Abstract
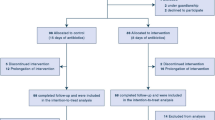
Background Non-ventilator associated hospital-acquired pneumonia accounts for significant antibiotic use and is associated with a high rate of resistance emergence. However, the optimal duration of antibiotic treatment is uncertain, especially in cases of non-fermenting gram-negative bacilli. Objective To compare a short course (5–7 days) to a prolonged course (10–14 days) of antibiotics for non-ventilator associated hospital-acquired pneumonia. Methods Data collected retrospectively on patients completed treatment in a Malaysian tertiary hospital from January 2017 till December 2018. Regression analysis determined variables independently associated with clinical outcome. Main outcome measures Clinical resolution, superinfection, 30-day and 90-day all-cause mortality between short and prolonged courses. Results Of the 167 patients included, 112 patients were treated with a short course antibiotic, whereas 55 patients received a prolonged course of therapy. Neither short nor prolonged course group has a significantly higher rate of clinical resolution. Short course group had significantly higher mean ± SD antibiotic-free days (21.9 ± 3.5 versus 15.1 ± 6.2 days, p < 0.001). Higher rate of superinfection was observed in prolonged course group compared to short course group (6.3% versus 18.2%, p = 0.027). For non-ventilator associated hospital-acquired pneumonia caused by non-fermenting gram-negative bacilli, the superinfection rate was higher in prolonged course group (35.7% versus 15.4%, p = 0.385) while 30-day mortality rate was higher in the short course group (38.5% versus 14.3%, p = 0.209). Non-fermenting gram-negative bacilli cause higher rate of superinfection (p = 0.010). Conclusion We found no clinical benefit as defined by clinical resolution and reduction in all-cause mortality in prolonging antimicrobial therapy. Superinfections emerge more frequently in prolonged course of antibiotic therapy and more likely to develop in non-fermenting gram-negative bacilli.

Similar content being viewed by others
Abbreviations
- AOR:
-
At own risk
- APACHE II:
-
Acute Physiologic and Chronic Health Evaluation II
- CHF:
-
Congestive heart failure
- COAD:
-
Chronic obstructive airway disease
- CPIS:
-
Clinical Pulmonary Infection Score
- CRP:
-
C-reactive protein
- DM:
-
Diabetes mellitus
- ESRF:
-
End-stage renal failure
- GOLD:
-
Global Initiative for Chronic Obstructive Lung Disease
- HAP:
-
Hospital-acquired pneumonia
- IV:
-
Intravenous
- MRSA:
-
Methicillin-resistant Staphylococcus aureus
- MSSA:
-
Methicillin-susceptible Staphylococcus aureus
- NF-GNB:
-
Non-fermenting gram-negative bacilli
- NV-HAP:
-
Non-ventilator associated hospital-acquired pneumonia
- SOFA:
-
Sequential Organ Failure Assessment
- VAP:
-
Ventilator-associated pneumonia
References
Nicholls TM, Morris AJ. Nosocomial infection in Auckland healthcare hospitals. N Z Med J. 1997;110:314–6.
Thompson DA, Makary MA, Dorman T, Pronovost PJ. Clinical and economic outcomes of hospital acquired pneumonia in intra-abdominal surgery patients. Ann Surg. 2006;243(4):547–52.
Infectious Diseases Society of America. Guidelines for the management of adults with hospital-acquired, ventilator associated, and healthcare associated pneumonia. Am J Respir Crit Care Med. 2005;171:388–416.
Eber MR, Laxminarayan R, Perencevich EN, Malani A. Clinical and economic outcomes attributable to health care-associated sepsis and pneumonia. Arch Intern Med. 2010;170(4):347–53.
Davis J, Finley E. The breadth of hospital-acquired pneumonia: non-ventilated versus ventilated patients in Pennsylvania. Pa Patient Saf Advis. 2012;9(3):99–105.
Chastre J, Wolff M, Fagon JY, Chevret S, Thomas F, Wermert D, et al. Comparison of 8 vs 15 days of antibiotic therapy for ventilator associated pneumonia in adults: a randomized trial. JAMA. 2003;290(19):2588–98.
Pugh R, Grant C, Cooke RPD, Dempsey G. Short-course versus prolonged-course antibiotic therapy for hospital-acquired pneumonia in critically ill adults (Review). Cochrane Database Syst Rev. 2015;8:1–43.
Dimopoulos G, Poulakou G, Pneumatikos IA, Armaganidis A, Kollef MH, Matthaiou DK. Short-vs long-duration antibiotic regimens for ventilator-associated pneumonia: a systematic review and meta-analysis. Chest. 2013;144:1759–67.
Kollef MH, Chastre J, Clavel M, Restrepo MI, Michiels B, Kaniga K, et al. A randomized trial of 7-day doripenem versus 10-day imipenem-cilastatin for ventilator-associated pneumonia. Crit Care. 2012;16:R218.
Helmy TA, Shehata SA, Noiem RS. Short course versus long-course antibiotic therapy for ventilator associated pneumonia. Am J Res Commun. 2015;3(11):111–22.
Capellier G, Mockly H, Charpentier C, Annane D, Blasco G, Desmette T, et al. Early-onset ventilator-associated pneumonia in adults randomized clinical trial: comparison of 8 versus 15 days of antibiotic treatment. PLoS ONE. 2012;7:e41290.
Yilmaz G, Salyan S, Aksoy F, Köksal İ. Individualized antibiotic therapy in patients with ventilator-associated pneumonia. J Med Microbiol. 2017;66(1):78–82.
Chawla K, Vishwanath S, Munim FC. Nonfermenting gram-negative bacilli other than Pseudomonas Aeruginosa and Acinetobacter spp. causing respiratory tract infections in a tertiary care center. J Glob Infect Dis. 2013;5(4):144–8.
Hedrick TL, McElearney ST, Smith RL, Evans HL, Pruett TL, Sawyer RG. Duration of antibiotic therapy for ventilator-associated pneumonia caused by non-fermentative gram-negative bacilli. Surg Infect (Larchmt). 2007;8(6):589–97.
Eagye KJ, Nicolau DP, Kuti JL. Impact of superinfection on hospital length of stay and costs in patients with ventilator-associated pneumonia. Semin Respir Crit Care Med. 2009;30(1):116–23.
Kuster SP, Rudnick W, Shigayeva A, Green K, Baqi M, Gold WL, et al. Previous antibiotic exposure and antimicrobial resistance in invasive pneumococcal disease: results from prospective surveillance. Clin Infect Dis. 2014;59(7):944–52.
Falagas ME, Rafailidis PI, Kofteridis D, Virtzili S, Chelvatzoglou FC, Papaioannou V, et al. Risk factors of carbapenem-resistant Klebsiella pneumoniae infections: a matched case control study. J Antimicrob Chemother. 2007;60:1124–30.
Chung DR, Song JH, Kim SH, Thamlikitkul V, Huang SG, Wang H, et al. High prevalence of multidrug-resistant nonfermenters in hospital-acquired pneumonia in Asia. Am J Resp Crit Care Med. 2011;184:1409–17.
Bonell A, Azarrafiy R, Huong VTL, Viet TL, Phu VD, Dat VQ, et al. A systematic review and meta-analysis of ventilator-associated pneumonia in adults in Asia: an analysis of national income level on incidence and etiology. Clin Infect Dis. 2019;68(3):511–8.
Enne VI, Personne Y, Grgic L, Gant V, Zumla A. Aetiology of hospital-acquired pneumonia and trends in antimicrobial resistance. Curr Opin Pulm Med. 2014;20(3):252–8.
Chawla R. Epidemiology, etiology, and diagnosis of hospital-acquired pneumonia and ventilator-associated pneumonia in Asian countries. Am J Infect Control. 2008;36(4):S93-100.
Acknowledgements
The authors would like to thank the Director General of Health Malaysia for his permission to publish this article. We are grateful to Nur Elya Shakirah and Siti Masuri for their involvement in assisting this study.
Funding
This research did not receive any specific grant from funding agencies in public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tan, Y.X., Wong, G.W. & Tan, Y.H. Superinfection associated with prolonged antibiotic use in non-ventilator associated hospital-acquired pneumonia. Int J Clin Pharm 43, 1555–1562 (2021). https://doi.org/10.1007/s11096-021-01282-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-021-01282-7