positively associated with ADHD overall; the findings for ADHD diagnosis were similar with the exception that there were too few effect sizes available to examine pre-pregnancy weight and lack of breastfeeding. Prenatal testosterone was significantly associated with inattention and hyperactivity/impulsivity. Effect sizes were generally small (range 1.1–1.6 ORs, -0.16–0.11 CCs). Risk factors occurring at the time of birth (perinatal asphyxia, labor complications, mode of delivery) were not significantly associated with ADHD. A better understanding of factors that are consistently associated with ADHD may inform future prevention strategies. The findings reported here suggest that prenatal and postnatal factors may serve as potential targets for preventing or mitigating the symptoms of ADHD.

Similar content being viewed by others
References
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (DSM-5). American Psychiatric Publishing. https://doi.org/10.1176/appi.books.9780890425596
Ananth, C. V., Berkowitz, G. S., Savitz, D. A., & Lapinski, R. H. (1999). Placental abruption and adverse perinatal outcomes. Journal of the American Medical Association, 282(17), 1646–1651. https://doi.org/10.1001/jama.282.17.1646
Ananth, C. V., Keyes, K. M., & Wapner, R. J. (2013). Pre-eclampsia rates in the United States, 1980–2010: Age-period-cohort analysis. British Medical Journal, 347, f6564. https://doi.org/10.1136/bmj.f6564
Ben Amor, L., Grizenko, N., Schwartz, G., Lageix, P., Baron, C., Ter-Stepanian, M., Zappitelli, M., Mbekou, V., & Joober, R. (2005). Perinatal complications in children with attention-deficit hyperactivity disorder and their unaffected siblings. Journal of Psychiatry & Neuroscience: JPN, 30, 120–126.
Berlin, J. A., Laird, N. M., Sacks, H. S., & Chalmers, T. C. (1989). A comparison of statistical methods for combining event rates from clinical trials. Statistics and Medicine, 8, 141–151. https://doi.org/10.1002/sim.4780080202
Bhatia, M. S., Nigam, V. R., Bohra, N., & Malik, S. C. (1991). Attention deficit disorder with hyperactivity among paediatric outpatients. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 32, 297–306. https://doi.org/10.1111/j.1469-7610.1991.tb00308.x
Blom, E. A., Jansen, P. W., Verhulst, F. C., Hofman, A., Raat, H., Jaddoe, V. W., Coolman, M., Steegers, E. A., & Tiemeier, H. (2010). Perinatal complications increase the risk of postpartum depression. The Generation R Study. BJOG: An International Journal of Obstetrics and Gynaecology, 117(11), 1390–1398. https://doi.org/10.1111/j.1471-0528.2010.02660.x
Böhm, S., Curran, E. A., Kenny, L. C., O’Keeffe, G. W., Murray, D., & Khashan, A. S. (2019). The effect of hypertensive disorders of pregnancy on the risk of ADHD in the offspring. Journal of Attention Disorders, 23, 692–701. https://doi.org/10.1177/1087054717690230
Bos-Veneman, N. G. P., Kuin, A., Minderaa, R. B., & Hoekstra, P. J. (2010). Role of perinatal adversities on tic severity and symptoms of attention deficit/hyperactivity disorder in children and adolescents with a tic disorder. Journal of Developmental and Behavioral Pediatrics, 31, 100–106. https://doi.org/10.1097/DBP.0b013e3181cc7cbc
Brion, M. J., Zeegers, M., Jaddoe, V., Verhulst, F., Tiemeier, H., Lawlor, D. A., & Smith, G. D. (2011). Intrauterine effects of maternal prepregnancy overweight on child cognition and behavior in 2 cohorts. Pediatrics, 127, e202-211. https://doi.org/10.1542/peds.2010-0651
Brundage, S. C., & Shearer, C. (2019). Plan and Provider Opportunities to Move Toward Integrated Family Health Care. March 21. United Hospital Fund, pp. 1–13. Available at: https://uhfnyc.org/media/filer_public/c1/0b/c10bfb65-dbf9-4d2c-9f97-ecd2a3928a9e/plan_and_provider_opportunities_uhf.pdf. Accessed 6 May 2021.
Centers for Disease Control and Prevention. (2020). Breastfeeding Report Card. https://www.cdc.gov/breastfeeding/pdf/2020-Breastfeeding-Report-Card-H.pdf. Accessed 6 May 2020.
Chandola, C. A., Robling, M. R., Peters, T. J., Melville-Thomas, G., & McGuffin, P. (1992). Pre- and perinatal factors and the risk of subsequent referral for hyperactivity. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 33, 1077–1090. https://doi.org/10.1111/j.1469-7610.1992.tb00926.x
Chen, H., Cohen, P., & Chen, S. (2010). How big is a big odds ratio? Interpreting the magnitudes of odds ratios in epidemiological studies. Communications in Statistics - Simulation and Computation, 39, 860–864. https://doi.org/10.1080/03610911003650383
Chen, M. H., Pan, T. L., Wang, P. W., Hsu, J. W., Huang, K. L., Su, T. P., Li, C. T., Lin, W. C., Tsai, S. J., Chen, T. J., & Bai, Y. M. (2019). Prenatal exposure to acetaminophen and the risk of attention-deficit/hyperactivity disorder: A nationwide study in Taiwan. The Journal of Clinical Psychiatry, 80(5). https://doi.org/10.4088/JCP.18m12612
Chiorean, A., Savoy, C., Beattie, K., El Helou, S., Silmi, M., & Van Lieshout, R. J. (2020). Childhood and adolescent mental health of NICU graduates: an observational study. Archives of disease in childhood, Published online 23 Jan 2020. https://doi.org/10.1136/archdischild-2019-318284
Claussen, A. H., Holbrook, J. R., Hutchins, H., Robinson, L. R., Bloomfield, J., Meng, L., Bitsko, R. H., O'Masta, B., Cerles, A., Maher, B., Rush, M., & Kaminski, J. W. (this issue). All in the family? A systematic review and meta-analysis of parenting and family environment as risk factors for attention-deficit/hyperactivity disorder (ADHD) in children. Prevention Science.
Claycomb, C. D., Ryan, J. J., Miller, L. J., & Schnakenberg-Ott, S. D. (2004). Relationships among attention deficit hyperactivity disorder, induced labor, and selected physiological and demographic variables. Journal of Clinical Psychology, 60, 689–693. https://doi.org/10.1002/jclp.10238
Clements, C. C., Castro, V. M., Blumenthal, S. R., Rosenfield, H. R., Murphy, S. N., Fava, M., Erb, J. L., Churchill, S. E., Kaimal, A. J., Doyle, A. E., Robinson, E. B., Smoller, J. W., Kohane, I. S., & Perlis, R. H. (2015). Prenatal antidepressant exposure is associated with risk for attention-deficit hyperactivity disorder but not autism spectrum disorder in a large health system. Molecular Psychiatry, 20, 727–734. https://doi.org/10.1038/mp.2014.90
Cohen, J. R. (1988). Statistical Power Analysis for the Behavioral Sciences. Routledge.
Curran, E. A., Khashan, A. S., Dalman, C., Kenny, L. C., Cryan, J. F., Dinan, T. G., & Kearney, P. M. (2016). Obstetric mode of delivery and attention-deficit/hyperactivity disorder: A sibling-matched study. International Journal of Epidemiology, 45, 532–542. https://doi.org/10.1093/ije/dyw001
D’Souza, S., Waldie, K. E., Peterson, E. R., Underwood, L., & Morton, S. M. B. (2019). Antenatal and postnatal determinants of behavioural difficulties in early childhood: Evidence from Growing Up in New Zealand. Child Psychiatry and Human Development, 50, 45–60. https://doi.org/10.1007/s10578-018-0816-6
Dachew, B. A., Scott, J. G., Mamun, A., & Alati, R. (2019). Pre-eclampsia and the risk of attention-deficit/hyperactivity disorder in offspring: Findings from the ALSPAC birth cohort study. Psychiatry Research, 272, 392–397. https://doi.org/10.1016/j.psychres.2018.12.123
Danielson, M. L., Bitsko, R. H., Ghandour, R. M., Holbrook, J. R., Kogan, M. D., & Blumberg, S. J. (2018). Prevalence of parent-reported ADHD diagnosis and associated treatment among U.S. children and adolescents, 2016. Journal of Clinical Child & Adolescent Psychology, 47(2), 199–212. https://doi.org/10.1080/15374416.2017.1417860
de Bruin, E., Verheij, F., Wiegman, T., & Ferdinand, R. (2006). Differences in finger length ratio between males with autism, pervasive developmental disorder-not otherwise specified, ADHD, and anxiety disorders. Developmental Medicine and Child Neurology, 48, 962–965. https://doi.org/10.1017/S0012162206002118
Dean, R. S., & Davis, A. S. (2007). Relative risk of perinatal complications in common childhood disorders. School Psychology Quarterly, 22, 13–25. https://doi.org/10.1037/1045-3830.22.1.13
DerSimonian, R., & Laird, N. (1986). Meta-analysis in clinical trials. Controlled Clinical Trials, 7, 177–188. https://doi.org/10.1016/0197-2456(86)90046-2
Dias, C. C., & Figueiredo, B. (2015). Breastfeeding and depression: A systematic review of the literature. Journal of Affective Disorders, 171, 142–154. https://doi.org/10.1016/j.jad.2014.09.022
Dimitrov, L. V., Kaminski, J. W., Holbrook, J. R., Bitsko, R. H., Yeh, M., O'Masta, B., Maher, B., Cerles, A., & Rush, M. (under review in this issue). A systematic review and meta-analysis of chemical exposures and attention-deficit, hyperactivity disorder. Prevention Science. Ehrenstein, V., Pedersen, L., Grijota, M., Nielsen, G. L., Rothman, K. J., & Sorensen, H. T. (2009). Association of Apgar score at five minutes with long-term neurologic disability and cognitive function in a prevalence study of Danish conscripts. BMC Pregnancy and Childbirth, 9,14. https://doi.org/10.1186/1471-2393-9-14
Ehrenstein, V., Pedersen, L., Grijota, M., Nielsen, G. L., Rothman, K. J., & Sorensen, H. T. (2009). Association of Apgar score at five minutes with long-term neurologic disability and cognitive function in a prevalence study of Danish conscripts. BMC Pregnancy and Childbirth, 9, 14. https://doi.org/10.1186/1471-2393-9-14.
Erskine, H. E., Norman, R. E., Ferrari, A. J., Chan, G. C., Copeland, W. E., Whiteford, H. A., & Scott, J. G. (2016). Long-term outcomes of attention-deficit/hyperactivity disorder and conduct disorder: A systematic review and meta-analysis. Journal of the American Academy of Child and Adolescent Psychiatry, 55, 841–850. https://doi.org/10.1016/j.jaac.2016.06.016
Faraone, S. V., Banaschewski, T., Coghill, D., Zheng, Y., Biederman, J., Bellgrove, M. A., Newcorn, J. H., Gignac, M., Al Saud, N. M., Manor, I., Rohde, L. A., Yang, L., Cortese, S., Almagor, D., Stein, M., A., Albatti, T. H., Aljoudi, H. F., Alqahtani, M. M. J., Asherson, P., & Wang, Y. (2021). The World Federation of ADHD International Consensus Statement: 208 evidence-based conclusions about the disorder. Neuroscience & Biobehavioral Reviews. Online ahead of print 4 Feb 2021. https://doi.org/10.1016/j.neubiorev.2021.01.022
Fianu, S., & Joelsson, I. (1979). Minimal brain dysfunction in children born in breech presentation. Acta Obstetricia Et Gynecologica Scandinavica, 58, 295–299. https://doi.org/10.3109/00016347909154052
Fink, B., Manning, J., Williams, J., & Podmore-Nappin, C. (2007). The 2nd to 4th digit ratio and developmental psychopathology in school-aged children. Personality and Individual Differences, 42, 369–379. https://doi.org/10.1016/j.paid.2006.07.018
Froehlich, T. E., Lanphear, B. P., Auinger, P., Hornung, R., Epstein, J. N., Braun, J., & Kahn, R. S. (2009). Association of tobacco and lead exposures with attention-deficit/hyperactivity disorder. Pediatrics, 124, e1054-1063. https://doi.org/10.1542/peds.2009-0738
Froehlich, T. E., Anixt, J. S., Loe, I. M., Chirdkiatgumchai, V., Kuan, L., & Gilman, R. C. (2011). Update on environmental risk factors for attention-deficit/hyperactivity disorder. Current Psychiatry Reports, 13, 333–344. https://doi.org/10.1007/s11920-011-0221-3
Getahun, D., Rhoads, G. G., Demissie, K., Lu, S. E., Quinn, V. P., Fassett, M. J., Wing, D. A., & Jacobsen, S. J. (2013). In utero exposure to ischemic-hypoxic conditions and attention-deficit/hyperactivity disorder. Pediatrics, 131, e53-61. https://doi.org/10.1542/peds.2012-1298
Goldenberg, R. L., Culhane, J. F., Iams, J. D., & Romero, R. (2008). Epidemiology and causes of preterm birth. Lancet, 371, 75–84. https://doi.org/10.1016/S0140-6736(08)60074-4
Guhn, M., Emerson, S. D., Mahdaviani, D., & Gadermann, A. M. (2020). Associations of birth factors and socio-economic status with indicators of early emotional development and mental health in childhood: A population-based linkage study. Child Psychiatry and Human Development, 51, 80–93. https://doi.org/10.1007/s10578-019-00912-6
Gurevitz, M., Geva, R., Varon, M., & Leitner, Y. (2014). Early Markers in Infants and Toddlers for Development of ADHD. Journal of Attention Disorders, 18, 14–22. https://doi.org/10.1177/1087054712447858
Gustafsson, P., & Källén, K. (2011). Perinatal, maternal, and fetal characteristics of children diagnosed with attention-deficit-hyperactivity disorder: results from a population-based study utilizing the Swedish Medical Birth Register. Developmental Medicine and Child Neurology, 53(3), 263–268. https://doi.org/10.1111/j.1469-8749.2010.03820.x
Gustavson, K., Ask, H., Ystrom, E., Stoltenberg, C., Lipkin, W. I., Surén, P., Håberg, S. E., Magnus, P., Knudsen, G. P., Eilertsen, E., Bresnahan, M., Aase, H., Mjaaland, S., Susser, E. S., Hornig, M., & Reichborn-Kjennerud, T. (2019). Maternal fever during pregnancy and offspring attention deficit hyperactivity disorder. Scientific Reports, 9, 9519. https://doi.org/10.1038/s41598-019-45920-7
Han, J. Y., Kwon, H. J., Ha, M., Paik, K. C., Lim, M. H., Gyu Lee, S., Yoo, S. J., & Kim, E. J. (2015). The effects of prenatal exposure to alcohol and environmental tobacco smoke on risk for ADHD: A large population-based study. Psychiatry Research, 225, 164–168. https://doi.org/10.1016/j.psychres.2014.11.009
Hanć, T., Szwed, A., Slopien, A., Wolanczyk, T., Dmitrzak-Weglarz, M., & Ratajczak, J. (2018). Perinatal risk factors and ADHD in children and adolescents: a hierarchical structure of disorder predictors. Journal of Attention Disorders, 22, 855–863. https://doi.org/10.1177/1087054716643389
Hayatbakhsh, M. R., O’Callaghan, M. J., Bor, W., Williams, G. M., & Najman, J. M. (2012). Association of breastfeeding and adolescents’ psychopathology: A large prospective study. Breastfeeding Medicine, 7, 480–486. https://doi.org/10.1089/bfm.2011.0136
Hedges, L. V., & Olkin, I. (1985). Statistical methods for meta-analysis. Academic Press.
Hoffman, K., Webster, T. F., Weisskopf, M. G., Weinberg, J., & Vieira, V. M. (2010). Exposure to polyfluoroalkyl chemicals and attention deficit/hyperactivity disorder in U.S. children 12–15 years of age. Environmental Health Perspectives, 118(12), 1762–1767. https://doi.org/10.1289/ehp.1001898
Ilekis, J. V., Reddy, U. M., & Roberts, J. M. (2007). Preeclampsia–a pressing problem: An executive summary of a National Institute of Child Health and Human Development workshop. Reproductive Sciences, 14, 508–523. https://doi.org/10.1177/1933719107306232
Instanes, J. T., Halmoy, A., Engeland, A., Haavik, J., Furu, K., & Klungsoyr, K. (2017). Attention-deficit/hyperactivity disorder in offspring of mothers with inflammatory and immune system diseases. Biological Psychiatry, 81, 452–459. https://doi.org/10.1016/j.biopsych.2015.11.024
Ji, Y., Hong, X., Wang, G., Chatterjee, N., Riley, A. W., Lee, L. C., Surkan, P. J., Bartell, T. R., Zuckerman, B., & Wang, X. (2018). A prospective birth cohort study on early childhood lead levels and attention deficit hyperactivity disorder: New insight on sex differences. The Journal of Pediatrics, 199, 124-131.e8. https://doi.org/10.1016/j.jpeds.2018.03.076
Jin, W., Du, Y., Zhong, X., & David, C. (2014). Prevalence and contributing factors to attention deficit hyperactivity disorder: A study of five- to fifteen-year-old children in Zhabei District. Shanghai. Asia- Pacific Psychiatry, 6, 397–404. https://doi.org/10.1111/appy.12114
Jo, H., Schieve, L. A., Sharma, A. J., Hinkle, S. N., Li, R., & Lind, J. N. (2015). Maternal prepregnancy body mass index and child psychosocial development at 6 years of age. Pediatrics, 135, e1198–e1209. https://doi.org/10.1542/peds.2014-3058
Joelsson, P., Chudal, R., Talati, A., Suominen, A., Brown, A. S., & Sourander, A. (2016). Prenatal smoking exposure and neuropsychiatric comorbidity of ADHD: A finnish nationwide population-based cohort study. BMC Psychiatry, 16, 306. https://doi.org/10.1186/s12888-016-1007-2
Julvez, J., Ribas-Fito, N., Forns, M., Garcia-Esteban, R., Torrent, M., & Sunyer, J. (2007). Attention behaviour and hyperactivity at age 4 and duration of breast-feeding. Acta Paediatrica, 96, 842–847. https://doi.org/10.1111/j.1651-2227.2007.00273.x
Kadziela-Olech, H., & Piotrowska-Jastrzebska, J. (2005). The duration of breastfeeding and attention deficit hyperactivity disorder. Roczniki Akademii Medycznej w Białymstoku, 1995, 302–306. https://doi.org/10.1080/24694193.2020.1797236
Källén, A. J., Finnstrom, O. O., Lindam, A. P., Nilsson, E. M., Nygren, K. G., & Otterblad Olausson, P. M. (2011). Is there an increased risk for drug treated attention deficit/hyperactivity disorder in children born after in vitro fertilization? European Journal of Pediatrics Neurol, 15, 247–253. https://doi.org/10.1016/j.ejpn.2010.12.004
Kim, H. W., Cho, S. C., Kim, B. N., Kim, J. W., Shin, M. S., & Kim, Y. (2009). Perinatal and familial risk factors are associated with full syndrome and subthreshold attention-deficit hyperactivity disorder in a Korean community sample. Psychiatry Investigation, 6(4), 278–285. https://doi.org/10.4306/pi.2009.6.4.278
Korkman, M., Hilakivi-Clarke, L. A., Autti-Rämö, I., Fellman, V., & Granström, M. L. (1994). Cognitive impairments at two years of age after prenatal alcohol exposure or perinatal asphyxia. Neuropediatrics, 25, 101–105. https://doi.org/10.1055/s-2008-1071594
Kosidou, K., Dalman, C., Widman, L., Arver, S., Lee, B. K., Magnusson, C., & Gardner, R. M. (2017). Maternal polycystic ovary syndrome and risk for attention-deficit/hyperactivity disorder in the offspring. Biological Psychiatry, 82, 651–659. https://doi.org/10.1016/j.biopsych.2016.09.022
Lathi, R. B., Dahan, M. H., Reynolds-May, M. F., Milki, A. A., Behr, B., & Westphal, L. M. (2014). The role of serum testosterone in early pregnancy outcome: A comparison in women with and without polycystic ovary syndrome. Journal of Obstetrics and Gynaecology Canada, 36, 811–816. https://doi.org/10.1016/S1701-2163(15)30483-7
Leinonen, E., Gissler, M., Haataja, L., Rahkonen, P., Andersson, S., Metsaranta, M., & Rahkonen, L. (2018). Low Apgar scores at both one and five minutes are associated with long-term neurological morbidity. Acta Paediatrica, 107, 942–951. https://doi.org/10.1111/apa.14234
Li, F., Wu, T., Lei, X., Zhang, H., Mao, M., & Zhang, J. (2013). The apgar score and infant mortality. PLoS One, 8, e69072. https://doi.org/10.1371/journal.pone.0069072
Li, J., Olsen, J., Vestergaard, M., & Obel, C. (2011). Low Apgar scores and risk of childhood attention deficit hyperactivity disorder. The Journal of Pediatrics, 158, 775–779. https://doi.org/10.1016/j.jpeds.2010.10.041
Lin, Q., Hou, X. Y., Yin, X. N., Wen, G. M., Sun, D., Xian, D. X., Fan, L., Jiang, H., Jing, J., Jin, Y., Wu, C., & Chen, W. (2017). Prenatal exposure to environmental tobacco smoke and hyperactivity behavior in chinese young children. International Journal of Environmental Research and Public Health, 14(10). https://doi.org/10.3390/ijerph14101132
Linnet, K. M., Obel, C., Bonde, E., Hove Thomsen, P., Secher, N. J., Wisborg, K., & Brink Henriksen, T. (2006). Cigarette smoking during pregnancy and hyperactive-distractible preschooler’s: A follow-up study. Acta Paediatrica, 95, 694–700. https://doi.org/10.1080/08035250500459709
Liu, J., Portnoy, J., & Raine, A. (2012). Association between a marker for prenatal testosterone exposure and externalizing behavior problems in children. Development and Psychopathology, 24, 771–782. https://doi.org/10.1017/S0954579412000363
Lumley. (2018). Package ‘rmeta.’ Version 3.0. https://cran.r-project.org/web/packages/rmeta/rmeta.pdf. Accessed 13 Mar 2019.
Lutchmaya, S., Baron-Cohen, S., Raggatt, P., Knickmeyer, R., & Manning, J. T. (2004). 2nd to 4th digit ratios, fetal testosterone and estradiol. Early Human Development, 77, 23–28. https://doi.org/10.1016/j.earlhumdev.2003.12.002
Maher, B., Kaminski, J., O'Masta, B., Cerles, A., Holbrook, J. R., Mahmooth, Z., & Rush, M. (under review in this issue). A systematic meta-analysis of the relationship between exposure to parental substance use and attention-deficit/hyperactivity disorder. Prevention Science.
Maher, G. M., O’Keeffe, G. W., O’Keeffe, L. M., Matvienko-Sikar, K., Dalman, C., Kearney, P. M., McCarthy, F. P., & Khashan, A. S. (2020). The association between preeclampsia and childhood development and behavioural outcomes. Maternal and Child Health Journal, 24, 727–738. https://doi.org/10.1007/s10995-020-02921-7
Maia, C., Brandao, R., Roncalli, A., & Maranhao, H. (2011). Length of stay in a neonatal intensive care unit and its association with low rates of exclusive breastfeeding in very low birth weight infants. The Journal of Maternal-Fetal & Neonatal Medicine, 24, 774–777. https://doi.org/10.3109/14767058.2010.520046
Mann, J. R., & McDermott, S. (2011). Are maternal genitourinary infection and pre-eclampsia associated with ADHD in school-aged children? Journal of Attention Disorders, 15, 667–673. https://doi.org/10.1177/1087054710370566
Marques, A. H., Bjorke-Monsen, A. L., Teixeira, A. L., & Silverman, M. N. (2015). Maternal stress, nutrition and physical activity: Impact on immune function, CNS development and psychopathology. Brain Research, 1617, 28–46. https://doi.org/10.1016/j.brainres.2014.10.051
Martel, M. (2009). Conscientiousness as a mediator of the association between masculinized finger-length ratios and attention-deficit/hyperactivity disorder (ADHD). Journal of Child Psychology and Psychiatry, and Allied Disciplines, 50, 790–798. https://doi.org/10.1111/j.1469-7610.2009.02065.x
Martel, M., Gobrogge, K., Breedlove, S., & Nigg, J. (2008). Masculinized finger-length ratios of boys, but not girls, are associated with attention-deficit/hyperactivity disorder. Behavioral Neuroscience, 122, 273–281. https://doi.org/10.1037/0735-7044.122.2.273
McFadden, D., Westhafer, J., Pasanen, E., Carlson, C., & Tucker, D. (2005). Physiological evidence of hypermasculinization in boys with the inattentive type of attention-deficit/hyperactivity disorder (ADHD). Clinical Neuroscience Research, 5, 233–245. https://doi.org/10.1016/j.cnr.2005.09.004
McIntosh, D. E., Mulkins, R. S., & Dean, R. S. (1995). Utilization of maternal perinatal risk indicators in the differential diagnosis of ADHD and UADD children. The International Journal of Neuroscience, 81, 35–46. https://doi.org/10.3109/00207459509015297
Melchior, M., Hersi, R., van der Waerden, J., Larroque, B., Saurel-Cubizolles, M. J., Chollet, A., Galéra, C., & the EDEN Mother-Child Cohort Study Group. (2015). Maternal tobacco smoking in pregnancy and children’s socio-emotional development at age 5: The EDEN mother-child birth cohort study. European Psychiatry, 30, 562–568. https://doi.org/10.1016/j.eurpsy.2015.03.005
Milberger, S., Biederman, J., Faraone, S. V., Guite, J., & Tsuang, M. T. (1997). Pregnancy, delivery and infancy complications and attention deficit hyperactivity disorder: issues of gene-environment interaction. Biological psychiatry, 41, 65–75. https://doi.org/10.1016/0006-3223(95)00653-2
Mimouni-Bloch, A., Kachevanskaya, A., Mimouni, F. B., Shuper, A., Raveh, E., & Linder, N. (2013). Breastfeeding may protect from developing attention-deficit/hyperactivity disorder. Breastfeeding Medicine, 8, 363–367. https://doi.org/10.1089/bfm.2012.0145
Mina, T. H., Denison, F. C., Forbes, S., Stirrat, L. I., Norman, J. E., & Reynolds, R. M. (2015). Associations of mood symptoms with ante- and postnatal weight change in obese pregnancy are not mediated by cortisol. Psychological Medicine, 45, 3133–3146. https://doi.org/10.1017/S0033291715001087
Motlagh, M. G., Katsovich, L., Thompson, N., Lin, H., Kim, Y. S., Scahill, L., et al. (2010). Severe psychosocial stress and heavy cigarette smoking during pregnancy An examination of the pre- and perinatal risk factors associated with ADHD and Tourette syndrome. European Child & Adolescent Psychiatry, 19, 755–764. https://doi.org/10.1007/s00787-010-0115-7
Murray, E., Pearson, R., Fernandes, M., Santos, I. S., Barros, F. C., Victora, C. G., Stein, A., & Matijasevich, A. (2016). Are fetal growth impairment and preterm birth causally related to child attention problems and ADHD? Evidence from a comparison between high-income and middle-income cohorts. Journal of Epidemiology and Community Health, 70, 704–709. https://doi.org/10.1136/jech-2015-206222
Nielsen, T. C., Nassar, N., Shand, A. W., Jones, H., Guastella, A. J., Dale, R. C., & Lain, S. J. (2021). Association of maternal autoimmune disease with attention-deficit/hyperactivity disorder in children. JAMA Pediatrics, 175, e205487. https://doi.org/10.1001/jamapediatrics.2020.5487
Padmanabhan, V., Manikkam, M., Recabarren, S., & Foster, D. (2006). Prenatal testosterone excess programs reproductive and metabolic dysfunction in the female. Molecular and Cellular Endocrinology, 246, 165–174. https://doi.org/10.1016/j.mce.2005.11.016
Park, S., Cho, S. C., Kim, J. W., Shin, M. S., Yoo, H. J., Oh, S. M., Han, D. H., Cheong, J. H., & Kim, B. N. (2014a). Differential perinatal risk factors in children with attention-deficit/hyperactivity disorder by subtype. Psychiatry Research, 219, 609–616. https://doi.org/10.1016/j.psychres.2014.05.036
Park, S., Kim, B. N., Kim, J. W., Shin, M. S., Yoo, H. J., & Cho, S. C. (2014b). Protective effect of breastfeeding with regard to children’s behavioral and cognitive problems. Nutrition Journal, 13, 111. https://doi.org/10.1186/1475-2891-13-111
Pineda, D. A., Palacio, L. G., Puerta, I. C., Merchán, V., Arango, C. P., Galvis, A. Y., Gómez, M., Aguirre, D. C., Lopera, F., & Arcos-Burgos, M. (2007). Environmental influences that affect attention deficit/hyperactivity disorder: Study of a genetic isolate. European Child & Adolescent Psychiatry, 16, 337–346. https://doi.org/10.1007/s00787-007-0605-4
Pires, T. D. O., da Silva, C. M. F. P., & de Assis, S. G. (2013). Association between family environment and attention deficit hyperactivity disorder in children–mothers’ and teachers’ views. BMC psychiatry, 13(1), 1–9. https://doi.org/10.1186/1471-244X-13-215
Pohlabeln, H., Rach, S., De Henauw, S., Eiben, G., Gwozdz, W., Hadjigeorgiou, C., Molnár, D., Moreno, L. A., Russo, P., Veidebaum, T., & Pigeot, I. (2017). Further evidence for the role of pregnancy-induced hypertension and other early life influences in the development of ADHD: Results from the IDEFICS study. European Child & Adolescent Psychiatry, 26, 957–967. https://doi.org/10.1007/s00787-017-0966-2
Pringsheim, T., Sandor, P., Lang, A., Shah, P., & O’Connor, P. (2009). Prenatal and perinatal morbidity in children with Tourette syndrome and attention-deficit hyperactivity disorder. Journal of Developmental and Behavioral Pediatrics, 30, 115–121. https://doi.org/10.1097/DBP.0b013e31819e6a33
Ramachenderan, J., Bradford, J., & McLean, M. (2008). Maternal obesity and pregnancy complications: A review. The Australia and New Zealand Journal of Obstetrics and Gynaecology, 48, 228–235. https://doi.org/10.1111/j.1479-828X.2008.00860.x
Rice, D., & Barone, S., Jr. (2000). Critical periods of vulnerability for the developing nervous system: Evidence from humans and animal models. Environmental Health Perspectives, 108, 511–533. https://doi.org/10.1289/ehp.00108s3511
Rivera, H. M., Christiansen, K. J., & Sullivan, E. L. (2015). The role of maternal obesity in the risk of neuropsychiatric disorders. Frontiers in Neuroscience, 9, 194. https://doi.org/10.3389/fnins.2015.00194
Roberts, B., & Martel, M. (2013). Prenatal testosterone and preschool Disruptive Behavior Disorders. Personality and Individual Differences, 55(8), 962–966. https://doi.org/10.1016/j.paid.2013.08.002
Robinson, L. R., Bitsko, R. H., O'Masta, B., Holbrook, J. R., Ko, J., Maher, B., Cerles, A., Saadeh, K., MacMillan, L., Mahmooth, Z., Bloomfield, J., Rush, M., & Kaminski, J. (this issue). A Systematic review and meta-analysis of parental depression, antidepressant usage, antisocial personality disorder, and stress and anxiety as risk factors for attention-deficit/hyperactivity disorder (ADHD) among children. Prevention Science.
Rodriguez, A. (2010). Maternal pre-pregnancy obesity and risk for inattention and negative emotionality in children. Journal of Child Psychology and Psychiatry, 51(2), 134–143. https://doi.org/10.1111/j.1469-7610.2009.02133.x
Rodriguez, A., Miettunen, J., Henriksen, T. B., Olsen, J., Obel, C., Taanila, A., Ebeling, H., Linnet, K. M., Moilanen, I., & Järvelin, M. R. (2008). Maternal adiposity prior to pregnancy is associated with ADHD symptoms in offspring: evidence from three prospective pregnancy cohorts. International Journal of Obesity (2005), 32(3), 550–557. https://doi.org/10.1038/sj.ijo.0803741
Russell, G., Rodgers, L. R., Ukoumunne, O. C., & Ford, T. (2014). Prevalence of parent-reported ASD and ADHD in the UK: Findings from the Millennium Cohort Study. Journal of Autism and Developmental Disorders, 44, 31–40. https://doi.org/10.1007/s10803-013-1849-0
Sacker, A., Quigley, M. A., & Kelly, Y. J. (2006). Breastfeeding and developmental delay: Findings from the Millennium Cohort Study. Pediatrics, 118, e682–e689. https://doi.org/10.1542/peds.2005-3141
Sanchez, C. E., Barry, C., Sabhlok, A., Russell, K., Majors, A., Kollins, S. H., & Fuemmeler, B. F. (2018). Maternal pre-pregnancy obesity and child neurodevelopmental outcomes: a meta-analysis. Obesity Reviews, 19(4), 464–484. https://doi.org/10.1111/obr.12643
Say, G. N., Karabekiroğlu, K., Babadağı, Z., & Yüce, M. (2016). Maternal stress and perinatal features in autism and attention deficit/hyperactivity disorder. Pediatrics International, 58, 265–269. https://doi.org/10.1111/ped.12822
Schoenfelder, E. N., & Kollins, S. H. (2016). Topical Review: ADHD and Health-Risk Behaviors: Toward Prevention and Health Promotion. Journal of Pediatric Psychology, 41, 735–740. https://doi.org/10.1093/jpepsy/jsv162
Sciberras, E., Mulraney, M., Silva, D., & Coghill, D. (2017). Prenatal Risk Factors and the Etiology of ADHD-Review of Existing Evidence. Current Psychiatry Reports, 19, 1. https://doi.org/10.1007/s11920-017-0753-2
Sciberras, E., Ukoumunne, O. C., & Efron, D. (2011). Predictors of parent-reported attention-deficit/hyperactivity disorder in children aged 6–7 years: A national longitudinal study. Journal of Abnormal Child Psychology, 39, 1025–1034. https://doi.org/10.1007/s10802-011-9504-8
Shih, P., Huang, C. C., Pan, S. C., Chiang, T. L., & Guo, Y. L. (2020). Hyperactivity disorder in children related to traffic-based air pollution during pregnancy. Environmental Research, 188, 109588. https://doi.org/10.1016/j.envres.2020.109588
Silva, D., Colvin, L., Hagemann, E., & Bower, C. (2014). Environmental risk factors by gender associated with attention-deficit/hyperactivity disorder. Pediatrics, 133, e14-22. https://doi.org/10.1542/peds.2013-1434
So, M., Dziuban, E. J., Pedati, C., Holbrook, J. R., Claussen, A. H., O'Masta, B., Maher, B., Cerles, A., Mahmooth, Z., MacMillan, L., Kaminski, J. W., & Rush, M. (under review in this issue). Attention-deficit/hyperactivity disorder and childhood physical health: a systematic review and meta-analysis. Prevention Science.
Smith, T. F., Schmidt-Kastner, R., McGeary, J. E., Kaczorowski, J. A., & Knopik, V. S. (2016). Pre- and perinatal ischemia-hypoxia, the ischemia-hypoxia response pathway, and ADHD risk. Behavior Genetics, 46, 467–477. https://doi.org/10.1007/s10519-016-9784-4
St. Sauver, J. L., Barbaresi, W. J., Katusic, S. K., Colligan, R. C., Weaver, A. L., & Jacobsen, S. J. (2004). Early life risk factors for attention-deficit/hyperactivity disorder: A population-based cohort study. Mayo Clinic Proceedings, 79, 1124–1131. https://doi.org/10.4065/79.9.1124
Stadler, D. D., Musser, E. D., Holton, K. F., Shannon, J., & Nigg, J. T. (2016). Recalled initiation and duration of maternal breastfeeding among children with and without ADHD in a well characterized case-control sample. Journal of Abnormal Child Psychology, 44, 347–355. https://doi.org/10.1007/s10802-015-9987-9
Stevenson, J. C., Everson, P. M., Williams, D. C., Hipskind, G., Grimes, M., & Mahoney, E. R. (2007). Attention deficit/hyperactivity disorder (ADHD) symptoms and digit ratios in a college sample. American Journal of Human Biology, 19, 41–50. https://doi.org/10.1002/ajhb.20571
Sucksdorff, M., Lehtonen, L., Chudal, R., Suominen, A., Gissler, M., & Sourander, A. (2018). Lower Apgar scores and Caesarean sections are related to attention-deficit/hyperactivity disorder. Acta Paediatrica, 107, 1750–1758. https://doi.org/10.1111/apa.14349
Sullivan, E. L., Nousen, E. K., & Chamlou, K. A. (2014). Maternal high fat diet consumption during the perinatal period programs offspring behavior. Physiology and Behavior, 123, 236–242. https://doi.org/10.1016/j.physbeh.2012.07.014
Sullivan, M. C., Msall, M. E., & Miller, R. J. (2012). 17-year outcome of preterm infants with diverse neonatal morbidities: Part 1–Impact on physical, neurological, and psychological health status. Journal for Specialists in Pediatric Nursing: JSPN, 17, 226–241. https://doi.org/10.1111/j.1744-6155.2012.00337.x
Sutton, A. J., Abrams, K. R., Jones, D. R., Sheldon, T. A., & Song, F. (2000). Methods for meta-analysis in medical research. New York: J. Wiley Chichester. https://doi.org/10.1002/sim.1565
Tervo, T., Michelsson, K., Launes, J., & Hokkanen, L. (2017). A prospective 30-year follow-up of ADHD associated with perinatal risks. Journal of Attention Disorders, 21, 799–810. https://doi.org/10.1177/1087054714548036
Tseng, P. T., Yen, C. F., Chen, Y. W., Stubbs, B., Carvalho, A. F., Whiteley, P., Chu, C. S., Li, D. J., Chen, T. Y., Yang, W. C., Tang, C. H., Liang, H. Y., Yang, W. C., Wu, C. K., & Lin, P. Y. (2019). Maternal breastfeeding and attention-deficit/hyperactivity disorder in children: A meta-analysis. European Child & Adolescent Psychiatry, 28, 19–30. https://doi.org/10.1007/s00787-018-1182-4
U.S. Department of Health and Human Services, Health Resources and Services Administration, Maternal and Child Health Bureau. (2013). Child Health USA 2013. Rockville, Maryland. https://mchb.hrsa.gov/sites/default/files/mchb/Data/Chartbooks/childhealth2013.pdf. Accessed 6 May 2021.
Vanderbilt, D., & Gleason, M. M. (2010). Mental health concerns of the premature infant through the lifespan. Child and Adolescent Psychiatric Clinics of North America, 19(2), 211–228. https://doi.org/10.1016/j.chc.2010.02.003
Wagner, A. I., Schmidt, N. L., Lemery-Chalfant, K., Leavitt, L. A., & Goldsmith, H. H. (2009). The limited effects of obstetrical and neonatal complications on conduct and attention-deficit hyperactivity disorder symptoms in middle childhood. Journal of Developmental and Behavioral Pediatrics: JDBP, 30, 217–225. https://doi.org/10.1097/DBP.0b013e3181a7ee98
Walfish, M., Neuman, A., & Wlody, D. (2009). Maternal haemorrhage. British Journal of Anaesthesia, 103, i47-56. https://doi.org/10.1093/bja/aep303
Walker, C. K., Krakowiak, P., Baker, A., Hansen, R. L., Ozonoff, S., & Hertz-Picciotto, I. (2015). Preeclampsia, placental insufficiency, and autism spectrum disorder or developmental delay. JAMA Pediatrics, 169, 154–162. https://doi.org/10.1001/jamapediatrics.2014.2645
Wang, Y., Hu, D., Chen, W., Xue, H., & Du, Y. (2019). Prenatal tobacco exposure modulated the association of genetic variants with diagnosed ADHD and its symptom domain in children: A community based case-control study. Scientific Reports, 9, 4274. https://doi.org/10.1038/s41598-019-40850-w
Wiggs, K., Elmore, A. L., Nigg, J. T., & Nikolas, M. A. (2016). Pre- and perinatal risk for attention-deficit hyperactivity disorder: Does neuropsychological weakness explain the link? Journal of Abnormal Child Psychology, 44, 1473–1485. https://doi.org/10.1007/s10802-016-0142-z
Zhu, P., Hao, J. H., Tao, R. X., Huang, K., Jiang, X. M., Zhu, Y. D., & Tao, F. B. (2015). Sex-specific and time-dependent effects of prenatal stress on the early behavioral symptoms of ADHD: A longitudinal study in China. European Child & Adolescent Psychiatry, 24, 1139–1147. https://doi.org/10.1007/s00787-015-0701-9
Acknowledgements
The authors would like to acknowledge Lu (Mary) Meng, Ph.D., and Jaleal Sanjak, Ph.D. for their assistance in creating the Forest Plots for these analyses.
Funding
National Center on Birth Defects and Developmental Disabilities,ID04130157.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
All authors report no potential conflicts of interest.
Research Involving Human Participants and/or Animals
This study includes analyses of data previously published in the literature.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The findings and conclusions in this manuscript are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bitsko, R.H., Holbrook, J.R., O’Masta, B. et al. A Systematic Review and Meta-analysis of Prenatal, Birth, and Postnatal Factors Associated with Attention-Deficit/Hyperactivity Disorder in Children. Prev Sci (2022). https://doi.org/10.1007/s11121-022-01359-3
Accepted:
Published:
DOI: https://doi.org/10.1007/s11121-022-01359-3