Abstract
Background
Medication errors significantly compromise patient safety in emergency departments. Although previous studies have investigated the prevalence of these errors in this setting, results have varied widely.
Aim
The aim was to report pooled data on the prevalence and severity of medication errors in emergency departments, as well as the proportion of patients affected by these errors.
Method
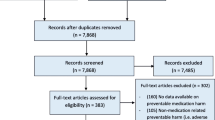
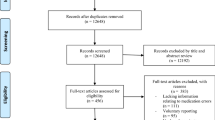
Systematic searches were conducted in Embase, PubMed, and the Cochrane Library from database inception until June 2023. Studies provided numerical data on medication errors within emergency departments were eligible for inclusion. Random-effects meta-analysis was employed to pool the prevalence of medication errors, the proportion of patients experiencing these errors, and the error severity levels. Heterogeneity among studies was assessed using the I2 statistic and Cochran’s Q test.
Results
Twenty-four studies met the inclusion criteria. The meta-analysis gave a pooled prevalence of medication errors in emergency departments of 22.6% (95% Confidence Interval [CI] 19.2–25.9%, I2 = 99.9%, p < 0.001). The estimated proportion of patients experiencing medication errors was 36.3% (95% CI 28.3–44.3%, I2 = 99.8%, p < 0.001). Of these errors, 42.6% (95% CI 5.0–80.1%) were potentially harmful but not life-threatening, while no-harm errors accounted for 57.3% (95% CI 14.1–100.0%).
Conclusion
The prevalence of medication errors, particularly those potentially harmful, underscores potential safety issues in emergency departments. It is imperative to develop and implement effective interventions aimed at reducing medication errors and enhancing patient safety in this setting.



Similar content being viewed by others
References
Dietz I, Borasio GD, Schneider G, et al. Medical errors and patient safety in palliative care: a review of current literature. J Palliat Med. 2010;13(12):1469–74. https://doi.org/10.1089/jpm.2010.0228.
Ehsani SR, Cheraghi MA, Nejati A, et al. Medication errors of nurses in the emergency department. J Med Ethics Hist Med. 2013;6:11.
Acheampong F, Anto BP, Koffuor GA. Medication safety strategies in hospitals–a systematic review. Int J Risk Saf Med. 2014;26(3):117–31. https://doi.org/10.3233/jrs-140623.
Nikpeyma N, Gholamnejad H. Reason for medication errors in nurses’ views. Adv Nurs Midwifery. 2009;19:18–24.
National Coordinating Council for Medication Error Reporting and Prevention. About Medication Errors. In: The National Coordinating Council for Medication Error Reporting and Prevention (NCC MERP). https://www.nccmerp.org/about-medication-errors. Accessed 30 June 2023.
Bates DW, Slight SP. Medication errors: What is their impact? Mayo Clin Proc. 2014;89(8):1027–9. https://doi.org/10.1016/j.mayocp.2014.06.014.
Glavin RJ. Drug errors: consequences, mechanisms, and avoidance. Br J Anaesth. 2010;105(1):76–82. https://doi.org/10.1093/bja/aeq131.
Elliott RA, Camacho E, Jankovic D, et al. Economic analysis of the prevalence and clinical and economic burden of medication error in England. BMJ Qual Saf. 2021;30(2):96–105. https://doi.org/10.1136/bmjqs-2019-010206.
Gautam PL. Minimizing medication errors: Moving attention from individual to system. J Anaesthesiol Clin Pharmacol. 2013;29(3):293–4. https://doi.org/10.4103/0970-9185.117037.
Phillips DP, Christenfeld N, Glynn LM. Increase in US medication-error deaths between 1983 and 1993. Lancet. 1998;351(9103):643–4. https://doi.org/10.1016/s0140-6736(98)24009-8.
Bates DW, Spell N, Cullen DJ, et al. The costs of adverse drug events in hospitalized patients. Adverse Drug Events Prevention Study Group. JAMA. 1997;277(4):307–11. https://doi.org/10.1001/jama.1997.03540280045032.
Walsh EK, Hansen CR, Sahm LJ, et al. Economic impact of medication error: a systematic review. Pharmacoepidemiol Drug Saf. 2017;26(5):481–97. https://doi.org/10.1002/pds.4188.
Källberg AS, Göransson KE, Östergren J, et al. Medical errors and complaints in emergency department care in Sweden as reported by care providers, healthcare staff, and patients—a national review. Eur J Emerg Med. 2013;20(1):33–8. https://doi.org/10.1097/MEJ.0b013e32834fe917.
Brennan-Bourdon LM, Vázquez-Alvarez AO, Gallegos-Llamas J, et al. A study of medication errors during the prescription stage in the pediatric critical care services of a secondary-tertiary level public hospital. BMC Pediatr. 2020;20(1):549. https://doi.org/10.1186/s12887-020-02442-w.
Kandil M, Sayyed T, Emarh M, et al. Medication errors in the obstetrics emergency ward in a low resource setting. J Matern Fetal Neonatal Med. 2012;25(8):1379–82. https://doi.org/10.3109/14767058.2011.636091.
Kozer E, Scolnik D, Macpherson A, et al. Variables associated with medication errors in pediatric emergency medicine. Pediatrics. 2002;110(4):737–42. https://doi.org/10.1542/peds.110.4.737.
Vazin A, Zamani Z, Hatam N. Frequency of medication errors in an emergency department of a large teaching hospital in southern Iran. Drug Healthc Patient Saf. 2014;6:179–84. https://doi.org/10.2147/dhps.S75223.
Vilà-de-Muga M, Colom-Ferrer L, Gonzàlez-Herrero M, et al. Factors associated with medication errors in the pediatric emergency department. Pediatr Emerg Care. 2011;27(4):290–4. https://doi.org/10.1097/PEC.0b013e31821313c2.
Howard I, Howland I, Castle N, et al. Retrospective identification of medication related adverse events in the emergency medical services through the analysis of a patient safety register. Sci Rep. 2022;12(1):2622. https://doi.org/10.1038/s41598-022-06290-9.
Bowman B. The cost of medication errors in the emergency department: implications for clinical pharmacy practice. In: MPA/MPP/MPFM Capstone Projects. 2010. https://uknowledge.uky.edu/mpampp_etds/120. Accessed 23 June 2023.
Hosseini Marznaki Z, Pouy S, Salisu WJ, et al. Medication errors among Iranian emergency nurses: a systematic review. Epidemiol Health. 2020;42:e2020030. https://doi.org/10.4178/epih.e2020030.
Naseralallah L, Stewart D, Price M, et al. Prevalence, contributing factors, and interventions to reduce medication errors in outpatient and ambulatory settings: a systematic review. Int J Clin Pharm. 2023;45(6):1359–77. https://doi.org/10.1007/s11096-023-01626-5.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372: n71. https://doi.org/10.1136/bmj.n71.
Thu ATP, Van BNV, Ha TN, et al. Prevalence of medication errors in the emergency department: a systematic review and meta-analysis. PROSPERO 2022 CRD42022316181. 2022. https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42022316181. Accessed 30 June 2023.
Alsulami Z, Conroy S, Choonara I. Medication errors in the Middle East countries: a systematic review of the literature. Eur J Clin Pharmacol. 2013;69(4):995–1008. https://doi.org/10.1007/s00228-012-1435-y.
Ghaleb MA, Barber N, Franklin BD, et al. Systematic review of medication errors in pediatric patients. Ann Pharmacother. 2006;40(10):1766–76. https://doi.org/10.1345/aph.1g717.
Salmasi S, Khan TM, Hong YH, et al. Medication errors in the Southeast Asian countries: a systematic review. PLoS One. 2015;10(9):e0136545. https://doi.org/10.1371/journal.pone.0136545.
Ouzzani M, Hammady H, Fedorowicz Z, et al. Rayyan—a web and mobile app for systematic reviews. Syst Rev. 2016;5(1):210. https://doi.org/10.1186/s13643-016-0384-4.
Allan EA, Barker KN. Fundamentals of medication error research. Am J Hosp Pharm. 1990;47(3):555–71.
National Coordinating Council for Medication Error Reporting and Prevention. NCC MERP Index for Categorizing Medication Errors Algorithm. The National Coordinating Council for Medication Error Reporting and Prevention (NCC MERP). 2001. https://www.nccmerp.org/categorizing-medication-errors-algorithm-color. Accessed 30 June 2023.
Borenstein M, Hedges LV, Higgins JP, et al. Introduction to meta-analysis. Wiley; 2021.
Petitti DB. Approaches to heterogeneity in meta-analysis. Stat Med. 2001;20(23):3625–33. https://doi.org/10.1002/sim.1091.
Abdel-Qader DH, Al Meslamani AZ, El-Shara’ AA, et al. Investigating prescribing errors in the emergency department of a large governmental hospital in Jordan. J Pharm Health Serv Res. 2020;11(4):375–82. https://doi.org/10.1111/jphs.12376.
Acheampong F, Tetteh AR, Anto BP. Medication administration errors in an adult emergency department of a tertiary health care facility in Ghana. J Patient Saf. 2016;12(4):223–8. https://doi.org/10.1097/pts.0000000000000105.
Jain S, Basu S, Parmar VR. Medication errors in neonates admitted in intensive care unit and emergency department. Indian J Med Sci. 2009;63(4):145–51.
Zeraatchi A, Talebian MT, Nejati A, et al. Frequency and types of the medication errors in an academic emergency department in Iran: the emergent need for clinical pharmacy services in emergency departments. J Res Pharm Pract. 2013;2(3):118–22. https://doi.org/10.4103/2279-042x.122384.
Beatriz GC, María José O, Inés JL, et al. Medication errors in children visiting pediatric emergency departments. Farm Hosp. 2023;47(4):141–7. https://doi.org/10.1016/j.farma.2023.03.006.
Bakhsh HT, Perona SJ, Shields WA, et al. Medication errors in psychiatric patients boarded in the emergency department. Int J Risk Saf Med. 2014;26(4):191–8. https://doi.org/10.3233/jrs-140634.
Dabaghzadeh F, Rashidian A, Torkamandi H, et al. Medication errors in an emergency department in a large teaching hospital in Tehran. Iran J Pharm Res. 2013;12(4):937–42.
Gregory H, Cantley M, Calhoun C, et al. Incidence of prescription errors in patients discharged from the emergency department. Am J Emerg Med. 2021;46:266–70. https://doi.org/10.1016/j.ajem.2020.07.061.
Marcin JP, Dharmar M, Cho M, et al. Medication errors among acutely ill and injured children treated in rural emergency departments. Ann Emerg Med. 2007;50(4):361–77. https://doi.org/10.1016/j.annemergmed.2007.01.020.
Murray KA, Belanger A, Devine LT, et al. Emergency department discharge prescription errors in an academic medical center. Proc (Bayl Univ Med Cent). 2017;30(2):143–6. https://doi.org/10.1080/08998280.2017.11929562.
Akhil N, Thomas PP, Shivaraj D, et al. Assessment, evaluation, and analysis of the medication errors of the patients admitted at the emergency department of a tertiary care teaching hospital of a South Indian city. Asian J Pharm Clin Res. 2017;10:161. https://doi.org/10.22159/ajpcr.2017.v10i5.17170.
Shitu Z, Aung MMT, Tuan Kamauzaman TH, et al. Prevalence and characteristics of medication errors at an emergency department of a teaching hospital in Malaysia. BMC Health Serv Res. 2020;20(1):56. https://doi.org/10.1186/s12913-020-4921-4.
Stasiak P, Afilalo M, Castelino T, et al. Detection and correction of prescription errors by an emergency department pharmacy service. CJEM. 2014;16(3):193–206. https://doi.org/10.2310/8000.2013.130975.
Taylor BL, Selbst SM, Shah AE. Prescription writing errors in the pediatric emergency department. Pediatr Emerg Care. 2005;21(12):822–7. https://doi.org/10.1097/01.pec.0000190239.04094.72.
Patanwala AE, Warholak TL, Sanders AB, et al. A prospective observational study of medication errors in a tertiary care emergency department. Ann Emerg Med. 2010;55(6):522–6. https://doi.org/10.1016/j.annemergmed.2009.12.017.
Pham JC, Story JL, Hicks RW, et al. National study on the frequency, types, causes, and consequences of voluntarily reported emergency department medication errors. J Emerg Med. 2011;40(5):485–92. https://doi.org/10.1016/j.jemermed.2008.02.059.
Selbst SM, Fein JA, Osterhoudt K, et al. Medication errors in a pediatric emergency department. Pediatr Emerg Care. 1999;15(1):1–4. https://doi.org/10.1097/00006565-199902000-00001.
Anzan M, Alwhaibi M, Almetwazi M, et al. Prescribing errors and associated factors in discharge prescriptions in the emergency department: a prospective cross-sectional study. PLoS One. 2021;16(1):e0245321. https://doi.org/10.1371/journal.pone.0245321.
Negash G, Kebede Y, Hawaze S. Medication errors in the adult emergency unit of a tertiary care teaching hospital in Addis Ababa. Arch Pharm Pract. 2013;4(4):147–53. https://doi.org/10.4103/2045-080X.123220.
Thomas B, Paudyal V, MacLure K, et al. Medication errors in hospitals in the Middle East: a systematic review of prevalence, nature, severity and contributory factors. Eur J Clin Pharmacol. 2019;75(9):1269–82. https://doi.org/10.1007/s00228-019-02689-y.
Mira JJ, Lorenzo S, Guilabert M, et al. A systematic review of patient medication error on self-administering medication at home. Expert Opin Drug Saf. 2015;14(6):815–38. https://doi.org/10.1517/14740338.2015.1026326.
Montesi G, Lechi A. Prevention of medication errors: detection and audit. Br J Clin Pharmacol. 2009;67(6):651–5. https://doi.org/10.1111/j.1365-2125.2009.03422.x.
Malone PM, Malone MJ, Park SK. Drug information: a guide for pharmacists. McGraw-Hill, Medical Publication Division; 2006.
Cohen MR. Medication errors. American Pharmacist Association; 2007.
Gates PJ, Baysari MT, Gazarian M, et al. Prevalence of medication errors among paediatric inpatients: systematic review and meta-analysis. Drug Saf. 2019;42(11):1329–42. https://doi.org/10.1007/s40264-019-00850-1.
Aronson JK. Medication errors: what they are, how they happen, and how to avoid them. QJM. 2009;102(8):513–21. https://doi.org/10.1093/qjmed/hcp052.
Cloete L. Reducing medication errors in nursing practice. Nurs Stand. 2015;29(20):50–9. https://doi.org/10.7748/ns.29.20.50.e9507.
Merry AF, Anderson BJ. Medication errors—new approaches to prevention. Paediatr Anaesth. 2011;21(7):743–53. https://doi.org/10.1111/j.1460-9592.2011.03589.x.
Elden NMK, Ismail A. The importance of medication errors reporting in improving the quality of clinical care services. Glob J Health Sci. 2016;8(8):54510. https://doi.org/10.5539/gjhs.v8n8p243.
Likic R, Maxwell SR. Prevention of medication errors: teaching and training. Br J Clin Pharmacol. 2009;67(6):656–61. https://doi.org/10.1111/j.1365-2125.2009.03423.x.
Acknowledgements
We extend our sincere gratitude to Dr. Chia Jie Tan, Department of Pharmacotherapy, College of Pharmacy, University of Utah, U.S., for his invaluable review and insightful contributions to this work.
Funding
No sources of funding were used to assist in the preparation of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors of this article have no conflicts of interest that are directly relevant to the content of this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nguyen, P.T.L., Phan, T.A.T., Vo, V.B.N. et al. Medication errors in emergency departments: a systematic review and meta-analysis of prevalence and severity. Int J Clin Pharm (2024). https://doi.org/10.1007/s11096-024-01742-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11096-024-01742-w