Abstract
Purpose
Granular cell tumors (GCT) are highly vascularized and adherent to adjacent structures, and so, complete resection represents a challenge. Adjuvant therapy decisions for residual GCTs currently relies on individual clinician decisions due to a paucity of systematic literature data. We present a comprehensive analysis about the impact of adjuvant therapy in reported cases of patients with incomplete GCT resection.
Methods
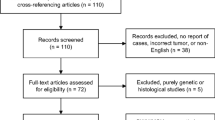
One database (PubMed) and crossed references were queried for GCT with incomplete resection or biopsy from 1962 to 2020. Literature review was performed according to the PRISMA guidelines. Also, two patients with residual GCT from our institutions are added to the analysis. Data regarding clinical presentation, surgical approach, use of adjuvant therapy, Ki-67 labeling, and follow up assessments were extracted and analyzed from selected publications.
Results
Thirty-three studies met the predetermined inclusion criteria and 53 patients were selected (including our two reported cases). The median of age was 49 [IQR, 39–60 years], with a slight male predominance (1.2:1). Among the surgical procedures, seven (13%) were biopsies alone. Adjuvant therapy was used in 18 patients (radiotherapy, 94.5%; chemotherapy, 5.5%) but there is no statistical correlation with adjuvant therapy and the progression of the remnant tumor (p = 0.33). Our institutions’ patients did not receive adjuvant therapy and did not show tumor progression on MRI.
Conclusion
Our systematic literature review suggests there is a limited role for chemo and/or radiotherapy in the management of incomplete GCT resection. It may be reasonable recommending close clinical follow up in patients with incomplete resection.





Similar content being viewed by others
Abbreviations
- GCT:
-
Granular cell tumor
- STR:
-
Subtotal resection
- PR:
-
Partial resection
- MRI:
-
Magnetic resonance imaging
- CT:
-
Computed tomography
- GTR:
-
Gross total resection
- RT:
-
Radiotherapy
- CTX:
-
Chemotherapy
- CFU:
-
Close follow up
- WHO:
-
World Health Organization
References
Boyce R, Beadles CF (1893) A further contribution to the study of the pathology of the hypophysis cerebri. J Pathol Bacteriol 1:359–383
Glazer N, Hauser H, Slade H (1956) Granular cell tumor of the neurohypophysis. Am J Roentgenol Radium Ther Nucl Med. https://doi.org/10.1007/978-3-7091-8420-2_8
Luse SA, Kernohan JW (1955) Granular-cell tumors of the stalk and posterior lobe of the pituitary gland. Cancer 8:616–622
DeLellis RA (2004) Pathology and genetics of tumours of endocrine organs. IARC, Lyon
Mete O, Lopes MB, Asa SL (2013) Spindle cell oncocytomas and granular cell tumors of the pituitary are variants of pituicytoma. Am J Surg Pathol. https://doi.org/10.1097/PAS.0b013e31829723e7
Lopes MBS (2017) The 2017 World Health Organization classification of tumors of the pituitary gland: a summary. Acta Neuropathol 134:521–535
Louis DN, Perry A, Reifenberger G et al (2016) The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131:803–820
Orning JL, Trembath DG, Zanation AM, Germanwala AV (2013) Endoscopic endonasal approach for resection of infundibular granular cell tumor: case report and literature review. J Case Rep Med. https://doi.org/10.4303/jcrm/235775
Famini P, Maya MM, Melmed S (2011) Pituitary magnetic resonance imaging for sellar and parasellar masses: ten-year experience in 2598 patients. J Clin Endocrinol Metab. https://doi.org/10.1210/jc.2011-0168
Han F, Gao L, Wang Y et al (2018) Clinical and imaging features of granular cell tumor of the neurohypophysis. Medicine (United States). https://doi.org/10.1097/MD.0000000000009745
Tomita T, Gates E (1999) Pituitary adenomas and granular cell tumors: Incidence, cell type, and location of tumor in 100 pituitary glands at autopsy. Am J Clin Pathol. https://doi.org/10.1093/ajcp/111.6.817
Liwnicz BH, Liwnicz BH, Liwnicz RG et al (1984) Giant granular cell tumor of the suprasellar area; immunocytochemical and electron microscopic studies. Neurosurgery 15:246–251
Gibbs WN, Monuki ES, Linskey ME, Hasso AN (2006) Pituicytoma: diagnostic features on selective carotid angiography and MR imaging. Am J Neuroradiol 24:1639–1642
Zhang Y, Teng Y, Zhu H et al (2018) Granular cell tumor of the neurohypophysis: 3 cases and a systematic literature review of 98 cases. World Neurosurg 118:e621–e630
Cone L, Srinivasan M, Romanul FC (1990) Granular cell tumor (choristoma) of the neurohypophysis: two cases and a review of the literature. Am J Neuroradiol 11:403–406
Melmed S (2020) Pituitary-tumor endocrinopathies. N Engl J Med 382:937–950
Gagliardi F, Losa M, Boari N et al (2013) Suprasellar granular cell tumor of the neurohypophysis in a child: unusual presentation in pediatric age of a rare tumor. Child’s Nerv Syst 29:1031–1034
Faramand A, Kano H, Flickinger JC et al (2018) A Case of symptomatic granular cell tumor of the pituitary treated with stereotactic radiosurgery. Stereotact Funct Neurosurg 96:1–7
Schaller B, Kirsch E, Tolnay M, Mindermann T (1998) Symptomatic granular cell tumor of the pituitary gland: case report and review of the literature. Neurosurgery. https://doi.org/10.1097/00006123-199801000-00036
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol. https://doi.org/10.1016/j.jclinepi.2009.06.005
Koutourousiou M, Gardner PA, Kofler JK et al (2013) Rare infundibular tumors: clinical presentation, imaging findings, and the role of endoscopic endonasal surgery in their management. J Neurol Surgery B 74:1–11. https://doi.org/10.1055/s-0032-1329619
Saint-Blancard P, Pierre B, Philippe C, de Soultrait FR (2007) Une cause rare de diminution de l’acuité visuelle : la tumeur à cellules granuleuses neurohypophysaire. Neurochirurgie 53:296–298. https://doi.org/10.1016/j.neuchi.2007.05.004
Kobayashi TK, Bamba M, Oka H et al (2006) Granular cell tumour of the neurohypophysis on cytological squash preparations. Cytopathology 17:153–154
Nishio S, Takeshita I, Yoshimoto K, Yamaguchi T (1998) Granular cell tumor of the pituitary stalk. Clin Neurol Neurosurg. https://doi.org/10.1016/S0303-8467(98)00017-1
Higuchi M, Tsuji M, Iked HA (1997) Sym ptom atic hypophyseal granular cell tum our: endocrinological and clinicopathological analysis. Br J Neurosurg 11:582–586
Bello CT, Cipriano P, Henriques V et al (2018) Granular cell tumour of the neurohypophysis: an unusual cause of hypopituitarism. Endocrinol Diabetes Metab Case Rep. https://doi.org/10.1530/edm-17-0178
Friede RL, Yasargil MG (1977) Suprasellar neoplasm with a granular cell component. J Neuropathol Exp Neurol. https://doi.org/10.1097/00005072-197709000-00001
Liu HL, Huang BY, Zhang MS et al (2017) Sellar and suprasellar granular cell tumor of neurohypophysis. Chin Med J (Engl) 130:741–743. https://doi.org/10.4103/0366-6999.201605
Freda PU, Beckers AM, Katznelson L et al (2011) Pituitary incidentaloma: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. https://doi.org/10.1210/jc.2010-1048
Freda PU, Wardlaw SL (1999) Clinical review 110: diagnosis and treatment of pituitary tumors. J Clin Endocrinol Metab 84:3859–3866
Cohen-Gadol AA, Pichelmann MA, Link MJ et al (2003) Granular cell tumor of the sellar and suprasellar region: clinicopathologic study of 11 cases and literature review. Mayo clinic proceedings. Elsevier, Amsterdam, pp 567–573
Ahmed AK, Dawood HY, Cote DJ et al (2019) Surgical resection of granular cell tumor of the sellar region: three indications. Pituitary. https://doi.org/10.1007/s11102-019-00999-z
Feng Z, Mao Z, Wang Z et al (2018) Non-adenomatous pituitary tumours mimicking functioning pituitary adenomas. Br J Neurosurg. https://doi.org/10.1080/02688697.2018.1464121
Shuangshoti S, Navalitloha Y, Shuangshoti S et al (1998) Atypical granular cell tumor of the neurohypophysis: a case report with review of the literature. J Med Assoc Thail 81:641–646
Becker DH, Wilson CB (1981) Symptomatic parasellar granular cell tumors. Neurosurgery 8:173–179. https://doi.org/10.1227/00006123-198102000-00006
Guerrero-Pérez F, Vidal N, Marengo AP et al (2019) Posterior pituitary tumours: the spectrum of a unique entity. A clinical and histological study of a large case series. Endocrine 63:36–43. https://doi.org/10.1007/s12020-018-1774-2
Kasashima S, Oda Y, Nozaki JI et al (2000) A case of atypical granular cell tumor of the neurohypophysis. Pathol Int 50:568–573. https://doi.org/10.1046/j.1440-1827.2000.01080.x
Doron Y, Behar A, Beller AJ (1965) Granular-cell “myoblastoma” of the neurohypophysis. J Neurosurg 22:95–99. https://doi.org/10.3171/jns.1965.22.1.0095
Menon G, Easwer HV, Radhakrishnan VV, Nair S (2008) Symptomatic granular cell tumour of the pituitary. Br J Neurosurg 22:126–130. https://doi.org/10.1080/02688690701604566
Fazekas JT (1977) Treatment of grades I and II brain astrocytomas. The role of radiotherapy. Int J Radiat Oncol Biol Phys. https://doi.org/10.1016/0360-3016(77)90045-1
Stieber VW, Mehta MP (2007) Advances in radiation therapy for brain tumors. Neurol Clin 25:1005–1033
Al-Mefty O, Kersh JE, Routh A, Smith RR (1990) The long-term side effects of radiation therapy for benign brain tumors in adults. J Neurosurg. https://doi.org/10.3171/jns.1990.73.4.0502
Surma-Aho O, Niemelä M, Vilkki J et al (2001) Adverse long-term effects of brain radiotherapy in adult low-grade glioma patients. Neurology. https://doi.org/10.1212/WNL.56.10.1285
Donahue B (1992) Short- and long-term complications of radiation therapy for pediatric brain tumors. Pediatr Neurosurg 18:207–217
Rim CH, Yang DS, Park YJ et al (2011) Radiotherapy for pituitary adenomas: long-term outcome and complications. Radiat Oncol J. https://doi.org/10.3857/roj.2011.29.3.156
Jang JW, Chan AW (2013) Prevention and management of complications after radiotherapy for skull base tumors: a multidisciplinary approach. Adv Otorhinolaryngol. https://doi.org/10.1159/000342293
Cook B, Withrow LA, Spencer SA et al (2004) Radiation tolerance of the optic apparatus. Int J Radiat Oncol. https://doi.org/10.1016/j.ijrobp.2004.07.289
Burston J, John R, Spencer H (1962) Myoblastoma ” of the neurohypophysis. J Pathol Bacteriol 83:455–461
Moriyama E, Matsumoto Y, Meguro T, Mano S (1996) Suprasellar granular cell tumor: case report. Neurol Med Chir (Tokyo) 36:237–240. https://doi.org/10.2176/nmc.36.237
Ogata S, Shimazaki H, Aida S et al (2001) Giant intracranial granular-cell tumor arising from the abducens. Pathol Int 51:481–486. https://doi.org/10.1046/j.1440-1827.2001.01229.x
Rhee JS, Wackym PA, Hague K et al (2002) Granular cell tumor of the pituitary fossa. Ann Otol Rhinol Laryngol. https://doi.org/10.1177/000348940211100818
Lee CC, Liu CH, Wei CP, How SW (2004) Symptomatic granular cell tumor of the neurohypophysis. J Formos Med Assoc 103:58–62
Aquilina K, Kamel M, Kalimuthu SG et al (2006) Granular cell tumour of the neurohypophysis: a rare sellar tumour with specific radiological and operative features. Br J Neurosurg 20:51–54. https://doi.org/10.1080/02688690600600996
Shizukuishi T, Abe O, Haradome H et al (2014) Granular cell tumor of the neurohypophysis with optic tract edema. Jpn J Radiol 32:179–182. https://doi.org/10.1007/s11604-013-0279-4
Lettau M, Munk R (2014) Granularzelltumor des Infundibulums. RoFo Fortschritte auf dem Gebiet der Rontgenstrahlen und der Bildgeb Verfahren 186:805–806. https://doi.org/10.1055/s-0033-1356188
Gregoire A, Bosschaert P, Godfraind C (2015) Granular cell tumor of the pituitary stalk: a rare and benign entity. J Belg Soc Radiol 99:79–81. https://doi.org/10.5334/jbr-btr.841
Li P, Yang Z, Wang Z et al (2016) Granular cell tumors in the central nervous system: a report on eight cases and a literature review. Br J Neurosurg 30:611–618. https://doi.org/10.1080/02688697.2016.1181152
Gagliardi F, Spina A, Barzaghi LR et al (2016) Suprasellar granular cell tumor of the neurohypophysis: surgical outcome of a very rare tumor. Pituitary. https://doi.org/10.1007/s11102-016-0704-7
Thakkar K, Ramteke-Jadhav S, Kasaliwal R et al (2020) Sellar surprises: a single-centre experience of unusual sellar masses. Endocr Connect. https://doi.org/10.1530/EC-19-0497
Acknowledgements
We would like to acknowledge the meaningful contributions of Jose Otero, MD, PhD (Pathology Department, Ohio State University), who provided the pathological slides and helped with the histology description.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Daniel M. Prevedello is a consultant for Integra LifeSciences Corp, Stryker Corporation and Medtronic Corp. Daniel Prevedello has equity on 3 rivers LLC, eLUM Technologies, LLC and Soliton LLC. Daniel Prevedello receives royalties from KLS-Martin, ACE Medical and Mizuho.
Informed consent
To participate, prior informed consent from the patients was obtained. Data collection was performed under the protocols of the Human Research Protection Office of both institutions.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rubino, F., Martinez-Perez, R., Vieira, S. et al. Granular cell tumors of the sellar region: what should be done after subtotal resection? A systematic review. Pituitary 23, 721–732 (2020). https://doi.org/10.1007/s11102-020-01068-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-020-01068-6