Abstract
Purpose
Delayed postoperative hyponatremia (DPH) is a unique complication of transsphenoidal surgery (TSS) in pituitary tumors. Growth hormone (GH) enhances renal sodium reabsorption; however, the association between postoperative GH reduction and DPH in acromegaly is unclear. This study was performed to clarify the incidence of and the predictive factors for DPH in patients with acromegaly who underwent TSS.
Methods
Ninety-four patients with active acromegaly were examined retrospectively. During the postoperative course, patients with serum sodium levels ≤ 134 mEq/L were classified into the DPH group. We compared basic clinical characteristics, tumor characteristics, and preoperative and postoperative examination findings between the DPH and non-DPH groups.
Results
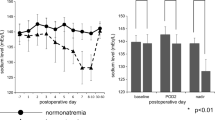
DPH occurred in 39 patients (41.5%), and the lowest serum sodium levels were generally observed during postoperative days (PODs) 7–9. They needed a 3-day longer hospital stay than those without DPH. The DPH group had lower preoperative body weight and body mass index. In addition, a transient increase in body weight during PODs 5–7 occurred with a transient decrease in urinary volume in the DPH group. Preoperative and postoperative GH and insulin-like growth factor-1 levels did not differ between the two groups.
Conclusion
The findings suggested that lower preoperative weight and a postoperative transient gain in body weight are associated with an increased risk of DPH in acromegaly patients undergoing transsphenoidal surgery.



Similar content being viewed by others
Data availability
The data sets are not publicly available but are available from the corresponding author on reasonable request.
References
Melmed S (2009) Acromegaly pathogenesis and treatment. J Clin Invest 119:3189–3202. https://doi.org/10.1172/JCI39375
Petrossians P, Daly AF, Natchev E, Maione L, Blijdorp K, Sahnoun-Fathallah M, Auriemma R, Diallo AM, Hulting AL, Ferone D, Hana V Jr, Filipponi S, Sievers C, Nogueira C, Fajardo-Montañana C, Carvalho D, Hana V, Stalla GK, Jaffrain-Réa ML, Delemer B, Colao A, Brue T, Neggers SJCMM, Zacharieva S, Chanson P, Beckers A (2017) Acromegaly at diagnosis in 3173 patients from the Liege Acromegaly Survey (LAS) Database. Endocr Relat Cancer 24:505–518. https://doi.org/10.1530/ERC-17-0253
Cote DJ, Alzarea A, Acosta MA, Hulou MM, Huang KT, Almutairi H, Alharbi A, Zaidi HA, Algrani M, Alatawi A, Mekary RA, Smith TR (2016) Predictors and rates of delayed symptomatic hyponatremia after transsphenoidal surgery: a systematic review. World Neurosurg 88:1–6. https://doi.org/10.1016/j.wneu.2016.01.022
Hensen J, Henig A, Fahlbusch R, Meyer M, Boehnert M, Buchfelder M (1999) Prevalence, predictors and patterns of postoperative polyuria and hyponatraemia in the immediate course after transsphenoidal surgery for pituitary adenomas. Clin Endocrinol (Oxford) 50:431–439. https://doi.org/10.1046/j.1365-2265.1999.00666.x
Kelly DF, Laws ER Jr, Fossett D (1995) Delayed hyponatremia after transsphenoidal surgery for pituitary adenoma. J Neurosurg 83:363–367. https://doi.org/10.3171/jns.1995.83.2.0363
Patel KS, Shu CJ, Yuan F, Attiah M, Wilson B, Wang MB, Bergsneider M, Kim W (2019) Prediction of postoperative delayed hyponatremia after endoscopic transsphenoidal surgery. Clin Neurol Neurosurg 182:87–91. https://doi.org/10.1016/j.clineuro.2019.05.007
Zada G, Liu CY, Fishback D, Singer PA, Weiss MH (2007) Recognition and management of delayed hyponatremia following transsphenoidal pituitary surgery. J Neurosurg 106:66–71. https://doi.org/10.3171/jns.2007.106.1.66
Tomita Y, Kurozumi K, Inagaki K, Kameda M, Ishida J, Yasuhara T, Ichikawa T, Sonoda T, Otsuka F, Date I (2019) Delayed postoperative hyponatremia after endoscopic transsphenoidal surgery for pituitary adenoma. Acta Neurochir (Wien) 161:707–715. https://doi.org/10.1007/s00701-019-03818-3
Kinoshita Y, Tominaga A, Arita K, Sugiyama K, Hanaya R, Hama S, Sakoguchi T, Usui S, Kurisu K (2011) Postoperative hyponatremia in patients with pituitary adenoma: postoperative management with a uniform treatment protocol. Endocr J 58:373–379. https://doi.org/10.1507/endocrj.k10e-352
Hussain NS, Piper M, Ludlam WG, Ludlam WH, Fuller CJ, Mayberg MR (2013) Delayed postoperative hyponatremia after transsphenoidal surgery: prevalence and associated factors. J Neurosurg 119:1453–1460. https://doi.org/10.3171/2013.8.JNS13411
Staiger RD, Sarnthein J, Wiesli P, Schmid C, Bernays RL (2013) Prognostic factors for impaired plasma sodium homeostasis after transsphenoidal surgery. Br J Neurosurg 27:63–68. https://doi.org/10.3109/02688697.2012.714013
Olson BR, Gumowski J, Rubino D, Oldfield EH (1997) Pathophysiology of hyponatremia after transsphenoidal pituitary surgery. J Neurosurg 87:499–507. https://doi.org/10.3171/jns.1997.87.4.0499
Wei T, Zuyuan R, Changbao S, Renzhi W, Yi Y, Wenbin M (2003) Hyponatremia after transsphenoidal surgery of pituitary adenoma. Chin Med Sci J 18:120–123
Lee JI, Cho WH, Choi BK, Cha SH, Song GS, Choi CH (2008) Delayed hyponatremia following transsphenoidal surgery for pituitary adenoma. Neurol Med Chir (Tokyo) 48:489–494. https://doi.org/10.2176/nmc.48.489
Sata A, Hizuka N, Kawamata T, Hori T, Takano K (2006) Hyponatremia after transsphenoidal surgery for hypothalamo-pituitary tumors. Neuroendocrinology 83:117–122. https://doi.org/10.1159/000094725
de Herder WW (2016) The history of acromegaly. Neuroendocrinology 103:7–17. https://doi.org/10.1159/000371808
Bohl MA, Ahmad S, Jahnke H, Shepherd D, Knecht L, White WL, Little AS (2016) Delayed hyponatremia is the most common cause of 30-day unplanned readmission after transsphenoidal surgery for pituitary tumors. Neurosurgery 78:84–90. https://doi.org/10.1227/NEU.0000000000001003
Yoon HK, Lee HC, Kim YH, Lim YJ, Park HP (2019) Predictive factors for delayed hyponatremia after endoscopic transsphenoidal surgery in patients with nonfunctioning pituitary tumors: a retrospective observational study. World Neurosurg 122:e1457–e1464. https://doi.org/10.1016/j.wneu.2018.11.085
Tominaga A, Arita K, Kurisu K, Uozumi T, Migita K, Eguchi K, Iida K, Kawamoto H, Mizoue T (1998) Effects of successful adenomectomy on body composition in acromegaly. Endocr J 45:335–342. https://doi.org/10.1507/endocrj.45.335
Giustina A, Chanson P, Bronstein MD, Klibanski A, Lamberts S, Casanueva FF, Trainer P, Ghigo E, Ho K, Melmed S (2010) Acromegaly consensus group: a consensus on criteria for cure of acromegaly. J Clin Endocrinol Metab 95:3141–3148. https://doi.org/10.1210/jc.2009-2670
Sane T, Rantakari K, Poranen A, Tähtelä R, Välimäki M, Pelkonen R (1994) Hyponatremia after transsphenoidal surgery for pituitary tumors. J Clin Endocrinol Metab 79:1395–1398. https://doi.org/10.1210/jcem.79.5.7962334
Van Gompel JJ, Atkinson JLD, Choby G, Kasperbauer JL, Stokken JK, Janus JR, O’Brien EK, Little JT, Bancos I, Davidge-Pitts CJ, Ramachandran D, Herndon JS, Erickson D, Lanier WL (2021) Pituitary tumor surgery: comparison of endoscopic and microscopic techniques at a single center. Mayo Clin Proc 96:2043–2057. https://doi.org/10.1016/j.mayocp.2021
Song S, Wang L, Qi Q, Wang H, Feng L (2022) Endoscopic vs. microscopic transsphenoidal surgery outcomes in 514 nonfunctioning pituitary adenoma cases. Neurosurg Rev 45:2375–2383. https://doi.org/10.1007/s10143-022-01732-4
Whitaker SJ, Meanock CI, Turner GF, Smythe PJ, Pickard JD, Noble AR, Walker V (1985) Fluid balance and secretion of antidiuretic hormone following transsphenoidal pituitary surgery. A preliminary series. J Neurosurg 63:404–412. https://doi.org/10.3171/jns.1985.63.3.0404
Tymms J, Clark JD, Griffith HB, Reckless JP, Hartog M (1992) Pituitary surgery and inappropriate antidiuretic hormone secretion. J R Soc Med 85:302
Amann K, Benz K (2013) Structural renal changes in obesity and diabetes. Semin Nephrol 33:23–33. https://doi.org/10.1016/j.semnephrol.2012.12.003
Hoffman DM, Crampton L, Sernia C, Nguyen TV, Ho KK (1996) Short-term growth hormone (GH) treatment of GH-deficient adults increases body sodium and extracellular water, but not blood pressure. J Clin Endocrinol Metab 81:1123–1128. https://doi.org/10.1210/jcem.81.3.8772586
Asemota AO, Ishii M, Brem H, Gallia GL (2017) Comparison of complications, trends, and costs in endoscopic vs microscopic pituitary surgery: analysis from a US health claims database. Neurosurgery 81(3):458–472. https://doi.org/10.1093/neuros/nyx350
Takeuchi K, Nagatani T, Okumura E, Wakabayashi T (2014) A novel method for managing water and electrolyte balance after transsphenoidal surgery: preliminary study of moderate water intake restriction. Nagoya J Med Sci 76:73–82
Yu S, Taghvaei M, Reyes M, Piper K, Collopy S, Gaughan JP, Prashant GN, Karsy M, Evans JJ (2022) Delayed symptomatic hyponatremia in transsphenoidal surgery: systematic review and meta-analysis of its incidence and prevention with water restriction. Clin Neurol Neurosurg 214:107166. https://doi.org/10.1016/j.clineuro.2022.107166
Papadimitriou DT, Spiteri A, Pagnier A, Bayle M, Mischalowski MB, Bourdat G, Passagia JG, Plantaz D, Bost M, Garnier PE (2007) Mineralocorticoid deficiency in postoperative cerebral salt wasting. J Pediatr Endocrinol Metab 20:1145–1150. https://doi.org/10.1515/jpem.2007.20.10.1145
Funding
None declared.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. RM, SF, TH, MY, SK, HH and NH: performed data collection and data analysis. RM, SF and KA: wrote the main manuscript text. RM and SF: prepared all figures. YN, KY and RH: supervised the study. All coauthors read, commented, and revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflict of interest.
Ethical approval
This study was approved by the Kagoshima University Hospital Ethics Committee (Reference no. 21–0007). Study-specific informed consent was waived due to the retrospective and noninvasive nature of our study. An opt-out approach was offered to all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Makino, R., Fujio, S., Hanada, T. et al. Delayed postoperative hyponatremia in patients with acromegaly: incidence and predictive factors. Pituitary 26, 42–50 (2023). https://doi.org/10.1007/s11102-022-01288-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-022-01288-y